Arthroplasty

On this page
🔧 Arthroplasty: The Joint Replacement Revolution
Arthroplasty transforms lives by replacing damaged joints with precision-engineered implants, but success hinges on mastering biomechanical principles, recognizing which patients benefit most, and selecting the right prosthesis for each clinical scenario. You'll learn how surgeons integrate material science, anatomical restoration, and evidence-based protocols to achieve durable outcomes while navigating complications like infection, loosening, and instability. This lesson builds your clinical reasoning from implant mechanics through decision algorithms, equipping you to understand when joint replacement offers the best solution and how surgical technique determines long-term function.
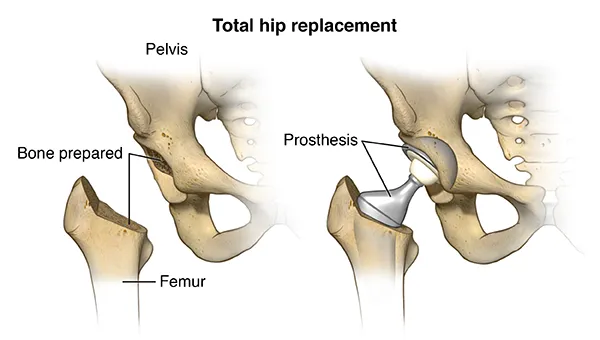
🦴 Foundation Arsenal: Joint Replacement Fundamentals
Arthroplasty represents the definitive surgical intervention for end-stage joint disease, involving complete or partial replacement of damaged joint surfaces with prosthetic components. This procedure addresses >95% of severe arthritis cases when conservative management fails, affecting >1 million patients annually in the United States alone.
📌 Remember: PARTS - Prosthetic replacement, Arthritis indication, Restoration of function, Total or partial, Surgical precision required. Each component must achieve <2mm positioning tolerance for optimal 15-20 year survival rates.
The fundamental principle involves mechanical restoration of joint biomechanics through precise component positioning, optimal soft tissue balancing, and durable fixation methods. Success depends on achieving anatomical alignment within 3° of normal, maintaining joint line restoration within 5mm, and ensuring component stability under 3000+ loading cycles daily.
- Primary Arthroplasty Categories
- Total Joint Replacement: Complete joint surface replacement (85% of procedures)
- Hip arthroplasty: >450,000 annually in US
- Knee arthroplasty: >750,000 annually in US
- Shoulder arthroplasty: >70,000 annually in US
- Partial Joint Replacement: Selective surface replacement (15% of procedures)
- Unicompartmental knee: 10-15% of knee replacements
- Hemiarthroplasty hip: 20% of hip replacements
- Resurfacing procedures: <5% of total volume
- Total Joint Replacement: Complete joint surface replacement (85% of procedures)
⭐ Clinical Pearl: Weight-bearing joints (hip, knee, ankle) demonstrate 2-3x higher revision rates compared to non-weight-bearing joints (shoulder, elbow) due to increased mechanical stress and wear particle generation. Hip replacements show >95% 10-year survival, while ankle replacements achieve 85-90% 10-year survival.
| Joint Type | 10-Year Survival | 20-Year Survival | Annual Volume (US) | Revision Rate | Primary Indication |
|---|---|---|---|---|---|
| Hip THA | 95-98% | 85-90% | 450,000 | 8-12% | Osteoarthritis (75%) |
| Knee TKA | 90-95% | 80-85% | 750,000 | 10-15% | Osteoarthritis (85%) |
| Shoulder TSA | 85-92% | 75-85% | 70,000 | 15-20% | Osteoarthritis (60%) |
| Ankle TAA | 85-90% | 70-80% | 8,000 | 20-25% | Osteoarthritis (45%) |
| Elbow TEA | 80-88% | 65-75% | 3,000 | 25-30% | Rheumatoid arthritis (50%) |
The biomechanical foundation requires understanding load transmission patterns, wear mechanisms, and fixation biology. Hip joints experience 3-5x body weight during normal walking, while knee joints encounter 6-8x body weight during stair climbing. These forces demand precise component alignment and optimal material selection to minimize wear particle generation and osteolysis progression.
