OA Shoulder: Intro & Epi - Creaky Joint Culprits
- Definition: Cartilage degeneration in Glenohumeral (GH) or Acromioclavicular (AC) joints.
- Types:
- Primary: Idiopathic, age-related wear.
- Secondary: Due to trauma, Rotator Cuff (RC) tear, instability, overuse, genetics, obesity.
- Prevalence: Common, incidence ↑ with age. Affects women more than men, especially post-menopause.
- Key Risk Factors: Age >50 yrs, female, obesity, prior trauma, repetitive overuse, RC tears, chronic instability, genetics.
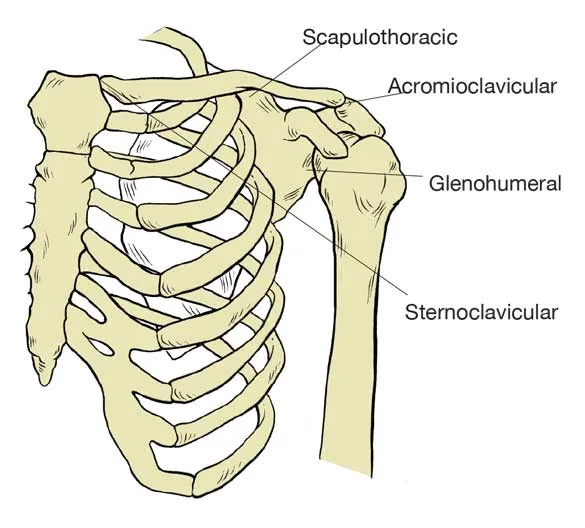
⭐ Glenohumeral OA is less common than knee/hip OA but significantly disabling.
OA Shoulder: Patho & Types - Joint's Slow Grind
- Pathophysiology: Joint's slow grind.
- Cartilage: Initial loss of proteoglycans & water, then collagen network disruption, and chondrocyte dysfunction/death.
- Subchondral Bone: Sclerosis (thickening), marginal osteophytes (bone spurs), and subchondral cyst formation.
- Synovitis: Mild, chronic inflammation of the synovial lining.
- Classification (GH OA): Samilson-Prieto (humeral/glenoid osteophytes).
- Grade 1: Osteophytes <3 mm.
- Grade 2: Osteophytes 3-7 mm.
- Grade 3: Osteophytes >7 mm; may show joint space narrowing, sclerosis.
⭐ > Posterior glenoid wear is a common finding in advanced glenohumeral OA.
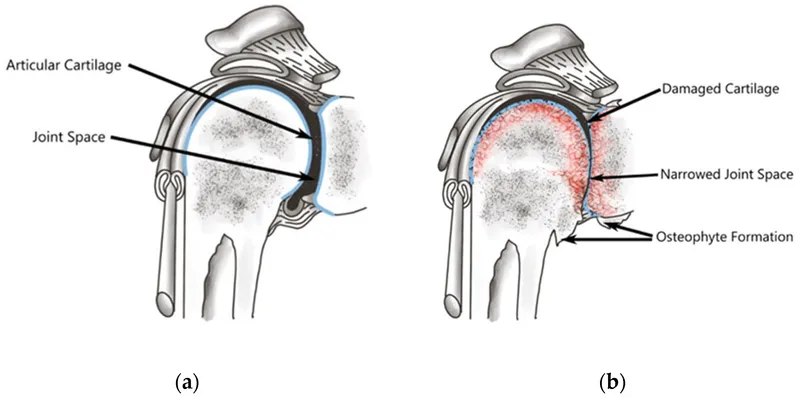
OA Shoulder: Clinical & Dx - Spotting the Stiffness
- Symptoms:
- Pain: Insidious onset, activity-related, night pain, progressive.
- Stiffness: Morning or after inactivity, progressive.
- Crepitus: Grinding/popping sensation with movement.
- ↓Range of Motion (ROM): Global, particularly external rotation & abduction.
- Functional limitation: Difficulty with ADLs (dressing, combing hair), overhead activities.
- Signs:
- Tenderness: Over glenohumeral joint line (anterior/posterior).
- Muscle atrophy: Supraspinatus, infraspinatus, deltoid in advanced stages.
- Deformity: Flattening of shoulder contour (late).
- Diagnosis:
- History & Physical Exam:
- Apley's scratch test: Assesses functional internal/external rotation.
- Hawkins-Kennedy, Neer's: For associated rotator cuff pathology.
