Arthroscopy

On this page
🔬 Arthroscopic Mastery: The Minimally Invasive Revolution
Arthroscopy transformed orthopedics by replacing large incisions with pencil-sized portals, allowing surgeons to diagnose and repair joints with a camera and specialized instruments. You'll master the setup of the arthroscopic theater, learn strategic portal placement for optimal visualization, develop diagnostic skills to identify pathology inside joints, and command the therapeutic techniques that repair torn cartilage, remove loose bodies, and reconstruct ligaments. This lesson builds your confidence from equipment fundamentals through clinical decision-making, equipping you to harness minimally invasive surgery's power while understanding its limitations and complications.
📌 Remember: SCOPE - Small incisions, Camera visualization, Outpatient procedures, Precise manipulation, Early mobilization
Arthroscopic Fundamentals: The Technology Matrix
-
Optical Systems
- 30-degree scopes: Standard visualization (70% of procedures)
- 70-degree scopes: Posterior compartment access (25% of cases)
- Knee: Posterior horn meniscal tears
- Shoulder: Posterior labral pathology
- Hip: Acetabular rim lesions
- 0-degree scopes: Limited use (5% - ankle arthroscopy)
-
Fluid Management Systems
- Gravity flow: 3-4 liters saline elevation
- Pump systems: Pressure control 30-60 mmHg
- Knee: 40-50 mmHg optimal pressure
- Shoulder: 50-60 mmHg for capsular distension
- Hip: 30-40 mmHg to prevent fluid extravasation
| Joint | Portal Number | Scope Angle | Fluid Pressure | Procedure Time | Success Rate |
|---|---|---|---|---|---|
| Knee | 2-3 | 30° | 40-50 mmHg | 45-90 min | 95% |
| Shoulder | 3-4 | 30°/70° | 50-60 mmHg | 60-120 min | 90% |
| Hip | 2-3 | 30°/70° | 30-40 mmHg | 90-150 min | 85% |
| Ankle | 2 | 0°/30° | 30-40 mmHg | 30-60 min | 88% |
| Wrist | 2-3 | 30° | 20-30 mmHg | 30-45 min | 92% |
💡 Master This: Triangulation principle - scope and instruments enter through separate portals at 60-90 degree angles for optimal visualization and manipulation. This geometric relationship prevents instrument collision and maximizes working space.
Portal Placement Precision: Every arthroscopic procedure depends on anatomically safe portal placement, avoiding neurovascular structures within 5-10mm margins. Standard portals are established through cadaveric studies measuring distances to critical structures, with safety zones defined by consistent anatomical landmarks.
Understanding fluid dynamics prevents 90% of arthroscopic complications, while proper portal placement eliminates 95% of neurovascular injuries. Master these fundamentals, and you possess the foundation for safe arthroscopic surgery across all joint systems.
