Nerve Anatomy & Injury Types - Hand's Wiring Woes
- Major Hand Nerves:
- Median N.:
- Motor: LOAF (Lumbricals 1&2, Opponens Pollicis, APB, FPB-superficial).
- Sensory: Palm: thumb, index, middle, radial ½ ring; Dorsal tips.
- 📌 Mnemonic: "Median LOAF".
- Ulnar N.:
- Motor: Intrinsics (Hypothenar, Interossei, Lumbricals 3&4, AdP, FPB-deep).
- Sensory: Medial 1.5 fingers (palm & dorsum).
- Radial N. (Superficial branch):
- Sensory: Dorsal radial hand, thumb, index, middle fingers (proximal).
- Motor (from main radial nerve before superficial branch): Wrist/finger extensors.
- Median N.:
- Nerve Injury Classification (Seddon):
- Neuropraxia: Conduction block, myelin damage, full recovery. No Wallerian degeneration.
- Axonotmesis: Axon damaged, endoneurium intact. Wallerian degeneration occurs. Good recovery.
- Neurotmesis: Complete nerve transection (axon + connective tissue). Needs surgery.
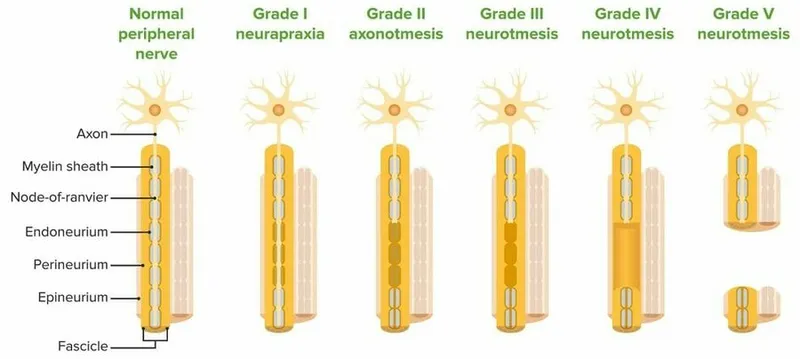
- Sunderland Grades (Detail Seddon):
- Grade I: Neuropraxia.
- Grade II: Axonotmesis (axon damage, endoneurium intact).
- Grade III: Endoneurium damaged, perineurium intact.
- Grade IV: Perineurium damaged, epineurium intact.
- Grade V: Complete transection (neurotmesis).
⭐ The ulnar nerve is most commonly injured at the elbow (cubital tunnel syndrome) or wrist (Guyon's canal).
Median Nerve Injury - Ape's Anguish
- Etiology: Supracondylar fracture, lunate dislocation, Carpal Tunnel Syndrome (CTS).
- Motor Loss (LOAF muscles):
- Thenar muscles (Abductor Pollicis Brevis, Opponens Pollicis, Flexor Pollicis Brevis superficial head) & lateral 2 Lumbricals.
- Results in thenar wasting, weak thumb opposition & abduction.
- Deformities:
- Ape Hand: Thumb adducted, extended, and laterally rotated; no opposition.

- Benediction Sign (High Lesion): Index & middle fingers remain extended on fist attempt. 📌 "Can't make 'M' (Median) with hand."
- Ape Hand: Thumb adducted, extended, and laterally rotated; no opposition.
- Sensory Loss: Palmar aspect of lateral 3.5 digits; dorsal tips of same.
- Key Tests: Pen test (inability to abduct thumb), Ochsner's clasping test, Phalen's test / Tinel's sign (for CTS).
⭐ Benediction Sign (dynamic, on attempting fist) vs. Ulnar Claw Hand (static, at rest) is a key high-yield differentiator often tested to distinguish nerve injuries.
Ulnar Nerve Injury - Claw's Curse
- Sites: Elbow (cubital tunnel, supracondylar #), Wrist (Guyon's, hook of hamate #), Leprosy.
- Motor:
- High lesions: FCU, FDP (ulnar ½).
- All lesions: Hand intrinsics (hypothenar, interossei, AdP, medial 2 lumbricals).
- Deformity: Claw Hand (4th & 5th fingers): MCPJ hyperextension, IPJ flexion.
- 📌 Ulnar Paradox: High lesion → less claw (FDP paralyzed); Low lesion → more claw.
- Signs:
- Froment's Sign: Thumb IPJ hyperflexion on pinch (AdP weak).
