Tissue Engineering in Orthopaedics - Ortho's Bio‑Builders
- Definition: An interdisciplinary field applying life sciences & engineering principles to develop biological substitutes that restore, maintain, or improve tissue function.
- Goals: Promote regeneration & repair of musculoskeletal tissues (bone, cartilage, ligaments, tendons).
- Core Triad: 📌 CSS for success!
- Cells (e.g., osteoblasts, chondrocytes, stem cells)
- Scaffolds (biomaterials providing structural support & promoting cell attachment/growth)
- Signals (e.g., growth factors like BMPs, TGF-β; mechanical stimuli)
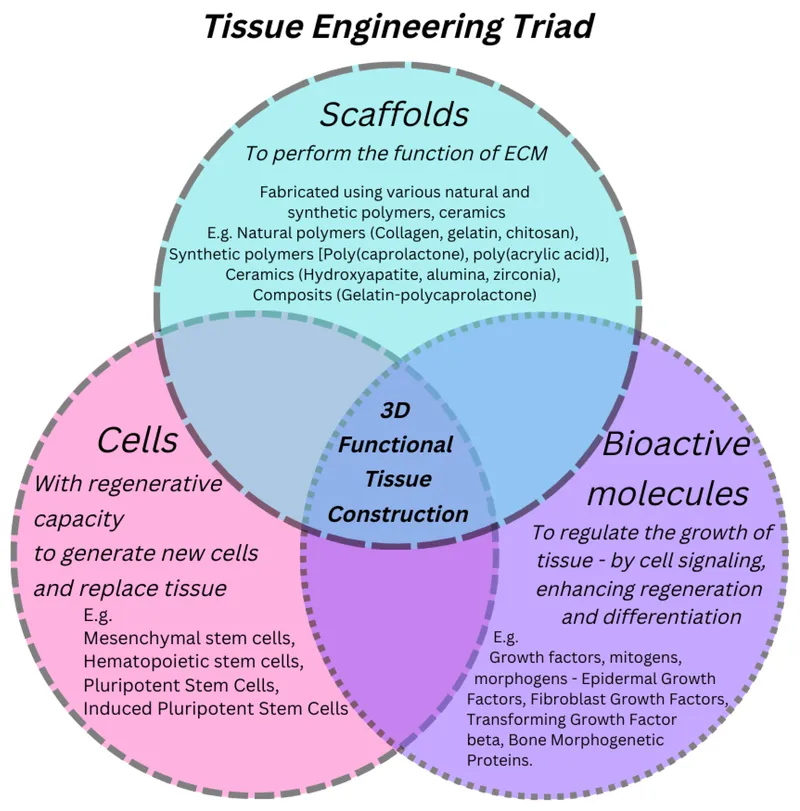
⭐ The 'Diamond Concept' in bone healing (osteogenic cells, osteoinductive signals, osteoconductive scaffold, mechanical stability, and vascularization) is an expansion of the basic triad for optimal bone formation and repair an exam favourite for NEET PG orthopaedics questions on bone grafts and substitutes, particularly tissue engineering principles..
Cells in Ortho TE - The Living Legos
| Cell Type | Source(s) | Potency | Key Pro(s) | Key Con(s) |
|---|---|---|---|---|
| MSCs | Autologous (marrow, adipose), Allogeneic | Multipotent | Immunomodulatory, osteo/chondro potential | Morbidity (auto), rejection (allo), senescence |
| Chondrocytes | Autologous, Allogeneic | Unipotent | Cartilage-specific | Dedifferentiation, limited proliferation, morbidity (auto) |
| Osteoblasts | Autologous (bone) | Unipotent | Direct bone formation | Limited supply, expansion difficulty |
| iPSCs | Reprogrammed somatic cells (Auto) | Pluripotent | Patient-specific, unlimited supply, versatile | Teratoma risk, complex culture, ethical |
⭐ Mesenchymal Stem Cells (MSCs) are the most commonly investigated cell type for orthopaedic tissue engineering due to their multipotency and availability.
Scaffolds in Ortho TE - The 3D Frameworks
Scaffolds are 3D porous biomaterials guiding tissue regeneration.
- Ideal Properties (📌 BPM-POS):
- Biocompatible & Biodegradable (controlled rate)
- Porosity (interconnected, optimal: 100-400 µm for vascularization & bone ingrowth)
- Mechanical strength (matching host tissue)
- Osteoconductive, Osteoinductive
- Surface chemistry (promotes cell adhesion, proliferation, differentiation)
- Materials:
- Natural: Collagen, Hyaluronic acid, Alginate, Chitosan.
