Robotic Surgery in Orthopaedics - Precision Pioneers
- Definition: Use of robotic systems to enhance surgeon's ability during orthopaedic procedures.
- Goals: ↑Precision, ↑Accuracy, ↑Safety, ↓Invasiveness, ↓Radiation exposure, improved implant positioning & patient outcomes.
- Components:
- Robotic arm: Executes surgical tasks.
- Computer console: Surgeon interface, pre-operative planning.
- Tracking system: Monitors patient & instrument position.
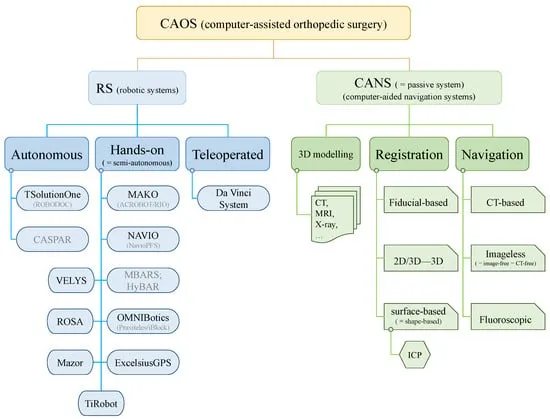
- Types:
- Active: Robot performs pre-programmed tasks (e.g., ROBODOC).
- Semi-active: Surgeon guides robot, robot provides haptic feedback & defines safe zones (e.g., MAKO, NAVIO).
- Passive: Robot holds/positions instruments/endoscopes (e.g., AESOP).
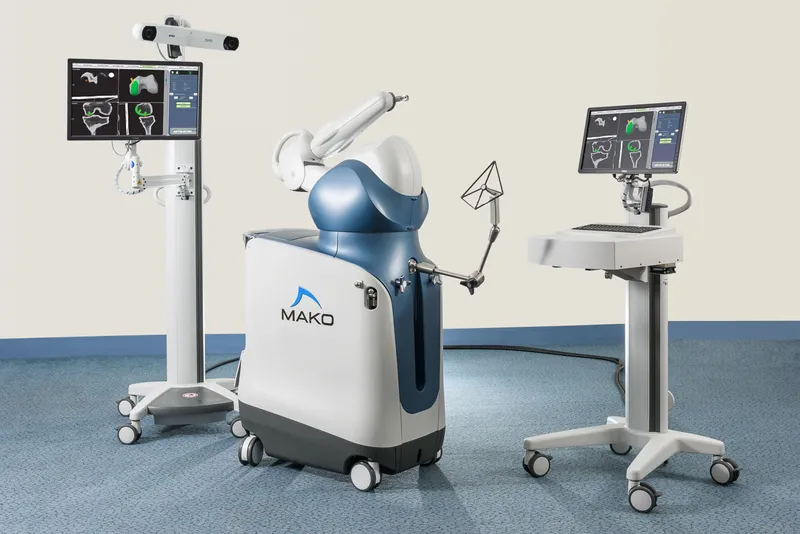
⭐ Robotic assistance in unicompartmental knee arthroplasty (UKA) has shown superior accuracy in component positioning compared to conventional techniques.
- Benefits: Precise bone cuts, optimal implant alignment, potentially faster recovery, reduced outliers.
- Limitations: High cost, steep learning curve, increased operative time initially, specialized training required.
- Applications: Total Knee Arthroplasty (TKA), Total Hip Arthroplasty (THA), UKA, Spine surgery, Trauma (pelvic fracture fixation).
Robotic Surgery in Orthopaedics - The Bot Brigade
- Robotic System Types:
- Active: Robot autonomously executes pre-programmed surgical tasks (e.g., ROBODOC).
- Passive: Surgeon directly controls robot; system offers enhanced stability/navigational guidance (e.g., Navio). Haptic feedback.
- Semi-active (Shared Control): Surgeon leads, robot provides haptic boundaries, constraining actions to safe zones (e.g., MAKO, ROSA).
- Key Components:
- Robotic arm: Holds & manipulates surgical tools.
- Navigation system: Tracks patient anatomy & instruments (optical/EM).
- Computer console: For pre-operative planning and intra-operative control.
⭐ MAKO system (semi-active) for arthroplasty enhances surgeon's control with haptic feedback, improving implant positioning accuracy and potentially reducing revision rates.
Robotic Surgery in Orthopaedics - Bots in Action
Error generating content for this concept group: Failed to process successful response
Robotic Surgery in Orthopaedics - Edge & Hurdles
- Edge (Advantages):
- ↑ Precision & accuracy: component placement, limb alignment (THA, TKA).
- ↓ Intra-op errors & outliers.
- Reduced soft tissue trauma, ↓ blood loss.
- Potential for ↑ implant survivorship & better functional outcomes.
- Advanced pre-operative 3D planning.
- Hurdles (Disadvantages & Challenges):
- High acquisition & maintenance costs.
- Steep learning curve for surgeons & staff.
- ↑ Initial operative duration.
- Specific complications: pin-tract issues, neurovascular injury.
- Radiation exposure (fluoroscopy-based systems).
- Lack of haptic feedback (some systems).
- Limited long-term data for all applications.
⭐ Robotic systems significantly improve acetabular cup inclination and anteversion accuracy in THA, aiming to ↓ dislocation rates.
High‑Yield Points - ⚡ Biggest Takeaways
- Robotic surgery boosts precision and accuracy in implant placement (e.g., TKA, THA).
- Types: Active (autonomous), Semi-active (haptic-guided, e.g., MAKO), Passive (navigation).
- Reduces alignment outliers, potentially improving implant longevity and function.
- May decrease soft tissue trauma, blood loss, and enable faster recovery.
- Relies on preoperative CT/MRI for 3D planning and precise execution.
- Limitations: High cost, steep learning curve, and initial longer operative times.
- Widely used in knee/hip arthroplasty and spine surgery.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

