Amputation: Indications & Planning - Chopping Block Choices
- Absolute Indications: Uncontrolled tumor (infection, fungation); pathological fracture with extensive soft tissue involvement; neurovascular encasement making salvage impossible; recurrence post-limb salvage.
- Relative Indications: Poor patient compliance for salvage protocols; extensive bone loss requiring complex reconstruction; patient preference.
- Pre-operative Evaluation:
- Biopsy: Crucial; longitudinal incision, avoid neurovascular bundles & tumor contamination.
- Staging: TNM, Enneking (📌 GTM: Grade, Tumor site, Metastasis).
- Imaging: MRI (local extent, NV involvement), CT Chest (metastasis).
- Functional & psychological assessment.
⭐ Contraindications to limb salvage surgery often include major neurovascular involvement, extensive muscle infiltration, or pathological fracture through a tumor with significant soft tissue contamination.
Amputation: Levels & Principles - Surgical Slice Savvy
- Oncologic Principles:
- Wide margins: 3-5 cm healthy tissue. Crucial to prevent local recurrence; avoid tumor breach.
- No-touch technique: Minimize tumor cell seeding during surgery.
- Neurovascular bundle: Careful dissection; ligate vessels, nerves gently pulled, transected cleanly to retract.
- Stump quality: Myodesis (muscle-to-bone) or myoplasty (muscle-to-muscle/fascia) for optimal prosthetic fit & function, reducing pain.
⭐ Myodesis, anchoring muscle to bone, is crucial for a functional stump, improving prosthetic control and reducing muscle atrophy.
- Common Amputation Levels (Bone Tumors):
- Upper Limb:
- Forequarter: For extensive shoulder girdle tumors (e.g., scapula, clavicle).
- Shoulder Disarticulation: For proximal humerus tumors.
- Lower Limb:
- Hemipelvectomy/Hip Disarticulation: For large pelvic or proximal femur tumors.
- Above-Knee (AK/Transfemoral): For femur or proximal tibia tumors.
- Below-Knee (BK/Transtibial): For tibia/fibula tumors; knee preservation is key for function.
- Syme's: Ankle disarticulation for distal tibia/foot tumors; creates an end-bearing stump.
- Upper Limb:

Amputation: Complications & Care - Post-Op Pitfalls
Early Complications:
- Hematoma, Infection: Prompt drainage; targeted antibiotics.
- Wound Dehiscence, Flap Necrosis: Surgical debridement & revision.
- DVT/PE: Crucial prophylaxis (LMWH); early mobilization.
- Acute Stump Pain: Multimodal analgesia.
Late Complications:
- Phantom Limb Pain: Management: analgesics (gabapentin, amitriptyline), mirror therapy, TENS.
- Neuroma Formation: Painful nerve end. Local injections, surgical excision, TMR.
- Stump Skin Problems (ulcers, dermatitis): Daily hygiene, proper socket fit, skin care.
- Joint Contractures: Regular physiotherapy, correct positioning.
- Psychological Sequelae (depression, anxiety): Counseling, peer support.
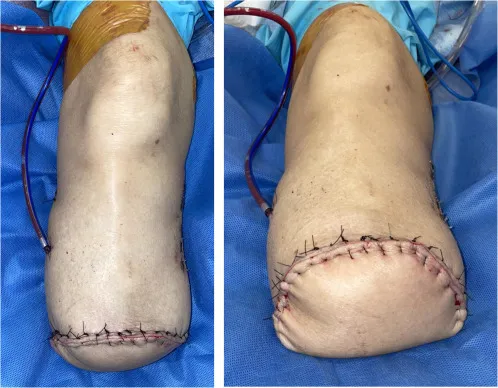
⭐ Phantom limb pain is experienced by a majority of amputees and requires a proactive, multimodal management approach, distinct from phantom limb sensation.
Amputation: Rehab & Results - Life After Limb Loss
- Multidisciplinary Team (MDT): Crucial for holistic care. Includes surgeon, physiatrist, physiotherapist, occupational therapist, prosthetist, psychologist.
- Rehabilitation Pathway: A phased approach.
- Factors Influencing Outcome & Prosthetic Success:
- Level of amputation (energy expenditure varies)
- Stump quality: well-shaped, pain-free, good soft tissue
- Patient motivation & active participation
- Comorbidities (e.g., diabetes, peripheral vascular disease)
- Prosthetic design, fit, and alignment
- Psychosocial Support: Essential for adjustment to limb loss, body image, and Quality of Life (QoL); peer support groups.
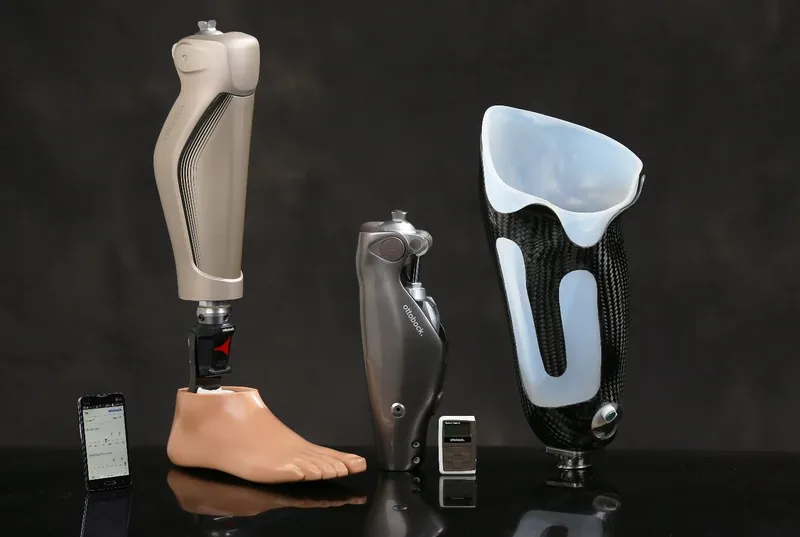
⭐ Early mobilization and a well-fitted prosthesis, combined with strong patient motivation, are key determinants of successful rehabilitation after amputation for bone tumors.
High‑Yield Points - ⚡ Biggest Takeaways
- Amputation for bone tumors: a salvage procedure when limb preservation fails or is contraindicated.
- Key indications: locally advanced unresectable tumors, neurovascular encasement, severe pathological fractures, infection post-salvage.
- Wide surgical margins are crucial for oncologic control and minimizing local recurrence.
- Phantom limb pain is a frequent challenge; requires multimodal management.
- Early rehabilitation and prosthetic fitting are essential for optimal functional outcome.
- Skip metastases can influence the level of amputation required for complete tumor eradication.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

