Bone Composition & Cells - Microscopic Marvels
- Composition (Matrix):
- Organic (~35%):
- Collagen Type I (90% of organic): Tensile strength.
- Ground Substance: Proteoglycans, Glycoproteins (e.g., osteonectin, osteocalcin).
- Inorganic (~65%):
- Hydroxyapatite crystals: $Ca_{10}(PO_4)_6(OH)_2$. Compressive strength.
- Organic (~35%):
- Cells (The Bone Workforce): 📌 Blasts Build, Clasts Carve.
- Osteoblasts: Form bone. Synthesize osteoid (unmineralized matrix). Marker: Alkaline Phosphatase (ALP).
- Osteocytes: Mature osteoblasts in lacunae. Mechanosensors, orchestrate remodeling.
- Osteoclasts: Resorb bone. Multinucleated. Found in Howship's lacunae. Marker: TRAP.
- Bone Lining Cells: Quiescent osteoblasts on bone surface.
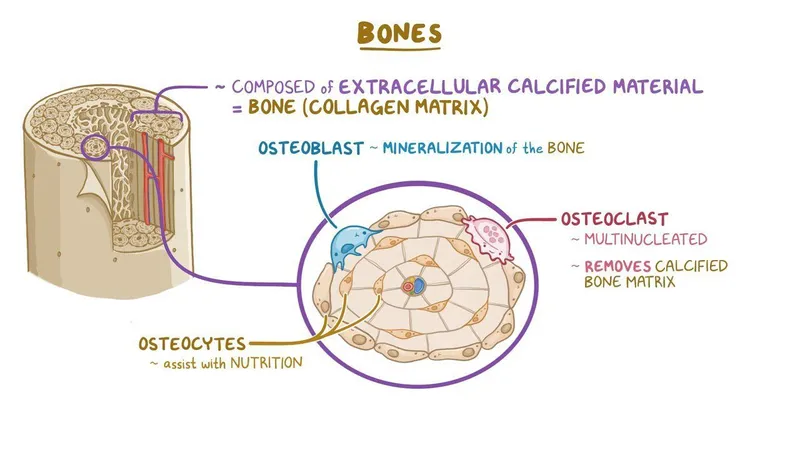
⭐ Osteocalcin, secreted by osteoblasts, is a key non-collagenous protein; serum levels reflect bone formation rate (Vitamin K-dependent).
Bone Architecture - Skeleton's Scaffolding
- Macroscopic:
- Cortical (Compact): Dense outer (80% mass). Resists bending/torsion. Unit: Osteon.
- Cancellous (Spongy): Inner porous (20% mass). Trabeculae on stress lines. Metabolically active.
- Microscopic:
- Woven Bone: Immature, disorganized collagen. Rapid formation (fetus, fracture, tumors).
- Lamellar Bone: Mature, organized collagen layers. Stronger. Forms osteons, trabeculae.
- Key Lamellar Features:
- Osteon (Haversian System): Central canal (vessels/nerves), lamellae, lacunae (osteocytes), canaliculi.
- Volkmann's Canals: Connect Haversian canals.
- Linings:
- Periosteum: Outer fibrous (Sharpey's fibers), inner osteogenic.
- Endosteum: Lines internal surfaces; osteogenic.
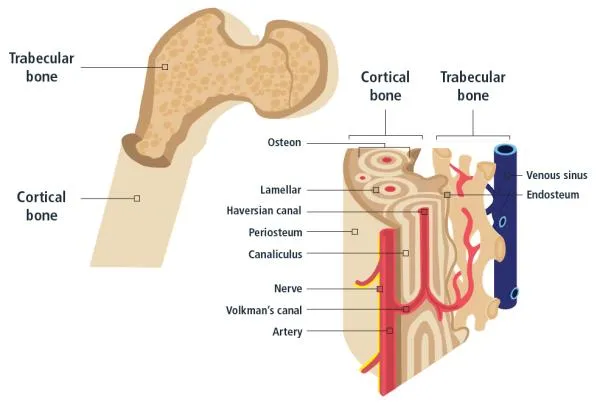
⭐ Wolff's Law: Bone adapts to loads; trabeculae align with stress.
Bone Formation & Remodeling - Dynamic Development
- Bone Formation (Ossification):
- Intramembranous: Direct formation from mesenchymal condensations. Osteoblasts deposit osteoid. E.g., skull, clavicle.
- Endochondral: Cartilage scaffold replaced by bone. Primary (diaphysis) & secondary (epiphysis) ossification centers. E.g., long bones.
- Epiphyseal plate zones: Resting, Proliferation, Hypertrophy, Calcification, Ossification (📌 RPHCO: "Real People Have Career Options").
- Bone Remodeling: Lifelong resorption (osteoclasts) & formation (osteoblasts) by Basic Multicellular Unit (BMU).
- Phases: Activation → Resorption → Reversal → Formation → Quiescence.