Understanding these foundational principles establishes the framework for exploring the sophisticated mechanisms that enable successful joint replacement outcomes.
🔧 Arthroplasty: The Joint Replacement Revolution
⚙️ Biomechanical Engineering: The Precision Mechanics
🔬 Tribological Mastery: Wear and Friction Control
Tribology governs implant longevity through friction, wear, and lubrication mechanisms. Modern bearing surfaces achieve wear rates <0.1mm/year through advanced material engineering and optimal surface geometry. Polyethylene wear remains the primary failure mechanism, generating >10^9 particles annually in poorly designed interfaces.
📌 Remember: WEAR - Wear particles cause osteolysis, Elevated friction increases loosening, Adhesive wear dominates early phases, Roughness amplifies particle generation. Surface roughness >0.05μm increases wear rates 10-fold compared to polished surfaces <0.02μm.
- Bearing Surface Combinations
- Metal-on-Polyethylene: Standard of care (70% of implants)
- Wear rate: 0.1-0.2mm/year with conventional PE
- Highly cross-linked PE: 50-80% wear reduction
- Osteolysis threshold: >0.1mm/year wear rate
- Ceramic-on-Ceramic: Ultra-low wear (15% of implants)
- Wear rate: <0.005mm/year with alumina
- Fracture risk: 0.02% with modern ceramics
- Squeaking incidence: 1-5% of cases
- Metal-on-Metal: Historical option (<5% current use)
- Wear rate: 0.001-0.05mm/year initially
- Ion release: Cobalt >7μg/L indicates concern
- Pseudotumor formation: 8-12% incidence
- Metal-on-Polyethylene: Standard of care (70% of implants)
⭐ Clinical Pearl: Component positioning errors >5° increase wear rates 2-4x and reduce implant survival by 30-50%. Cup inclination 40-45° and anteversion 15-25° optimize wear performance while maintaining stability. Stem alignment within 3° of anatomical axis prevents stress concentration and early loosening.
| Material Combination | Linear Wear Rate | Volumetric Wear | Osteolysis Risk | Cost Factor | Primary Advantage |
|---|---|---|---|---|---|
| CoCr-XLPE | 0.05-0.1mm/yr | 20-40mm³/yr | Low (5-10%) | 1.0x | Proven durability |
| Ceramic-Ceramic | <0.005mm/yr | <1mm³/yr | Minimal (<2%) | 2.5x | Ultra-low wear |
| CoCr-Conventional PE | 0.15-0.25mm/yr | 60-120mm³/yr | High (20-30%) | 0.8x | Cost effectiveness |
| Metal-Metal | 0.001-0.05mm/yr | 1-10mm³/yr | Variable (5-25%) | 1.8x | Low wear initially |
| Ceramic-XLPE | 0.02-0.08mm/yr | 10-30mm³/yr | Low (3-8%) | 1.5x | Balanced performance |
Fixation biomechanics involves load transfer from prosthetic components to host bone through mechanical interlock or biological integration. Cemented fixation provides immediate stability through polymethylmethacrylate (PMMA) with compressive strength >70 MPa. Cementless fixation achieves biological integration through bone ingrowth requiring initial stability <150μm micromotion.
These biomechanical principles create the foundation for understanding how surgeons apply these concepts in clinical pattern recognition and decision-making frameworks.
⚙️ Biomechanical Engineering: The Precision Mechanics
🎯 Clinical Decision Matrix: Pattern Recognition Mastery
🔍 Patient Selection Architecture: The Candidacy Framework
Systematic patient evaluation determines surgical candidacy through evidence-based criteria balancing functional improvement potential against complication risks. Success rates >95% depend on optimal patient selection using validated assessment tools and risk stratification protocols.
