Vascularized Bone Grafts - Living Scaffolds
Vascularized Bone Grafts (VBGs) are segments of bone transferred with their intrinsic blood supply, ensuring immediate viability.
- Principles:
- Osteogenesis: Direct bone formation by viable osteoblasts.
- Osteoinduction: Stimulates host cells to form bone.
- Osteoconduction: Provides scaffold for new bone growth.
- Rapid incorporation & healing.
- Potential for hypertrophy under load.
- Comparison with Non-Vascularized Bone Grafts (NVBGs):
- VBGs: Living tissue, faster union, ↓ resorption, better in compromised beds.
- NVBGs: Rely on host bed for revascularization (creeping substitution), slower union, ↑ resorption.
⭐ Vascularized grafts heal by primary osteonal bone union, not creeping substitution.
Vascularized Bone Grafts - Donor Site Deep Dive
Donor sites: Fibula, Iliac Crest, Rib, Scapula, Radius. Each has unique vessels & bone.
| Site | Vessels | Bone (L/Type) | Pedicle (cm) | Uses | Morbidity |
|---|---|---|---|---|---|
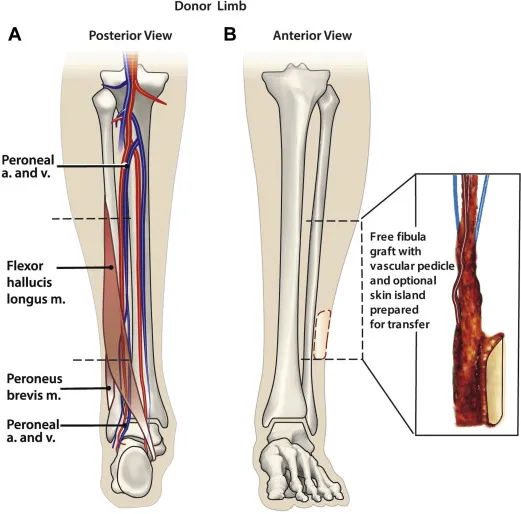
| Fibula | Peroneal a.v. | Cortical, ~20-25 cm | 4-8 | Long bones, mandible | Ankle, sensory loss |
| Iliac Crest | DCIA a.v. | Corticocancellous, curved | 5-7 | Pelvis, mandible | Hernia, gait |
| Rib | Post. Intercostal a.v. | Corticocancellous, pliable | 6-12 | Chest wall, mandible | Pneumothorax, pain |
| Scapula | Circumflex Scapular a.v. | Cortical, thin | 6-8 | Maxillofacial | Shoulder stiff |
| Radius | Radial a. (palm. carp.) & v. | Corticocancellous, small | 2-3 | Scaphoid, small defects | ↓ Grip, fracture |
⭐ Free fibula: workhorse for long bone defects (length, straightness, robust periosteal supply).
Vascularized Bone Grafts - Prime Time Uses
Key indications for using vascularized bone grafts (VBGs) include:
- Large segmental bone defects (typically >6-8 cm)
- Avascular necrosis (AVN), especially of the femoral head or scaphoid
- Recalcitrant nonunions, particularly if infected
- Reconstruction after malignant tumor resection
- Congenital pseudarthrosis of the tibia
⭐ Vascularized fibular graft is a workhorse for long bone defects; iliac crest graft (based on deep circumflex iliac artery - DCIA) is common for scaphoid AVN or jaw reconstruction.
Vascularized Bone Grafts - Balancing Act
| Advantages | Disadvantages |
|---|---|
| * Maintains bone viability | * Technically demanding (microvascular skills) |
| * Resists infection effectively | * Longer operative time |
| * Rapid union, early healing | * Donor site morbidity (pain, nerve injury) |
| * Hypertrophy potential | * Potential flap failure (e.g., thrombosis) |
| * Useful in compromised beds | * Limited availability & donor sites |
Vascularized Bone Grafts - Trouble Shooters
- Early Complications:
- Vascular thrombosis (arterial/venous)
- Hematoma
- Infection
- Late Complications:
- Nonunion, delayed union
- Graft fracture
- Donor site: stress fracture, nerve injury
⭐ Venous thrombosis is more common than arterial thrombosis in free vascularized bone flaps.
High‑Yield Points - ⚡ Biggest Takeaways
- Vascularized bone grafts (VBGs) maintain viability and osteogenic potential, promoting rapid healing and hypertrophy.
- Key indications include large segmental defects (>6-8 cm), avascular necrosis (AVN), infected nonunions, and reconstruction in irradiated beds.
- The free fibula is the most common donor site, valued for its length, strength, and potential for osteocutaneous flaps.
- Successful VBGs require meticulous microvascular anastomosis to ensure graft survival.
- VBGs undergo direct osteointegration and primary union, largely bypassing creeping substitution.
- Offer superior resistance to infection and faster incorporation compared to non-vascularized grafts.
- Potential complications: anastomotic failure, donor site morbidity, and stress fracture of the graft.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

