Elbow Arthroplasty - Joint Journey Kickoff
- Definition: Surgical replacement of elbow joint with artificial components (prosthesis).
- Goals: ↓Pain, ↑Range of Motion (ROM), ↑Function.
- Types:
- Total Elbow Arthroplasty (TEA): Replaces both humeral and ulnar articular surfaces.
- Hemiarthroplasty: Replaces one surface (e.g., radial head, distal humerus).
- Key Indications:
- Severe arthritis (Rheumatoid Arthritis, Osteoarthritis, Post-traumatic)
- Comminuted distal humerus fractures (elderly, low-demand patients)
- Non-union/malunion of distal humerus
- Failed previous elbow surgery
⭐ Rheumatoid arthritis is the most common indication for total elbow arthroplasty, though post-traumatic arthritis is increasingly common.
Elbow Arthroplasty - Choosing Your Champion
- Prosthesis Types & Selection Factors:
- Unlinked (Resurfacing):
- For good bone stock, intact ligaments, younger active patients.
- Preserves bone, more physiological motion.
- Risk: Instability.
- Linked (Semi-constrained):
- For poor bone stock, ligamentous insufficiency, older/low-demand patients, revision cases.
- Provides inherent stability.
- Most common.
- Linked (Constrained):
- Historical, rarely used due to ↑ loosening.
- Unlinked (Resurfacing):

⭐ Linked (semi-constrained) prostheses are generally preferred in patients with poor bone stock or ligamentous insufficiency to provide inherent stability.
Elbow Arthroplasty - Navigating the Nerves
- Ulnar Nerve: Highest risk; lies posterior to medial epicondyle.
- Crucial: meticulous identification, gentle handling, and protection.
- Prophylactic anterior transposition often performed to reduce tension/compression.
- Radial Nerve: Vulnerable with anterior/anterolateral surgical approaches.
- Located anterior to the lateral epicondyle, near the radiocapitellar joint.
- Injury can result in wrist drop and supinator muscle weakness.
- Median Nerve: Less frequently injured but at risk.
- Risk during extensive anterior exposure; courses medial to the biceps tendon and brachial artery.
⭐ Routine ulnar nerve identification and protection (often involving anterior transposition) is critical during elbow arthroplasty to prevent postoperative neuropathy.
Elbow Arthroplasty - Dodging the Dangers
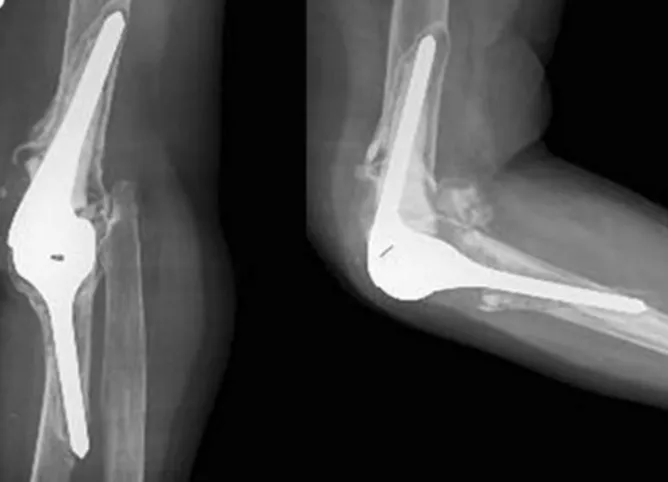
- Key Complications:
- Infection: Early (<3 mo) vs. Late. Aggressive treatment.
- Nerve Injury: Ulnar nerve (📌). Monitor; consider exploration.
- Aseptic Loosening: Ulnar component. Pain, instability → revision.
- Periprosthetic Fracture: Intra/post-op. Manage by type/stability.
- Instability: Balance ligaments, ensure component position.
- Triceps Insufficiency: Weak extension. Repair/reconstruct.
- Wear & Osteolysis: Polyethylene wear → bone loss.
⭐ Aseptic loosening, particularly of the ulnar component, is the most common long-term complication leading to revision of total elbow arthroplasty.
Elbow Arthroplasty - Beyond the Horizon

- Prognosis & Outcomes:
- Good pain relief & functional improvement.
- Implant survival: ~80-90% at 10 years.
- Lifelong activity modification crucial.
- Complications Leading to Revision:
- Aseptic loosening (most common).
- Infection.
- Periprosthetic fracture.
- Implant wear/breakage.
- Revision Arthroplasty:
- Technically demanding.
- Higher complication rates than primary TEA.
- Outcomes generally inferior to primary.
⭐ Patients undergoing total elbow arthroplasty are typically advised a permanent lifting restriction of 5-10 lbs (2-5 kg) to maximize implant longevity.
High‑Yield Points - ⚡ Biggest Takeaways
- TEA indications: inflammatory arthritis (e.g., Rheumatoid Arthritis), elderly comminuted distal humerus fractures, and severe post-traumatic arthritis.
- Hemiarthroplasty is an option for distal humerus fractures with intact collateral ligaments and stable ulna.
- Key contraindications include active infection, inadequate soft tissue envelope, neuropathic joint, and non-compliance.
- Common complications: infection (highest rate), aseptic loosening, ulnar neuropathy, and periprosthetic fractures.
- Linked (constrained) implants offer stability but ↑stress and loosening; unlinked (unconstrained) require good ligaments, risk ↑dislocation.
- Lifelong activity restrictions (e.g., lifting <2-5 kg) are crucial post-TEA to prevent implant failure.
- TEA generally has higher revision rates and lower long-term survivorship compared to hip or knee arthroplasty.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more


