Revision Arthroplasty: Indications & Goals - Second Chance Surgery
- Key Indications for Revision:
- Aseptic Loosening: Most frequent; implant detaches from bone.
⭐ Aseptic loosening is the most common indication for revision Total Hip Arthroplasty (THA) and Total Knee Arthroplasty (TKA).
- Periprosthetic Joint Infection (PJI): Critical to diagnose and treat.
- Recurrent Instability/Dislocation: Leads to functional impairment.
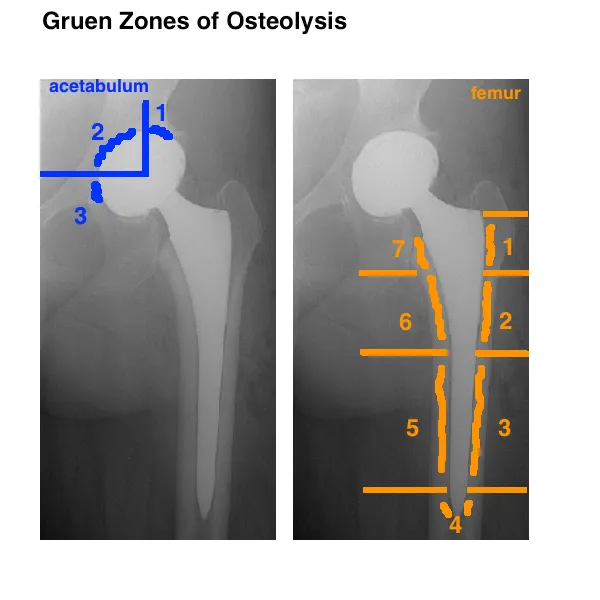
- Component Wear & Osteolysis: Material debris causes bone resorption.
- Periprosthetic Fractures: Bone fracture around the implant.
- Implant Breakage/Mechanical Failure.
- Aseptic Loosening: Most frequent; implant detaches from bone.
- Core Goals of Revision Surgery:
- Significant Pain Alleviation.
- Restoration of Joint Function and Mobility.
- Achieve a Stable, Well-fixed, and Durable Implant.
- Complete Eradication of Infection (if PJI).
- Address and Reconstruct Bone Stock Deficiency.
 oka
oka
Revision Arthroplasty: Pre-op Workup - Detective Work
- Goal: Pinpoint failure cause (septic/aseptic), assess patient, strategize surgery.
- Clinical:
- History: Pain (type, onset), prior surgeries, infection signs.
- Exam: ROM, stability, sinuses, neurovascular.
- Labs & Imaging:
- Bloods: ESR >30, CRP >10 mg/L for PJI.
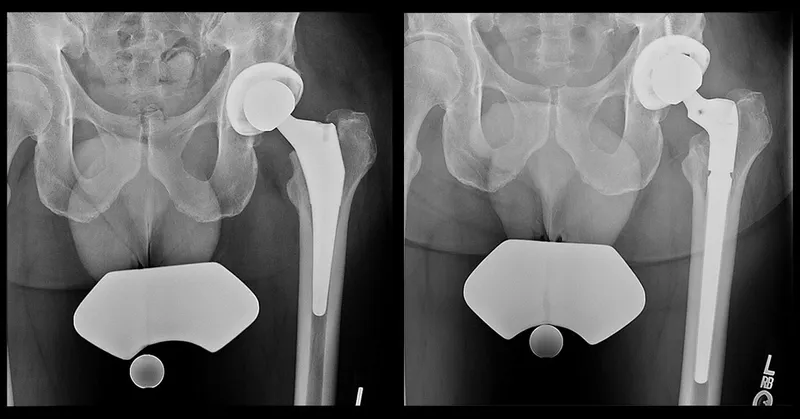
- X-rays (serial): Loosening, osteolysis, wear.
- CT/Bone Scan: Bone stock, occult issues.
- Joint Aspiration (Crucial for PJI):
- Synovial WBC >1700, PMN% >65%.
- Culture (aerobic/anaerobic).
- Alpha-defensin, Leukocyte esterase.
⭐ Pre-operative joint aspiration (cell count, culture) is vital for septic vs. aseptic failure. Hold antibiotics 2 weeks prior if PJI suspected.
- Consults: Medical, Anesthesia, ID (for PJI).
Revision Arthroplasty: Intra-op Challenges & Solutions - Battlefield Tactics
- Exposure & Implant Removal:
- Challenge: Scarring, distorted anatomy, well-fixed implants/cement.
- Solutions: Extensile approaches (e.g., Extended Trochanteric Osteotomy - ETO), specialized power tools, ultrasonic devices for cement removal, implant-specific extraction instruments.
- Bone Stock Deficiency:
- Challenge: Significant bone loss affecting implant stability and fixation.
- Solutions: Impaction Bone Grafting (IBG), structural allografts, metal augments (tantalum, titanium), porous metal cones/sleeves, custom triflange components.
- Achieving Stability & Optimal Biomechanics:
- Challenge: Ligamentous laxity, abductor insufficiency, component malposition.
- Solutions: Meticulous soft tissue balancing, constrained liners, larger femoral heads, offset/anteversion options, trial components.
- Managing Potential Infection:
- Challenge: Pre-existing or occult infection.
- Solutions: Thorough debridement, copious pulse lavage, multiple intra-operative samples, antibiotic-loaded cement/spacers (if staged).
- Intra-op Complications:
- Challenge: Iatrogenic fractures, neurovascular injury, bleeding.
- Solutions: Careful surgical technique, prophylactic cerclage, fracture fixation (plates, cables), meticulous dissection, hemostasis.
⭐ Paprosky classification (acetabulum) and AAOS/SOFCOT classification (femur) are vital for assessing bone loss and planning reconstruction in revision arthroplasty.
Revision Arthroplasty: Complications & Prognosis - The Aftermath
- Major Complications:
- Periprosthetic Joint Infection (PJI): Most feared; diagnosis crucial.
- Dislocation/Instability: ↑ risk vs primary.
- Periprosthetic fractures: Intra-op or post-op.
- Nerve palsy: e.g., peroneal (TKR), sciatic (THR).
- Aseptic loosening: Persistent concern.
- Implant wear/failure.
- Prognosis:
- Outcomes generally less favorable than primary.
- Functional recovery variable; depends on bone loss, indication for revision.
- ↑ Re-revision rates.
⭐ The risk of major complications (e.g., PJI, dislocation, nerve injury) is significantly higher in revision arthroplasty compared to primary procedures.
High‑Yield Points - ⚡ Biggest Takeaways
- Aseptic loosening: Most common reason for revision arthroplasty.
- PJI (Periprosthetic Joint Infection): Often needs two-stage revision.
- Differentiating septic vs. aseptic failure is paramount pre-operatively.
- Bone loss: A major challenge; managed with impaction grafting, augments, or allografts.
- Pre-operative planning: Essential to identify failure cause and assess bone stock.
- Instability, component malposition, and periprosthetic fractures are other key indications.
- Wear debris (e.g., polyethylene) leads to osteolysis and subsequent implant failure.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

