Dupuytren's Disease: Intro & Risk Factors - Puckering Palms Primer
- Benign, progressive fibroproliferative disorder of palmar/digital fascia.
- Forms nodules, cords → flexion contractures (MCP, PIP joints). Ulnar digits (ring, little) common.
- Risk Factors:
- Age (>50 yrs), Male, Family Hx, Northern European descent.
- 📌 DDAShT (Mnemonic: Diabetics Drink Alcohol & Smoke Tobacco):
- Diabetes, Dyslipidemia
- Alcohol
- Smoking
- Hepatic disease, HIV
- Trauma, anti-epilepTics
⭐ Most common in males of Northern European descent, often bilateral.
Dupuytren's Disease: Pathoanatomy & Genetics - Fibrous Finger Fiasco
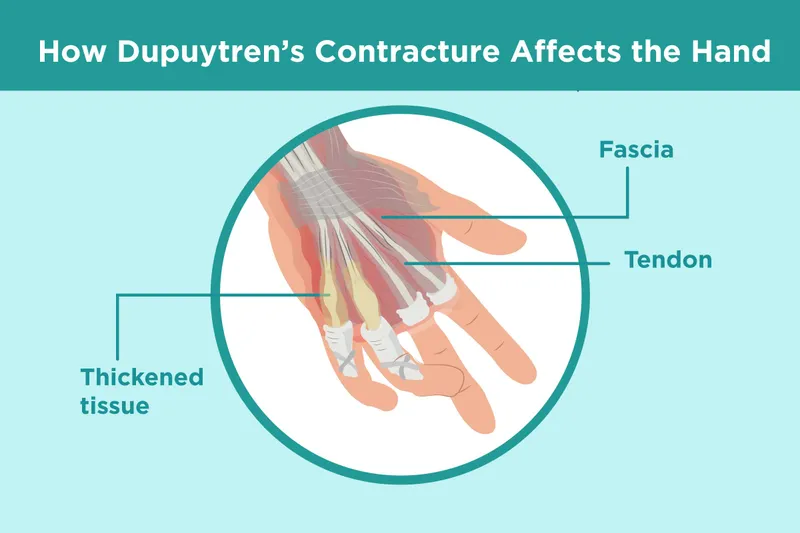
- Pathoanatomy: Fibroproliferative disorder of palmar/digital fascia.
- Key cells: Myofibroblasts (α-SMA+).
- Collagen: ↑ Type III, ↓ Type I.
- Affected structures:
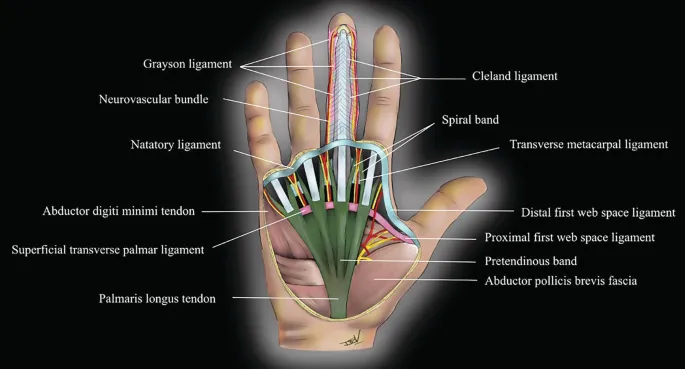
- Prebendinous bands → cords.
- Natatory ligaments → web space contractures.
- Spiral cord (of Gosset) → PIP joint contracture; displaces neurovascular bundle (NVB) superficially & medially.
- Lateral digital sheet.
- Grayson's & Cleland's ligaments (less common).
- Genetics:
- Autosomal dominant inheritance, variable penetrance.
- Strong association: Northern European descent ("Viking disease").
- Possible gene links: Wnt signaling pathway (e.g., WNT2, WNT7B).
⭐ Pathologically characterized by proliferation of myofibroblasts and deposition of Type III collagen replacing Type I collagen.
Dupuytren's Disease: Clinical Features & Staging - Contracture Clues & Count
- Features:
- Palmar/digital nodules → cords.
- Skin: Pitting, tethering.
- Contractures: MCPJ, PIPJ (ring, little finger common).
- Garrod's pads (dorsal PIPJ, ~50%).
- Hueston's Tabletop Test: Palm flat on table? Positive if unable (MCPJ contracture).
⭐ Positive Hueston's test: MCPJ contracture. Surgery: MCPJ >30° or any PIPJ contracture.
- Staging (Tubiana): Total flexion deformity (MCPJ+PIPJ+DIPJ).
Stage Deformity (°) 0 No lesion N Nodule only 1 1-45 2 46-90 3 91-135 4 >135
Dupuytren's Disease: Management Spectrum - Releasing the Grip
-
Conservative Management:
- Observation: Mild disease, no functional loss.
- Splinting: Generally ineffective for preventing progression.
- Steroid injections: May soften nodules, limited long-term benefit.
-
Minimally Invasive Options:
- Collagenase Clostridium Histolyticum (CCH) Injection: Enzymatic fasciotomy. For palpable cords, MCPJ/PIPJ contractures.
- Needle Aponeurotomy (NA): Percutaneous cord disruption. Best for single, well-defined MCPJ cords.
-
Surgical Management: Indications: MCPJ contracture >30°, any PIPJ contracture, or significant functional impairment.
- Fasciectomy:
- Limited/Segmental: Excision of diseased fascia. Most common.
- Radical/Total: Excision of all palmar fascia (↑morbidity, less common).
- Dermofasciectomy: Excision of fascia + overlying skin, then skin graft. For severe/recurrent disease.
- Salvage: Amputation (rare, severe recurrent cases).
- Fasciectomy:
-
Post-Intervention Care:
- Splinting (night-time, extension).
- Hand therapy: Crucial for ROM and function.
⭐ Needle aponeurotomy is suitable for mild, single-cord MCPJ contractures but has a higher recurrence rate than fasciectomy.
High‑Yield Points - ⚡ Biggest Takeaways
- Progressive fibroproliferative disorder of the palmar and digital fascia.
- Strong links: Northern European descent, diabetes mellitus, alcoholism, smoking.
- Features painless palmar nodules and cords, causing progressive flexion contractures.
- Primarily affects the ring and little fingers (ulnar side).
- Hueston's tabletop test is positive (patient cannot lay hand flat on table).
- Surgery (e.g., fasciectomy) for MCP contracture >30° or any PIP joint contracture.
- Myofibroblasts are the key pathological cells involved in contracture.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