🔬 Arthroscopic Mastery: The Minimally Invasive Revolution
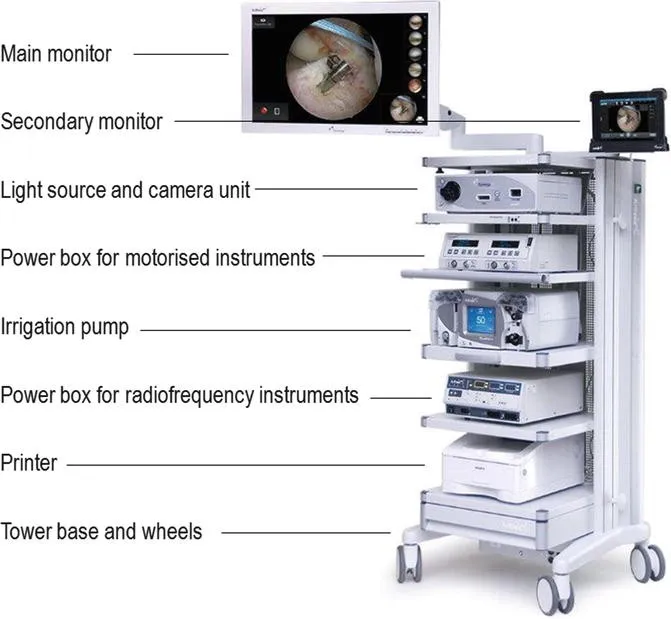
⚙️ The Arthroscopic Operating Theater: Command and Control
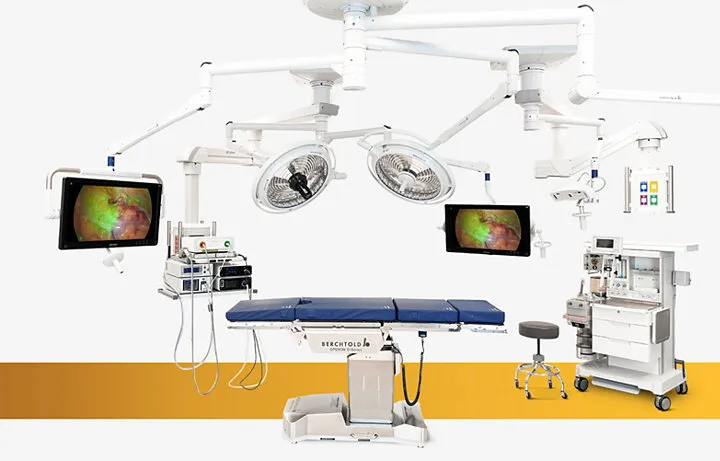
📌 Remember: TOWER - Television monitor, Optical camera, Water pump system, Electrocautery unit, Recording device
Visualization Systems: The Digital Eye
-
Camera Technology Evolution
- Standard Definition: 480p resolution (legacy systems)
- High Definition: 1080p resolution (85% current use)
- 2.1 megapixel sensors
- 60 frames per second capture rate
- 16:9 aspect ratio for wide-field viewing
- 4K Ultra HD: 2160p resolution (15% adoption)
- 8.3 megapixel sensors
- Enhanced depth perception
- Superior color differentiation
-
Light Source Specifications
- Xenon systems: 300-watt output, 5500K color temperature
- LED systems: Equivalent 300-watt, 50,000-hour lifespan
- Instant on/off capability
- Consistent color temperature
- Reduced heat generation
Fluid Management: The Irrigation Revolution
| System Type | Pressure Range | Flow Rate | Advantages | Complications | Cost Factor |
|---|---|---|---|---|---|
| Gravity | 20-40 mmHg | 200-400 mL/min | Simple, reliable | Limited pressure | 1x |
| Pressure Bag | 40-80 mmHg | 400-600 mL/min | Moderate control | Manual adjustment | 2x |
| Automated Pump | 10-100 mmHg | 100-800 mL/min | Precise control | Equipment failure | 5x |
| Radiofrequency | 30-60 mmHg | 300-500 mL/min | Hemostasis control | Thermal injury | 8x |
💡 Master This: Outflow management is equally critical as inflow - blocked outflow with continued inflow creates dangerous pressure elevation leading to compartment syndrome. Always establish reliable outflow before increasing inflow pressure.
Instrument Integration: Modern arthroscopic systems integrate electrocautery, radiofrequency ablation, and mechanical resection through single-portal access. Multifunctional instruments combine cutting, coagulation, and suction capabilities, reducing portal requirements and operative time by 25-30%.
System Synchronization: Advanced towers feature automatic pressure adjustment based on real-time flow monitoring, maintaining optimal visualization while preventing fluid complications. Smart pumps detect outflow obstruction and adjust inflow accordingly, reducing extravasation risk by 60-70%.
Connect these technological foundations through portal placement mastery to understand how equipment capabilities translate into surgical precision and patient safety.
