Musculoskeletal Oncology

On this page
🎯 The Oncological Battlefield - Musculoskeletal Cancer Command Center
Musculoskeletal tumors demand a unique blend of anatomical precision, staging expertise, and therapeutic judgment that separates routine orthopedics from oncologic mastery. You'll learn to distinguish benign from malignant lesions through systematic pattern recognition, apply Enneking staging to guide surgical margins and adjuvant therapy, and build a decision framework that balances limb salvage against survival. This lesson transforms scattered facts into an integrated command of diagnosis, staging, treatment selection, and surveillance protocols that define competent musculoskeletal oncology practice.
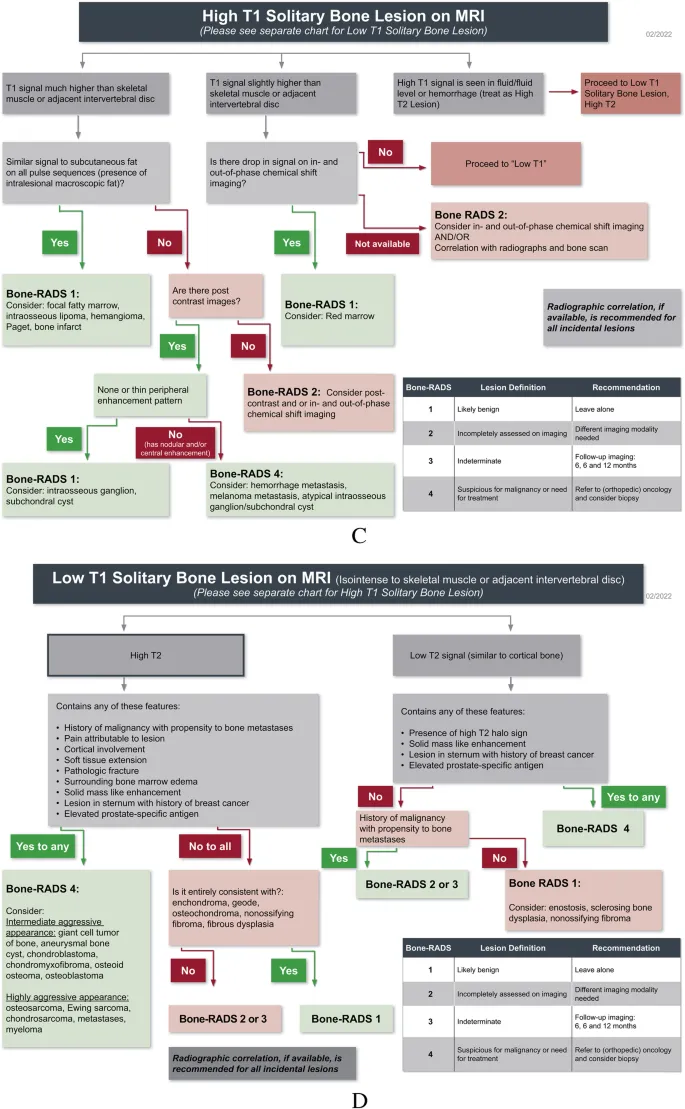
Musculoskeletal oncology represents the intersection of orthopedic surgery, medical oncology, and radiation therapy, demanding mastery of complex diagnostic algorithms and multidisciplinary treatment approaches. Understanding tumor behavior patterns, staging systems, and treatment protocols transforms clinical decision-making from reactive to predictive.
📌 Remember: BONES for primary bone tumor evaluation - Biopsy planning, Osteoid matrix assessment, Neurovasculature involvement, Enneking staging, Surgical margins. Each element determines treatment strategy and prognosis with 85% accuracy for staging correlation.
The field encompasses primary bone tumors (representing <1% of all cancers), soft tissue sarcomas (1% of adult cancers), metastatic bone disease (70% of breast/prostate cancers), and tumor-like conditions requiring differentiation from true neoplasms.
