Refractive Surgery

On this page
🎯 Refractive Surgery: The Precision Vision Revolution
Refractive surgery has transformed millions of lives by permanently correcting vision through precise corneal reshaping, yet success hinges on understanding which laser technology fits which eye, which patient qualifies, and why technique selection determines outcomes. You'll master the physics behind excimer and femtosecond lasers, learn the candidacy algorithms that separate ideal from risky candidates, and build a decision framework for choosing between LASIK, PRK, and SMILE. This lesson moves you from observer to strategic decision-maker, integrating anatomy, technology, and patient factors into confident surgical planning.
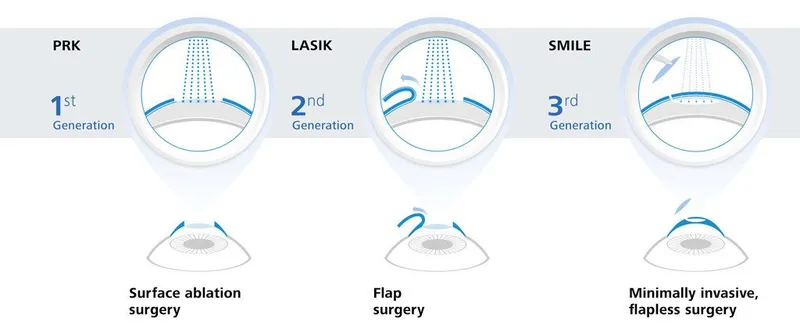
Refractive surgery represents the pinnacle of precision medicine, transforming corneal architecture with sub-micron accuracy to eliminate dependence on corrective lenses. Understanding these surgical principles unlocks the logic behind every visual outcome and complication pattern.
📌 Remember: LASER - Light Amplification by Stimulated Emission of Radiation. Excimer lasers operate at 193 nm wavelength, removing 0.25 microns of corneal tissue per pulse with ±0.1 diopter accuracy.
Refractive Surgery Classification Matrix
| Procedure Type | Tissue Removal | Flap Creation | Recovery Time | Max Correction | Corneal Thickness |
|---|---|---|---|---|---|
| LASIK | Stromal ablation | 160 μm flap | 24-48 hours | -12.0 D myopia | >500 μm required |
| PRK | Surface ablation | No flap | 3-5 days | -8.0 D myopia | >400 μm required |
| SMILE | Lenticule extraction | 2-4 mm incision | 24-72 hours | -10.0 D myopia | >300 μm residual |
| Phakic IOL | No tissue removal | No corneal surgery | Immediate | -20.0 D myopia | Any thickness |
- Tensile strength: 3.8 MPa in healthy corneas
- Young's modulus: 0.29 MPa anterior stroma vs 0.18 MPa posterior
- Anterior 40% provides 70% of biomechanical strength
- Posterior stromal preservation critical for ectasia prevention
- Optical Zone Parameters
- Standard optical zone: 6.0-6.5 mm diameter
- Transition zone: 8.0-9.0 mm total ablation
- Smaller zones increase spherical aberration by 300%
- Larger zones reduce night vision complaints by 60%
⭐ Clinical Pearl: Residual stromal bed thickness <250 μm increases ectasia risk by 15-fold. Always calculate: Original thickness - Flap thickness - Ablation depth = Residual bed.
💡 Master This: Excimer laser photoablation removes 0.25 μm per pulse with 1.0 mm² spot size, enabling ±0.1 D precision in refractive correction through controlled stromal reshaping.
The corneal healing response determines surgical success, with epithelial regeneration completing in 3-5 days and stromal remodeling continuing for 6-12 months. Connect these healing timelines through biomechanical stability concepts to understand long-term refractive outcomes.
🎯 Refractive Surgery: The Precision Vision Revolution
⚡ Laser Vision Correction: The Excimer Precision Engine
📌 Remember: ABLATION - Accurate Beam Laser Adjusts Tissue In Optical Needs. Each diopter of myopia correction requires 12-14 μm of central corneal ablation over 6.0 mm optical zone.
