Composite Grafts - Mix & Match Miracles
- Definition: Combinations of ≥2 graft materials (autograft, allograft, xenograft, synthetic).
- Goal: Capitalize on strengths of each component; overcome individual limitations.
- Provides optimal mix of: osteoconduction, osteoinduction, osteogenesis.
- Common Combinations:
- Autograft + Allograft: ↑ volume, ↓ donor site morbidity.
- DBM + Ceramics (HA/β-TCP): Osteoinductive + osteoconductive scaffold.
- Synthetic scaffold + Growth Factors (e.g., BMP-2, BMP-7).
- Cell-seeded matrices (e.g., MSCs on ceramic).

⭐ Composite grafts aim to provide the "diamond concept" of bone healing: scaffold, cells, growth factors, and mechanical stability (often addressed by fixation).
Building Blocks - The Perfect Blend
Composite grafts synergistically combine materials, aiming to fulfill the "diamond concept" of bone healing by providing all three essential elements.
- Definition: Grafts uniting ≥2 distinct materials or tissue types to enhance bone regeneration.
- The Ideal Mix (Diamond Concept) 💎:
- Osteoconductive Scaffold: Structural framework for cell attachment & ingrowth. E.g., allograft, ceramics (Hydroxyapatite, Tricalcium Phosphate), collagen.
- Osteoinductive Signals: Growth factors stimulating osteoprogenitor cell differentiation. E.g., Bone Morphogenetic Proteins (BMPs), Demineralized Bone Matrix (DBM).
- Osteogenic Cells: Viable cells capable of forming new bone. E.g., Bone Marrow Aspirate (BMA), autograft chips, Mesenchymal Stem Cells (MSCs).
- Common Combinations:
- DBM + BMA
- Allograft + BMA/BMPs
- Synthetic scaffold + Cells (e.g., BMA)
- Advantage: Overcomes limitations of single-component grafts by addressing multiple biological pathways for more robust bone formation.
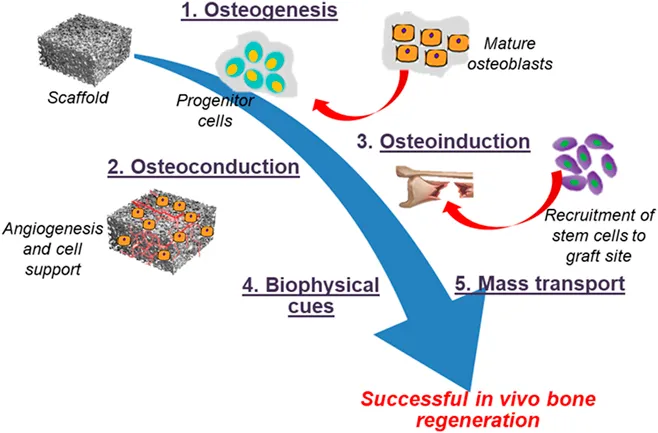
⭐ DBM provides osteoinductive signals and some osteoconductive properties, but lacks osteogenic cells; adding BMA (Bone Marrow Aspirate) completes the triad for effective bone healing (osteogenic, osteoinductive, osteoconductive).
Clinical Showcase - Healing Heroes
- Spinal Fusion Procedures:
- Enhancing interbody fusion: Cages filled with Demineralized Bone Matrix (DBM) & ceramic granules (e.g., Hydroxyapatite/Tricalcium Phosphate).
- Augmenting posterolateral fusion: Local autograft combined with allograft chips or synthetic extenders.
- Trauma & Non-union Management:
- Bridging segmental bone defects: Synthetic scaffolds (e.g., calcium phosphate cements) fortified with Bone Morphogenetic Proteins (BMPs).
- Treating atrophic non-unions: DBM or Platelet-Rich Plasma (PRP) combined with cancellous autograft/allograft.
- Reconstructive Orthopaedics:
- Filling voids after tumor resection: Allograft struts combined with DBM putty or synthetic bone substitutes.
- Periprosthetic fracture stabilization: Cement-antibiotic-allograft composites.
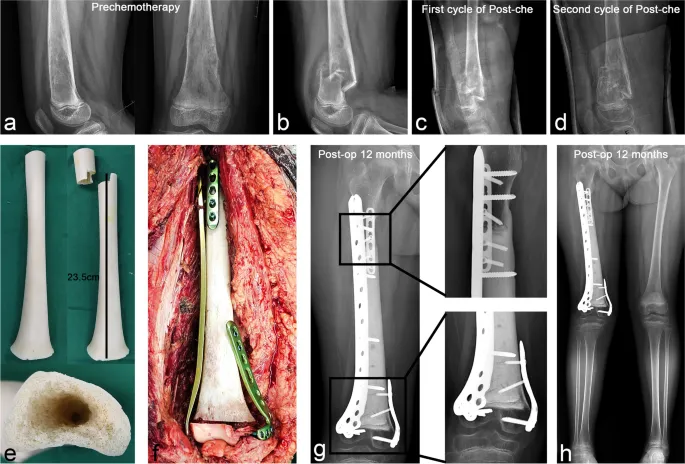
⭐ Composite grafts aim to provide a multi-faceted approach by combining osteoconductive matrices, osteoinductive signals, and sometimes osteogenic cells to optimize healing in challenging bone defects or fusions where a single graft type may be insufficient. This synergy often leads to improved clinical outcomes compared to using individual components alone for complex cases like revision surgeries or in compromised hosts (e.g., smokers, diabetics).
Pros & Cons - Balancing Act
- Advantages (Pros):
- Enhanced properties: Combines osteoconduction (scaffold), osteoinduction (signals), +/- osteogenesis (cells).
- Tailored solutions: Customizable for specific defect requirements.
- Reduced autograft need: ↓ donor site morbidity.
- Improved handling/mechanics: Better structural integrity or delivery.
- Versatile applications: Broad clinical utility.
- Disadvantages (Cons):
- Increased complexity: Potential for component interaction issues.
- Higher cost: Often more expensive than individual grafts.
- Variable resorption: Components may resorb at different rates.
- Regulatory hurdles: Newer composites require extensive validation.
- Immunogenicity risk: Possible with allograft components.
⭐ A key advantage of composite grafts is the potential to combine an osteoconductive matrix with osteoinductive factors like BMPs, enhancing bone regeneration.
High‑Yield Points - ⚡ Biggest Takeaways
- Composite grafts combine multiple materials to achieve osteoconduction, osteoinduction, and osteogenesis.
- Typically pair scaffolds (e.g., ceramics, DBM) with biologics like BMPs or cells (e.g., BMA).
- Used to enhance healing in nonunions, spinal fusions, and large bone defects.
- Significantly reduce autograft volume, thus minimizing donor site morbidity and pain.
- Examples: DBM with ceramic carriers, allograft chips with BMP-2, or synthetic grafts with BMA.
- Offer both structural support and active biological stimulation for bone repair.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