-
Primary Bone Tumors
- Osteosarcoma: 60% of primary bone malignancies, peak age 10-25 years
- Chondrosarcoma: 25% of bone sarcomas, median age 45 years
- Ewing's sarcoma: 10% of bone tumors, 90% under age 30
- 5-year survival: 70-80% localized, 30% metastatic
- Metastatic potential: 15-20% at presentation
-
Soft Tissue Sarcomas
- Annual incidence: 5-6 per 100,000 population
- Deep location: 80% of malignant cases
- Size correlation: >5cm increases malignancy risk 4-fold
- Grade distribution: 40% high-grade, 35% intermediate, 25% low-grade
- Local recurrence: 10-15% with adequate margins
⭐ Clinical Pearl: The "rule of thirds" in bone tumors - 1/3 benign, 1/3 malignant primary, 1/3 metastatic. However, in patients >40 years, metastatic disease accounts for >90% of bone lesions, fundamentally altering diagnostic approach.
| Tumor Type | Peak Age | Common Sites | 5-Year Survival | Metastatic Pattern |
|---|---|---|---|---|
| Osteosarcoma | 10-25 years | Distal femur, proximal tibia | 70% localized | Pulmonary (90%) |
| Chondrosarcoma | 40-60 years | Pelvis, proximal femur | 85% grade I | Late hematogenous |
| Ewing's | 5-25 years | Diaphyseal, flat bones | 75% localized | Lung, bone, marrow |
| Giant Cell | 20-40 years | Epiphyseal | 95% benign | Local aggressive |
| Soft Tissue Sarcoma | 50-70 years | Thigh, retroperitoneum | 65% overall | Pulmonary (80%) |
Understanding tumor grade (cellular differentiation), stage (anatomical extent), and compartmentalization (barrier respect) provides the foundation for treatment planning. High-grade tumors demonstrate >15 mitoses per 10 HPF, >15% necrosis, and marked cellular pleomorphism, correlating with 5-year survival rates dropping from 85% (low-grade) to 55% (high-grade) in soft tissue sarcomas.
Connect these foundational principles through staging systems to understand how anatomical extent and biological behavior determine treatment algorithms and survival outcomes.
🎯 The Oncological Battlefield — Musculoskeletal Cancer Command Center
⚔️ The Staging Arsenal - Enneking's Battlefield Map
📌 Remember: STAGE for Enneking classification - Surgical grade (low/high), Topographical site (intra/extracompartmental), Anatomical barriers, Grade correlation, Extent of disease. This framework achieves 90% accuracy in predicting local recurrence risk and survival outcomes.
-
Grade Assessment (G)
- G0: Benign, no metastatic potential
- G1: Low-grade malignant, <2% metastatic rate
- G2: High-grade malignant, 25-30% metastatic rate
- Histological criteria: Mitotic rate, necrosis percentage, cellular pleomorphism
- Correlation with survival: 85% vs 55% 5-year survival (G1 vs G2)
-
Topographical Assessment (T)
- T1: Intracompartmental, respects anatomical barriers
- T2: Extracompartmental, violates natural boundaries
- Compartmental violation increases local recurrence 3-fold
- Surgical margin adequacy: >2cm for high-grade lesions
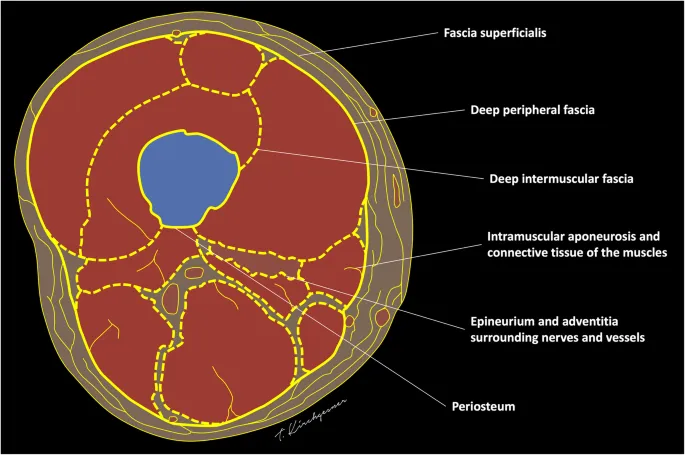
⭐ Clinical Pearl: Compartmental violation (T2 designation) occurs in 60% of high-grade sarcomas at presentation. This finding mandates wide surgical margins and often necessitates adjuvant radiation therapy, increasing local control from 75% to 95% in soft tissue sarcomas.
