Biomaterials Basics - Body's Best Friends?
- Biomaterial: Non-viable material in a medical device, interacting with biological systems.
- Biocompatibility: Material performs with appropriate host response in a specific application.
- Crucial: Non-toxic, non-immunogenic, non-carcinogenic.
- Resists corrosion, degradation, wear. E.g., Ti, $Al_2O_3$.
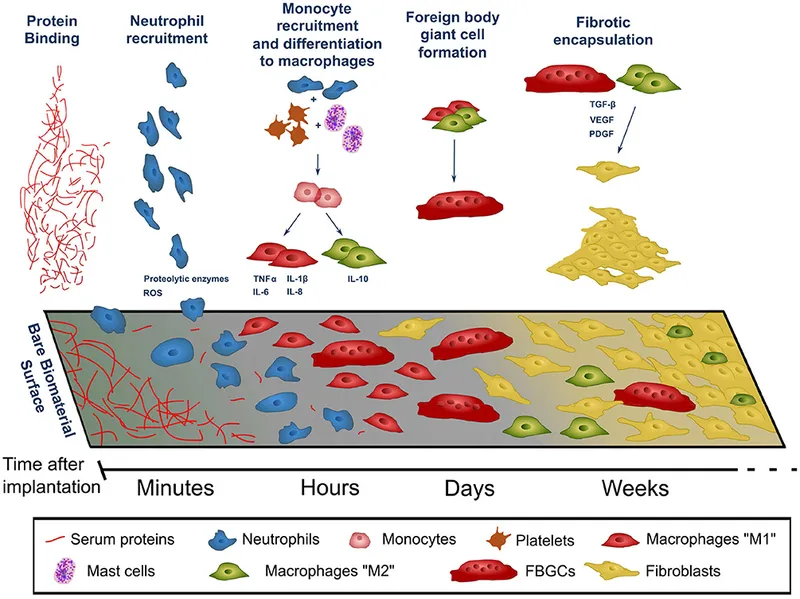
- Host Response Sequence:
- Injury → Acute Inflam. → Chronic Inflam. → Granulation → FBR (FBGCs) → Fibrous Encapsulation.
- Key Material Attributes:
- Mechanical (Young's modulus matching bone).
- Surface properties (bioactive/inert).
- Sterilizability.
⭐ Bioinert materials seek minimal host reaction for stable fibrous encapsulation, vital for implant longevity.
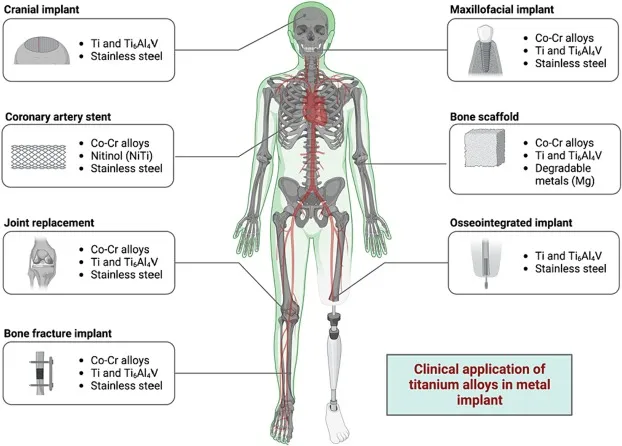
Metallic Implants - Strong & Shiny
- Types: Stainless Steel (SS 316L), Cobalt-Chromium (Co-Cr), Titanium (Ti) alloys.
- Properties: High strength, ductile, fracture toughness. Passivation layer for corrosion resistance.
- SS 316L: Fe-Cr-Ni-Mo. Trauma implants. Risk: Ni allergy.
- Co-Cr: High wear/corrosion resistance. Bearing surfaces (femoral heads).
- Risks: Metal ion release (Co, Cr) → metallosis, ALVAL.
- Ti-alloys (Ti-6Al-4V): ↓Modulus (↓stress shielding), biocompatible, osseointegration. For stems, porous coatings.
- Poor articular wear.
⭐ Ti-6Al-4V's lower Young's modulus (
110 GPa) is closer to bone (10-30 GPa), reducing stress shielding.
Polymeric Implants - Plastic & Paste
- UHMWPE (Ultra-High Molecular Weight Polyethylene)
- Primary bearing surface; low friction, high wear resistance.
- Cross-linked PE (XLPE): ↑ wear resistance, but may ↓ fracture toughness. Vitamin E added to ↓ oxidation & improve longevity.
- Sterilization: Gas plasma or Ethylene Oxide (EtO) preferred over gamma irradiation in air to minimize oxidative degradation.
- Wear particles (0.1-1 µm) → macrophage activation → periprosthetic osteolysis.
- PMMA (Polymethylmethacrylate) Bone Cement
- Acrylic polymer; exothermic polymerization (setting time ~8-15 min).
