Biomechanics of Spine - Vertebral Blueprint
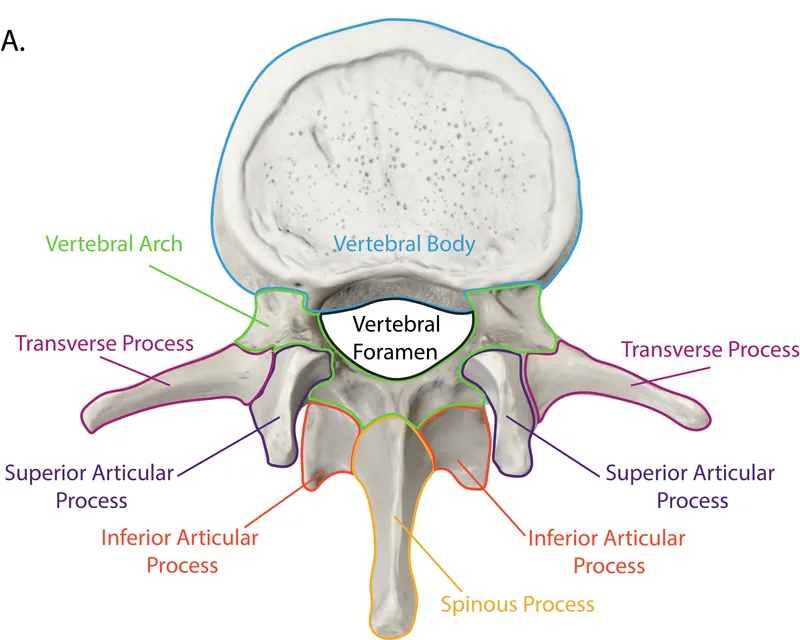
- Typical Vertebra Components:
- Vertebral Body: Weight-bearing, anterior.
- Vertebral Arch: Posterior, protects spinal cord.
- Pedicles: Connect body to arch.
- Laminae: Form roof of vertebral canal.
- Processes (for muscle/ligament attachment & articulation):
- Spinous Process (1)
- Transverse Processes (2)
- Articular Processes (4): Superior (2), Inferior (2) - form facet joints.
- Regional Variations: Adapt to function (e.g., C1/C2 for rotation, lumbar for weight-bearing).
⭐ The pars interarticularis is a critical region of the lamina between the superior and inferior articular processes; defects here (spondylolysis) are common, especially in the lumbar spine (L5).
Biomechanics of Spine - Flex & Twist Dynamics
- Flexion:
- Anterior structures compress (disc, body).
- Posterior elements stretch (ligaments, facets).
- Nucleus pulposus shifts posteriorly.
- Foramen size ↑.
- Extension:
- Anterior elements stretch, posterior compress.
- Nucleus pulposus shifts anteriorly.
- Foramen size ↓.
- Axial Rotation (Twist):
- Maximal in cervical, then thoracic; lumbar limited (facet orientation).
- Annulus fibrosus resists torsion.
- Coupled with lateral bending.
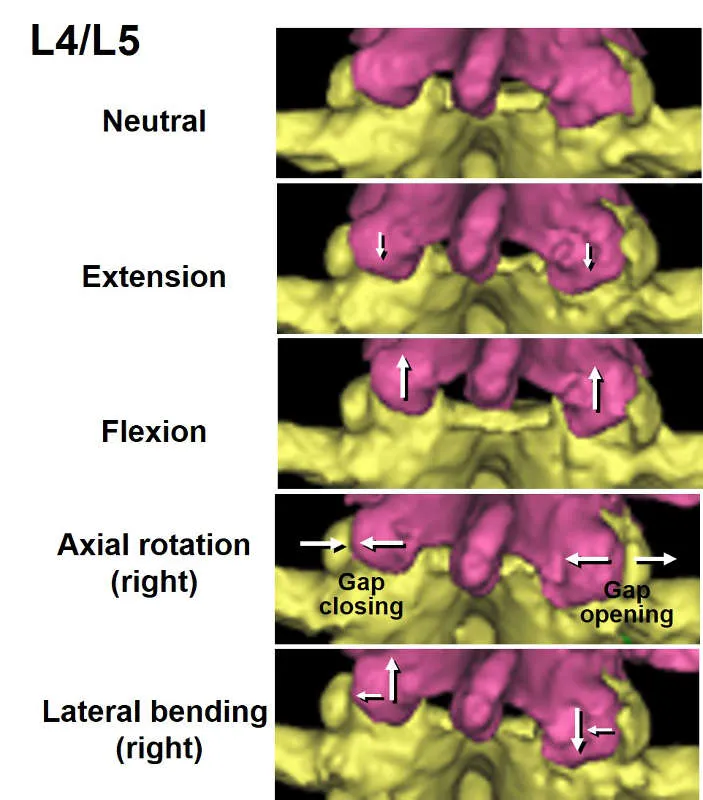
⭐ In lumbar spine rotation, only about 50% of annulus fibrosus fibers are loaded at any given time due to their alternating oblique orientation, providing significant torsional resistance.
Biomechanics of Spine - Load Bearing & Pressure
- Load Distribution:
- Anterior column (vertebral bodies, IVDs): Bears ~80% axial compression.