- Synthetic: PLLA, PGA, PLGA, PCL, Bioactive glasses, Calcium phosphates (HA, TCP).
- Fabrication: 3D printing, electrospinning, solvent casting.
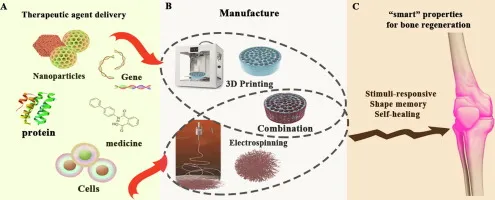
⭐ Hydroxyapatite (HA) is a widely used osteoconductive ceramic material due to its chemical similarity to natural bone mineral.
Growth Factors in Ortho TE - Molecular Messengers
Growth factors are pivotal signaling molecules in tissue engineering, orchestrating cellular responses.
- Role: Stimulate cell proliferation, differentiation, and migration.
- Key Examples & Primary Functions:
- Bone Morphogenetic Proteins (BMPs): Osteoinduction (e.g., BMP-2, BMP-7).
- Transforming Growth Factor-beta (TGF-β): Chondrogenesis, matrix synthesis.
- Platelet-Derived Growth Factor (PDGF): Angiogenesis, cell recruitment.
- Vascular Endothelial Growth Factor (VEGF): Angiogenesis, vascularization.
- Fibroblast Growth Factors (FGFs): Angiogenesis, mitogenesis.
- Delivery Systems: Direct incorporation into scaffolds, controlled release mechanisms, gene therapy.
⭐ Recombinant human BMP-2 (Infuse®) and BMP-7 (Osigraft®) are FDA-approved for specific orthopaedic applications like spinal fusion and tibial non-unions.
Clinical Applications of Ortho TE - Healing Horizons
- Key Applications:
- Bone regeneration: Addressing non-unions, critical-sized defects.
- Cartilage repair: Utilizing techniques like ACI (Autologous Chondrocyte Implantation), MACI.
- Ligament/Tendon engineering.
- Intervertebral disc (IVD) regeneration strategies.
- Major Challenges:
- Vascularizing large constructs, potential immune responses, high costs, complex regulatory pathways, and effective bench-to-bedside clinical translation.
- Future Directions:
- 3D bioprinting of complex tissues, smart biomaterials responsive to physiological cues, advanced gene delivery techniques, personalized medicine approaches.
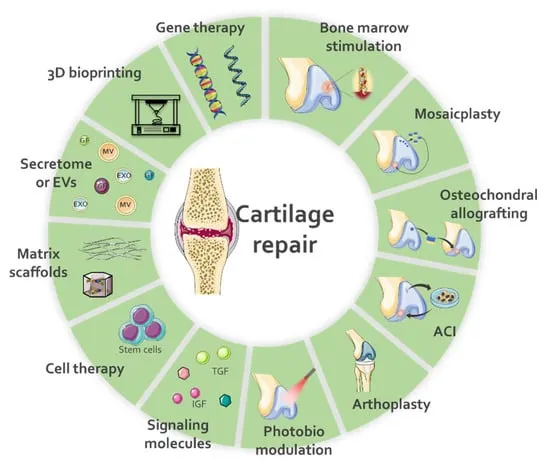
⭐ Autologous Chondrocyte Implantation (ACI) is an established cell-based therapy for treating symptomatic, focal chondral defects of the knee, particularly for lesions >2 cm² in younger patients with high functional demands.
High‑Yield Points - ⚡ Biggest Takeaways
- Tissue Engineering Triad: Cells (MSCs), Scaffolds (biocompatible, biodegradable), Growth Factors (BMPs).
- Mesenchymal Stem Cells (MSCs): Multipotent; sourced from bone marrow, adipose.
- Scaffolds: Provide 3D support; natural (collagen) or synthetic (PLLA, PGA).
- Growth Factors: BMP-2, BMP-7 FDA-approved for specific bone uses.
- Aim: Regenerate functional tissues like bone, cartilage, tendons/ligaments.
- Key Challenges: Vascularization, host tissue integration, cost.
- Applications: Non-unions, cartilage defects, osteonecrosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