📌 Remember: IDEAL - Indications met completely, Disease severity appropriate, Expectations realistic, Activity level suitable, Life expectancy adequate. Patients >80 years show equivalent outcomes to younger patients when medically optimized and functionally appropriate.
- Primary Indications Hierarchy
- Absolute Indications (>95% success probability)
- Severe pain with VAS >7/10 despite optimal medical management
- Functional limitation preventing activities of daily living
- Radiographic evidence of end-stage arthritis (Kellgren-Lawrence Grade 4)
- Relative Indications (80-90% success probability)
- Moderate pain with VAS 5-7/10 and activity limitation
- Progressive deformity affecting joint mechanics
- Recurrent joint instability despite conservative treatment
- Controversial Indications (60-80% success probability)
- Young patients <50 years with high activity demands
- Inflammatory arthritis with active disease
- Post-traumatic arthritis with bone deficiency
- Absolute Indications (>95% success probability)
⭐ Clinical Pearl: Patient age alone does not determine surgical candidacy. Physiological age, bone quality, activity level, and life expectancy provide better predictors of surgical success. Patients >90 years demonstrate equivalent pain relief and functional improvement compared to younger cohorts when appropriately selected.

| Risk Factor | Low Risk | Moderate Risk | High Risk | Relative Risk Increase | Mitigation Strategy |
|---|---|---|---|---|---|
| Age | <75 years | 75-85 years | >85 years | 1.5-2.0x | Medical optimization |
| BMI | <30 kg/m² | 30-35 kg/m² | >35 kg/m² | 2.0-3.0x | Weight reduction |
| ASA Score | ASA 1-2 | ASA 3 | ASA 4 | 3.0-5.0x | Perioperative management |
| Bone Quality | T-score >-1 | T-score -1 to -2.5 | T-score <-2.5 | 1.5-2.5x | Osteoporosis treatment |
| Activity Level | Sedentary | Moderate | High impact | 2.0-4.0x | Activity modification |
Implant selection algorithms integrate patient factors, surgeon experience, and evidence-based outcomes to optimize component choice. Cemented fixation suits patients >70 years with osteoporotic bone, while cementless fixation benefits younger patients with good bone quality and long life expectancy.
These pattern recognition frameworks enable surgeons to systematically analyze complex clinical scenarios and make evidence-based treatment decisions.
🎯 Clinical Decision Matrix: Pattern Recognition Mastery
⚖️ Comparative Analysis: Implant Selection Science
🔬 Material Science Discrimination: The Performance Matrix
Implant material selection determines long-term survival through wear characteristics, biocompatibility, and mechanical properties. Evidence-based selection requires understanding tribological performance, biological response, and failure mechanisms across diverse patient populations and activity levels.
📌 Remember: METALS - Mechanical strength superior, Electrolytic corrosion risk, Titanium biocompatible, Alloy composition critical, Long-term ion release, Stiffness mismatch potential. Titanium alloys demonstrate 40% lower elastic modulus compared to stainless steel, reducing stress shielding by 25-30%.
- Metallic Implant Categories
- Titanium Alloys (Ti-6Al-4V standard)
- Elastic modulus: 110 GPa (closest to bone 15-30 GPa)
- Corrosion resistance: Excellent with passive oxide layer
- Biocompatibility: Superior with <1% allergic reactions
- Fatigue strength: >500 MPa at 10^7 cycles
- Cobalt-Chromium Alloys (CoCrMo standard)
- Elastic modulus: 210 GPa (2x stiffer than titanium)
- Wear resistance: Superior for bearing surfaces
- Corrosion resistance: Excellent in physiological environment
- Hardness: 450-550 HV (2x harder than titanium)
- Stainless Steel (316L historical)
- Elastic modulus: 200 GPa with significant stress shielding
- Corrosion susceptibility: Higher than modern alloys
- Cost advantage: 30-40% lower than premium alloys
- Current use: <5% of modern implants
- Titanium Alloys (Ti-6Al-4V standard)
⭐ Clinical Pearl: Modulus mismatch between implant and bone creates stress shielding, leading to bone resorption and implant loosening. Titanium's lower modulus reduces stress shielding by 40-50% compared to stainless steel, improving long-term fixation and bone preservation.