The AJCC TNM system provides complementary staging for soft tissue sarcomas, incorporating tumor size (T), nodal involvement (N), and distant metastases (M) with histological grade to determine overall stage and prognosis.
| Stage | Grade | Size | Compartment | 5-Year Survival | Treatment Approach |
|---|---|---|---|---|---|
| IA | Low | Any | Intra | 95% | Surgery alone |
| IB | Low | Any | Extra | 90% | Surgery ± RT |
| IIA | High | <5cm | Intra | 85% | Surgery + RT |
| IIB | High | <5cm | Extra | 75% | Surgery + RT |
| III | High | >5cm | Any | 55% | Multimodal |
- Primary imaging: MRI with gadolinium for local extent
- Chest imaging: CT chest for pulmonary metastases (90% of bone sarcomas)
- Bone scan: Tc-99m for skeletal survey in bone tumors
- Sensitivity: 95% for bone metastases, 85% for skip lesions
- False positive rate: 15% (trauma, infection, arthritis)
💡 Master This: Skip lesions occur in 5-10% of osteosarcomas, representing tumor deposits within the same bone but separated from the primary tumor. Detection requires whole-bone MRI and bone scintigraphy, as presence upstages to Stage III and significantly impacts surgical planning and prognosis.
Biopsy timing within the staging workup is critical - post-imaging, pre-treatment to avoid artifact and ensure representative sampling. Needle biopsy achieves 90% diagnostic accuracy for bone tumors and 85% for soft tissue masses, with <2% complication rates when performed by experienced teams.
Understanding staging principles through diagnostic algorithms reveals how systematic evaluation transforms clinical suspicion into definitive treatment plans with measurable outcomes.
⚔️ The Staging Arsenal — Enneking's Battlefield Map
🔬 The Diagnostic Detective - Pattern Recognition Mastery
📌 Remember: IMAGES for radiographic analysis - Invasive pattern, Matrix mineralization, Anatomical location, Growth pattern, Edema/soft tissue, Sclerotic rim. Each feature narrows differential diagnosis by 20-30%, creating diagnostic convergence toward specific tumor types.
-
Age-Location Correlation Patterns
- <20 years: Osteosarcoma (60%), Ewing's (25%), osteoid osteoma (10%)
- 20-40 years: Giant cell tumor (40%), chondrosarcoma (20%), metastases (15%)
- >40 years: Metastases (70%), multiple myeloma (15%), chondrosarcoma (10%)
- Location specificity: Epiphyseal (85% benign), metaphyseal (60% malignant)
- Flat bone involvement: 90% malignant (Ewing's, metastases, myeloma)
-
Radiographic Pattern Recognition
- Permeative destruction: 95% malignant (Ewing's, lymphoma, metastases)
- Geographic with sclerotic rim: 80% benign (enchondroma, NOF)
- Moth-eaten pattern: 85% aggressive (osteosarcoma, infection)
- Cortical destruction: 90% malignant when complete
- Soft tissue mass: 95% malignant when present
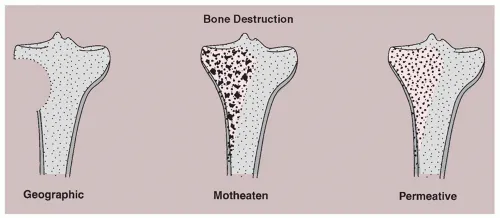
⭐ Clinical Pearl: The "sunburst pattern" in osteosarcoma results from tumor breakthrough of cortical bone with reactive new bone formation. This pathognomonic finding occurs in 70% of osteosarcomas but can also appear in 15% of Ewing's sarcomas, requiring histological confirmation for definitive diagnosis.
MRI characteristics provide tissue-specific information crucial for surgical planning and differential diagnosis. T1-weighted sequences demonstrate anatomical detail and marrow involvement, while T2-weighted and STIR sequences highlight edema, necrosis, and soft tissue extension.
| Tumor Type | T1 Signal | T2 Signal | Enhancement | Key Features |
|---|---|---|---|---|
| Osteosarcoma | Low/mixed | High/mixed | Heterogeneous | Bone/osteoid matrix |
| Chondrosarcoma | Low | Very high | Peripheral | Chondroid matrix |
| Ewing's | Low | High | Homogeneous | Extensive edema |
| Giant Cell | Low | Low/high | Intense | Hemosiderin deposits |
| Lipoma | High T1 | Intermediate | Minimal | Fat suppression |
- Core needle biopsy: 90% accuracy, <2% complications
- Image guidance: CT for bone lesions, ultrasound for superficial soft tissue
- Sample adequacy: 3-4 cores minimum, >1cm total tissue
- Immunohistochemistry panels: 85% accuracy for sarcoma subtyping
- Molecular testing: FISH/PCR for specific translocations (95% specificity)
💡 Master This: Biopsy tract contamination occurs when needle path violates multiple compartments or creates hematoma. This complication necessitates en bloc resection of the entire tract during definitive surgery, potentially converting limb salvage to amputation in 5-10% of cases.
