Indications & Contraindications - Gatekeeping TKA
Indications:
- Severe knee pain (often >6/10 VAS) with functional limitation, refractory to conservative treatment.
- Primary Osteoarthritis (most common)
- Rheumatoid Arthritis
- Post-traumatic Arthritis
- Avascular Necrosis (AVN) of knee
- Failed conservative measures (analgesia, physiotherapy, intra-articular injections, unicompartmental knee arthroplasty)
- Significant deformity (varus/valgus >15-20°)
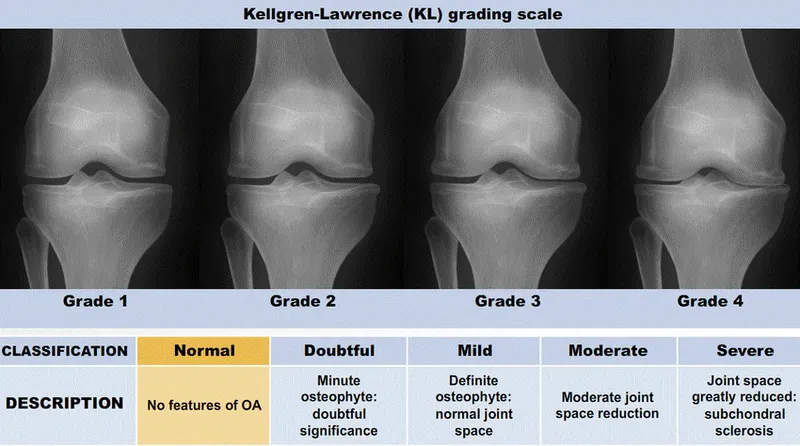
- Radiographic evidence of advanced arthritis (e.g., Kellgren-Lawrence Grade 3-4)
Contraindications:
- Absolute:
- Active knee sepsis or systemic infection
- Extensor mechanism dysfunction (e.g., patellar tendon rupture)
- Severe vascular disease (PVD)
- Neuropathic joint (Charcot knee) - relative to absolute depending on severity & stability
- Recurvatum deformity due to muscular weakness
- Relative:
- Medical instability (uncontrolled comorbidities)
- Obesity (BMI >40 kg/m²)
- Young age (<50-55 years) - risk of earlier revision
- Non-compliance with rehabilitation
- Skin conditions over the knee (e.g., psoriasis)
⭐ Exam Favourite: Active infection in the knee joint is an absolute contraindication to TKA due to the high risk of prosthetic joint infection (PJI), a devastating complication requiring prolonged antibiotics and often multiple revision surgeries.
Pre-op Planning & Biomechanics - Blueprint & Balance
- Pre-operative Assessment:
- History: Pain, functional limitation, patient expectations.
- Examination: ROM, deformity (varus/valgus), ligamentous stability, neurovascular status.
- Optimize co-morbidities.
- Radiographic Planning:
- Essential X-rays: AP, Lateral, Skyline views.
- Long leg films (scanogram): Crucial for mechanical axis & deformity assessment.
- Templating: Component sizing, alignment, bone resection levels.
- Biomechanical Goals:
- Mechanical Axis: Restore to $\mathbf{0}^\circ \pm \mathbf{3}^\circ$ (Hip → Knee → Ankle).
- Anatomical-Mechanical Angle: Femur approx. $\mathbf{6}^\circ$ valgus.
- Joint Line Restoration: Critical for patellar tracking & mid-flexion stability.
- Gap Balancing: Symmetrical, rectangular flexion & extension gaps.
- Femoral Rollback: Ensure posterior femoral translation in flexion.
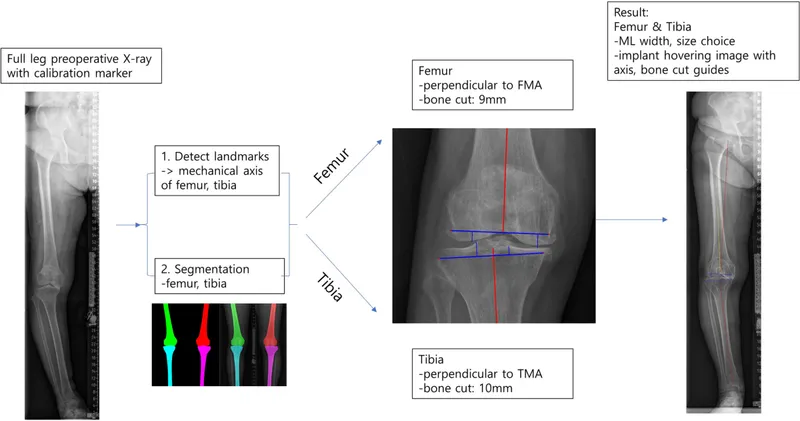
⭐ Deviation from the target mechanical axis (neutral plus or minus three degrees) significantly increases polyethylene wear and risk of aseptic loosening.