| Material Property | Titanium Ti-6Al-4V | CoCr Alloy | Ceramic Al2O3 | UHMWPE | Bone (Cortical) |
|---|---|---|---|---|---|
| Elastic Modulus (GPa) | 110 | 210 | 380 | 0.8 | 15-30 |
| Yield Strength (MPa) | 880 | 450 | 400 | 21 | 100-200 |
| Fatigue Limit (MPa) | 500 | 300 | 200 | 15 | 50-100 |
| Density (g/cm³) | 4.4 | 8.3 | 3.9 | 0.94 | 1.8-2.0 |
| Wear Rate (mm³/Nm×10⁻⁶) | 1-10 | 0.1-1 | 0.01-0.1 | 1-100 | N/A |
Fixation method selection depends on patient age, bone quality, activity level, and surgeon preference. Cemented fixation provides immediate stability and excellent outcomes in patients >70 years, while cementless fixation offers biological integration and potential longevity in younger patients with adequate bone stock.
-
Cemented Fixation Advantages
- Immediate stability with <50μm micromotion
- Excellent outcomes in osteoporotic bone
- Lower initial cost by 15-20%
- Proven longevity with >20-year data
-
Cementless Fixation Advantages
- Biological integration through bone ingrowth
- No cement-related complications (fat embolism, thermal necrosis)
- Easier revision surgery without cement removal
- Potential for unlimited longevity with successful osseointegration
These comparative analyses provide the foundation for understanding evidence-based treatment algorithms and clinical decision-making protocols.
⚖️ Comparative Analysis: Implant Selection Science
🏥 Treatment Algorithms: Evidence-Based Protocols
🎯 Surgical Protocol Mastery: The Execution Framework
Evidence-based protocols standardize surgical decision-making through validated algorithms that optimize patient outcomes and minimize complications. Protocol adherence improves surgical efficiency by 25-30% and reduces complications by 40-50% compared to non-standardized approaches.
📌 Remember: PROTOCOL - Patient optimization first, Risk assessment complete, Operative planning detailed, Technique standardized, Outcome monitoring systematic, Complications prevented, OLL follow-up structured. Standardized protocols reduce surgical time by 15-20 minutes and complication rates by 2-3%.
- Pre-operative Optimization Protocol
- Medical Clearance (100% of patients)
- Cardiac evaluation for patients >65 or risk factors
- Pulmonary function assessment if respiratory disease
- Diabetes control with HbA1c <7.5% target
- Anemia correction to Hgb >12 g/dL pre-operatively
- Infection Prevention (Zero tolerance)
- Nasal decolonization with mupirocin for MRSA carriers
- Chlorhexidine bathing 2 days pre-operatively
- Antibiotic prophylaxis within 60 minutes of incision
- Surgical site preparation with alcohol-based solutions
- Nutritional Optimization (Malnutrition screening)
- Albumin >3.5 g/dL and transferrin >200 mg/dL
- Protein supplementation if deficient
- Vitamin D >30 ng/mL for bone health
- Weight optimization if BMI >35 kg/m²
- Medical Clearance (100% of patients)
⭐ Clinical Pearl: Enhanced Recovery After Surgery (ERAS) protocols reduce hospital length of stay by 1-2 days and complications by 30-40%. Multimodal pain management, early mobilization, and optimized fluid management form the cornerstone of successful ERAS implementation.
