Definition & Risk Factors - Knee's Creaky Saga
- Definition: Degenerative joint disease of the knee involving progressive loss of articular cartilage, osteophyte formation, subchondral sclerosis, and synovial inflammation.
- Primary Risk Factors:
- Age (> 50 years): Most significant non-modifiable.
- Female sex (especially post-menopausal).
- Genetic factors.
- Secondary Risk Factors:
- Obesity (BMI > 30).
- Previous knee injury (e.g., meniscectomy, ACL tear).
- Occupational stress (repetitive kneeling, squatting, heavy lifting).
- Joint malalignment (genu varum/valgum).
⭐ Obesity (BMI > 30) is the most significant modifiable risk factor for knee osteoarthritis, increasing load and inflammation.
Pathophysiology - Cartilage Calamity
- Triggers: Mechanical stress, aging, genetics.
- Chondrocyte Role: Dysregulation → ↑Catabolic enzymes (MMPs, ADAMTS), ↓Anabolic factors.
- Pro-inflammatory cytokines (IL-1, TNF-α) amplify damage.
- ECM Failure:
- Proteoglycan loss → ↓hydration, ↓resilience.
- Collagen II network breakdown → fibrillation, erosion.
- Bone Response: Subchondral sclerosis, osteophytes.
- Synovitis: Contributes to pain and progression.
⭐ MMP-13 (Collagenase-3) is a key enzyme responsible for Type II collagen degradation in OA.
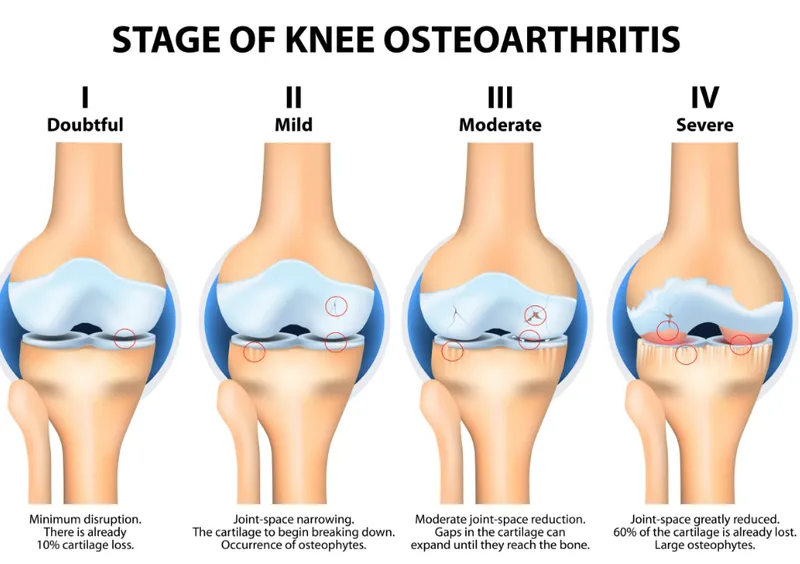
Clinical Features & Diagnosis - Groans & Grades
- Symptoms: Insidious pain (worse with activity, relieved by rest), morning stiffness < 30 min, "gelling" after inactivity, crepitus, joint swelling (cool effusion/bony).
- Signs: Restricted ROM, tenderness, bony enlargement, deformities (varus > valgus).
- Antalgic gait.
- Diagnosis: Primarily clinical.
- X-ray (weight-bearing): Confirms.
- Kellgren-Lawrence (KL) Grades (0-4).
- Key findings: Joint space narrowing (JSN), osteophytes, subchondral sclerosis & cysts. 📌 Mnemonic: LOSS.
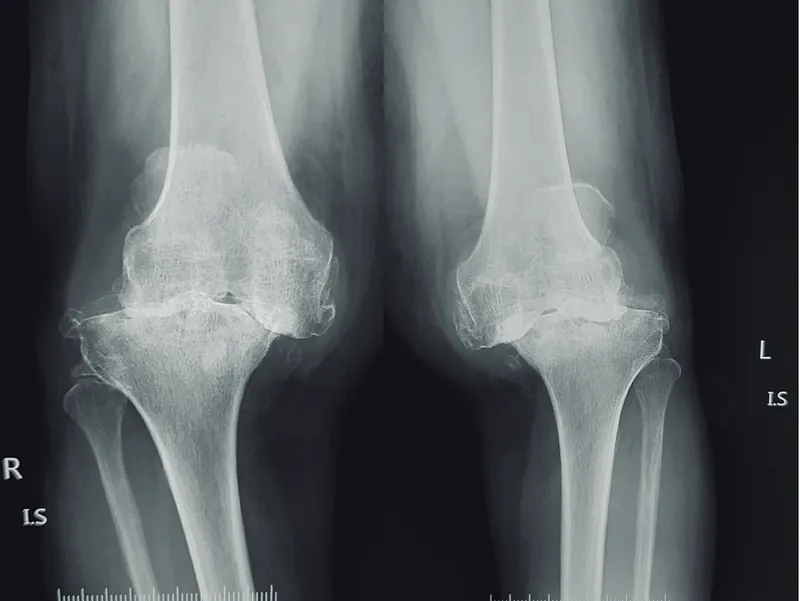
- X-ray (weight-bearing): Confirms.
