Bone Graft Immunology - Graft Encounters
- Antigenicity: Allografts & xenografts possess antigens; autografts are non-immunogenic.
- Primary Antigens: Cell-surface Major Histocompatibility Complex (MHC/HLA) on donor cells.
- Host Response:
- Cell-mediated: T-lymphocytes (e.g., cytotoxic T-cells) attack graft.
- Humoral: B-lymphocytes produce antibodies against donor antigens.
- Processing Impact: Methods like freezing or irradiation reduce immunogenicity but may alter graft properties.
⭐ The most significant antigens triggering rejection in bone allografts are Class I and Class II MHC (HLA in humans) molecules expressed on donor cells.
Bone Graft Immunology - ID Tags & Donor Files
- Immune response primarily cell-mediated, targeting donor antigens.
- Key Antigens ("ID Tags"):
- MHC (HLA in humans): Most critical.
- Class I: On all nucleated cells.
- Class II: On Antigen Presenting Cells (APCs); most potent stimulators.
- ABO blood group antigens: On vascular endothelium.
- Minor histocompatibility antigens.
- MHC (HLA in humans): Most critical.
- Graft Types & Immunogenicity:
| Graft Type | Immunogenicity | Key Antigens |
|---|---|---|
| Autograft | None | N/A |
| Allograft | Variable | MHC I & II, ABO |
| - Fresh | ↑↑ High | MHC I, II (passenger leukocytes) |
| - Frozen | ↑ Moderate | MHC I, ↓MHC II |
| - Freeze-dried | ↓ Low | Residual MHC |
| - Demineralized | ↓↓ Very Low | Acellular, minimal |
| Xenograft | ↑↑↑ Very High | Xenoantigens (e.g., α-Gal), Non-human MHC |
Bone Graft Immunology - The Rejection Reaction
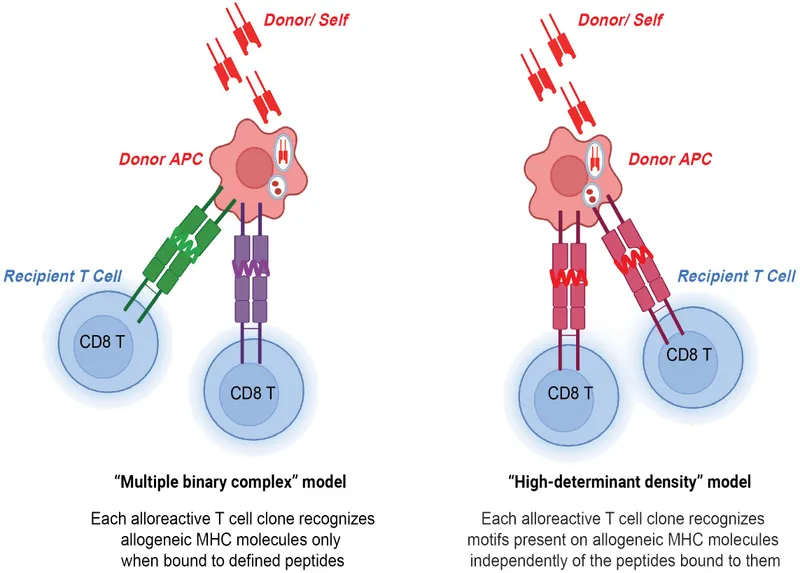
- Trigger: Donor Major Histocompatibility Complex (MHC) Class I & II antigens on allograft cells.
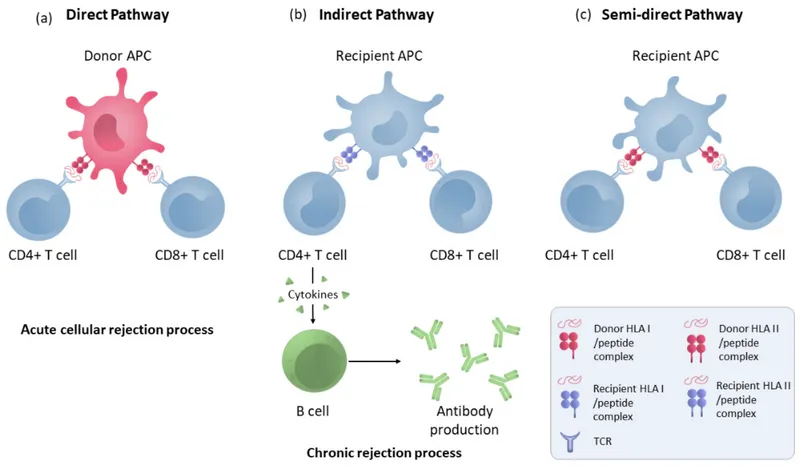
- Recognition:
- Direct: Host T-cells vs. donor MHC on donor APCs.
- Indirect: Host APCs process & present donor antigens to T-cells.
- Immune Response Pathway:
- Outcome: Inflammation, impaired healing, graft resorption, failure.
⭐ Fresh, cellular allografts elicit the strongest immune response; processing (freeze-drying, demineralization) reduces immunogenicity.
Bone Graft Immunology - Tweaking the Transplant
- Goal: Minimize host immune response to allografts/xenografts.
- Key Factors Influencing Immunogenicity:
- Cellularity: Viable cells (osteocytes, marrow) are primary antigen source.
- MHC/HLA Antigens: Expressed on donor cells, trigger T-cell mediated rejection.
- Graft Type: Autograft (none) < Allograft (moderate) < Xenograft (high).
- Graft Processing to ↓ Immunogenicity:
- Freezing (-20°C to -80°C) / Freeze-drying: Kills cells, preserves matrix. Most common.
- Irradiation (e.g., 25 kGy): Sterilizes, devitalizes cells.
- Washing/Solvent treatment: Removes cellular debris, lipids.
- Decellularization: Removes cells, aims to preserve scaffold.
⭐ Fresh, unprocessed allografts elicit the strongest immune response due to viable donor cells expressing MHC antigens.
 oka
oka
Bone Graft Immunology - Outcomes & Outlooks
- Graft Failure: Immune-mediated rejection due to donor Major Histocompatibility Complex (MHC) antigens on osteocytes, osteoblasts, and passenger leukocytes is a key concern for allografts, potentially leading to resorption or non-union.
- Strategies to Enhance Success:
- Graft Processing: Freezing, freeze-drying, irradiation significantly ↓ antigenicity.
- Autografts: Ideal, circumvent immune rejection.
- Immunomodulation: Limited role in routine bone grafting due to systemic effects.
- Outlook: Focus on developing less immunogenic allografts and advanced tissue-engineered constructs.
⭐ Creeping substitution: Host cells gradually resorb and replace graft material, essential for successful allograft incorporation and remodeling over months to years.
High‑Yield Points - ⚡ Biggest Takeaways
- Fresh allografts are most immunogenic due to MHC (HLA) antigens on donor cells.
- Cell-mediated immunity (T-lymphocytes) is the primary mechanism of allograft rejection.
- Graft processing (e.g., freezing, freeze-drying, irradiation) reduces immunogenicity but can impair biological activity.
- Autografts are non-immunogenic (gold standard); xenografts are highly immunogenic.
- HLA matching is not routinely performed for bone allografts, unlike solid organ transplants.
- Immune response can lead to inflammation, graft resorption, and eventual failure.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

