Overview of Degeneration - Wear & Tear Tales
- Progressive, age-related structural failure from chronic biomechanical stress ("wear & tear").
- Key targets: Intervertebral discs (IVD), facet joints, vertebral endplates, ligaments.
- Pathophysiology Highlights:
- IVD: Initial ↓proteoglycans & water (nucleus pulposus) → ↓disc height, desiccation → annular tears, fissures → herniation.
- Facet Joints (Zygapophyseal): Cartilage erosion → inflammation → osteophyte formation (spondylosis) → arthropathy, hypertrophy.
- Ligaments: Hypertrophy (esp. ligamentum flavum), ossification.
- Clinical Sequelae: Segmental instability, nerve root impingement (radiculopathy), spinal stenosis, myelopathy, chronic axial pain.
⭐ Most common initial change in degenerative disc disease is loss of proteoglycans and water content in the nucleus pulposus.
Cervical Spondylosis - Cranky Neck Crisis
- Degenerative cascade affecting cervical discs, vertebrae, facet joints.
- Pathophysiology: Disc desiccation & collapse → osteophytes → ↓canal/foraminal space.
- Clinical Syndromes:
- Axial Neck Pain: Chronic, activity-related.
- Cervical Radiculopathy: Unilateral arm pain, paresthesia, weakness. Positive Spurling's test.
- Cervical Myelopathy: Insidious onset. Gait disturbance (spastic), clumsiness, Lhermitte's sign, Hoffman's sign. Bowel/bladder changes late.
- Diagnosis:
- X-ray: ↓Disc height, osteophytes, foraminal narrowing.
- MRI: Definitive for neural compression.

- Management:
- Conservative: NSAIDs, physiotherapy, cervical collar.
- Surgical: Decompression (ACDF, laminectomy) for progressive myelopathy or failed conservative Rx for radiculopathy.
⭐ Nurick scale is commonly used to grade the severity of cervical spondylotic myelopathy.
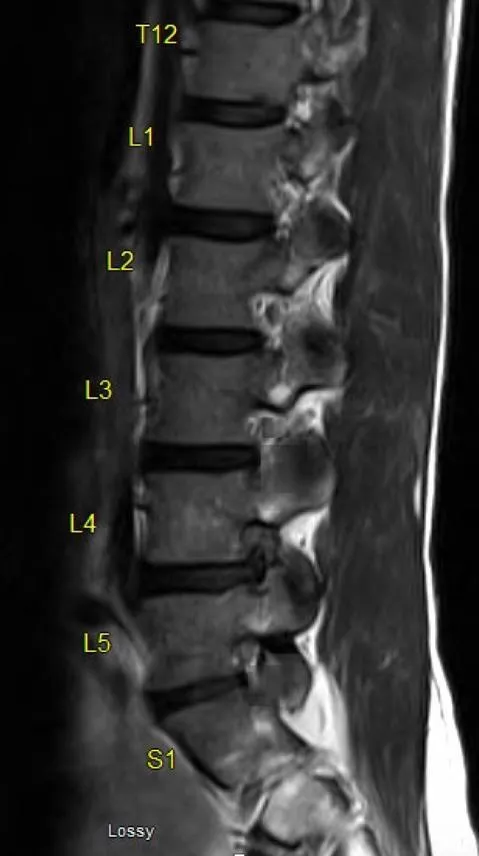
Lumbar Degeneration - Low Back Breakdown
- Core Issues: Age-related wear & tear of lumbar discs, facets, ligaments. Leads to Low Back Pain (LBP), radiculopathy (e.g., sciatica), and/or neurogenic claudication.
- Key Conditions:
- Disc Herniation: Nucleus pulposus extrusion. Common at L4-L5, L5-S1. Positive Straight Leg Raise (SLR).
- Lumbar Spinal Stenosis (LSS): Central canal or foraminal narrowing.
- Degenerative Spondylolisthesis: Anterior vertebral slippage, often L4-L5.
- Diagnosis: History, neuro exam. X-ray (osteophytes, ↓disc height). MRI is gold standard.
⭐ The "shopping cart sign" (symptoms improve with leaning forward) is characteristic of lumbar spinal stenosis.
- Management Approach:
Clinical Approach - Spine Sleuth & Fix
- History: Focus on red flags (📌 PINNT: Progressive deficit, Incontinence, Night pain/fever/weight loss, Numbness/weakness (new/progressive), Trauma). Pain: onset, character, radiation, aggravating/relieving factors.
- Exam:
- Observe: Gait, deformity (scoliosis, kyphosis).
- Palpate: Tenderness.
- Assess: ROM.
- Neuro: Motor (power 0-5), Sensory (dermatomes), Reflexes. Special tests (SLR, Lasegue's, Femoral stretch, Spurling's).
- Investigations:
- X-ray: Initial (AP/Lat), dynamic views for instability.
- MRI: Gold standard for discs, nerves, cord.
- CT: For bony detail, fractures, severe stenosis.
- Management Principles:
- Conservative: Rest, analgesia (NSAIDs), physiotherapy, epidural injections.
- Surgical: Indications: progressive neuro deficit, intractable pain, instability, failure of conservative Rx.
⭐ Cauda equina syndrome is a surgical emergency requiring urgent decompression.

High‑Yield Points - ⚡ Biggest Takeaways
- Lumbar spondylosis is most common, affecting L4-L5 & L5-S1 levels.
- Cervical spondylosis presents with radiculopathy (nerve root) or myelopathy (cord compression).
- Neurogenic claudication, relieved by flexion, is key for lumbar spinal stenosis.
- MRI is the gold standard for diagnosis and assessing severity.
- Conservative management (rest, NSAIDs, physiotherapy) is the initial approach.
- Surgical decompression is for progressive neurological deficits or intractable pain.
- Degenerative spondylolisthesis commonly occurs at L4-L5.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more