⭐ Morning stiffness < 30 minutes is a key differentiator from inflammatory arthritis (e.g., Rheumatoid Arthritis).
Imaging - X-Ray Exposé
-
Key Views: Weight-bearing Anteroposterior (AP), Lateral, and Skyline (patellofemoral).
-
📌 LOSS Mnemonic for X-ray findings:
- Loss of joint space (esp. medial compartment)
- Osteophytes (marginal)
- Subchondral sclerosis
- Subchondral cysts
-
Kellgren-Lawrence (K-L) Grading (Grades 0-4):
Grade Description 0 Normal 1 Doubtful joint space narrowing (JSN), possible osteophytes 2 Definite osteophytes, possible JSN 3 Moderate osteophytes, definite JSN, sclerosis, possible deformity 4 Large osteophytes, severe JSN, marked sclerosis, definite deformity
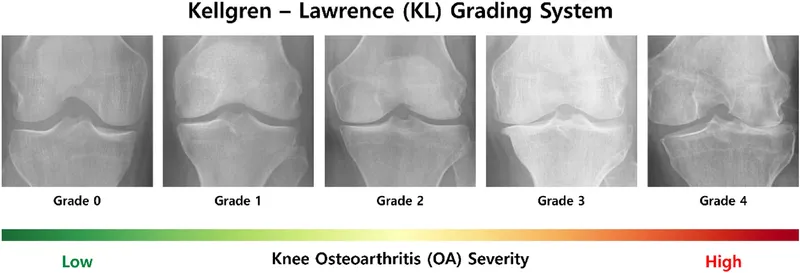
⭐ Weight-bearing AP X-rays are crucial for accurately assessing joint space narrowing, a hallmark of knee OA progression.
Management - Joint Relief Roadmap
- Goals: Pain relief, improve function, improve quality of life.
- Stepwise Approach:
- Conservative Pillars:
- Lifestyle: Weight reduction (5-10% if overweight).
- Physiotherapy: Quadriceps strengthening, ROM exercises, low-impact aerobics.
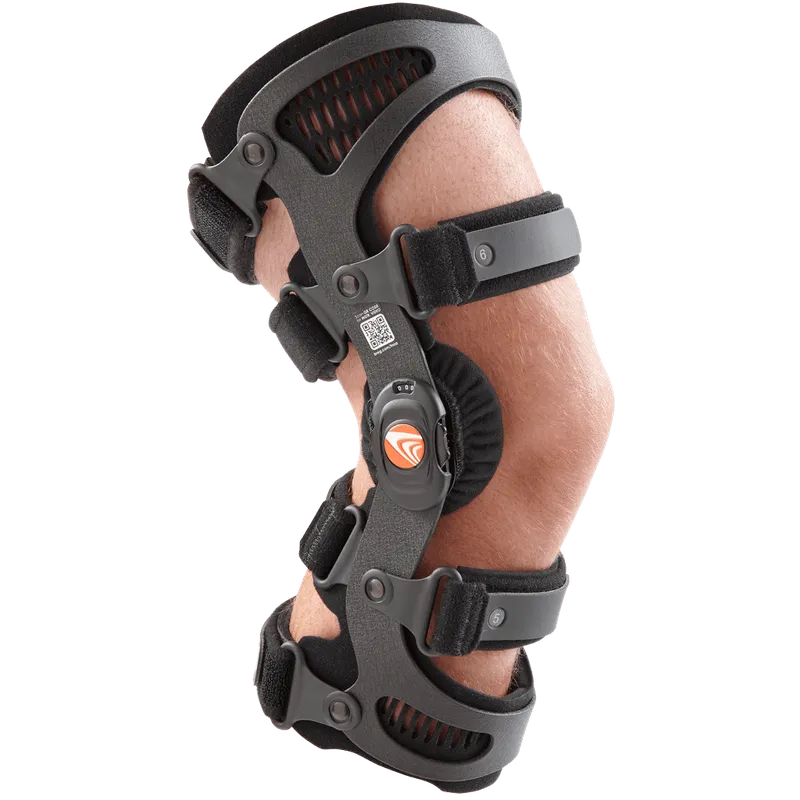
- Aids: Cane (contralateral), valgus knee brace (for medial compartment OA).
- Pharmacotherapy Ladder:
- 1st line: Paracetamol (up to 1g QID, max 4g/day).
- 2nd line: Topical NSAIDs. If ineffective, oral NSAIDs (lowest dose; +PPI if GI risk).
- Intra-articular: Corticosteroids (short-term, max 3-4/year), Hyaluronic acid.
- Surgical Intervention (End-stage):
⭐ High Tibial Osteotomy (HTO) for active patients <60 years with medial unicompartmental OA and varus deformity, aiming to delay TKA.
High‑Yield Points - ⚡ Biggest Takeaways
- Knee is the most common large joint affected by Osteoarthritis (OA).
- Primary OA is idiopathic; Secondary OA results from trauma or pre-existing joint disease.
- Medial compartment involvement is most common, often leading to genu varum.
- Radiographic hallmarks: Joint space narrowing (JSN), osteophytes, subchondral sclerosis, and cysts.
- Key symptoms: Activity-related pain, morning stiffness <30 minutes, crepitus, and decreased range of motion.
- Conservative management: Weight reduction, exercise, NSAIDs; Total Knee Replacement (TKR) for end-stage disease.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