| Protocol Component | Standard Care | ERAS Protocol | Outcome Improvement | Evidence Level | Implementation Rate |
|---|---|---|---|---|---|
| Pre-op Education | Variable | Standardized | 25% anxiety reduction | Level I | >90% |
| Pain Management | Opioid-based | Multimodal | 50% opioid reduction | Level I | >85% |
| Fluid Management | Liberal | Goal-directed | 30% complication reduction | Level II | >70% |
| Early Mobilization | POD 1-2 | Day of surgery | 1 day LOS reduction | Level I | >95% |
| Discharge Planning | Reactive | Proactive | 40% readmission reduction | Level II | >80% |
Post-operative protocols focus on rapid recovery, complication prevention, and functional restoration. Standardized pathways include pain management algorithms, mobilization schedules, and discharge criteria that optimize patient outcomes while minimizing healthcare costs.
- Post-operative Milestones
- Day 0 (Surgery day): Pain control, mobilization, DVT prophylaxis
- Day 1: Physical therapy, wound assessment, laboratory monitoring
- Day 2-3: Discharge planning, home safety evaluation, follow-up scheduling
- 2 weeks: Wound check, suture removal, early complications
- 6 weeks: Clinical assessment, radiographic evaluation, activity progression
- 3 months: Functional assessment, patient satisfaction, return to activities
These evidence-based protocols create the framework for understanding multi-system integration and advanced surgical concepts.
🏥 Treatment Algorithms: Evidence-Based Protocols
🌐 Multi-System Integration: Advanced Surgical Ecosystems
🧬 Biological Integration Networks: The Healing Cascade
Successful arthroplasty requires coordinated biological responses across multiple organ systems, integrating inflammatory cascades, bone remodeling, soft tissue healing, and neural adaptation. System integration determines long-term success through complex feedback mechanisms and adaptive responses.
📌 Remember: SYSTEMS - Surgical trauma response, Yielding inflammatory cascade, Soft tissue healing, Tissue integration, Endocrine adaptation, Metabolic demands, Sensory neural plasticity. Peak inflammatory response occurs 24-48 hours post-operatively with IL-6 levels 100-fold elevated and CRP >150 mg/L.
- Cardiovascular System Integration
- Hemodynamic Response to surgical stress
- Cardiac output increases 20-30% during perioperative period
- Systemic vascular resistance decreases 15-20% with anesthesia
- Blood loss averages 300-500 mL for hip replacement, 200-400 mL for knee replacement
- Fluid shifts require careful monitoring to prevent volume overload or hypotension
- Thromboembolism Risk Management
- VTE incidence reaches 40-60% without prophylaxis
- Mechanical prophylaxis reduces risk by 50-60%
- Chemical prophylaxis provides additional 70-80% reduction
- Duration: 10-14 days for knee, 28-35 days for hip
- Hemodynamic Response to surgical stress
⭐ Clinical Pearl: Bone remodeling following arthroplasty involves complex mechanotransduction where osteocytes sense mechanical loading and coordinate osteoblast/osteoclast activity. Wolff's Law governs adaptive remodeling with optimal loading promoting bone formation and stress shielding causing bone resorption at 5-10% annually.

| System Component | Acute Phase (0-2 weeks) | Healing Phase (2-12 weeks) | Remodeling Phase (3-24 months) | Long-term (>2 years) | Clinical Significance |
|---|---|---|---|---|---|
| Inflammatory | Peak IL-6, TNF-α | Resolution | Baseline | Surveillance | Healing coordination |
| Cardiovascular | ↑CO 20-30% | Normalization | Baseline | Improved fitness | Perioperative risk |
| Bone Metabolism | ↑Resorption | ↑Formation | Adaptive remodeling | Steady state | Implant integration |
| Neural Plasticity | Pain signals | Adaptation | Motor learning | Optimized patterns | Functional recovery |
| Immune Response | Acute activation | Regulation | Tolerance | Surveillance | Infection prevention |
Endocrine system integration involves stress hormone responses, bone metabolism regulation, and glucose homeostasis during perioperative period. Cortisol levels increase 3-5 fold during surgery and normalize over 48-72 hours. Parathyroid hormone and vitamin D metabolism influence bone healing and implant integration.
