Shoulder & Upper Arm - Sling Central Station
- Rotator Cuff (📌 SITS):
- Supraspinatus: Initiates abduction (0-15°).
- Infraspinatus: External rotation.
- Teres minor: External rotation.
- Subscapularis: Internal rotation.
- Axillary Nerve (C5, C6):
- Passes through quadrangular space (with posterior circumflex humeral artery).
- Vulnerable: Surgical neck of humerus fractures, anterior shoulder dislocations. Risk during deltoid splitting (safe zone >5 cm distal to acromion).
- Deltopectoral Approach:
- Internervous plane: Deltoid (axillary n.) & Pectoralis major (pectoral nn.).
- Key structure: Cephalic vein in deltopectoral groove (preserve).
- Brachial Plexus (C5-T1 Roots):
- Overview: Roots → Trunks → Divisions → Cords → Branches.
- Common Injuries: Erb's palsy (C5-C6, upper trunk; "waiter's tip"), Klumpke's palsy (C8-T1, lower trunk; "claw hand").

⭐ Supraspinatus is the most commonly torn rotator cuff muscle, often at its insertion on the greater tuberosity of the humerus.
Elbow & Forearm - Hinge & Twist Zone
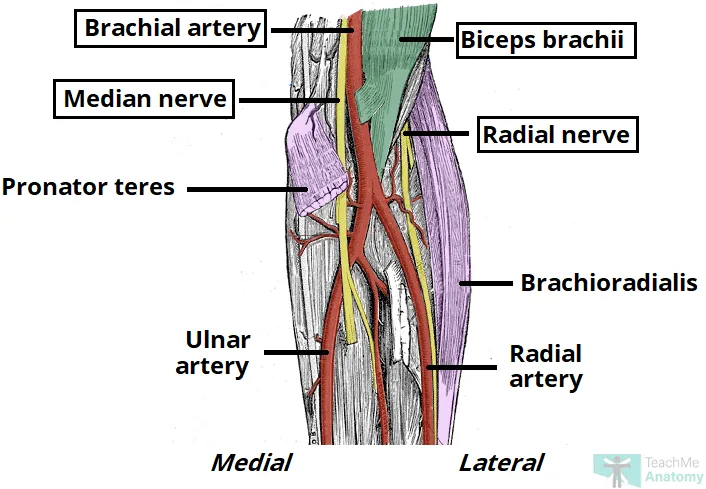
- Cubital Fossa:
- Boundaries: Brachioradialis (lat), Pronator teres (med), inter-epicondylar line (sup).
- Contents (📌 MBBR - My Bottoms Turned Red): Median N, Brachial A, Biceps tendon, Radial N (deep).
- Nerves at Risk (Elbow):
- Ulnar N: Cubital tunnel (posterior to medial epicondyle).
- Median N: Anteriorly (e.g., supracondylar fracture).
- Radial N/Posterior Interosseous Nerve (PIN): Supinator muscle (e.g., radial head/neck fracture).
- Key Fractures & Neurovascular Risks:
- Supracondylar Humerus #: Brachial Artery, Median N (Anterior Interosseous Nerve - AIN - most common palsy).
- Monteggia (Proximal Ulna # + Radial Head Dislocation): PIN.
- Galeazzi (Distal Radius # + Distal Radioulnar Joint - DRUJ - Dislocation): AIN, Ulnar N.
- Forearm Compartments:
- Anterior: Flexors/pronators (Median/Ulnar N).
- Posterior: Extensors/supinator (Radial N/PIN).
- Lateral (Mobile Wad): Brachioradialis, ECRL, ECRB (Radial N).

