GF Basics & Cascade - Healing Signals
- Growth Factors (GFs): Polypeptide signaling molecules essential for bone regeneration.
- Source: Released from platelets, inflammatory cells (macrophages), osteoprogenitor cells, and bone matrix.
- Action: Bind to specific cell surface receptors, activating intracellular pathways for repair.
- Healing Cascade: A precisely orchestrated sequence of GF release and cellular responses.
- Key Cellular Events: Chemotaxis (recruitment), mitogenesis (proliferation), angiogenesis (vascularization), differentiation (osteogenic lineage), and matrix synthesis (osteoid production).
⭐ Growth factors are polypeptide signaling molecules crucial for cell proliferation, differentiation, and matrix synthesis during bone repair.
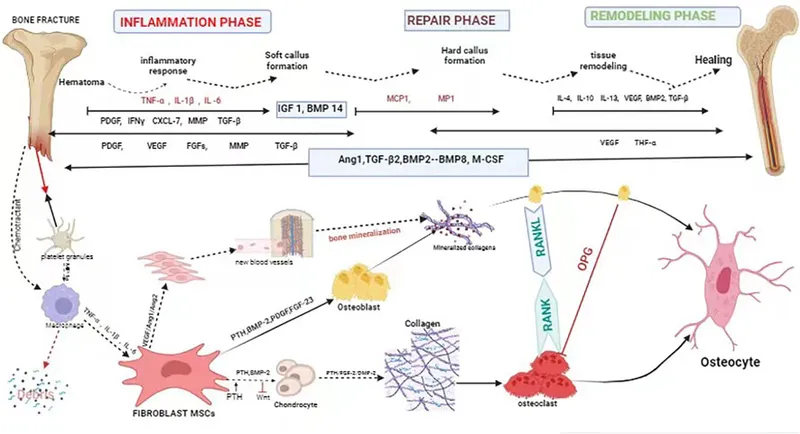
Key Players: The GF Lineup - Bone's Best Buds
Several key growth factors orchestrate the complex process of bone healing, each playing a specific role:
| Growth Factor (GF) | Source | Receptor | Key Bone Healing Function(s) | Mnemonic 📌 |
|---|---|---|---|---|
| BMPs | Osteoprogenitors, osteoblasts, platelets | BMPRs (Serine/Threonine Kinase) | Osteoinduction (MSC differentiation to osteoblasts), chondrogenesis. Most potent osteoinductive GFs. | Bone Makers Potent! |
| PDGF | Platelets, macrophages, osteoblasts | PDGFR (Tyrosine Kinase) | Potent mitogen (MSCs, osteoblasts), promotes angiogenesis & chemotaxis for repair cells. | Promotes Division & Growth. |
| TGF-β | Platelets, bone matrix, osteoblasts | TGF-βR (Serine/Threonine Kinase) | Stimulates MSC proliferation & differentiation to osteoblasts, ↑ECM (collagen I) synthesis, ↓osteoclast activity. | Transforms & Grows Fibrous βone. |
| FGFs | Osteoblasts, chondrocytes, MSCs | FGFRs (Tyrosine Kinase) | Key angiogenic factor, promotes MSC & osteoblast proliferation, chondrocyte proliferation & differentiation. | Fast Growth of Fibroblasts. |
| VEGF | Endothelial cells, osteoblasts, MSCs | VEGFRs (Tyrosine Kinase) | Critical for angiogenesis & neovascularization, endothelial cell proliferation/migration, supports osteoblast differentiation. | Vascular Enhancement Great For healing. |
Clinical Use & Future - Bench to Bedside
- FDA-Approved GFs:
- rhBMP-2 (Infuse®): Spinal fusion, open tibial fractures. Dose: 1.5 mg/mL with ACS.
- rhBMP-7 (OP-1®): Tibial non-unions, revision spinal fusion.
⭐ Recombinant human BMP-2 (Infuse®) and BMP-7 (OP-1®) are FDA-approved for specific applications like spinal fusion and tibial non-unions, but their use requires careful consideration of cost and potential side effects (e.g., heterotopic ossification, seroma).
- Delivery Systems:
- Carriers: Absorbable Collagen Sponge (ACS), ceramics, polymers.
- Function: Localize GFs, control release.
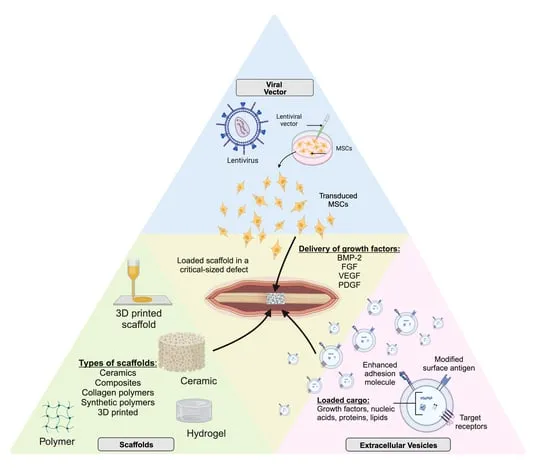
- Clinical Applications:
- Non-unions (long bones).
- Spinal arthrodesis.
- Critical-sized bone defects.
- Limitations & Concerns:
- High cost.
- ⚠️ Side Effects: Heterotopic ossification (HO), seroma, inflammation.
- Contraindications: Skeletal immaturity, infection, tumor site.
- Future Directions:
- Novel GFs (GDF-5, FGF, PDGF).
- Gene therapy.
- Smart biomaterials (controlled release).
- Combination therapies (GFs + cells).
High‑Yield Points - ⚡ Biggest Takeaways
- BMPs (BMP-2, BMP-7) are powerful osteoinductive agents, crucial for new bone.
- PDGF boosts angiogenesis and mesenchymal cell proliferation at fracture sites.
- VEGF is essential for vascularization, enabling nutrient delivery for bone repair.
- TGF-β stimulates matrix production and recruits mesenchymal cells.
- FGFs enhance angiogenesis, osteoblast and chondrocyte activity.
- Growth factors signal through specific cell surface receptors to drive healing.
- Key uses: non-unions, spinal fusion, improving graft incorporation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

