Introduction - Joint's Slow Grind
- Chronic, progressive degeneration of hip articular cartilage; "wear & tear" arthritis.
- Results in joint pain, stiffness, ↓ function, and ↓ range of motion (ROM).
- Types:
- Primary (Idiopathic): Most common, age-related (typically >50 yrs).
- Secondary: Due to pre-existing conditions (e.g., trauma, Developmental Dysplasia of Hip (DDH), Femoroacetabular Impingement (FAI), Avascular Necrosis (AVN), Perthes disease).
- Key pathology: Cartilage loss, osteophyte formation, subchondral sclerosis.
- Prevalence ↑ with age, obesity, genetics, previous joint injury.
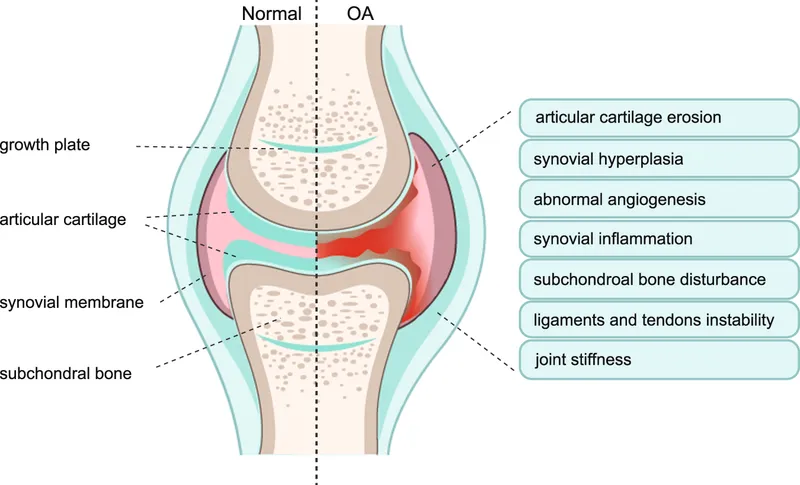
⭐ Osteoarthritis of the hip is the most common form of arthritis affecting this joint, primarily characterized by cartilage degradation and osteophyte formation.
Risk Factors - Pathway to Pain
- Primary (Idiopathic):
- Age >50 years
- Female (post-menopause)
- Genetics
- Obesity (BMI >30): stress, adipokines
- Secondary:
- Trauma (fractures)
- Developmental (DDH, Perthes, SUFE)
- Inflammatory (RA)
- AVN
- Occupational stress
- Pathway: Cartilage loss → bone changes (sclerosis, cysts) → osteophytes → synovitis → pain.
⭐ Previous hip injury significantly increases the risk of developing secondary osteoarthritis.
Clinical Features - Groans & Gaits
- Pain (Groans):
- Insidious onset, deep aching character.
- Location: Groin (commonest, C-sign), anterior thigh, buttock; may refer to knee.
- Worse with activity/weight-bearing, improves with rest.
- "Start-up" pain after inactivity.
- Stiffness:
- Morning stiffness, typically < 30 minutes.
- Gelling phenomenon (stiffness after rest).
- Gait Disturbances (Gaits):
- Antalgic gait (shortened stance phase on affected side).
- Trendelenburg gait (due to abductor weakness, pelvis drops on contralateral side).
- Limp.
- Functional Limitation: Difficulty with ADLs (e.g., stairs, putting on socks/shoes).
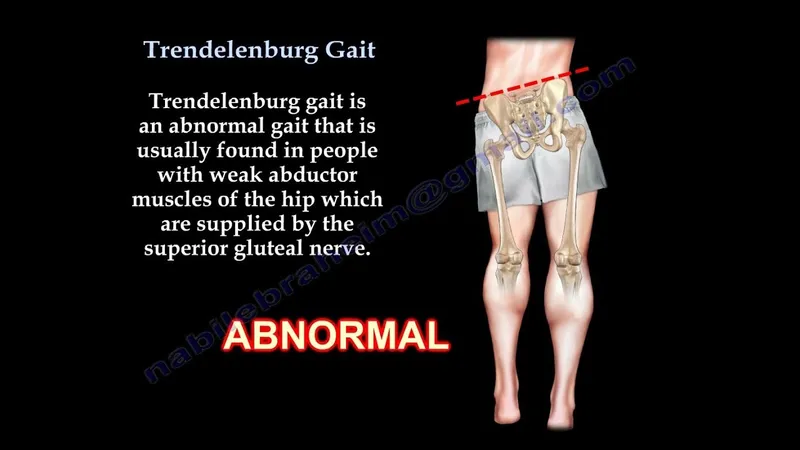
⭐ Restricted and painful internal rotation is often the earliest clinical sign of hip osteoarthritis.
Diagnosis - Imaging Insights
- X-ray (AP pelvis & lateral hip): Initial & primary imaging.
- Hallmark findings (📌 Mnemonic: LOSS):
- Loss of joint space (superior > medial)
- Osteophytes (femoral & acetabular)
- Subchondral sclerosis
- Subchondral cysts
- Hallmark findings (📌 Mnemonic: LOSS):
- Kellgren-Lawrence (KL) Grading: Assesses severity (Grade 0-4).
- Grade 2: Definite osteophytes, possible joint space narrowing (JSN).
- Grade 3: Moderate osteophytes, definite JSN, some sclerosis.
- Grade 4: Large osteophytes, severe JSN, marked sclerosis, cysts.
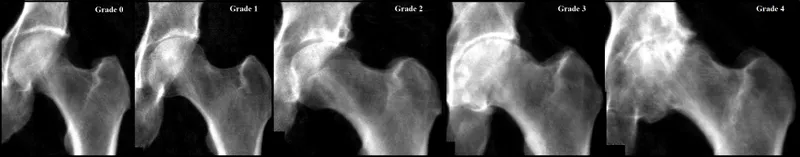
⭐ Earliest sign on X-ray: Osteophytes, often at the femoral head-neck junction or acetabular rim.
- MRI: Not routine; for early changes or when X-ray is normal but suspicion high (cartilage loss, labral tears, bone marrow edema).
Management - Motion Makeover
- Goals: Pain relief, ↑ function, delay progression.
- Conservative:
- Lifestyle: Weight loss (if BMI > 25), activity modification.
- Physiotherapy: Exercises, assistive devices (cane).
- Pharmacological: Paracetamol, NSAIDs, intra-articular corticosteroids/hyaluronic acid.
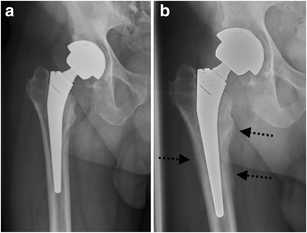
- Surgical Details:
- Total Hip Replacement (THR): Primary choice for advanced OA.
- Osteotomy: Realigns joint; for younger patients.
⭐ Total Hip Replacement (THR) is one of the most successful and cost-effective surgical interventions in medicine.
High‑Yield Points - ⚡ Biggest Takeaways
- Groin/anterior thigh pain, worse with activity, is characteristic of hip OA.
- Loss of internal rotation is an early and significant clinical sign.
- Radiographs reveal superolateral joint space narrowing, osteophytes, and subchondral sclerosis/cysts.
- Morning stiffness is typically brief, lasting < 30 minutes.
- Trendelenburg gait may be present due to abductor muscle weakness or pain.
- Total Hip Arthroplasty (THA) is the definitive surgical treatment for advanced, debilitating disease.
- Major risk factors include advanced age, obesity, and prior hip joint injury or disease.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

