THA Basics - Hip Hits Reset
Total Hip Arthroplasty (THA) replaces a damaged hip joint with a prosthesis, aiming for pain relief & function restoration.
Key Indications:
- Osteoarthritis (OA) - most common
- Avascular Necrosis (AVN) - femoral head
- Displaced Neck of Femur Fracture (#NOF) - elderly, active
- Rheumatoid Arthritis (RA) - severe joint damage
- Developmental Dysplasia of Hip (DDH) - secondary OA
Contraindications:
- Absolute:
- Active sepsis
- Severe medical comorbidities (prohibitive surgical risk)
- Relative:
- Neuromuscular compromise affecting stability
- Skeletal immaturity
- Charcot joint (neuroarthropathy)
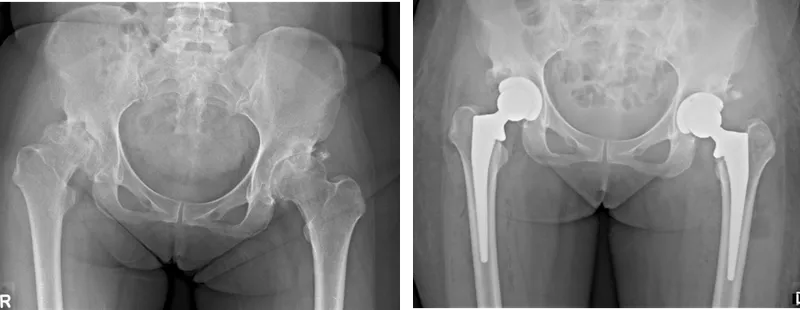
⭐ Primary osteoarthritis is the most common indication for THA.
THA Blueprint - Plan & Pathways
Pre-operative Evaluation:
- Hx: Pain, functional limitation. P/E: Harris Hip Score (HHS: <70 Poor, 70-79 Fair, 80-89 Good, 90-100 Excellent), abductor strength (Trendelenburg).
- Investigations: X-rays (AP Pelvis, Lat Hip), ESR/CRP (infection screen).
- Medical Fitness: Optimize co-morbidities (cardiac, diabetes).
Templating Goals (Digital/Analog):
- Restore biomechanical hip center of rotation.
- Achieve leg length equality.
- Optimize femoral offset & version for stability.
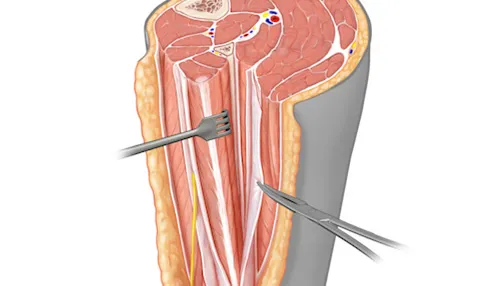
Surgical Approaches Overview:
- Posterior (Moore): Most common. Risk: Sciatic n., ↑early dislocation.
- Lateral (Hardinge): Transgluteal. Risk: Sup. gluteal n., abductor weakness.
- Anterolateral (Watson-Jones): Interval: TFL & Gluteus Medius.
- Anterior (DAA): Internervous. Risk: LFCN. Potential faster early recovery.
⭐ The posterior approach is the most commonly used worldwide but carries a higher risk of early dislocation.