- Components: Powder (PMMA beads, Benzoyl Peroxide initiator, BaSO₄/ZrO₂ radiopacifier) & Liquid (MMA monomer, DMPT accelerator, Hydroquinone inhibitor).
- Function: Mechanical interlock (grout), not an adhesive.
- Antibiotic-loaded cement (e.g., gentamicin, tobramycin) used for infection prophylaxis/treatment.
- ⭐ > Bone Cement Implantation Syndrome (BCIS) is a critical intraoperative risk characterized by hypoxia, hypotension, arrhythmias, and/or cardiac arrest.
Ceramic Implants - Smooth Operators
- Materials: Alumina ($Al_2O_3$), Zirconia ($ZrO_2$), Biolox Delta (Alumina-Zirconia composite).
- Key Advantages:
- Lowest coefficient of friction → ultra-low wear rates.
- Excellent biocompatibility, high hardness, scratch resistance.
- Key Disadvantages:
- Brittle nature → potential for fracture (though modern ceramics are tougher).
- Audible squeaking (rare).
- Higher cost.
- Common Bearings: Ceramic-on-Ceramic (CoC), Ceramic-on-Polyethylene (CoP).
⭐ CoC bearings offer the lowest wear rates among common arthroplasty options but carry a small risk of catastrophic fracture. oka
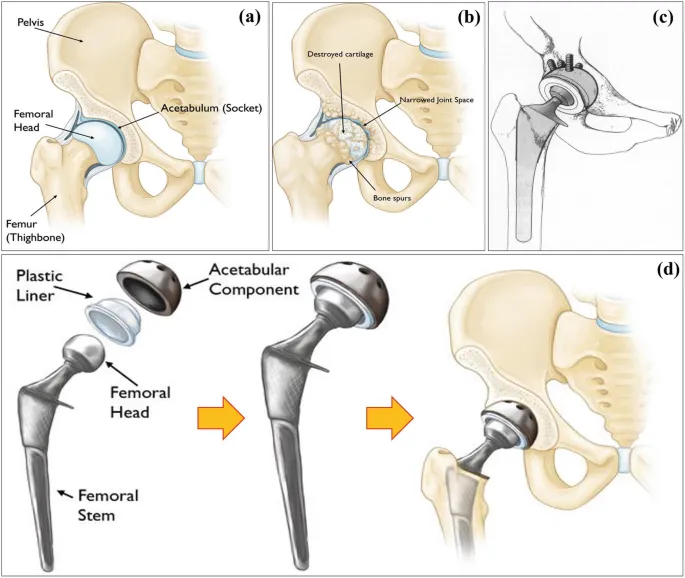
Implant Design & Fixation - Sticking Around
- Goal: Achieve primary (initial) & secondary (long-term) stability.
- Cemented Fixation (PMMA):
- Mechanical interlock (grout).
- Pros: Immediate stability, suits osteoporotic bone.
- Cons: Debris, thermal necrosis, interface failure.
- Cementless (Biological) Fixation:
- Osseointegration (bone ingrowth/ongrowth).
- Requires porous-coated surfaces (e.g., sintered beads, HA).
- Pros: Durable, biological interface.
- Cons: Needs good bone stock, press-fit crucial.
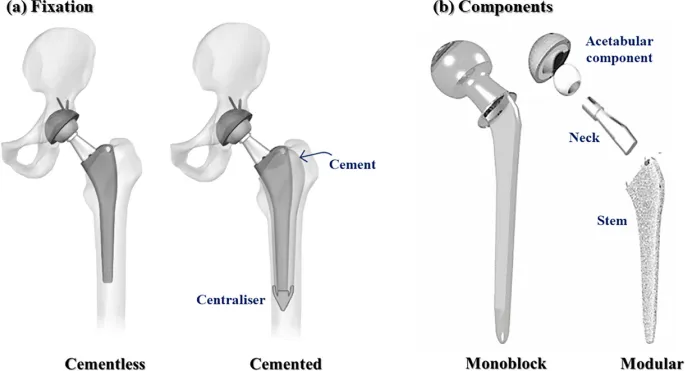
⭐ Cementless stems often feature proximal porous coating for metaphyseal bone ingrowth, ensuring stable long-term fixation.
High‑Yield Points - ⚡ Biggest Takeaways
- UHMWPE: most common bearing surface; key issues are wear and subsequent osteolysis.
- XLPE (Cross-linked Polyethylene): significantly ↓ wear versus UHMWPE, but potential for ↓ fracture toughness.
- Cobalt-Chromium (CoCr) alloys: used for femoral heads/cups due to high strength and corrosion resistance.
- Titanium (Ti) alloys: preferred for stems due to bone-like stiffness (↓ stress shielding) and excellent biocompatibility.
- Ceramic-on-Ceramic (CoC): lowest wear rates; risks include fracture and audible squeaking.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more