Implant Design & Surgical Steps - Nuts, Bolts & Action
Error generating content for this concept group: No object generated: the tool was not called.
Post-op Care & Complications - Recovery & Roadblocks
- Immediate Post-op:
- Mobilization: Weight bearing as tolerated (WBAT) from Day 0/1.
- DVT Prophylaxis: LMWH/DOACs for 10-35 days. Intermittent Pneumatic Compression (IPC).
- Pain Control: Multimodal analgesia (opioids, NSAIDs, regional nerve blocks).
- Wound Care: Sutures/staples out at 10-14 days; monitor for discharge/erythema.
- Rehabilitation:
- Physiotherapy: Key for Range of Motion (ROM; target 0-120° flexion), quadriceps & hamstring strengthening.
- Continuous Passive Motion (CPM): Use debated; may offer early ROM benefits.
- Complications:
- Early (<3 months):
- Infection (Superficial Site Infection [SSI], Periprosthetic Joint Infection [PJI])
- Deep Vein Thrombosis (DVT)/Pulmonary Embolism (PE)
- Stiffness (Arthrofibrosis) - consider Manipulation Under Anesthesia (MUA) if <90° flexion by 6-12 weeks.
- Periprosthetic fracture
- Wound dehiscence/hematoma
- Late (>3 months):
- Aseptic Loosening (Most common cause of late failure)
- Polyethylene Wear & Osteolysis
- Late PJI
- Instability
- Patellofemoral pain/tracking issues
- Early (<3 months):
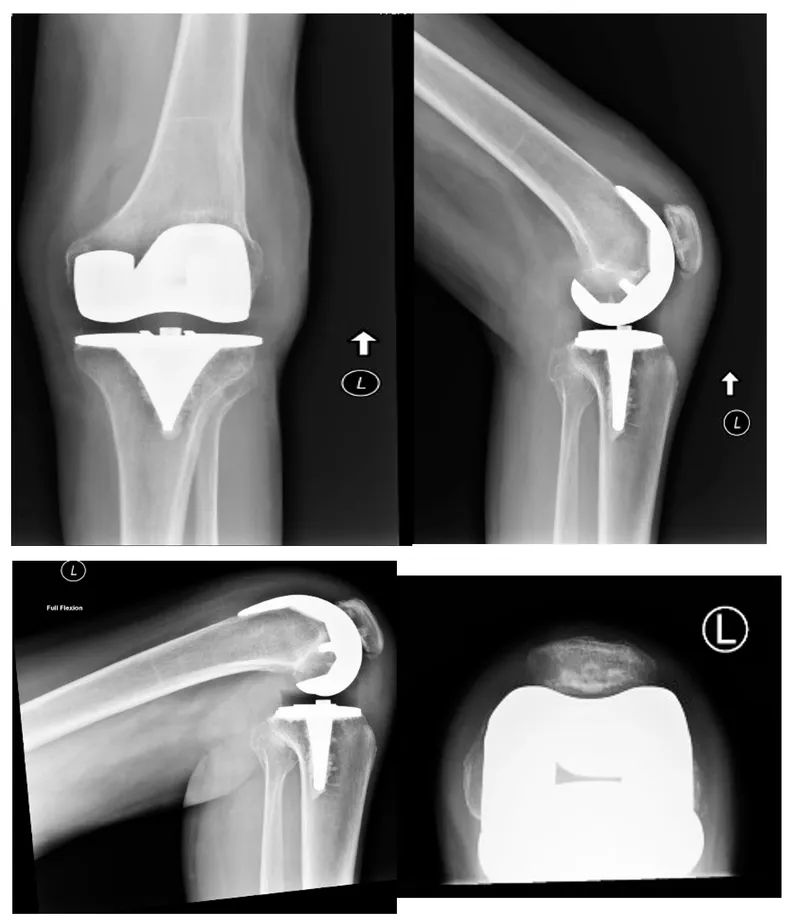
⭐ Mechanical axis alignment post-TKA within ±3° of neutral is critical for long-term implant survival and optimal function.
High‑Yield Points - ⚡ Biggest Takeaways
- Osteoarthritis (severe, tricompartmental) is the most common indication for TKA.
- Active knee sepsis and extensor mechanism dysfunction are key contraindications.
- Femoral rollback is vital for deep flexion, facilitated by PS or CR designs.
- Aim for neutral mechanical axis alignment (0°) for implant longevity.
- Patellar resurfacing is considered for anterior knee pain or patellofemoral arthritis.
- Aseptic loosening is the most common long-term complication; PJI is a serious early one.
- Cemented fixation is the gold standard, especially in older patients.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

