Definition & Epidemiology - Bone Gone Wild
- Chronic, focal disorder of accelerated, disorganized bone remodelling.
- Pathophysiology: ↑ Osteoclastic resorption → chaotic ↑ osteoblastic formation → structurally weak, enlarged, deformed bone.
- Prevalence: Affects 1-3% of adults > 55 yrs. M > F.
- Geography: Common in Western countries; rare in India/Asia.
- Etiology: Likely viral (Paramyxovirus) + genetic (SQSTM1 gene mutations in 15-40% familial cases).
⭐ Paget's disease is often asymptomatic and discovered incidentally on X-ray or due to isolated ↑ Alkaline Phosphatase (ALP).
Pathophysiology - Osteoclast Frenzy
- Trigger: Likely viral (e.g., paramyxovirus) or genetic (SQSTM1 mutations) → initiates osteoclast dysfunction.
- Osteoclast Frenzy:
- Marked ↑ in osteoclast number, size (giant cells, up to 100 nuclei), and resorptive activity.
- Hyper-responsive to RANKL and Vitamin D.
- Phases of Bone Remodeling:
- Lytic Phase: Intense, localized osteoclastic bone resorption.
- Mixed Phase: Compensatory but chaotic, excessive osteoblastic formation of woven bone.
- Sclerotic Phase: Dense, disorganized, structurally weak bone results.
- Outcome: Enlarged, deformed, hypervascular, mechanically compromised bone.
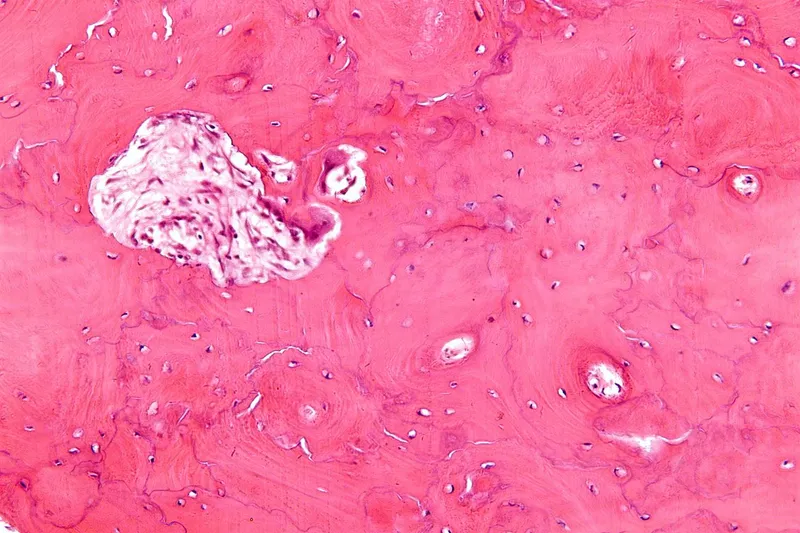
⭐ Histology: Pathognomonic "mosaic pattern" (jigsaw/cement lines) from irregular turnover.
Clinical Manifestations - Signs of the Storm
- Often asymptomatic; many diagnosed incidentally.
- Bone Pain: Most common; deep, aching, nocturnal.
- Deformities:
- Skull: ↑ Head size (hats don't fit), frontal bossing.
- Long bones: Bowing (tibia: "saber shin"; femur).
- Warmth over affected bone (hypervascularity).
- Pathological Fractures: "Chalkstick" type (esp. femur).
- Joint pain from secondary osteoarthritis.
- Neurological: Deafness (CN VIII compression), spinal stenosis.
⭐ Increased hat size or needing a larger hat is a classic sign of skull involvement.
- Rare: High-output heart failure, osteosarcoma (<1%).
 oka
oka
Diagnosis - Cracking the Case
- Biochemical Markers:
- ↑ Serum Alkaline Phosphatase (ALP) - markedly elevated.
- ↑ Urine hydroxyproline, N/C-telopeptides (turnover markers).
- Serum $Ca^{2+}$ & $PO_4^{3-}$ usually normal.
- Radiology (X-ray):
- Lytic ("blade of grass" sign), mixed, sclerotic ("cotton wool" skull, "picture frame" vertebra) phases.
- Bone expansion, cortical thickening.

- Bone Scan (Scintigraphy):
- ↑ Uptake ("hot spots") - shows disease extent.
⭐ Serum ALP is the most crucial biochemical marker for diagnosis and monitoring treatment response.
- Biopsy: For suspected sarcoma; reveals mosaic pattern.
Complications & Management - Taming the Tide
-
Complications:
- Fractures: Pathological ("chalkstick" type, common in femur, tibia).
- Deformity: Bowing of long bones (e.g., tibia, femur), skull enlargement ("Tam o' Shanter" sign).
- Arthritis: Secondary osteoarthritis in adjacent joints (hip, knee).
- Neurological: Deafness (CN VIII compression), spinal stenosis, nerve root compression, hydrocephalus.
- Neoplastic Transformation: Osteosarcoma (<1% of cases, poor prognosis), giant cell tumor (rare, benign).
- Cardiac: High-output cardiac failure (rare, with extensive skeletal involvement >15%).
- Metabolic: Hypercalcemia (esp. with immobilization), hypercalciuria & kidney stones.
-
Management Aims: Reduce bone pain, slow disease progression, prevent/treat complications.
-
Indications for Treatment:
- Symptomatic disease (bone pain, neurological symptoms).
- Specific complications (e.g., fractures, arthritis, neurological compromise).
- Serum Alkaline Phosphatase (ALP) >2-4x upper limit of normal, or rising.
- Planned surgery on a pagetic bone.
- Asymptomatic involvement of high-risk sites (e.g., skull base, vertebrae, weight-bearing long bones).
-
Pharmacological (First-line):
- Bisphosphonates (inhibit osteoclast activity):
- Zoledronic acid: 5 mg IV infusion once (preferred due to long remission).
- Oral: Alendronate, Risedronate (daily or weekly regimens).
- Calcitonin: Second-line (if bisphosphonates contraindicated/intolerable).
- Bisphosphonates (inhibit osteoclast activity):
-
Surgical Intervention: For complications like fractures, severe deformity requiring osteotomy, joint replacement for arthritis, or decompression for neurological impingement.
-
Monitoring: Symptom assessment, serial ALP levels (aim for normalization or significant reduction).

⭐ Osteosarcoma, though rare (<1%), is the most dreaded complication of Paget's disease, often presenting with a sudden increase in bone pain, new swelling, and a rapidly rising Alkaline Phosphatase level.
High‑Yield Points - ⚡ Biggest Takeaways
- Disordered bone remodeling: Excessive osteoclastic resorption followed by disorganized osteoblastic bone formation.
- Key symptoms: Bone pain, pathological fractures; often asymptomatic.
- Lab hallmark: Markedly ↑ Alkaline Phosphatase (ALP); normal serum calcium and phosphate.
- X-ray findings: "Cotton wool" skull, "blade of grass" sign, thickened cortices.
- Major complications: Osteosarcoma (<1%), deafness (skull involvement), high-output cardiac failure.
- Treatment cornerstone: Bisphosphonates (e.g., zoledronic acid).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

