General Complications - Scope's General Gripes
- Infection: Superficial, deep (septic arthritis).
- Thromboembolism (VTE): DVT/PE; risk with prolonged surgery/immobilization.
- Neurovascular Injury:
- Nerve: Neuropraxia (common), traction/portals.
- Vascular: Rare; pseudoaneurysm.
- Instrument Breakage: Potential retained body.
- Compartment Syndrome: Monitor high-risk (e.g., tibial) procedures.
- Fluid Extravasation: Edema; airway risk (shoulder).
- Tourniquet: Pain, palsy, burns. Limit use.
- Anesthesia Risks: Standard.
⭐ Neuropraxia is the most common nerve injury, usually transient.
Local & Procedure-Specific Complications - Trouble at the Portal
- Nerve Injury:
- Most frequent portal-specific issue.
- Common sites & nerves at risk:
- Knee (Anteromedial portal): Infrapatellar branch of Saphenous nerve.
- Ankle (Anterolateral portal): Superficial peroneal nerve.
- Shoulder (Posterior portal): Axillary nerve.
- Hip (Anterolateral portal): Lateral femoral cutaneous nerve.
- Mechanism: Direct trauma, traction, fluid extravasation pressure.
- Prevention: Anatomical knowledge, precise portal placement, blunt dissection.
⭐ Saphenous nerve (infrapatellar branch) injury is the most common nerve injury in knee arthroscopy, particularly vulnerable with anteromedial portal placement.
- Vascular Injury:
- Less common; potentially severe (e.g., popliteal artery with posterior knee portals).
- Risk ↑ with aberrant anatomy or poor technique.
- Portal Site Infection:
- Superficial (cellulitis) or deep (septic arthritis).
- Staphylococcus aureus is the most common pathogen.
- Risk factors: prolonged procedure, multiple portals, immunocompromised patient.
- Hematoma/Hemarthrosis:
- Common; usually self-limiting.
- Can cause pain, swelling, and restricted motion.
- Persistent Portal Drainage/Sinus Tract:
- May indicate low-grade infection, suture reaction, or retained foreign body.
- Instrument Breakage:
- Rare; requires retrieval, potentially via arthrotomy.
- Careful handling and inspection of instruments crucial.
- Fluid Extravasation & Edema:
- Common, especially with prolonged procedures.
- ⚠️ Massive extravasation can lead to compartment syndrome (critical in shoulder, hip, ankle).
- Subcutaneous emphysema if CO2 is used for insufflation.
- Stitch Abscess/Granuloma:
- Inflammatory reaction to suture material at the portal site.
Neurovascular & Joint-Specific Complications - Nerves & Vessels Beware
- General Risks: Direct trauma (instruments), traction, fluid extravasation (↑compartment pressure), thermal injury (RF).
- Prevention: Anatomic knowledge, careful portal placement, avoid over-distension, awareness of "safe zones".
- Shoulder:
- Axillary n. (anteroinferior, lateral portals)
- Musculocutaneous n. (anterior portals)
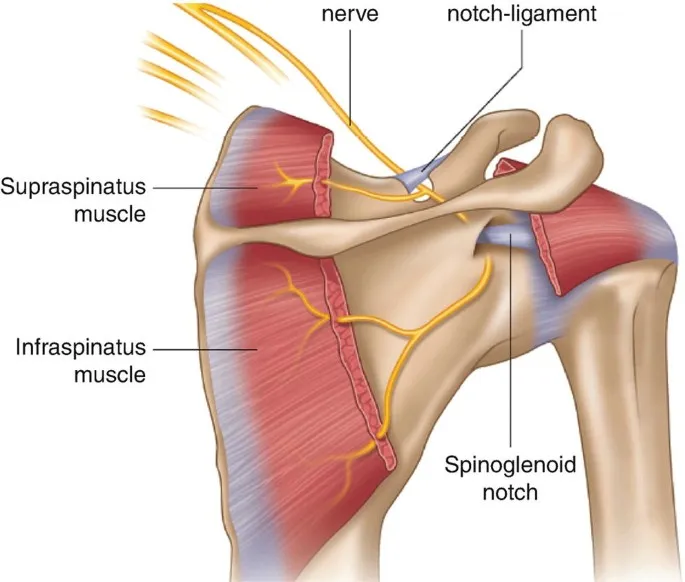
- Suprascapular n. (posterior portals)
- Knee:
- Saphenous n. (infrapatellar branch - anteromedial portal)
- Common peroneal n. (posterolateral portal, lateral meniscus repair)
- Popliteal a./v. (posterior portals, ACL tibial tunnel)
⭐ Injury to the infrapatellar branch of the saphenous nerve is the most frequent neurological complication in knee arthroscopy, often linked to anteromedial portal usage.
- Ankle:
- Superficial peroneal n. (anterolateral portal)
- Sural n. (posterolateral portal)
- Posterior tibial n./a. (posteromedial portal)
- Hip:
- Sciatic n. (posterior portals, excessive traction)
- Femoral n./a. (anterior portals)
- Lateral femoral cutaneous n. (anterolateral portals)
- Elbow:
- Ulnar n. (anteromedial, posteromedial portals)
- Median n. & Brachial a. (anterior portals)
- Radial n. (anterolateral portal)
Prevention & Management Strategies - Keeping Scopes Safe
- Pre-operative Shield:
- Thorough patient assessment; optimize co-morbidities.
- Prophylactic antibiotics (e.g., Cefazolin 1-2g IV).
- Confirm surgical site; full equipment check.
- Intra-operative Guard:
- Strict asepsis; precise, anatomical portal placement.
- Limit tourniquet time: aim <90 min (max 120 min).
- Maintain low irrigation fluid pressure (e.g., 30-50 mmHg).
- Minimize operative duration; gentle tissue handling.
- Post-operative Vigilance:
- Meticulous wound care; DVT prophylaxis for high-risk.
- Early recognition and prompt management of any adverse event.
⭐ To minimize neurovascular injury, carefully plan portal placement, especially near superficial nerves like saphenous (knee) or axillary (shoulder).
High‑Yield Points - ⚡ Biggest Takeaways
- Infection is the most serious complication; Staphylococcus aureus is a key pathogen.
- Thromboembolic events (DVT/PE) are significant risks, particularly after lower limb arthroscopy.
- Peripheral nerve injuries (e.g., saphenous nerve in knee, axillary nerve in shoulder) can result from portal placement.
- Instrument breakage with retained intra-articular fragments is a critical concern.
- Excessive fluid extravasation can lead to compartment syndrome, a surgical emergency.
- Hemarthrosis is a common cause of post-operative pain and joint stiffness_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