- Wolff's Law: Bone adapts to load. ↑ stress → ↑ density.
⭐ Wolff's Law: Mechanical stress dictates bone architecture; crucial for fracture healing and osteoporosis understanding.
- Hormonal control: PTH, Calcitonin, Vit D.
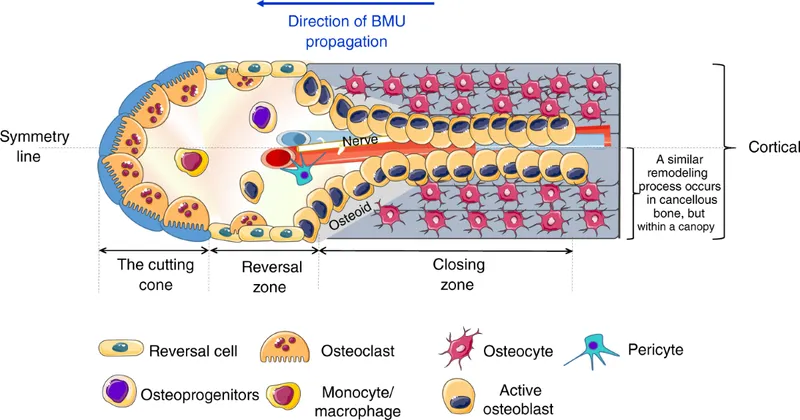
Bone Mechanics & Blood Supply - Force & Flow
- Bone Mechanics
- Wolff's Law: Bone remodels to adapt to mechanical stress. "Form follows function."
- Stress-Strain Curve: Describes bone's response to load.
- Elastic deformation: Recovers.
- Plastic deformation: Permanent.
- Ultimate failure point: Fracture.
- Anisotropy: Strength varies with direction of force.
- Viscoelasticity: Response depends on loading rate (stiffer with faster load).
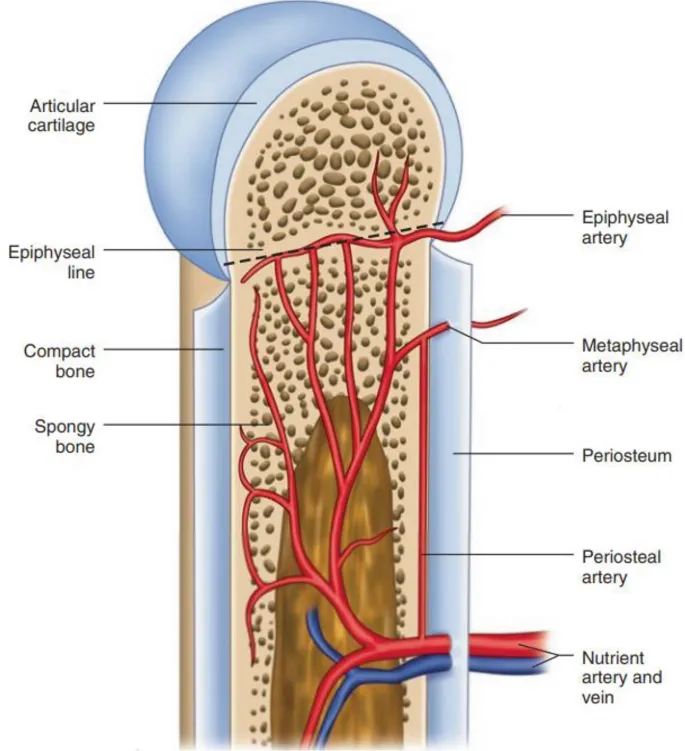
- Blood Supply (Primarily centrifugal flow: marrow outwards)
- Nutrient Artery: Main diaphyseal supply (inner 2/3 cortex).
- Periosteal Arteries: Outer 1/3 cortex; vital in fractures, growth.
- Metaphyseal & Epiphyseal Arteries: From periarticular vascular plexus.
⭐ Femoral head AVN post #NOF (Neck of Femur fracture) is high-risk due to precarious supply mainly from medial circumflex femoral artery.
High‑Yield Points - ⚡ Biggest Takeaways
- Bone is a dynamic, specialized connective tissue; Type I collagen provides tensile strength, while hydroxyapatite crystals confer compressive strength.
- Osteoblasts are responsible for bone formation (ossification & calcification); Osteoclasts are responsible for bone resorption.
- Woven bone (immature) is characterized by random collagen fiber orientation, found in fetal development and fracture calluses; Lamellar bone (mature) is organized and stronger.
- The Haversian system (osteon) is the fundamental structural unit of compact (cortical) bone.
- Wolff's Law states that bone adapts its structure to the mechanical loads it experiences.
- The periosteum is crucial for blood supply, appositional growth, and fracture healing, especially in children.
- Vitamin D is essential for calcium and phosphate absorption, vital for bone mineralization and health.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

