Prevention of Orthopaedic Infections - Bug Battle Basics
- Surgical Site Infection (SSI): CDC defined.
- Superficial Incisional: Skin/subcutaneous; within 30 days.
- Deep Incisional: Fascia/muscle; 30 days (no implant), 1 year (implant).
- Organ/Space: Manipulated anatomy (joint, bone).
- Prosthetic Joint Infection (PJI): Infection involving implant/periprosthetic tissue.
- Common Pathogens: Staphylococcus aureus (MSSA/MRSA), CoNS, Gram-negatives (Pseudomonas).
- Risk Factors:
- Patient: Diabetes, obesity, smoking, malnutrition, immunosuppression.
- Procedure: Prolonged surgery, poor asepsis, implants.

⭐ Staphylococcus aureus is the most common pathogen in orthopaedic infections, including SSI and PJI.
Prevention of Orthopaedic Infections - Pre-Surgery Armor Up
- Patient Optimization: Minimize SSI risk.
- Smoking: Cessation ≥4 wks pre-op.
- Diabetes: Control HbA1c < 7% (better healing).
- Nutrition: Correct malnutrition & anemia.
- Obesity: Manage BMI >35-40 kg/m² (counsel SSI risk).
- MRSA/MSSA Decolonization (if carrier):
- Mupirocin 2% intranasal: BID x 5 days pre-op.
- CHG body washes: Daily x 3-5 days pre-op.
- Preoperative Antibiotic Prophylaxis:
- Timing: IV antibiotics within 60 mins pre-incision. 📌 "An Hour to Empower!"
- Agent: Procedure-specific, local antibiogram, patient allergies.

- Re-dosing: Surgery >3-4h (or >2 drug half-lives), or blood loss >1500mL.
⭐ Vancomycin infusion should start within 120 minutes before surgical incision due to longer infusion time.
Prevention of Orthopaedic Infections - OR Germ Warfare
- Operating Room (OR) Environment:
- Positive pressure ventilation system.
- Laminar airflow to reduce airborne contaminants.
- Air changes: ≥15-25 per hour.
- Minimize OR traffic and door openings.
- UV germicidal irradiation (adjunctive).
- Surgical Team Preparedness:
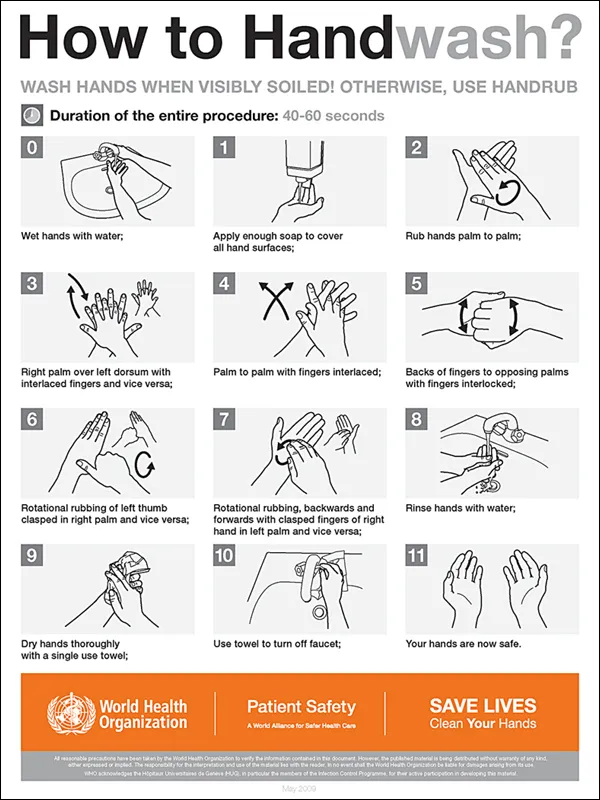
- Hand hygiene: meticulous surgical scrubbing or alcohol-based rubs.
- Surgical attire: sterile, impermeable gowns, masks, headgear, shoe covers.
- Double gloving, especially for implant surgery.
- Patient Skin Preparation:
- Antiseptic agents: Chlorhexidine-alcohol is often preferred.
⭐ Chlorhexidine-alcohol is generally preferred over povidone-iodine for surgical skin preparation due to superior efficacy and residual activity.
- Meticulous Surgical Technique:
- Atraumatic tissue handling to preserve vascularity.
- Obliteration of dead space.
- Copious irrigation to remove debris.
- Effective hemostasis.
- Minimize operative time.
- Appropriate suture material and wound closure.
- Specific Prophylaxis:
- Antibiotic-laden bone cement (ALBC) for selected high-risk arthroplasty cases.
Prevention of Orthopaedic Infections - Healing's Watchful Eye
- Wound Care:
- Sterile dressings: Maintain until dry or per protocol.
- Incision care: Keep clean, dry; educate patient.
- Suture/Staple Removal: Typically 7-14 days post-op; site-dependent.
- Antibiotic Prophylaxis:
- Discontinue within 24 hours post-op, even with drains.
- ⭐ > Prophylactic antibiotics should generally be discontinued within 24 hours after surgery, even with drains in place.
- Monitoring for Infection Signs:
- Local (📌 "RSPD" + Warmth): Redness, Swelling, ↑Pain, Discharge (purulent), Warmth.
- Visual aid:

- Visual aid:
- Systemic: Fever (>38°C), chills, tachycardia, ↑WBC, ↑CRP/ESR.
- Local (📌 "RSPD" + Warmth): Redness, Swelling, ↑Pain, Discharge (purulent), Warmth.
- Early Action:
- Promptly manage superficial SSI to prevent deep infection.
- Culture if suspected_
High‑Yield Points - ⚡ Biggest Takeaways
- Preoperative optimization: control diabetes (HbA1c <7%), stop smoking, ensure nutrition.
- Antibiotic prophylaxis: within 60 mins pre-incision (120 mins for Vancomycin/FQ); Cefazolin common; stop ≤24 hrs.
- Intraoperative sterility: laminar air flow, minimal OR traffic, CHG-alcohol skin prep.
- MRSA decolonization (mupirocin, CHG baths) for high-risk procedures like arthroplasty.
- Postoperative wound care: sterile dressings, monitor for SSI signs.
- Open fractures: urgent debridement and broad-spectrum antibiotics.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