THA Hardware - Parts & Performance
-
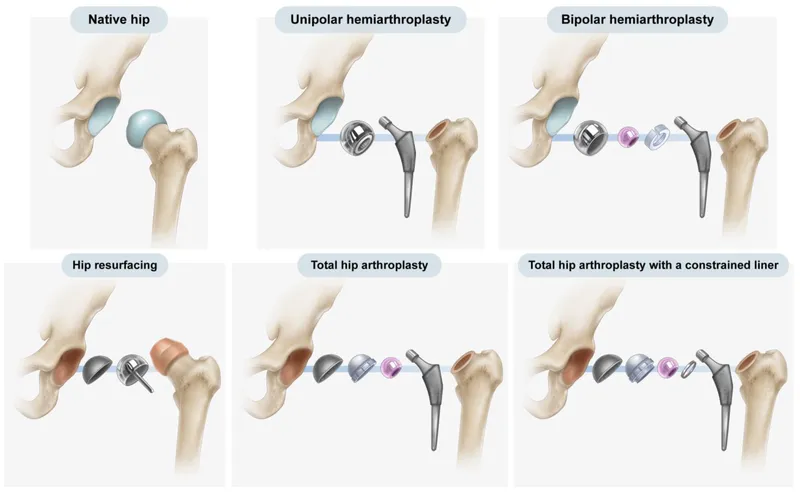
Components:
- Acetabular Cup: Ti/Co-Cr alloy; porous coating (uncemented).
- Liner: UHMWPE, Ceramic; locking mechanism.
- Femoral Stem: Ti/Co-Cr alloy; designs: tapered wedge, CPT (Collarless Polished Taper).
- Femoral Head: Ceramic (e.g., Biolox delta), Co-Cr; sizes: 28mm, 32mm, 36mm.
-
Fixation Methods:
- Cemented: Polymethylmethacrylate (PMMA). Indications: older patients, poor bone stock, irradiated bone.
- Uncemented (Press-fit): Relies on bony ingrowth. Indications: younger patients, good bone stock.
-
Bearing Surfaces: Choice impacts wear & longevity.
Surface Wear Rate Pros Cons Metal-on-Poly (MoP) Moderate Cost-effective, historical standard Polyethylene wear, osteolysis Ceramic-on-Poly (CoP) Low ↓Wear vs MoP, good biocompatibility Higher cost than MoP Ceramic-on-Ceramic (CoC) Lowest ↓↓Wear, inert, scratch-resistant Risk of fracture, squeaking, expensive Metal-on-Metal (MoM) Variable (Concerns) Allowed large heads; (Largely abandoned) Adverse Reactions to Metal Debris (ARMD), pseudotumors
⭐ Charnley's concept of low-friction arthroplasty revolutionized THA, using a small femoral head (22.225mm) and UHMWPE acetabular component, significantly reducing wear compared to previous designs.
THA Pitfalls & Fixes - Dodging Disasters
- Intra-op: Femoral/acetabular fracture, Leg Length Discrepancy (LLD), Nerve palsy (sciatic, femoral, sup. gluteal), Vascular injury, Implant malposition.
- Early Post-op (<6 wks):
- DVT/PE: Prophylaxis essential.
- PJI: Dx (MSIS criteria). Class (TSAI/Coventry). Mgmt: DAIR (acute), 1/2-stage revision (chronic).
* Dislocation: Posterior commonest. Risk factors: surgical approach, component malposition, patient factors. Closed/open reduction.
- Late Post-op (>6 wks):
- Aseptic Loosening: Most common late revision cause. Mechanisms: particle-induced osteolysis. Radiographic signs: radiolucent lines, component migration.
- Osteolysis; Implant wear/failure.
- Heterotopic Ossification (HO): Risk factors. Prophylaxis (NSAIDs, XRT). Brooker Stages I-IV.
- Periprosthetic Fracture: Vancouver Classification Types A, B1-B3, C.
⭐ Aseptic loosening is the most common cause for late revision of total hip arthroplasty.
High‑Yield Points - ⚡ Biggest Takeaways
- Primary osteoarthritis is the most common indication for THA.
- Posterior approach: most common, ↑ dislocation risk; Anterolateral: ↓ dislocation, potential abductor lurch.
- Components: acetabular cup, femoral stem & head, liner. Polyethylene wear is a key long-term issue.
- Cemented THA for older patients/poor bone stock; uncemented for younger/active individuals.
- Complications: dislocation (early), infection, periprosthetic fracture, aseptic loosening (late).
- Charnley: pioneer of low-friction arthroplasty (metal-on-polyethylene).
- Metal-on-metal bearings: risk of pseudotumors and metallosis due to ion release.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