- Volkmann's Ischemic Contracture: Consequence of untreated compartment syndrome; leads to muscle/nerve necrosis, fibrosis, and characteristic contractures.
⭐ In supracondylar humerus fractures, the brachial artery is the most critical vascular structure at risk, while the Anterior Interosseous Nerve (AIN) is the most commonly injured nerve component related to the median nerve proper.
Hip & Thigh - Ball & Socket Powerhouse
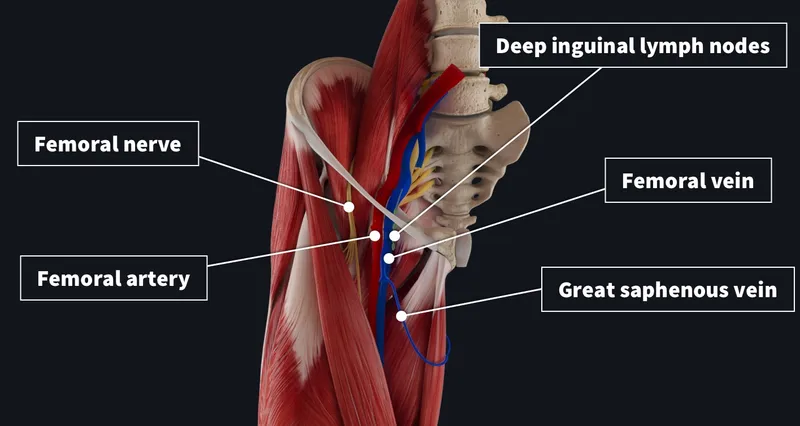
- Femoral Triangle:
- Boundaries: Inguinal lig. (sup.), Sartorius (lat.), Adductor longus (med.).
- Contents (lat.→med.): 📌 NAVEL (Nerve, Artery, Vein, Empty space, Lymphatics).
- Blood Supply (Femoral Head):
- Children: Artery of ligamentum teres.
- Adults: Medial & lateral circumflex femoral arteries (Medial dominant).
⭐ Main adult supply: Medial circumflex femoral artery.

- Sciatic Nerve:
- Course: Inferior to piriformis (common).
- Risk: Posterior hip approach.
- Hip Surgical Approaches (Internervous Plane; Risk):
- Posterior (Southern): Gluteus max split; Sciatic n.
- Lateral (Hardinge): TFL/Gluteus medius; Superior gluteal n.
- Anterior (Smith-Petersen): Sartorius/TFL; Lat. fem. cutaneous n.

- Trendelenburg Sign:
- Cause: Gluteus medius/minimus weakness.
- Nerve: Superior gluteal n. injury.
Knee & Leg - Crucial Crossroads
- Knee Ligaments:
- ACL: Attaches anterior tibia to lateral femoral condyle; prevents anterior tibial translation. Injury: Non-contact pivot.
- PCL: Attaches posterior tibia to medial femoral condyle; prevents posterior tibial translation. Injury: Dashboard.
- MCL: Resists valgus stress. LCL: Resists varus stress.

- Menisci: Medial ('C' shape, less mobile, often injured) vs. Lateral ('O' shape, more mobile). Blood supply to peripheral 1/3. Tears: e.g., bucket-handle.
- Popliteal Fossa: Boundaries: Biceps femoris (superolateral), Semitendinosus/Semimembranosus (superomedial), Gastrocnemius heads (inferior). Contents: 📌 "Serve And Volley Next Ball" (Popliteal Artery, Vein, Tibial Nerve, Common Peroneal Nerve).

- Common Peroneal Nerve: Courses around fibular neck; vulnerable to injury (fracture, compression) → foot drop.

- Leg Compartments (4): Anterior, Lateral, Superficial Posterior, Deep Posterior. Risk: Compartment syndrome (severe pain, paresthesia, pulselessness is late).
- Ankle Stability: Medial: Deltoid ligament. Lateral: Lateral ligament complex (ATFL, CFL, PTFL); ATFL most commonly sprained.
⭐ The Anterior Cruciate Ligament (ACL) is the most commonly injured ligament in the knee overall, especially in sports activities involving sudden stops or changes in direction (pivot).
High‑Yield Points - ⚡ Biggest Takeaways
- Axillary nerve: vulnerable at the surgical neck of humerus; Radial nerve: in the spiral groove.
- Femoral head blood supply: primarily from the medial circumflex femoral artery in adults.
- Scaphoid fractures: high risk of avascular necrosis due to its retrograde blood supply.
- Common peroneal nerve injury at the fibular neck typically causes foot drop.
- Anterior compartment of the leg: most common site for acute compartment syndrome.
- Rotator cuff muscles (SITS): Supraspinatus, Infraspinatus, Teres minor, Subscapularis.
- Erb's palsy (C5-C6 root injury): results in a "waiter's tip" deformity.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