- Posterior column (facet joints, ligaments): Bears ~20% axial load; guides motion, resists shear/tension.
- Intervertebral Disc (IVD):
- Nucleus Pulposus (NP): Hydrophilic; converts axial load to radial stress.
- Annulus Fibrosus (AF): Lamellar collagen; resists tension, torsion, shear.
- Intradiscal Pressure (IDP) - L3 Disc: (Values relative to standing = 100)
- Supine: 25 (lowest)
- Standing: 100
- Sitting unsupported: 140
- Forward bending (standing): 150
- Lifting 20kg (improperly): 340 (highest)
- 📌 Nachemson's classic study.
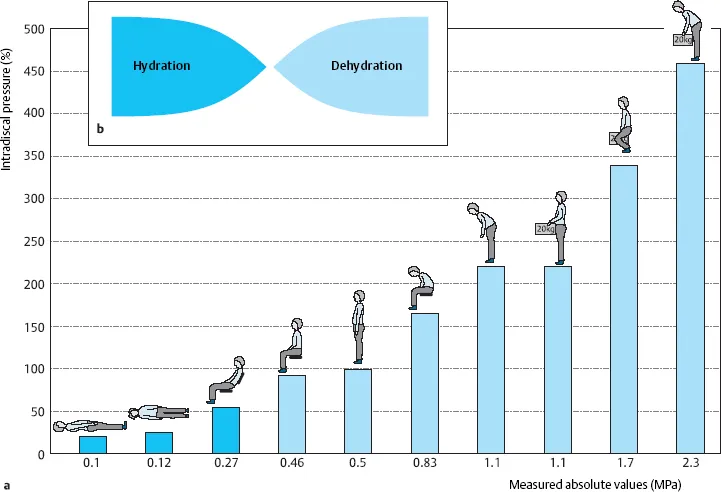
⭐ The nucleus pulposus, due to its high water content, behaves hydrostatically, distributing applied loads evenly to the annulus fibrosus and endplates.
Biomechanics of Spine - Stability & Strain Patterns
- Panjabi's Model:
- Passive: Bones, discs, ligaments (ALL, PLL, LF, ISL, SSL), capsules.
- Active: Muscles & tendons (paraspinal, abdominal).
- Neural: CNS/PNS control for dynamic stability.
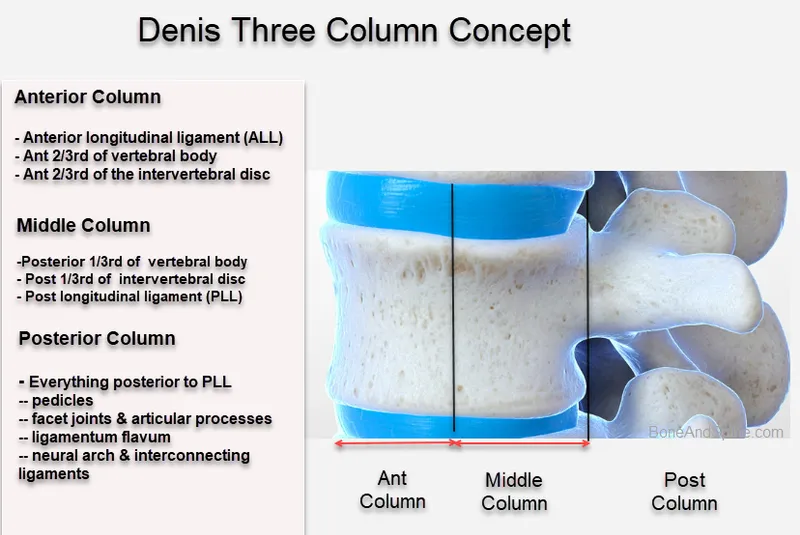
- Denis' 3 Columns:
- Anterior: ALL, ant. body/disc.
- Middle: PLL, post. body/disc.
- Posterior: Pedicles, facets, lamina, spinous proc., post. ligaments (PLC).
- Instability if ≥2 columns disrupted.
- Strain & Injury Patterns:
- Axial Load: Burst Fx, endplate #.
- Flexion: Ant. wedge Fx, PLC injury.
- Extension: Post. element Fx, ALL strain.
- Flexion-Distraction: Chance Fx (seatbelt), PLC disruption.
- Rotation/Shear: Facet injury, disc/annular tears.
- Neutral Zone (NZ): ↑NZ → instability.
- IAR (Instantaneous Axis of Rotation): Shifts with pathology.
⭐ An increased Neutral Zone (NZ) signifies reduced spinal stiffness and is a key indicator of clinical instability, implying higher injury risk with physiological loads.
High‑Yield Points - ⚡ Biggest Takeaways
- Nucleus pulposus resists axial compression; annulus fibrosus withstands tension and torsion.
- Spinal motion is often coupled: lateral bending usually occurs with axial rotation.
- The Instantaneous Axis of Rotation (IAR) shifts during motion and with degeneration.
- Fryette's Laws describe predictable coupled motions in thoracic/lumbar spine.
- Spinal curves: tensile forces maximal on convexity; compressive forces on concavity.
- Intradiscal pressure: lowest supine, highest sitting flexed with weight.
- Facet joints resist torsion and shear forces, vital in lumbar spine.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