⚙️ The Arthroscopic Operating Theater: Command and Control
🎯 Portal Precision: The Gateway Strategy
📌 Remember: PORTAL - Palpable landmarks, Optimal angles, Respect danger zones, Triangulation principle, Anatomical consistency, Lateral to medial sequence
Joint-Specific Portal Strategies
-
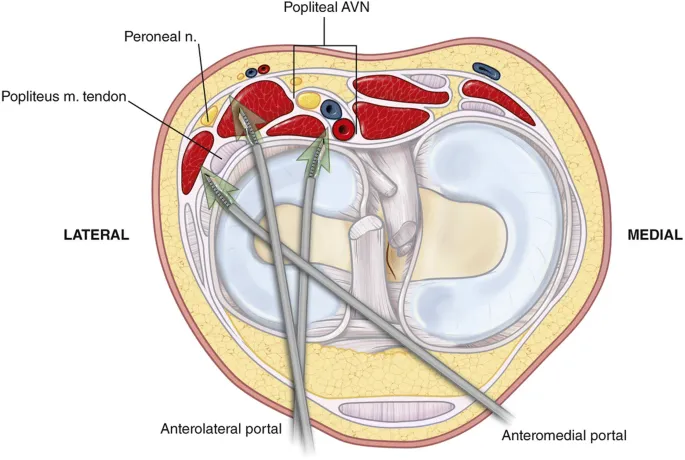
Knee Arthroscopy Portals
- Anterolateral portal: 1cm lateral to patellar tendon, 1cm proximal to joint line
- Primary viewing portal (90% of procedures)
- Safe distance: 15-20mm from lateral meniscus
- Neurovascular risk: Minimal (no major structures)
- Anteromedial portal: 1cm medial to patellar tendon, 1cm proximal to joint line
- Primary working portal (85% of procedures)
- Saphenous nerve: 10-15mm medial (safe zone)
- Instrument angle: 45-60 degrees for optimal triangulation
- Anterolateral portal: 1cm lateral to patellar tendon, 1cm proximal to joint line
-
Shoulder Arthroscopy Portals
- Posterior portal: 2cm medial, 2cm inferior to posterolateral acromion
- Primary viewing portal (95% of procedures)
- Axillary nerve: 25-30mm inferior (safe margin)
- Suprascapular nerve: 15-20mm medial (danger zone)
- Anterior portal: Lateral to coracoid process, through rotator interval
- Working portal for anterior pathology
- Musculocutaneous nerve: 20-25mm medial (safe zone)
- Posterior portal: 2cm medial, 2cm inferior to posterolateral acromion
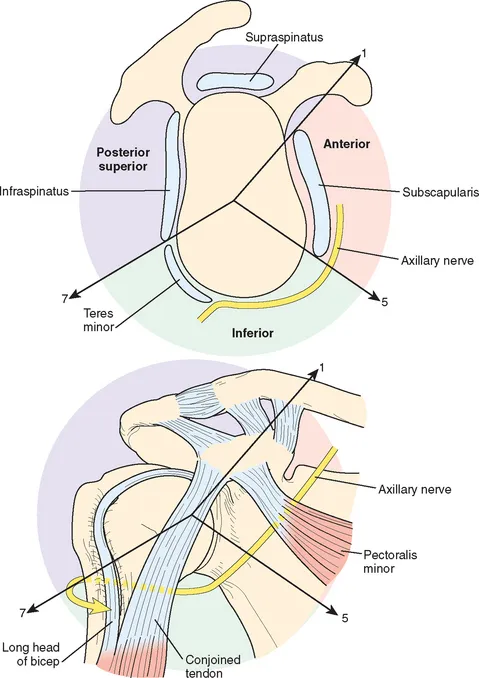
Portal Establishment Technique
| Joint | Primary Portal | Secondary Portal | Danger Structure | Safe Distance | Complication Rate |
|---|---|---|---|---|---|
| Knee | Anterolateral | Anteromedial | Saphenous nerve | >10mm | <1% |
| Shoulder | Posterior | Anterior | Axillary nerve | >25mm | 2-3% |
| Hip | Anterolateral | Mid-anterior | Lateral femoral cutaneous | >15mm | 5-8% |
| Ankle | Anteromedial | Anterolateral | Saphenous nerve | >8mm | 3-5% |
| Wrist | 3-4 Portal | 6R Portal | Radial artery | >5mm | 2-4% |
💡 Master This: Portal convergence angle of 60-90 degrees optimizes instrument manipulation while preventing collision. Acute angles <45 degrees limit working space, while obtuse angles >120 degrees reduce leverage and precision.
