Allograft Types & Properties - Bone's Best Buds
Allografts: Bone tissue transplanted from one individual to another of the same species (genetically non-identical).
-
Allograft Comparison: Key Properties
Type Osteoconduction Osteoinduction Osteogenesis Immunogenicity Strength Fresh/ Fresh-Frozen Yes High Yes (cells) High High Freeze-Dried (FDBA) Yes Minimal No Reduced Moderate Demineralized (DFDBA) Yes Good (BMPs) No Low Low Structural Variable Variable No Variable High -
Pros: Readily available in various forms/sizes, avoids donor site morbidity.
-
Cons: Potential immunogenicity, disease transmission risk (low but critical), slower incorporation than autograft, resorption.
⭐ DFDBA's superior osteoinductivity vs. FDBA is due to exposed Bone Morphogenetic Proteins (BMPs) post-demineralization.
Allograft Processing & Storage - Clean & Keep
- Procurement & Screening:
- Strict donor selection (age, medical history, no malignancy/infection).
- Mandatory serological testing: HIV, HBV, HCV, Syphilis.
- Processing Steps:
- Sterilization Methods:
- Gamma Irradiation: Dose 2.5 - 3.5 Mrad.
- Pros: Highly effective.
- Cons: ↓ Biomechanical strength.
- Ethylene Oxide (EtO):
- Pros: Less damage to graft strength.
- Cons: Potential toxic residues; aeration needed.
- Chemical Sterilants: (e.g., peracetic acid).
- Variable effects on graft.
- Gamma Irradiation: Dose 2.5 - 3.5 Mrad.
- Storage Techniques:
- Fresh: Rare; use within 24-72 hrs. Highest immunogenicity.
- Frozen (Deep-Freeze): -70°C to -80°C. Preserves biomechanics well. Shelf life: up to 5 years.
⭐ Deep freezing at -70°C to -80°C is the most common method for structural allografts, maintaining good biomechanical properties for up to 5 years.
- Freeze-dried (Lyophilized): Room temperature storage. Long shelf life. ↓ Immunogenicity, but weaker; requires rehydration.
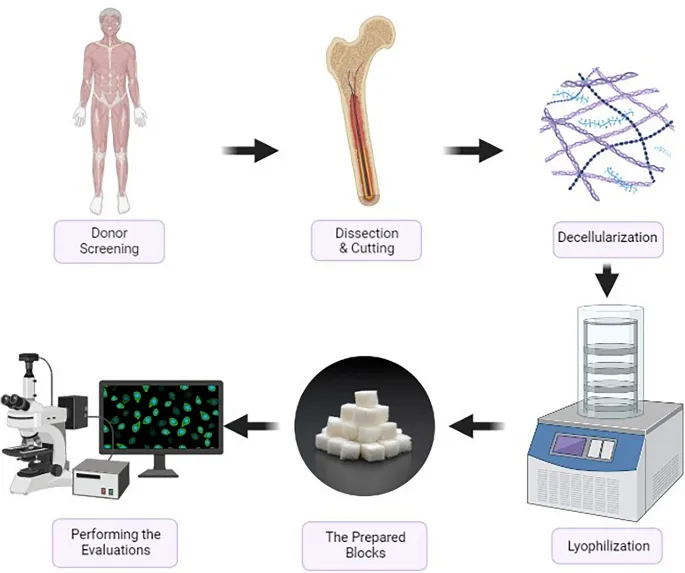 oka
oka
Allograft Clinical Applications - Ortho Fixes
📌 Mnemonic "JoiST-B": Joint, Spine, Trauma, Bone defects.
- Joint Reconstruction:
- Osteochondral allografts: Articular cartilage defects (e.g., femoral condyle, talus).
- Massive/segmental allografts: Limb salvage (tumors), severe bone loss in revision arthroplasty (e.g., Allograft-Prosthetic Composites - APCs).
- Spinal Surgery:
- Structural allografts (femoral rings, fibular struts): Interbody fusion (e.g., ALIF, PLIF).
- Morselized/crushed cancellous allograft: Graft extender.
- Trauma & Nonunions:
- Strut allografts: Periprosthetic fractures, nonunions needing structural support.
- Cancellous chips/cubes: Filling bone voids (comminuted fractures).
- Bone Defect Filling:
- Post-tumor curettage (e.g., GCT, ABC).
- Osteonecrosis.
⭐ Massive osteoarticular allografts are crucial for limb salvage after bone tumor resection, providing a biological reconstruction option.
Allograft Immunology & Complications - Host vs Graft
- Host Immune Response (HVGR):
- T-cell & B-cell mediated against donor HLA antigens.
- Fresh/frozen allografts most immunogenic; processing (freezing, irradiation) ↓ immunogenicity.
- Complications:
Type Prevention Management Rejection Processing (reduces immunogenicity). Graft removal if symptomatic. Disease Transmission Donor screening, serology, sterilization (gamma irradiation 25-35 kGy). Treat infection, graft removal. Graft Failure Stable fixation, good host bed, proper graft selection. Revision surgery. Delayed Incorporation Optimize host factors, appropriate graft choice. Bone stimulation.

⭐ Gamma irradiation (25-35 kGy) is a common method for sterilizing allografts and reducing immunogenicity, but can affect biomechanical properties.
High‑Yield Points - ⚡ Biggest Takeaways
- Allografts: Bone from genetically non-identical donors (same species), requiring careful processing.
- Processing (freezing, freeze-drying, irradiation) aims to ↓ immunogenicity and ensure sterility.
- Fresh allografts offer viable cells but carry high immunogenicity; thus, rarely used.
- FDBA (Freeze-Dried Bone Allograft) is primarily osteoconductive, providing a structural scaffold.
- DFDBA (Demineralized FDBA) is osteoinductive due to exposed BMPs, actively promoting bone formation.
- Applications: Filling large bone defects, spinal fusion, revision arthroplasty.
- Risks: Disease transmission (low), immune response, delayed incorporation via creeping substitution.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