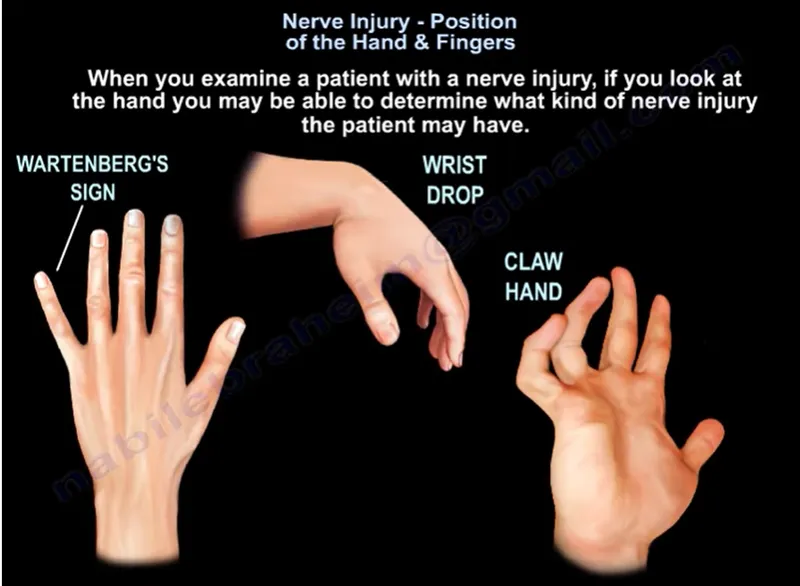
- Wartenberg's Sign: Abducted 5th finger.
- Card Test: Weak finger adduction.
- Sensory Loss: Ulnar 1.5 fingers (volar/dorsal).
⭐ Ulnar Paradox: High ulnar lesions cause less clawing than low lesions (FDP paralysis).
Radial Nerve & Repair Routes - Droop & Mend
-
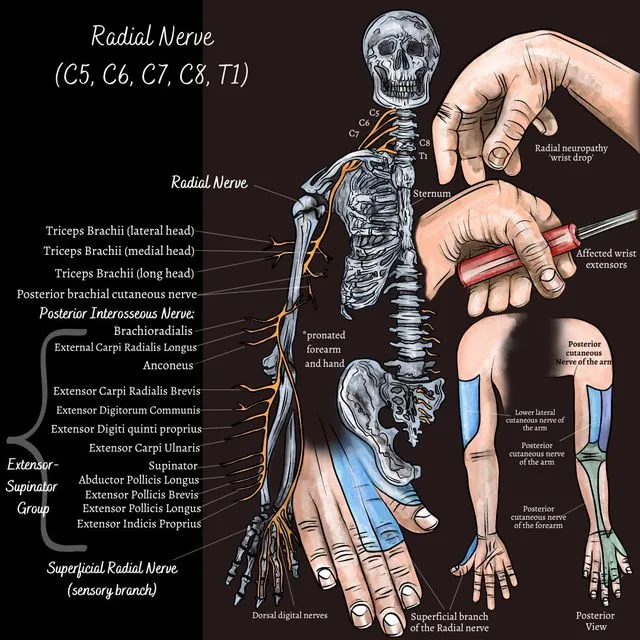
Radial Nerve Injury Manifestations:
- Motor: Wrist drop (loss of ECRL/ECRB), finger drop (loss of EDC/EIP/EDM), weak thumb abduction/extension (APL/EPL/EPB). Inability to make a fist effectively due to loss of wrist stabilization.
- Sensory: Loss over dorsal radial hand, anatomical snuffbox, dorsal aspect of radial 3.5 fingers (variable distribution).
- Common sites: Axilla (crutches), spiral groove of humerus (Holstein-Lewis fracture), supracondylar area, forearm (Posterior Interosseous Nerve syndrome - motor only, spares ECRL, so no complete wrist drop).
- 📌 "Saturday Night Palsy" from compression; also crutch palsy.
-
Diagnostic & Repair Pathway:
-
Assessment: Detailed motor (MRC scale) & sensory exam. Tinel's sign progression indicates regeneration.
-
Investigations: EMG/NCS after 3-4 weeks to confirm, localize lesion, and prognosticate recovery.
-
Management Strategy:
-
Surgical timing: Early for sharp transections; observation for 3-6 months in closed injuries before considering surgery if no recovery.
-
-
⭐ For high radial nerve palsy, standard tendon transfers include Pronator Teres (PT) to Extensor Carpi Radialis Brevis (ECRB) for wrist extension, Flexor Carpi Ulnaris (FCU) or Flexor Carpi Radialis (FCR) to Extensor Digitorum Communis (EDC) for finger extension, and Palmaris Longus (PL) to Extensor Pollicis Longus (EPL) for thumb extension (Boyes transfer principles).
High-Yield Points - ⚡ Biggest Takeaways
- Median nerve injury: Ape Hand, loss of thumb opposition, sensory loss radial 3.5 digits.
- Ulnar nerve injury: Claw Hand (4th & 5th), Froment's sign, sensory loss ulnar 1.5 digits.
- Radial nerve injury: Wrist drop, finger drop, sensory loss dorsal radial hand.
- High median lesion: Benediction Hand (fist attempt); Low lesion: Ape Hand.
- Ulnar paradox: High ulnar lesions cause less clawing than low lesions (FDP paralysis).
- Key tests: Ochsner's (Median), Card test (Ulnar), Pen test (Median-APB).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

