Fluorosis Intro - Fluoride's Footprint
- Definition: Chronic metabolic bone and dental disorder due to prolonged excessive fluoride exposure.
- Etiology: Ingestion/inhalation of high fluoride levels.
- Primary Source: Drinking water (WHO safe limit: <1.5 ppm).
- Other Sources: Certain foods (e.g., tea), industrial emissions, some dental products.
- Epidemiology:
- Endemic in over 20 countries; India is severely affected.
- "Fluoride belt" in India: Spans across numerous states.
⭐ Endemic fluorosis in India is primarily due to high fluoride content in drinking water.
- Pathogenesis Teaser: Fluoride ions ($F^-$) replace hydroxyl groups in bone's hydroxyapatite, forming less soluble fluoroapatite.

Fluoride's Effects - Bone & Tooth Bane
⭐ Fluoride replaces hydroxyl ions in hydroxyapatite to form fluoroapatite ($Ca_{10}(PO_4)_6F_2$), which is more resistant to acid dissolution but can make bone more brittle at high concentrations.
- Bone Pathophysiology:
- Reaction: $Ca_{10}(PO_4)_6(OH)2 + 2F^- \rightarrow Ca{10}(PO_4)_6F_2 + 2OH^-$
- ↑ Osteoblastic activity (early); impaired mineralization & ↓ bone quality (late/high dose).
- Results in: osteosclerosis, exostoses, ligamentous calcification, ↑ fracture risk.
- Skeletal fluorosis risk with water F > 4 ppm.
- Dental Effects:
- Dental fluorosis: mottling, chalky patches, pitting, brown stains.
- Occurs during tooth development; risk with water F > 1.5-2 ppm.
- Low F (<1 ppm) is caries-protective.

Fluorosis Manifestations - Telltale Traits
-
Dental Fluorosis (Earliest sign):
-
Symmetrical, chalky white opacities, yellow-brown discoloration, pitting.
-

-
Dean's Index for Dental Fluorosis:
Score Appearance 0 Normal 1 Questionable (Slight changes) 2 Very Mild (<25% opaque areas) 3 Mild (<50% opaque areas) 4 Moderate (All surfaces, stain) 5 Severe (Hypoplasia, pitting)
-
-
Skeletal Fluorosis:
- Phase 1: Sporadic pain, stiffness.
- Phase 2: Constant pain, joint stiffness, osteosclerosis (spine, pelvis).
- Phase 3 (Crippling): Limited movement, kyphosis, flexion contractures, genu valgum/varum.
- Ligament/interosseous membrane calcification.
- 📌 Mnemonic: "Stiff Spine, Sore Spots" (early skeletal).
-
Neurological: Radiculomyelopathy (nerve/cord compression).
-
Non-Skeletal: GI (anorexia, pain), muscle weakness.
⭐ Skeletal fluorosis can lead to crippling deformities, with spinal compression and radiculomyelopathy being severe complications.
Fluorosis Diagnosis - Pinpointing the Problem
- Clinical Suspicion: History of exposure (endemic area), dental mottling, non-specific musculoskeletal pain, restricted joint movement.
- Investigations:
- Radiography: Key for skeletal fluorosis.
- Urinary fluoride: ↑ levels (e.g., > 8 mg/L indicates high exposure; normal < 1 mg/L).
- Serum fluoride: Less reliable than urinary.
- Bone biopsy: Rarely needed.
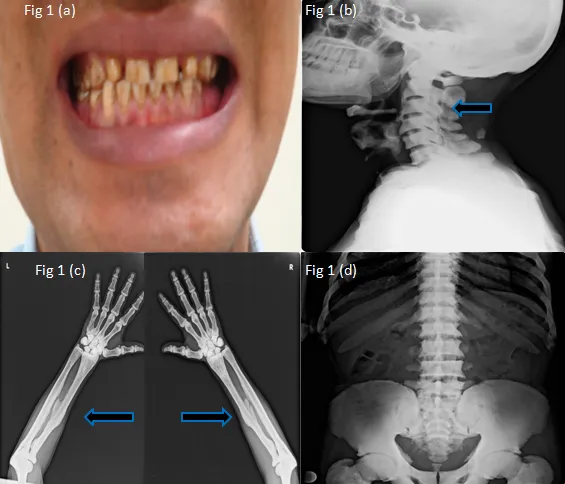
⭐ Radiological findings in skeletal fluorosis include osteosclerosis, osteophytosis, and calcification of ligaments and interosseous membranes (e.g., forearm, pelvis).
Fluorosis Control - Taming the Toxin
-
Prevention is Key:
- Safe Water Supply: Ensure drinking water fluoride levels are below 1.0 mg/L (WHO permissible limit) or 1.5 mg/L (Indian standard).
- Nutritional Support: Adequate calcium, vitamin C, and antioxidants.
-
Defluoridation Techniques:
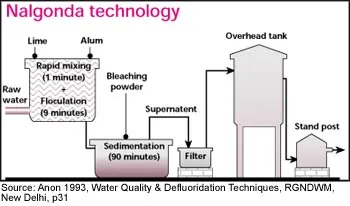
Method Principle Nalgonda Alum, lime, bleaching powder precipitation Activated Alumina Adsorption Bone Char Adsorption, ion exchange Reverse Osmosis Membrane filtration Electrodialysis Ion separation using electric current 📌 Nalgonda technique: Remember "NAL" - Nalgonda uses Alum and Lime.
⭐ The Nalgonda technique is a widely used community defluoridation method in India involving alum, lime, and bleaching powder.
- Management of Skeletal Fluorosis:
- No specific cure; focus on symptomatic relief (analgesics, physiotherapy).
- Surgical decompression for neurological complications in severe cases (e.g., crippling fluorosis).
High-Yield Points - ⚡ Biggest Takeaways
- Caused by chronic excess fluoride intake, mainly via drinking water (>1.5 ppm).
- Skeletal fluorosis features osteosclerosis, osteophytes, and ligamentous/tendon calcification (enthesopathy).
- Dental fluorosis presents as mottled enamel (chalky white to brown stains).
- Crippling fluorosis causes severe joint stiffness, deformities, and neurological compression (e.g., radiculomyelopathy).
- Key X-ray signs: ↑ bone density, calcification of interosseous membrane (forearm, leg).
- Genu valgum is a common deformity, especially in children in endemic fluorosis regions.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more