- Advanced Integration Concepts
- Mechanobiology: Loading patterns influence cellular responses and tissue adaptation
- Immunomodulation: Implant surfaces modulate immune responses and foreign body reactions
- Biofilm Formation: Bacterial adhesion and biofilm development on implant surfaces
- Wear Particle Biology: Macrophage activation and osteolysis from wear debris
These multi-system interactions create the foundation for understanding rapid mastery tools and clinical reference frameworks.
🌐 Multi-System Integration: Advanced Surgical Ecosystems
🚀 Clinical Mastery Arsenal: Rapid Reference Protocols
⚡ Essential Arsenal: The Surgeon's Toolkit
Rapid mastery requires immediate access to critical thresholds, decision algorithms, and troubleshooting protocols that enable optimal outcomes under time pressure and complex scenarios. Evidence-based reference tools reduce decision time by 40-50% and improve consistency across diverse clinical situations.
📌 Remember: ARSENAL - Anatomical landmarks critical, Radiographic parameters essential, Sizing algorithms precise, Emergency protocols ready, Numbers memorized completely, Alignment targets exact, Long-term surveillance planned. Component positioning within 5° determines 90% of long-term success.
- Critical Numerical Thresholds
- Hip Arthroplasty Parameters
- Cup inclination: 40-45° (range 35-50°)
- Cup anteversion: 15-25° (range 10-30°)
- Leg length discrepancy: <10mm acceptable
- Offset restoration: Within 5mm of contralateral
- Stem alignment: Within 3° of anatomical axis
- Knee Arthroplasty Parameters
- Mechanical axis: 0° ± 3° from neutral
- Femoral component: 5-7° valgus to anatomical axis
- Tibial slope: 3-7° posterior slope
- Joint line: Within 8mm of anatomical position
- Patellar tracking: Central without lateral tilt >5°
- Hip Arthroplasty Parameters
⭐ Clinical Pearl: Intraoperative complications require immediate recognition and systematic management. Fracture incidence ranges 1-5% depending on approach and bone quality. Immediate fixation with cables, plates, or longer stems maintains stability and prevents propagation.
| Complication | Incidence | Recognition | Immediate Management | Long-term Impact | Prevention Strategy |
|---|---|---|---|---|---|
| Intraoperative Fracture | 2-5% | Crack/displacement | Immediate fixation | Delayed healing | Gentle technique |
| Component Malposition | 5-10% | Imaging/trial | Immediate revision | Early failure | Navigation/robotics |
| Instability | 1-3% | Trial reduction | Component adjustment | Dislocation risk | Soft tissue balance |
| Nerve Injury | 0.5-2% | Motor/sensory loss | Immediate assessment | Permanent deficit | Anatomical awareness |
| Vascular Injury | <0.5% | Bleeding/hematoma | Vascular surgery | Limb threat | Careful dissection |
Emergency protocols address life-threatening complications including fat embolism syndrome, massive bleeding, and cardiovascular collapse. Fat embolism occurs in 0.5-2% of cases with mortality 5-15%. Recognition triad: respiratory distress, neurological changes, and petechial rash in 50-60% of cases.
- Rapid Assessment Tools
- Component Position Checklist: Systematic verification of alignment parameters
- Stability Testing Protocol: Range of motion and impingement assessment
- Soft Tissue Balance: Gap measurements and ligament tension
- Final Imaging: Intraoperative radiographs confirming position
Understanding these rapid mastery tools enables surgeons to execute complex procedures with confidence while maintaining optimal patient outcomes through systematic approaches and evidence-based protocols.
🚀 Clinical Mastery Arsenal: Rapid Reference Protocols
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























