General Candidacy - The Starting Line
- Age: ≥18 years (ideally ≥21 years for refractive maturity).
- Refractive Stability: Paramount.
- Change in Spherical Equivalent (SE) <0.50 D over 12 months.
- Verified by ≥2 refractions (cycloplegic if possible).
- Motivation & Expectations:
- Strong desire for spectacle/contact lens independence.
- Realistic understanding of risks, benefits, limitations, alternatives.
- Systemic Health:
- Good general health.
- No uncontrolled:
- Autoimmune diseases (e.g., SLE, RA).
- Immunodeficiency.
- Diabetes Mellitus (poorly controlled can affect healing & refraction).
- Ocular Health:
- No active ocular disease:
- Severe Dry Eye Syndrome (DES).
- Keratitis, Uveitis.
- Uncontrolled Glaucoma.
- Progressive corneal ectasias (Keratoconus, PMD).
- No active ocular disease:
- Key Contraindications (Absolute):
- Pregnancy or breastfeeding.
- Unrealistic expectations.
- Sole functioning eye (relative to absolute, requires extreme caution).
⭐ Documented refractive stability (<0.50D change in SE over 1 year) is the cornerstone of patient selection.
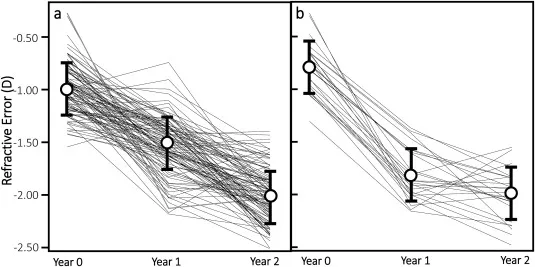
Ocular Examination - Eye Spy Fitness
Key assessments to ensure suitability for refractive surgery:
- Visual Acuity & Refraction:
- Uncorrected (UCVA) & Best-Corrected Visual Acuity (BCVA).
- Manifest & Cycloplegic refraction: Stability essential (change < 0.5D in 1 year).
- Corneal Evaluation:
- Topography/Tomography:
- Assesses corneal shape, power (K-values: avg 40-47D), regularity.
- Screens for ectasia (e.g., Keratoconus, Pellucid Marginal Degeneration).

- Pachymetry:
- Measures Central Corneal Thickness (CCT).
- Min CCT for LASIK often > 500 µm.
- Crucial for calculating Residual Stromal Bed (RSB) thickness (target > 250-300 µm).
- Topography/Tomography:
- Pupil Size:
- Scotopic pupil diameter measurement.
- Large pupils (> 6-7 mm) may ↑ risk of night vision issues (halos, glare) if > optical zone.
- Tear Film Assessment:
- TBUT, Schirmer's test.
- Identify & treat pre-existing Dry Eye Disease (DED).
- Intraocular Pressure (IOP):
- Rule out glaucoma or ocular hypertension. Normal range 10-21 mmHg.
- Slit-Lamp Examination:
- Detailed anterior segment evaluation (lids, conjunctiva, cornea, lens).
- Rule out blepharitis, active infection, cataract.
- Fundoscopy (Dilated):
- Posterior segment health (retina, optic nerve). Rule out retinal pathology.
⭐ Belin/Ambrósio Enhanced Ectasia Display (BAD) on Pentacam is a crucial tool to unmask subtle corneal ectatic changes, aiding in identifying unsuitable LASIK candidates.
Contraindications - Red Flags & Alerts
- Absolute Contraindications:
- Age < 18 years (typically < 21 yrs for stability)
- Unstable refraction: > 0.5D change/year
- Corneal ectasias: Keratoconus, PMD
- Insufficient corneal thickness (pachymetry < 480-500 µm)
- Active ocular infection (e.g., active herpes, microbial keratitis) or active uveitis
- Uncontrolled systemic diseases: active autoimmune dz, immunodeficiency
- Pregnancy or breastfeeding
- Unrealistic patient expectations
- Monocular patient (strong relative/absolute)
- Relative Contraindications (Caution Advised):
- Severe Dry Eye Disease (optimize pre-operatively)
- Glaucoma (IOP monitoring challenges, steroid response)
- History of HSV keratitis (reactivation risk; consider prophylaxis)
- Large pupils (>7mm scotopic) (night vision issues: glare, halos)
- Diabetes Mellitus (well-controlled; monitor healing, refractive stability)
- History of keloid formation
- Certain systemic medications (e.g., amiodarone, isotretinoin, sumatriptan)
⭐ Forme fruste keratoconus (FFKC), often subtle and missed on basic exam, is an absolute contraindication due to high risk of iatrogenic ectasia post-LASIK.
High-Yield Points - ⚡ Biggest Takeaways
- Stable refraction for at least 1 year is a primary criterion.
- Minimum age is typically 18-21 years; ensure skeletal maturity.
- Crucial: Adequate corneal thickness (pachymetry >500µm), ensuring sufficient residual stromal bed (RSB >250-300µm).
- Absolute contraindications: Keratoconus, active ocular surface disease, uncontrolled systemic conditions (e.g., autoimmune).
- Realistic expectations and patient motivation are key for success.
- Evaluate mesopic pupil size to minimize postoperative night vision symptoms.
- Pregnancy and lactation are temporary contraindications.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