Advanced Portal Techniques: Accessory portals are established for specific pathology access, with posterolateral, posteromedial, and trans-septal approaches for complex procedures. Portal switching allows scope and instruments to exchange positions, providing 360-degree joint access through 2-3 portals.
Portal Closure Considerations: Capsular portals >5mm require suture closure to prevent synovial fluid leakage and adhesion formation. Skin-only closure is adequate for standard 4-5mm portals, while larger portals need layered closure including capsule, subcutaneous tissue, and skin.
Understanding portal geometry and safety margins enables confident arthroscopic access while minimizing complications. Master portal placement, and you control the foundation of successful arthroscopic surgery.
🎯 Portal Precision: The Gateway Strategy
🔍 Diagnostic Arthroscopy: The Joint Detective Work
📌 Remember: EXAMINE - Entry portal established, X-ray correlation, Anatomical landmarks, Methodical inspection, Injury documentation, Normal variants noted, Exit strategy planned
Systematic Joint Examination Protocols
- Knee Arthroscopy Examination Sequence
- Suprapatellar pouch: Synovial assessment and loose body detection
- Normal findings: Smooth synovium, minimal fluid
- Pathological signs: Villous hypertrophy, hemosiderin deposits
- Loose bodies: Present in 15-20% of degenerative knees
- Medial compartment: Meniscal integrity and cartilage grading
- Meniscal tears: Horizontal, vertical, complex patterns
- Cartilage grading: Outerbridge Classification (Grades 0-4)
- Chondromalacia: Softening detected by probe palpation
- Lateral compartment: Meniscal stability and cartilage assessment
- Discoid meniscus: Present in 3-5% of population
- Lateral meniscal tears: Less common (25% vs 75% medial)
- Suprapatellar pouch: Synovial assessment and loose body detection
- Shoulder Arthroscopy Examination Protocol
- Glenohumeral joint: Labral integrity and cartilage assessment
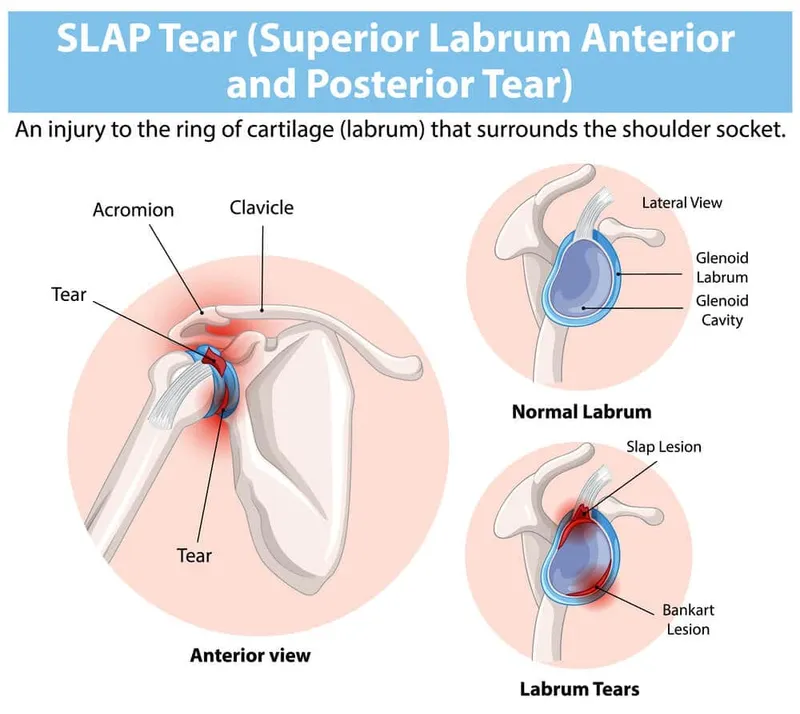
- SLAP lesions: Superior labral anterior-posterior tears
- Bankart lesions: Anterior-inferior labral detachment
- Hill-Sachs lesions: Posterior humeral head compression fractures
- Subacromial space: Rotator cuff evaluation and impingement assessment
- Partial-thickness tears: Articular vs bursal surface involvement
- Full-thickness tears: Size measurement in centimeters
- Acromion morphology: Type I-III classification
- Glenohumeral joint: Labral integrity and cartilage assessment
Pathology Recognition and Grading
| Structure | Normal Appearance | Grade 1 Changes | Grade 2 Changes | Grade 3 Changes | Grade 4 Changes |
|---|---|---|---|---|---|
| Cartilage | Smooth, white | Softening | Fibrillation | Fissuring | Bone exposure |
| Meniscus | Smooth, white | Degeneration | Partial tear | Complete tear | Complex tear |
| Synovium | Thin, pink | Mild thickening | Moderate hypertrophy | Severe inflammation | Villous formation |
| Ligament | Tight, intact | Mild laxity | Partial tear | Complete tear | Avulsion |
💡 Master This: Dynamic examination under varus/valgus stress reveals meniscal instability and ligament laxity not apparent during static visualization. Stress testing during arthroscopy changes treatment decisions in 20-25% of cases.