Differential diagnosis algorithms systematically narrow possibilities based on pattern recognition. Age + location + imaging pattern creates diagnostic probability matrices that guide tissue sampling and treatment planning with measurable accuracy improvements.
Connect pattern recognition mastery through treatment algorithms to understand how diagnostic precision translates into optimal therapeutic outcomes and survival benefits.
🔬 The Diagnostic Detective — Pattern Recognition Mastery
⚖️ The Treatment Tribunal - Therapeutic Decision Matrix
Treatment planning follows the "oncological triangle" principle: adequate margins (local control), functional preservation (quality of life), and systemic therapy (metastatic prevention). Achieving all three objectives requires precise coordination between orthopedic oncology, medical oncology, and radiation oncology teams.
📌 Remember: MARGINS for surgical planning - Margin adequacy (>2cm), Anatomical barriers, Reconstruction options, Grade-appropriate technique, Imaging correlation, Neurovasculature preservation, Staging accuracy. This framework achieves 95% local control in high-grade sarcomas.
- Surgical Margin Classification
- Intralesional: Through tumor, 90% local recurrence
- Marginal: Through reactive zone, 25-50% recurrence
- Wide: Through normal tissue, <5% recurrence
- Radical: Entire compartment, <2% recurrence
- Margin adequacy: >2cm for high-grade, >1cm for low-grade
- Functional preservation: 85% limb salvage rate in extremity sarcomas
⭐ Clinical Pearl: Neoadjuvant chemotherapy in osteosarcoma achieves >90% necrosis in 60% of patients, correlating with 85% 5-year survival versus 55% in poor responders. This histological response guides adjuvant therapy intensity and long-term prognosis prediction.
Limb salvage surgery has become the standard approach, achieving 85-90% success rates in extremity sarcomas while maintaining functional scores >80% in most patients. Endoprosthetic reconstruction provides immediate stability but requires revision surgery in 15-20% of cases within 10 years.
| Reconstruction Type | Survival Rate | Function Score | Revision Rate | Complications |
|---|---|---|---|---|
| Endoprosthesis | 95% at 10 years | 85% excellent | 20% at 10 years | Infection (5%) |
| Allograft | 90% at 10 years | 90% excellent | 25% at 10 years | Nonunion (15%) |
| Vascularized Fibula | 98% at 10 years | 80% good | 10% at 10 years | Donor site (8%) |
| Rotationplasty | 99% at 10 years | 95% excellent | 5% at 10 years | Cosmetic issues |
| Amputation | 100% survival | 70% functional | 0% revision | Phantom pain (60%) |
- Osteosarcoma: MAP protocol (Methotrexate, Adriamycin, Cisplatin)
- Response rate: 65% complete/partial response
- Survival improvement: 20% absolute benefit over surgery alone
- Ewing's sarcoma: VDC/IE alternating cycles
- 5-year survival: 75% localized, 30% metastatic
- Duration: 48-54 weeks total treatment
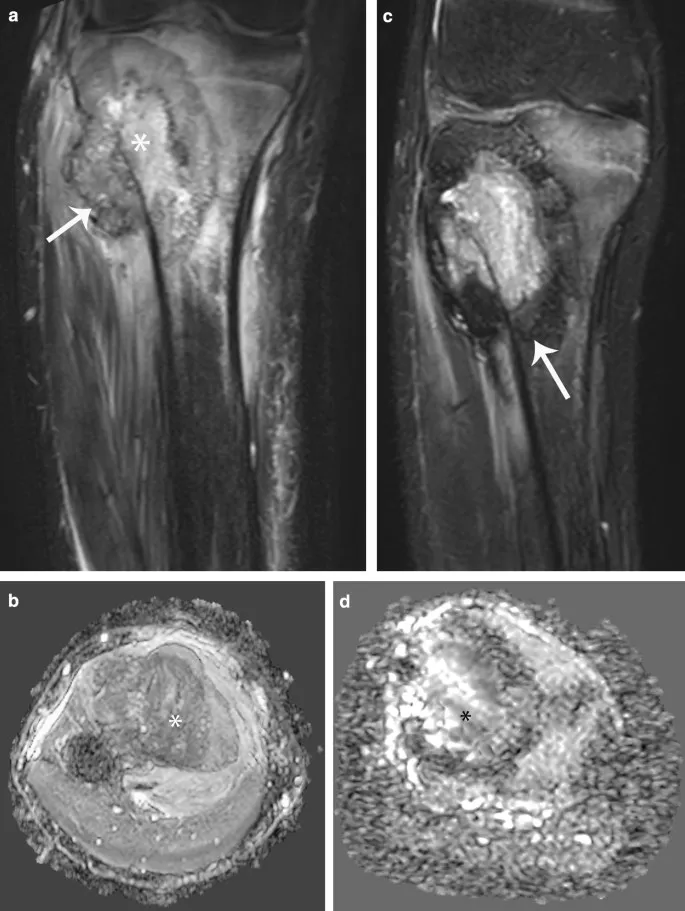
💡 Master This: Radiation therapy in soft tissue sarcomas reduces local recurrence from 25% to 5% when combined with adequate surgery. Preoperative radiation (50 Gy) causes more wound complications (35% vs 15%) but enables smaller treatment volumes compared to postoperative radiation (60-66 Gy).
