Tendon Transfer Principles & Donors - The Great Muscle Shuffle
-
Goal: Restore lost function via rerouted tendon.
-
Indications: Irreversible nerve palsy (radial, median, ulnar), muscle loss.
-
Timing: 3-6 months post-injury; stable soft tissues, supple joints.
-
Boyes' Pre-requisites (Critical):
- Supple joints (full passive ROM).
- Soft tissue equilibrium (mature scar, no inflammation).
- Donor muscle strength: MRC Grade ≥ 4/5.
- Expendable donor (no significant functional loss).
- Similar excursion & power to recipient if possible.
-
Core Principles:
- One transfer for one function.
- Synergistic muscles preferred.
- Straight line of pull.
- Correct tension (avoid too tight/loose).
- Secure fixation.
-
Common Donors (Forearm):
- PT (Pronator Teres)
- FCR (Flexor Carpi Radialis), FCU (Flexor Carpi Ulnaris)
- BR (Brachioradialis)
- ECRL (Extensor Carpi Radialis Longus), ECRB (Extensor Carpi Radialis Brevis), ECU (Extensor Carpi Ulnaris)
- APL (Abductor Pollicis Longus)
- Consider: Strength, excursion, direction.
⭐ Key Boyes' pre-requisites for successful tendon transfer: Supple joints & donor muscle strength of at least MRC Grade 4/5.
Radial Nerve Palsy Transfers - Wrist Drop Reversal
- Goal: Restore wrist, finger (MCPJ), & thumb extension/abduction.
- Wrist Extension (Workhorse):
- Pronator Teres (PT) → ECRB (Extensor Carpi Radialis Brevis).
- Finger (MCPJ) Extension:
- FCU (Flexor Carpi Ulnaris) / FCR (Flexor Carpi Radialis) / FDS (Flexor Digitorum Superficialis) (Middle/Ring) → EDC (Extensor Digitorum Communis).
- Thumb Extension/Abduction:
- PL (Palmaris Longus) → EPL (Extensor Pollicis Longus) (rerouted).
- FDS (Ring) / FCR (split) → EPL.
⭐ PT to ECRB is crucial for wrist extension. Insertion into ECRB, not ECRL (Extensor Carpi Radialis Longus), prevents unwanted radial deviation of the wrist during extension.
Median & Ulnar Nerve Palsy Transfers - Grasp & Pinch Revival
- Median Nerve Palsy (Ape Thumb):
- Goal: Restore thumb opposition.
- Common Transfers (Opponensplasty):
- EIP to APB (Bunnell).
- FDS (Ring) to APB (Riordan).
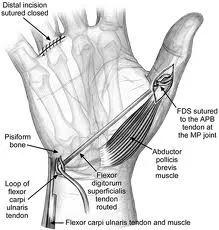
- PL to APB (Camitz).
- Ulnar Nerve Palsy (Claw Hand, Froment's sign):
- Goal: Correct clawing, restore key pinch.
- Claw Correction (Intrinsic Minus):
- Static: Zancolli lasso (FDS loop).
- Dynamic: Brand (FDS MF 4-tail), Fowler (ECRL + graft).
- Key Pinch (Adductor Pollicis): BR/ECRB + graft.
- 📌 Mnemonic: "BRAND new FDS for 4 fingers" (Brand: FDS for 4 fingers).
- Combined Palsy: Prioritize opposition > finger flexion > intrinsics.
⭐ For low ulnar nerve palsy, Zancolli lasso procedure (FDS loop through A1 pulley) is a common static transfer to correct clawing by preventing MCP hyperextension.
Tendon Transfer Post‑Op & Complications - Healing & Hurdles
- Post-Op Protocol:
- Immobilization: Splint/cast for 3-6 weeks.
- Mobilization: Early controlled passive motion, progressing to active motion.
- Rehabilitation: Phased physiotherapy crucial for strength, ROM, and function.
- Healing Dynamics: Tendon junction strength builds over weeks; maturation takes months.
- Potential Hurdles:
- Adhesions (most frequent, restrict glide).
- Rupture (risk with premature stress or poor compliance).
- Imbalance: Overcorrection or undercorrection.
- Joint stiffness/contracture.
⭐ Adhesions are the most common complication following tendon transfer, significantly limiting active range of motion and functional outcome.
High‑Yield Points - ⚡ Biggest Takeaways
- Radial Nerve Palsy: Common transfers: PT to ECRB (wrist), FCU to EDC (fingers), PL to EPL (thumb).
- Median Nerve Palsy: Opponensplasty is key (e.g., EIP to APB, FDS to APB).
- Ulnar Nerve Palsy: For claw hand: FDS lasso (Zancolli) or Brand transfer.
- Power Loss: Transferred tendon loses one grade of power.
- Prerequisites: Supple joints, good passive ROM, healthy soft tissue.
- Timing: After nerve recovery plateaus (typically 3-6 months).
- Goal: Restore essential functions, not anatomical normality.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