- Imaging:
- X-ray (Standard views: AP, axillary lateral, Grashey):
- 📌 LOSS: Loss of joint space (JSN - often superior/posterior), Osteophytes (humeral head/glenoid), Subchondral sclerosis, Subchondral cysts.
- Glenoid erosion patterns (e.g., Walch B2: biconcave glenoid, posterior wear).
- MRI/CT indications: Evaluate rotator cuff, bone stock for arthroplasty, diagnostic uncertainty.
- X-ray (Standard views: AP, axillary lateral, Grashey):
- History & Physical Exam:
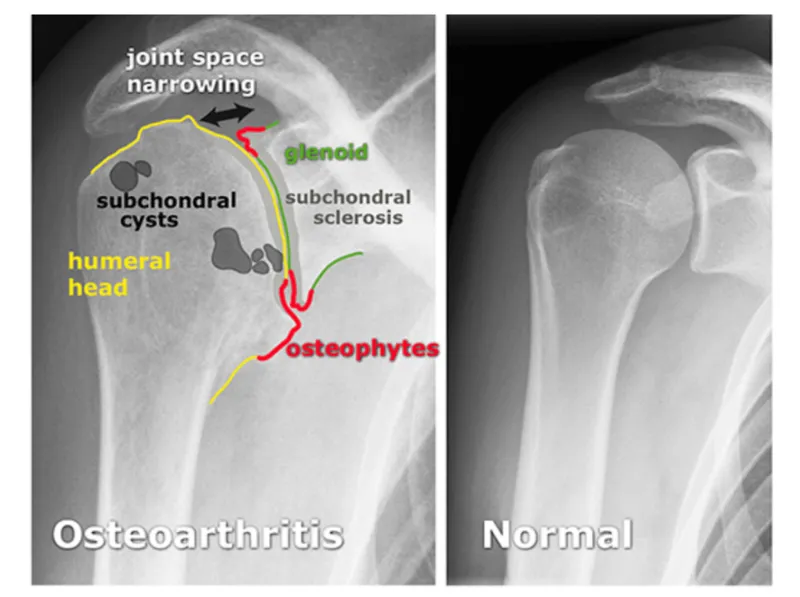
⭐ Axillary view is crucial for assessing glenohumeral joint space narrowing, posterior glenoid erosion, and osteophytes.
OA Shoulder: Management - Easing the Ache
Conservative:
- Patient education, activity modification (e.g. avoiding overhead work).
- Physiotherapy: ROM, strengthening - esp. rotator cuff & deltoid.
- NSAIDs for pain/inflammation.
- Intra-articular injections:
- Corticosteroids: Short-term relief (limit <3-4/year).
- Hyaluronic acid: Variable evidence for benefit.
- PRP: Emerging evidence, research ongoing.
Surgical Intervention: (For failed conservative Rx, persistent pain, functional limitation)
Surgical Options:
- Arthroscopic debridement: Limited role, mainly for mechanical symptoms, temporary relief.
- Hemiarthroplasty: For intact glenoid, functional cuff, younger patients.
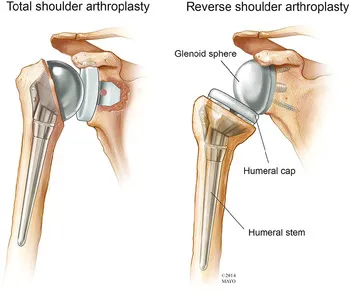
- Total Shoulder Arthroplasty (TSA): Gold standard for intact rotator cuff, good glenoid stock.
- Reverse TSA (rTSA): For cuff tear arthropathy, severe glenoid bone loss, or failed TSA. 📌 Deltoid driven.
⭐ rTSA is preferred in OA with irreparable rotator cuff tears or severe glenoid bone loss, as it biomechanically compensates for cuff deficiency, relying on the deltoid.
High‑Yield Points - ⚡ Biggest Takeaways
- Glenohumeral joint is the most common site for shoulder OA.
- Symptoms: activity-related pain, night pain, progressive stiffness.
- X-ray: joint space narrowing, osteophytes (inferior humeral head - "Goat's beard"), subchondral sclerosis.
- Primary OA is less common than secondary OA (e.g., post-traumatic, cuff tear arthropathy).
- Management: conservative (NSAIDs, physiotherapy) then surgical (arthroplasty).
- Total Shoulder Arthroplasty (TSA) for severe OA with intact rotator cuff.
- Reverse TSA if rotator cuff deficient.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