Advanced Diagnostic Techniques: Microfracture bleeding response indicates subchondral bone viability, while synovial biopsy provides histological diagnosis for inflammatory arthropathies. Intra-articular injection of local anesthetic during arthroscopy confirms pain source in complex cases.
Documentation Standards: Photographic documentation of all compartments and pathological findings provides medicolegal protection and surgical planning reference. Video recording captures dynamic instability and treatment response for educational purposes and quality assurance.
Correlation with Imaging: MRI correlation reveals sensitivity and specificity limitations, with arthroscopy detecting additional pathology in 15-25% of cases. Meniscal tears, cartilage lesions, and loose bodies are underestimated by MRI in 10-20% of patients.
Understanding diagnostic arthroscopy principles transforms joint examination from limited external assessment to comprehensive internal evaluation. Master systematic examination protocols, and you possess the foundation for accurate diagnosis and optimal treatment planning.
🔍 Diagnostic Arthroscopy: The Joint Detective Work
⚡ Therapeutic Arthroscopy: The Precision Repair Arsenal
📌 Remember: REPAIR - Remove damaged tissue, Evaluate remaining structures, Plan reconstruction, Anatomical restoration, Implant fixation, Rehabilitation protocol
Arthroscopic Therapeutic Techniques
- Meniscal Surgery Procedures
- Partial meniscectomy: Stable rim preservation with minimal tissue removal
- Success rate: 85-90% symptom relief
- Tissue removal: <25% of meniscal volume
- Technique: Smooth, stable edges without sharp transitions
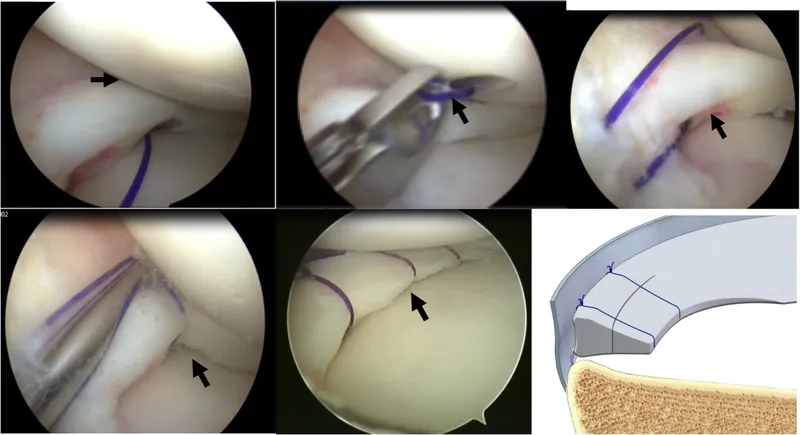
- Meniscal repair: Peripheral tears within vascular zone
- Healing rate: 80-90% for red-red zone tears
- Suture techniques: Inside-out, outside-in, all-inside methods
- Indications: Tears <10mm from peripheral rim
- Meniscal transplantation: Massive meniscal deficiency with intact ACL
