Introduction to BMPs - Protein Powerhouses
- Definition: Naturally occurring proteins, powerful growth factors. Part of the Transforming Growth Factor-beta (TGF-β) superfamily.
- Primary Function: Key regulators of osteogenesis (new bone formation) and chondrogenesis (cartilage development). Crucial for bone healing.
- Discovery: Identified by Marshall R. Urist in 1965 through demineralized bone matrix experiments.
⭐ BMPs are unique: the only known proteins that can induce de novo bone formation, even in ectopic (non-skeletal) sites. oka
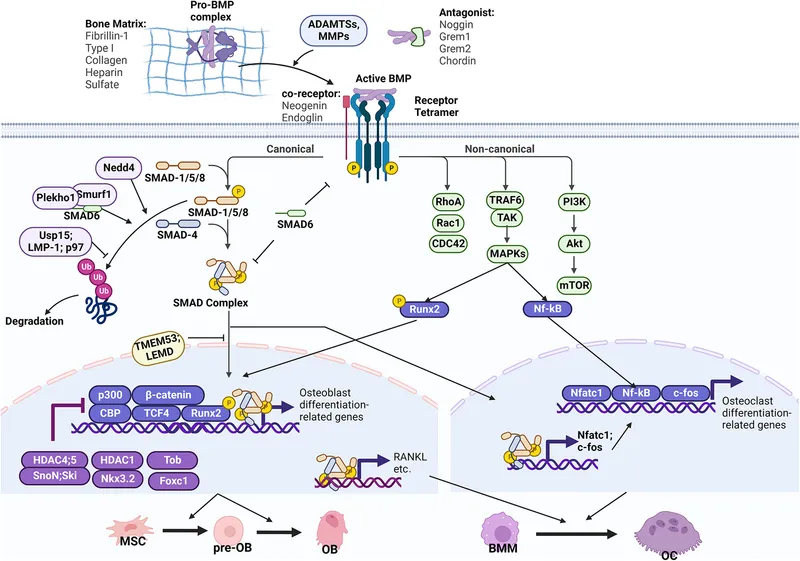
Mechanism of Action - Signal Senders
- BMPs: Osteoinductive cytokines (signal senders).
- Receptors: Transmembrane serine/threonine kinases.
- Type II (e.g., BMPR2): Ligand-binding; constitutively active.
- Type I (e.g., ALK2,3,6): Recruited by Type II-BMP complex; phosphorylated to activate.
- Signaling Pathways:
- SMAD-dependent (Canonical): Key for osteogenesis.
- **SMAD-independent**: Via MAPK (p38, ERK), PI3K/Akt pathways.
- Cellular Effect: Drives mesenchymal stem cell (MSC) chemotaxis, proliferation, & differentiation into osteoblasts.
⭐ SMAD proteins (SMAD1, SMAD5, SMAD8, and SMAD4) are key intracellular mediators of BMP signaling.
Types & Products - Key Players
- Key clinically significant Bone Morphogenetic Proteins: BMP-2, BMP-7.
- Recombinant human forms: rhBMP-2 (e.g., INFUSE), rhBMP-7 (e.g., OP-1).
| Feature | rhBMP-2 (INFUSE) | rhBMP-7 (OP-1 / Osigraft) |
|---|---|---|
| Carrier | Absorbable Collagen Sponge (ACS) | Bovine Type I Collagen + CMC |
| Common Uses | Spinal fusion, open tibial # | Long bone nonunions, revision spine |
| Osteoinduction | Stronger | Moderate |
Clinical Applications - Healing Helpers
- FDA-Approved:
- Spinal Fusion: e.g., Anterior Lumbar Interbody Fusion (ALIF) with rhBMP-2.
- Tibial Nonunions: Recalcitrant cases, treated with rhBMP-2 or rhBMP-7.
- Off-Label Uses (⚠️ Use with caution):
- Fracture Healing: Complex fractures, segmental defects.
- Avascular Necrosis (AVN): Early-stage femoral head AVN.
- Osseointegration: Enhancing implant fixation.
- Delivery Methods:
- Collagen Sponge (ACS): Most common carrier.
- Calcium Phosphate Ceramics: e.g., TCP, HA.
- DBM.
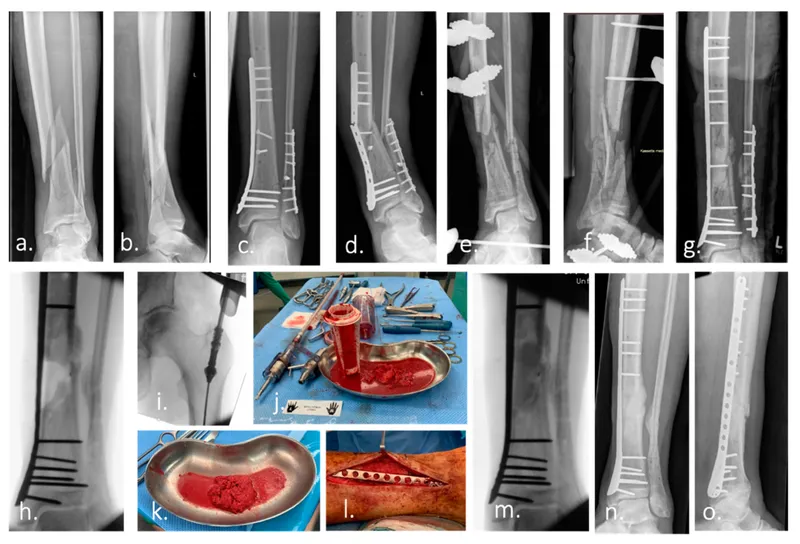
⭐ BMPs are crucial for challenging bone healing, especially in recalcitrant nonunions and significant segmental defects.
Pros, Cons & Cautions - Risks & Rewards
Table: BMPs - Pros vs. Cons
| Pros | Cons |
|---|---|
| * Strong osteoinductive action | * High cost |
| * Avoids autograft morbidity (↓pain, ↓infection) | * Post-op: inflammation, swelling, seroma |
| * Reduces operative time | * Heterotopic ossification (HO), esp. cervical |
| * Enhanced fusion rates (select cases) | * Transient radiculitis |
| * ⚠️ Carcinogenicity: theoretical risk; avoid if prior local malignancy. Data limited. |
- Cautions:
- Cervical spine: use judiciously (airway risk from swelling/HO).
- Monitor for inflammation/seroma.
- Contraindications:
- Skeletal immaturity
- Active infection
- Pregnancy/Lactation
- Hypersensitivity (BMP/carrier)
- Malignancy (current/history at site).
⭐ Heterotopic ossification is a significant concern with BMP use, especially in cervical spine procedures.
High‑Yield Points - ⚡ Biggest Takeaways
- BMPs are powerful osteoinductive agents, stimulating new bone growth.
- BMP-2 and BMP-7 are FDA-approved for spinal fusion and long bone non-unions.
- They signal via serine/threonine kinase receptors (Type I & II).
- Used in spinal arthrodesis, fracture non-union, and critical bone defects.
- Potential side effects: heterotopic ossification, transient inflammation, seroma.
- Delivered with a carrier (e.g., collagen sponge) for site-specific action.
- Avoid in skeletally immature patients, active infection, or pregnancy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