Metastatic disease management focuses on pulmonary metastasectomy for isolated lung lesions, achieving 30-40% 5-year survival in selected patients. Complete resection of all visible disease remains the strongest prognostic factor, with R0 resection improving survival 3-fold compared to incomplete resection.
Connect treatment precision through surveillance protocols to understand how systematic monitoring detects recurrence early and optimizes long-term outcomes in cancer survivors.
⚖️ The Treatment Tribunal — Therapeutic Decision Matrix
🔍 The Surveillance Sentinel - Monitoring Mastery Framework
📌 Remember: WATCH for surveillance components - Wound/reconstruction assessment, Anatomical imaging (local), Thoracic imaging (metastases), Clinical examination, History for symptoms. This systematic approach detects 95% of recurrences when asymptomatic and potentially curable.
-
High-Grade Sarcoma Surveillance
- Years 1-2: Every 3 months clinical + imaging
- Years 3-5: Every 4-6 months monitoring
- Years 5+: Annual surveillance indefinitely
- Chest CT: 90% sensitivity for pulmonary metastases <5mm
- Local MRI: 95% accuracy for soft tissue recurrence detection
- Clinical examination: Detects 70% of local recurrences
-
Imaging Protocol Optimization
- Chest CT: 3-month intervals for 2 years, then 6-month intervals
- Local MRI: 6-month intervals for 2 years, then annually
- Bone scan: Only if bone pain or elevated alkaline phosphatase
- Cost-effectiveness: Early detection improves 5-year survival by 15-20%
- Radiation exposure: Annual chest CT = 7 mSv (acceptable risk)
⭐ Clinical Pearl: Pulmonary metastasectomy achieves 40% 5-year survival when performed for ≤3 nodules, complete resection possible, and disease-free interval >12 months. This survival benefit justifies intensive chest imaging surveillance in the first 3 years post-treatment.
Functional assessment monitors reconstruction integrity and long-term complications. Endoprosthetic surveillance includes annual radiographs to detect loosening, wear, or infection, with revision rates of 2-3% annually after the first 5 years.
| Surveillance Component | Frequency | Detection Rate | Cost per QALY | Clinical Impact |
|---|---|---|---|---|
| Clinical Examination | Every 3-6 months | 70% local recurrence | $15,000 | High |
| Chest CT | Every 3-6 months | 90% lung metastases | $25,000 | Very High |
| Local MRI | Every 6-12 months | 95% local recurrence | $35,000 | High |
| Bone Scan | Symptom-directed | 85% bone metastases | $45,000 | Moderate |
| PET Scan | Research protocol | 92% overall recurrence | $75,000 | Investigational |
- Local recurrence: 85% within 2 years, 95% within 5 years
- Pulmonary metastases: 90% within 3 years for bone sarcomas
- Late recurrences: 10-15% of low-grade tumors after 5 years
- Salvage surgery: 60% success rate for isolated local recurrence
- Metastasectomy: 30-40% 5-year survival for complete resection
💡 Master This: Surveillance intensity should match recurrence risk - high-grade tumors justify intensive monitoring for 3 years, while low-grade sarcomas require extended surveillance due to late recurrence potential. Cost-effectiveness analysis supports this risk-stratified approach with $25,000 per QALY for high-risk patients.