- Survival rate: 75-85% at 10 years
- Size matching: ±5% of native meniscal dimensions
- Partial meniscectomy: Stable rim preservation with minimal tissue removal
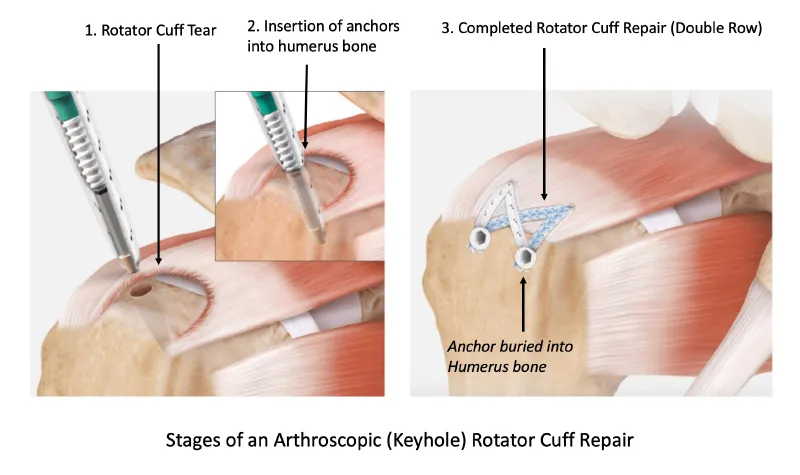
- Rotator Cuff Repair Techniques
- Single-row repair: Simple suture anchor fixation
- Indications: Small tears <2cm
- Anchor placement: 5-10mm from articular margin
- Success rate: 85-90% for small tears
- Double-row repair: Anatomical footprint restoration
- Indications: Medium-large tears 2-5cm
- Biomechanical advantage: 40-50% increased contact area
- Success rate: 90-95% for medium tears
- Transosseous-equivalent: Medial-lateral compression with anatomical restoration
- Indications: Large tears >3cm
- Technique: Medial anchors with lateral compression
- Single-row repair: Simple suture anchor fixation
Advanced Therapeutic Procedures
| Procedure | Success Rate | Recovery Time | Complication Rate | Return to Sport | Long-term Outcomes |
|---|---|---|---|---|---|
| ACL Reconstruction | 90-95% | 6-9 months | 5-8% | 85-90% | 90% at 10 years |
| Meniscal Repair | 80-90% | 3-4 months | 3-5% | 90-95% | 85% at 5 years |
| Rotator Cuff Repair | 85-95% | 4-6 months | 5-10% | 80-85% | 80% at 10 years |
| Labral Repair | 85-90% | 3-4 months | 8-12% | 75-80% | 75% at 5 years |
| Cartilage Restoration | 70-80% | 6-12 months | 10-15% | 60-70% | 70% at 5 years |
💡 Master This: Anatomical restoration of native tissue footprints and biomechanical properties determines long-term success. Non-anatomical repairs have 20-30% higher failure rates regardless of surgical technique quality.
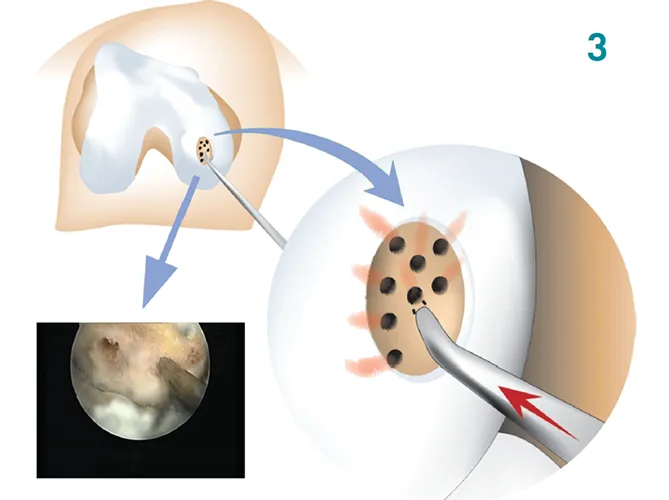
Cartilage Restoration Techniques: Microfracture, osteochondral autograft (OATS), and autologous chondrocyte implantation (ACI) address full-thickness cartilage defects with size-specific indications. Microfracture for lesions <2cm², OATS for 2-4cm², and ACI for >4cm² defects.
