Phakic IOLs: Fundamentals - Eyes Wide Open
- Definition: Implantable lens in an eye retaining its natural crystalline lens (phakic).
- Mechanism: Corrects refractive errors (myopia, hyperopia, astigmatism) by adding optical power within the eye.
- Advantages:
- Preserves the eye's natural accommodation.
- Reversibility: can be removed if needed.
- Corrects a wide range of refractive powers.
- Often provides excellent optical quality.
- General Indications:
- High myopia (e.g., typically > -8 D).
- High hyperopia (e.g., typically > +4 D).
- Significant astigmatism.
- Patients unsuitable for corneal laser surgery (e.g., thin corneas, very dry eyes).
⭐ Phakic IOLs excel in correcting very high myopia, often effective for powers up to or exceeding -20 D.
Phakic IOLs: Classification - Lens Lineup Logic
Categorized by placement:
- Anterior Chamber (AC):
- Angle-supported: AC angle. E.g., AcrySof Cachet (PMMA, withdrawn).
- Iris-fixated (claw): Anterior iris. E.g., Artisan/Verisyse (PMMA), Artiflex/Veriflex (foldable).
- Posterior Chamber (PC):
- Sulcus-supported: Ciliary sulcus. E.g., ICL/Visian ICL (Collamer). 📌 ICL: 'I Can See Clearly'.
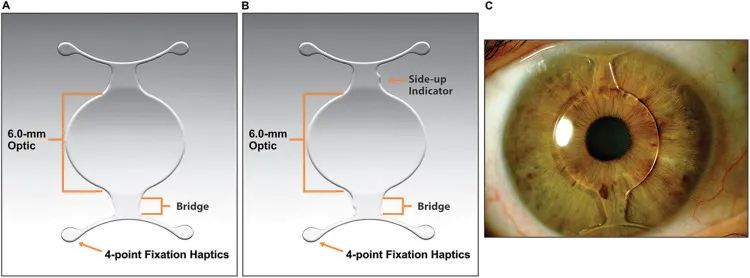
| Type | Fixation | Material(s) | Advantage(s) | Disadvantage(s)/Risk(s) |
|---|---|---|---|---|
| Angle-supported | AC Angle | PMMA | Anterior | Endothelial loss, PAS |
| Iris-fixated | Ant. Iris (claw) | PMMA, Silicone | Stable | Endothelial loss, Pupil oval |
| Sulcus-supported | Ciliary Sulcus | Collamer | Biocompatible, Reversible | Cataract, ↑IOP, Sizing |
Phakic IOLs: Candidacy & Workup - Sizing Up Success
- Indications:
- Stable high myopia (> -8D), hyperopia (> +4D), astigmatism.
- Poor LASIK/PRK candidates (thin corneas, dry eyes, irregular topography).
- Contraindications:
- Anterior Chamber Depth (ACD) < 3.0 mm (most types).
- Endothelial Cell Count (ECC) < 2000-2500 cells/mm².
- Active uveitis, glaucoma, cataract, progressive ectasia.
- Pre-operative Workup:
- Refraction (Manifest, Cycloplegic), Keratometry (K-values), Pachymetry.
- ACD, White-to-White (WTW) for sizing.
- Endothelial cell density & morphology.
- Gonioscopy, Dilated Fundus Exam.
- IOL Power Calculation: Van der Heijde, Olsen formulas.
- Sizing is Key: Proper sizing ensures adequate vault for Posterior Chamber IOLs, preventing complications.
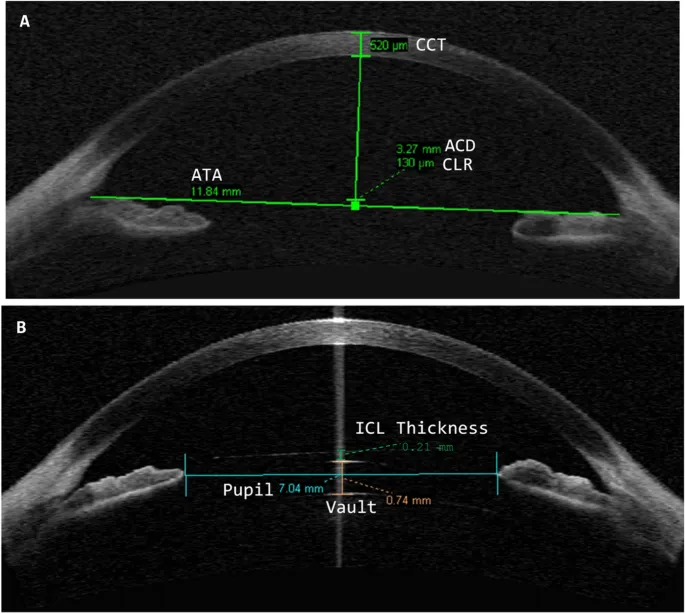
⭐ Accurate White-to-White (WTW) is crucial for sizing anterior chamber phakic IOLs; ACD is key for posterior chamber IOL vault.
Phakic IOLs: Technique & Troubles - Implant Insights & Issues
- Technique Highlights:
- Corneal incision, viscoelastic use.
- IOL insertion & precise positioning (AC/PC).
- PI/flow port for PC IOLs prevents pupillary block.
- Common & Serious Complications (Troubles):
- Endothelial cell loss: Critical for AC IOLs; acceptable annual loss <5%.
- Cataract formation: Esp. PC IOLs if vault low.
⭐ PC Phakic IOLs touching the crystalline lens (low vault) are a significant risk for anterior subcapsular cataract.
- Pupil ovalization (iris-fixated IOLs).
- Pigment dispersion syndrome/glaucoma.
- IOL decentration/dislocation.
- Glare/halos.
- Uveitis.
- Pupillary block (if PI/flow port absent/occluded).
- Management:
- Observation, topical steroids; explantation if severe.
High‑Yield Points - ⚡ Biggest Takeaways
- Phakic IOLs provide reversible correction for high refractive errors, preserving accommodation.
- Main types: Anterior chamber (angle-supported/iris-fixated) and Posterior chamber (ICL), placed behind the iris.
- ICL sizing is crucial; incorrect sizing risks vault issues, cataract formation, or angle closure.
- Key complications: Corneal endothelial cell loss, cataract (especially with ICLs), pupillary block, and increased IOP.
- Essential prerequisites: Adequate Anterior Chamber Depth (ACD) and a healthy endothelial cell count.
- Best suited for young patients with stable, high myopia or hyperopia, who are poor candidates for laser vision correction.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