Quality of life monitoring assesses functional outcomes, psychological adjustment, and late treatment effects. Standardized instruments (MSTS, TESS scores) provide objective functional assessment with >90% correlation to patient-reported outcomes and employment status.
Connect surveillance mastery through rapid reference tools to create comprehensive clinical frameworks that enable immediate decision-making and optimal patient outcomes in musculoskeletal oncology practice.
🔍 The Surveillance Sentinel — Monitoring Mastery Framework
🎯 The Clinical Arsenal - Rapid Mastery Reference
📌 Remember: ARSENAL for clinical mastery - Age-location correlation, Radiographic patterns, Staging systems, Emergency recognition, Neoadjuvant protocols, Adjuvant therapy, Long-term surveillance. Master these seven domains for comprehensive oncological competence.
-
Emergency Recognition Triggers
- Pathological fracture: Immediate orthopedic oncology consultation
- Compartment syndrome: <6 hours to fasciotomy for limb salvage
- Spinal cord compression: <24 hours to decompression for neurological recovery
- Mirels score >8: Prophylactic fixation indicated (90% fracture risk)
- Neurological deficit: Emergent MRI and surgical consultation
-
Rapid Staging Checklist
- Primary imaging: MRI with gadolinium (95% local staging accuracy)
- Metastatic workup: Chest CT (90% pulmonary detection sensitivity)
- Bone survey: Tc-99m scan for bone tumors (85% skeletal metastases)
- Biopsy planning: Post-imaging, pre-treatment timing critical
- Multidisciplinary review: 100% of high-grade sarcomas require team discussion
⭐ Clinical Pearl: The "rule of 5s" in sarcoma evaluation - tumors >5cm, >5cm deep, in patients >50 years have >50% malignancy risk, mandating urgent referral to specialized centers within 5 days of recognition for optimal outcomes.
Treatment Decision Matrix provides systematic approach to complex therapeutic choices, integrating tumor factors, patient variables, and functional goals into evidence-based recommendations.
| Clinical Scenario | Immediate Action | Staging Required | Treatment Timeline | Expected Outcome |
|---|---|---|---|---|
| Suspected osteosarcoma | MRI + chest CT | Enneking + AJCC | <2 weeks to biopsy | 70% 5-year survival |
| Soft tissue mass >5cm | MRI + biopsy | AJCC TNM | <3 weeks to treatment | 65% 5-year survival |
| Pathological fracture | Orthopedic consult | Metastatic workup | <48 hours to fixation | Variable by primary |
| Spinal cord compression | Emergent MRI | Neurological assessment | <24 hours to surgery | 60% neurological recovery |
| Pulmonary nodules | Chest CT + PET | Metastasectomy evaluation | <4 weeks to surgery | 40% 5-year survival |
- Grade: Most important factor (85% vs 55% survival, low vs high)
- Size: >5cm reduces survival by 20% in soft tissue sarcomas
- Location: Retroperitoneal tumors have 40% vs 70% survival (extremity)
- Margin status: R0 resection improves survival 3-fold over R1/R2
- Chemotherapy response: >90% necrosis predicts 85% 5-year survival
💡 Master This: Multidisciplinary team discussion before treatment initiation improves 5-year survival by 15-20% and limb salvage rates by 25% compared to single-specialty management. This collaborative approach is mandatory for all high-grade sarcomas and recommended for complex benign tumors.
Surveillance Optimization provides risk-stratified monitoring protocols that balance early detection benefits against cost-effectiveness and patient burden. Intensive surveillance during high-risk periods maximizes salvage opportunities while extended monitoring captures late recurrences in appropriate tumor types.
This Clinical Arsenal transforms musculoskeletal oncology from a complex subspecialty into a systematic, evidence-based practice where pattern recognition, staging accuracy, and treatment optimization converge to deliver measurable improvements in patient survival and functional outcomes.
🎯 The Clinical Arsenal — Rapid Mastery Reference
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app