Suture Anchor Technology: Modern anchors provide pullout strength >300N with bioabsorbable materials eliminating permanent implants. Knotless anchors reduce suture-related complications while maintaining equivalent fixation strength to traditional knotted repairs.
Biological Enhancement: Growth factors, stem cells, and scaffolds augment natural healing responses with 10-20% improvement in clinical outcomes. Combination therapies using multiple biological agents show synergistic effects in complex repairs.
Understanding therapeutic arthroscopy principles transforms joint surgery from tissue removal to biological restoration. Master repair techniques and biological principles, and you possess the tools for optimal patient outcomes and long-term joint preservation.
⚡ Therapeutic Arthroscopy: The Precision Repair Arsenal
🎯 Arthroscopic Mastery: The Clinical Command Center
📌 Remember: MASTER - Multisystem thinking, Adaptive techniques, Systematic approach, Tissue preservation, Evidence-based decisions, Rehabilitation integration
The Arthroscopic Decision Matrix
-
Patient Selection Optimization
- Age considerations: <40 years favor repair over debridement
- Meniscal repair: 90% success in patients <30
- Cartilage restoration: Best outcomes in patients <35
- Ligament reconstruction: Excellent results across all ages
- Activity level matching: Procedure selection based on functional demands
- High-demand athletes: Anatomical reconstruction preferred
- Recreational athletes: Simplified repairs often adequate
- Sedentary patients: Symptom relief primary goal
- Age considerations: <40 years favor repair over debridement
-
Intraoperative Decision Trees
- Unexpected pathology management: Real-time adaptation of surgical plan
- Additional tears: Extend procedure vs staged approach
- Tissue quality assessment: Repair feasibility determination
- Implant selection: Size and type based on tissue characteristics
- Unexpected pathology management: Real-time adaptation of surgical plan
Clinical Excellence Framework
| Mastery Level | Success Rate | Complication Rate | Revision Rate | Patient Satisfaction | Learning Curve |
|---|---|---|---|---|---|
| Novice | 75-80% | 8-12% | 15-20% | 80-85% | 50-100 cases |
| Competent | 85-90% | 5-8% | 8-12% | 90-92% | 100-200 cases |
| Proficient | 90-95% | 3-5% | 5-8% | 93-95% | 200-300 cases |
| Expert | 95-98% | 1-3% | 2-5% | 95-98% | >300 cases |
💡 Master This: Arthroscopic mastery combines precise technique with adaptive problem-solving - the ability to modify procedures based on intraoperative findings while maintaining optimal outcomes defines surgical expertise.
Quality Metrics and Benchmarks: Outcome tracking using validated scoring systems (IKDC, ASES, Harris Hip Score) provides objective assessment of surgical success. Benchmark comparisons with published literature ensure performance standards meet or exceed national averages.
Continuous Improvement Protocols: Regular case review, complication analysis, and technique refinement drive continuous improvement in surgical outcomes. Peer review and multidisciplinary conferences provide external validation and knowledge sharing opportunities.
Technology Integration: Advanced imaging, navigation systems, and robotic assistance enhance surgical precision while reducing learning curves. Augmented reality and 3D visualization provide enhanced spatial awareness during complex procedures.
Patient-Centered Care: Shared decision-making, realistic expectations, and comprehensive rehabilitation optimize patient satisfaction and functional outcomes. Patient education and engagement improve compliance and long-term success rates.
Understanding arthroscopic mastery principles transforms individual procedures into comprehensive patient care. Master clinical integration and adaptive expertise, and you possess the foundation for surgical excellence and optimal patient outcomes across all arthroscopic procedures.
🎯 Arthroscopic Mastery: The Clinical Command Center
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app





















