Introduction & Pathogenesis - Bone's Silent Siege
- Etiology: Mycobacterium tuberculosis.
- Spread: Hematogenous from primary focus (lungs > lymph nodes).
- Pathogenesis:
- Bacilli lodge in vascular bone: vertebral bodies, metaphysis/epiphysis, synovium.
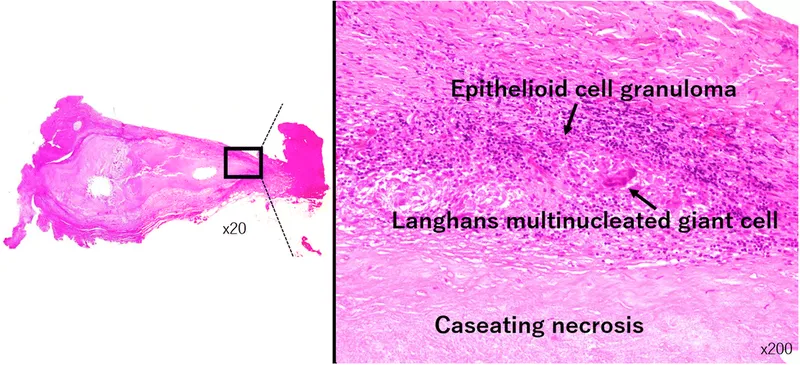
- Immune response → granuloma (epithelioid cells, Langhans cells, lymphocytes, caseous necrosis).
- Enzymatic destruction: cartilage (pannus), bone (lytic lesions).
- Results in: juxta-articular osteoporosis, cold abscess, sinus tracts.
- Common sites: Spine (Pott's disease) > Hip > Knee.
⭐ Spine (Pott's disease) is the most common site of skeletal TB.
Clinical Manifestations - TB's Crippling Clues
- General (Constitutional):
- Low-grade fever (evening rise)
- Weight loss, anorexia
- Night sweats, malaise
- Local (Affected Site):
- Pain: insidious, often worse at night (night cries in children), ↑ with activity
- Swelling: initially doughy, may progress to cold abscess
⭐ Cold abscess (lacks acute inflammation signs) is a characteristic feature of musculoskeletal TB.
- Deformity: e.g., kyphosis (Pott's spine), joint contractures
- Stiffness & ↓ range of motion (ROM)
- Muscle wasting (atrophy)
- Sinus tract formation (chronic cases)
- Site-Specific Highlights:
- Pott's Spine: Back pain, tenderness, spinal deformity (gibbus), neurological deficit (Pott's paraplegia)
- TB Hip/Knee: Limp, pain, swelling, restricted movement. oka
Diagnostic Workup - Finding TB's Footprint
- Baseline Bloods: ↑ ESR/CRP; Anemia; Lymphocytosis.
- Immunological Tests:
- Mantoux (TST): >10mm significant (HIV+ >5mm).
- IGRA (e.g., QuantiFERON-TB Gold): More specific. Both indicate exposure, not active disease.
- Imaging:
- X-ray:
- Early: Osteopenia, soft tissue swelling.
- Phemister's Triad (📌 PEM - Periarticular osteoporosis, Erosions peripherally/marginally, Slow joint space narrowing).
- Late: Destruction, deformity.

- MRI:
- Most sensitive for early changes (synovitis, marrow edema, pre-pus).
- Assesses soft tissue, abscesses, cord compression (spine).
⭐ MRI is the most sensitive imaging modality for early detection of osteoarticular TB and assessing soft tissue involvement, including pre-pus stages.
- CT Scan: Details bony destruction, sequestra.
- X-ray:
- Definitive Diagnosis (Gold Standard):
- Synovial Fluid / Pus / Tissue Biopsy:
- AFB Smear: Low sensitivity.
- Culture (LJ medium): Takes 4-6 weeks.
- NAAT (GeneXpert): Rapid, detects MTB & Rifampicin resistance.
- Histopathology (Biopsy): Caseating granulomas.
- Synovial Fluid / Pus / Tissue Biopsy:
Management Strategies - TB Treatment Triumph
- Goals: Eradicate infection, preserve function, prevent deformity.
- Cornerstone: Multi-drug Anti-Tubercular Therapy (ATT).
- 📌 RIPE Regimen: Rifampicin, Isoniazid, Pyrazinamide, Ethambutol.
- Duration: 9-12 months (paucibacillary); 12-18 months (multibacillary/spinal).
- DOTS strategy recommended.
- Supportive Care: Rest, nutrition, analgesia, physiotherapy.
- Surgical Indications:
- Biopsy for diagnosis.
- Drainage of large abscesses.
- Debridement of sequestra/infected tissue.
- Stabilization (spine/joints).
- Deformity correction.
- Salvage procedures (arthrodesis/arthroplasty) for destroyed joints.
⭐ Multi-drug anti-tubercular therapy (ATT) for an extended duration (e.g., 9-18 months depending on site/severity) is the cornerstone of treatment for bone and joint TB.
High‑Yield Points - ⚡ Biggest Takeaways
- Spine (Pott's spine) is the most common site, typically thoracolumbar junction.
- Phemister's triad (juxta-articular osteoporosis, peripheral erosions, joint narrowing) is key radiologically.
- Cold abscess formation is a hallmark; may track along fascial planes.
- Diagnosis: imaging (X-ray, MRI), biopsy/aspirate for AFB, culture, histopathology (caseating granulomas).
- Treatment: Multi-drug anti-tubercular therapy (ATT) for 9-12 months is standard.
- Watch for paradoxical worsening on ATT and gibbus deformity in spinal TB.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more