Osteomyelitis - Bone's Fiery Foes
- Bone & marrow inflammation, typically bacterial.
- Types:
- Acute (<2 wks), Chronic (>2 wks).
- Sources: Hematogenous, Contiguous, Direct Inoculation.
⭐ Staphylococcus aureus is the most common causative organism overall.
- Pathophysiology: Sequestrum (necrotic bone), Involucrum (new periosteal bone), Cloaca (draining sinus). Brodie's abscess (chronic, localized).
- Diagnosis:
- Labs: ↑ESR, ↑CRP.
- Imaging: MRI (best early detection & extent). X-ray (late: lytic changes, periostitis).
- Gold Standard: Bone biopsy with culture & histology.
- Specific Organisms:
- Sickle Cell Disease: Salmonella spp.
- IV Drug Users: Pseudomonas aeruginosa, S. aureus.
- Puncture wound (foot, through shoe): Pseudomonas aeruginosa.

Osteomyelitis - Spotting the Siege
- Bone infection (marrow & cortex). Routes: Hematogenous (kids: metaphysis), contiguous, direct implantation.
- Key Labs: ↑ ESR/CRP. MRI (most sensitive for early diagnosis). Bone biopsy (gold standard).
| Feature | Acute Osteomyelitis | Chronic Osteomyelitis |
|---|---|---|
| Onset | Sudden, < 2 weeks | Insidious, > 6 weeks / recurrent |
| Symptoms/Signs | Fever, severe pain, local inflammation | Draining sinus, persistent pain, deformity |
| X-ray Hallmark | Periosteal reaction (late), lytic areas | Sequestrum, involucrum, cloaca |
| Organism (Common) | S. aureus | S. aureus, Pseudomonas aeruginosa |
⭐ Brodie's abscess: A subacute or chronic localized osteomyelitis; appears as a well-circumscribed lytic lesion, often in the metaphysis of long bones (e.g., tibia), surrounded by a sclerotic rim on X-ray. Typically caused by S. aureus.
Osteomyelitis - Unmasking the Enemy
- Initial Clues:
- Labs: ↑ ESR (>70mm/hr), ↑ CRP (acute phase, therapy response). Leukocytosis variable. Blood cultures (+ve ~50% hematogenous).
- Imaging Journey:
- X-ray: First line. Early: soft tissue swelling. Later (10-14 days): periosteal reaction, lytic areas. Chronic: sequestrum, involucrum.
- MRI:
⭐ MRI: most sensitive (>90%) & specific for early osteomyelitis (marrow edema, abscess in 1-2 days).
- CT: Details cortical destruction, sequestra, sinus tracts.
- Bone Scan (Tc-99m): Sensitive (↑ uptake), not specific; good for multifocal.
- Definitive Diagnosis:
- Bone biopsy (image-guided/open): Gold standard. Tissue for culture (aerobic, anaerobic, fungal, AFB) & histopathology.
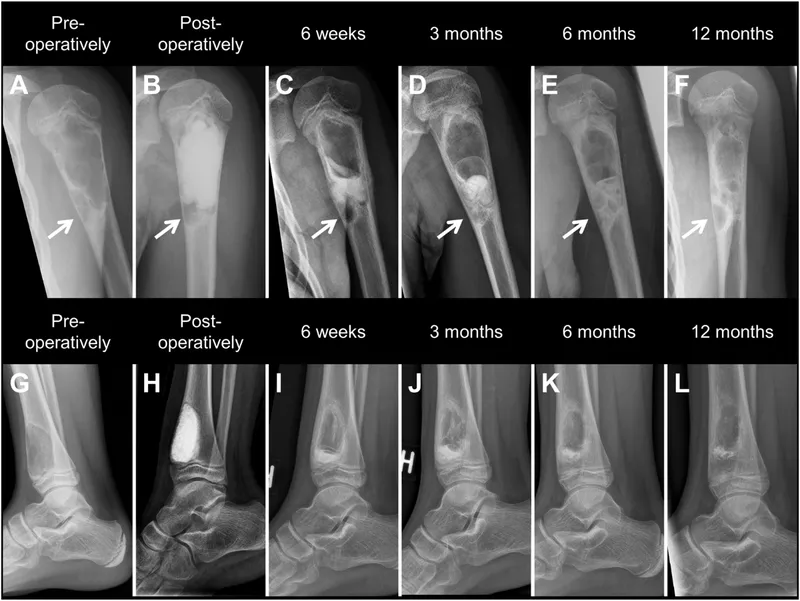
Osteomyelitis - Victory & Vigilance
- Therapeutic Goals: Infection eradication, pain relief, function restoration, recurrence prevention.
- Medical Therapy:
- Prolonged antibiotics: Crucial. IV initially (e.g., Vancomycin + Ceftriaxone if MRSA suspected), then culture-guided oral.
⭐ Typical duration of antibiotic therapy for acute osteomyelitis is 4-6 weeks, can be longer for chronic.
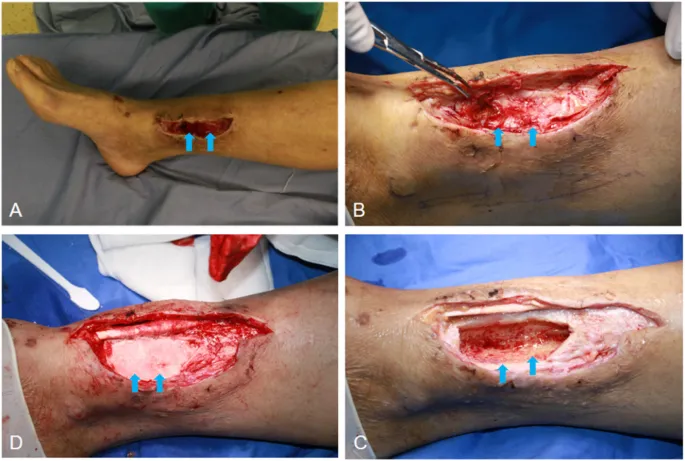
- Surgical Strategy: Often mandatory for chronic/complicated cases.
- Aggressive debridement: Removal of all infected/necrotic bone (sequestrectomy) & soft tissue.
- Dead space management: Antibiotic-impregnated beads (PMMA), muscle flaps, bone grafts.
- Stabilization: For pathological fractures or instability.
- Long-term Vigilance & Complications:
- Chronic osteomyelitis, recurrence.
- Pathological fracture.
- Brodie's abscess.
- Marjolin's ulcer (SCC in chronic sinus ⚠️).
- Growth plate damage (children).
High‑Yield Points - ⚡ Biggest Takeaways
- Staphylococcus aureus: Most common organism in osteomyelitis.
- Children: Primarily hematogenous spread. Adults: Often contiguous source or direct inoculation.
- Brodie's abscess: A chronic, localized form of osteomyelitis.
- Hallmark signs: Sequestrum (dead bone fragment) and involucrum (new bone formation).
- MRI: Most sensitive for early diagnosis. Bone biopsy/culture: Gold standard.
- Treatment: Prolonged antibiotics (IV then oral) and surgical debridement if needed.
- Sickle cell disease: Increased risk of Salmonella osteomyelitis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

