Intro & Causes - The Trigger Tale
- Reactive Arthritis (ReA): A seronegative spondyloarthropathy, an immune-mediated aseptic synovitis triggered by infection elsewhere.
- Key Triggers:
- Urogenital: Chlamydia trachomatis
- Gastrointestinal: Salmonella, Shigella, Yersinia, Campylobacter spp.
- 📌 Mnemonic (GI/GU): ShY ChiCS (Shigella, Yersinia, Chlamydia, Campylobacter, Salmonella)
- Genetic Link: Strong HLA-B27 association (↑ susceptibility, often more severe disease).
⭐ Reactive arthritis is classically an aseptic synovitis occurring after an extra-articular infection.
oka
Symptoms - Can't See, Can't Pee, Can't Climb a Tree
📌 Classic Triad: "Can't see, can't pee, can't climb a tree"
- Arthritis: Asymmetric oligoarthritis (≤ 4 joints), predominantly lower limbs. (Can't Climb a Tree)
- Dactylitis ("sausage digits").
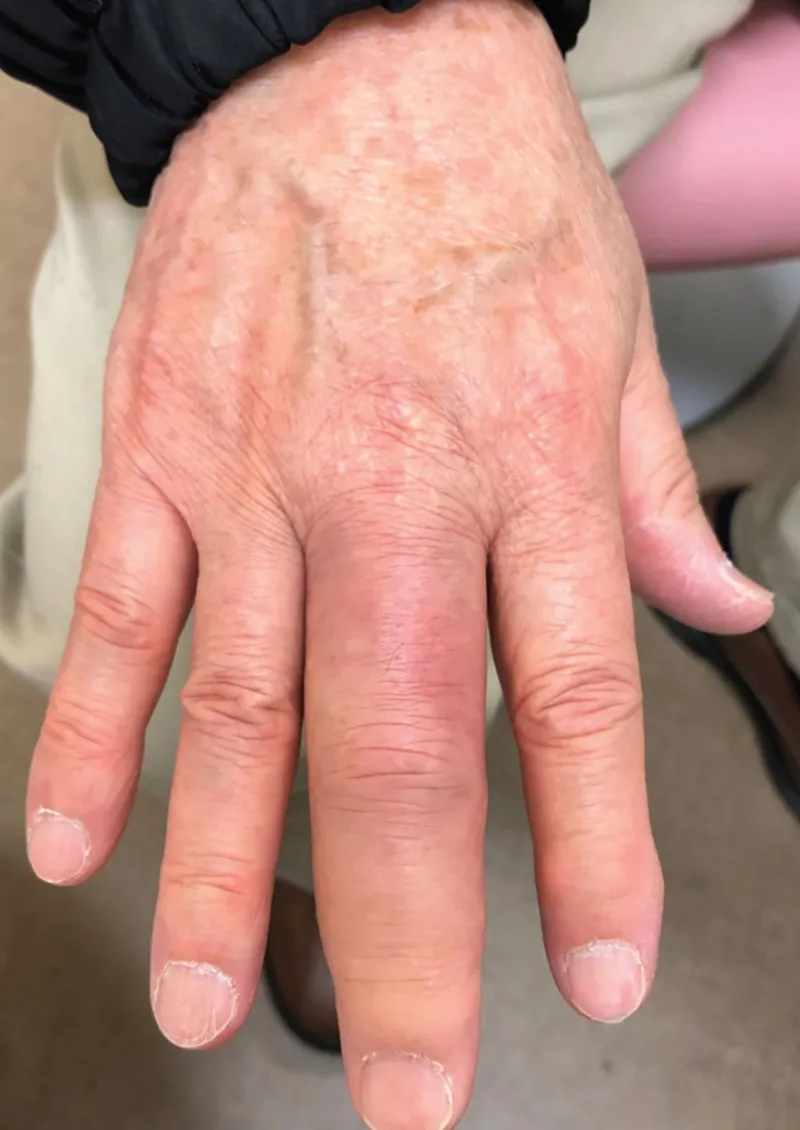
- Enthesitis (e.g., Achilles tendonitis, plantar fasciitis).
- Sacroiliitis & inflammatory low back pain.
- Dactylitis ("sausage digits").
- Urethritis/Cervicitis: Dysuria, discharge. (Can't Pee)
- Conjunctivitis/Uveitis: Eye pain, redness. (Can't See)
Extra-articular Manifestations:
- Skin: Keratoderma blenorrhagicum (palms/soles), circinate balanitis.
- Nails: Onycholysis, subungual hyperkeratosis.
- GI: Diarrhea (often preceding).
- Cardiac (rare): Aortitis, conduction abnormalities.
⭐ Dactylitis ('sausage digit') is a characteristic feature of reactive arthritis and other spondyloarthropathies.
Diagnosis - Detective Work
Primarily a clinical diagnosis; no single pathognomonic test.
-
Laboratory Findings:
- ↑ESR, ↑CRP (indicate inflammation).
- HLA-B27: Positive in 30-50% of patients.
- Synovial fluid: Inflammatory, culture-negative.
-
Imaging (X-rays):
- Features: Erosions, joint space narrowing, periostitis ('fluffy').
- Key sites: Sacroiliitis (often asymmetric), enthesophytes (e.g., heel).
-
Exclude Triggering Infections:
- Stool and urine cultures.
- Chlamydia PCR (if clinically suspected).
⭐ Synovial fluid analysis in reactive arthritis typically shows inflammatory changes (WBC 5,000-50,000/mm³) but is culture-negative.
Rule-Outs - Not That Arthritis!
| Condition | Key Differentiator vs. ReA (Sterile, Asymmetric) |
|---|---|
| Septic Arthritis | Fever, monoarticular, purulent fluid, +Gram/culture |
| Gout/Pseudogout | Crystals (urate/CPPD) in synovial fluid, acute monoarthritis |
| Psoriatic Arth. | Psoriasis, nail pitting, dactylitis, DIP involvement |
| Ankylosing Spond. | Predominantly axial (sacroiliitis), HLA-B27 >90% |
| Rheumatoid Arth. | Symmetric polyarthritis (small joints), RF/Anti-CCP +ve |
Treatment - Taming the Reaction
Goals: Relieve symptoms, eradicate active infection (if present), prevent chronic complications.
- NSAIDs: First-line for acute arthritis and enthesitis, providing symptomatic relief.
- Corticosteroids: Intra-articular or systemic for refractory symptoms unresponsive to NSAIDs.
- DMARDs: Sulfasalazine, Methotrexate for chronic or severe disease to prevent progression.
- Antibiotics: Only if active infection (e.g., Chlamydia) is proven; controversial for post-dysenteric ReA.
⭐ Antibiotics are generally not recommended for post-enteric reactive arthritis unless an active infection is proven.
- Physiotherapy: Essential for maintaining joint function and muscle strength throughout.
Outlook & Issues - The Long Haul
- Prognosis: Variable; often self-limiting (weeks/months). Chronic/recurrent in 15-30% of cases.
- Complications:
- Chronic arthritis, sacroiliitis, ankylosing spondylitis.
- Recurrent uveitis.
- Cardiac: conduction defects, aortic regurgitation.
⭐ A significant minority (15-30%) of patients with reactive arthritis may develop chronic or recurrent disease.
High‑Yield Points - ⚡ Biggest Takeaways
- Reactive Arthritis: an aseptic inflammatory arthritis triggered by GI (Salmonella, Shigella, Yersinia) or GU (Chlamydia) infections.
- Classic triad: "Can't see, can't pee, can't climb a tree" (conjunctivitis/uveitis, non-gonococcal urethritis, arthritis).
- Strong association with HLA-B27 positivity.
- Typically an asymmetrical oligoarthritis, predominantly affecting lower limb large joints.
- Extra-articular features: enthesitis, dactylitis, keratoderma blenorrhagicum, circinate balanitis.
- Synovial fluid: inflammatory, sterile (culture-negative).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