Laser Parameters and Tissue Interaction
- Excimer Laser Specifications
- Wavelength: 193 nm (argon fluoride)
- Pulse duration: 10-20 nanoseconds
- Energy density: 160 mJ/cm² per pulse
- Repetition rate: 200-500 Hz modern systems
- Ablation Characteristics
- Penetration depth: 0.25 μm per pulse
- Thermal damage zone: <1.0 μm (minimal thermal effect)
- Bond breaking energy: 6.4 eV for corneal proteins
- Precision: ±0.1 D refractive accuracy achievable
| Refractive Error | Ablation Depth | Tissue Removal | Optical Zone | Treatment Time |
|---|---|---|---|---|
| -1.0 D myopia | 12 μm central | Prolate shaping | 6.0 mm | 15 seconds |
| -6.0 D myopia | 72 μm central | Steep prolate | 6.5 mm | 90 seconds |
| +3.0 D hyperopia | 45 μm peripheral | Oblate shaping | 6.0 mm | 60 seconds |
| 3.0 D astigmatism | 36 μm meridional | Cylindrical | 6.5 mm | 45 seconds |
⭐ Clinical Pearl: Asphericity (Q-value) changes from -0.26 (normal cornea) to +0.5 after myopic ablation, increasing spherical aberration by 0.3 μm for 6 mm pupils.
💡 Master This: Munnerlyn formula calculates ablation depth: Depth = (D × A²)/3, where D = diopters corrected, A = ablation zone radius in mm. Critical for surgical planning.
Advanced wavefront-guided treatments reduce higher-order aberrations by 40% compared to conventional ablation, with pupil-optimized algorithms minimizing night vision symptoms in 85% of patients. These precision improvements through femtosecond flap creation techniques reveal enhanced safety profiles.
⚡ Laser Vision Correction: The Excimer Precision Engine
🔬 Femtosecond Technology: The Flap Creation Revolution
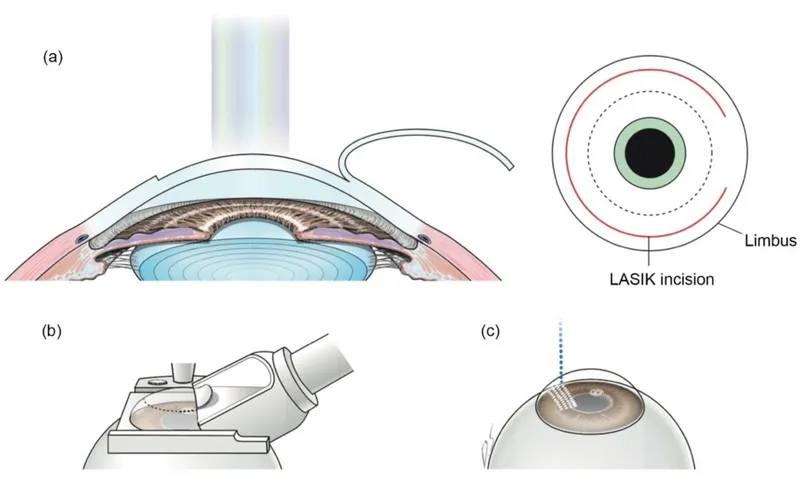
Femtosecond lasers operate at 1053 nm wavelength with pulse durations of 300-600 femtoseconds, creating photodisruption through plasma formation without thermal damage. Each pulse generates 1-2 μm cavitation bubbles that coalesce into tissue planes.
📌 Remember: FEMTO - Fast Energy Micro Tissue Opening. Femtosecond = 10⁻¹⁵ seconds, enabling intrastromal photodisruption without surface damage at 1053 nm wavelength.
Femtosecond Flap Parameters
- Laser Specifications
- Pulse energy: 0.5-2.0 μJ per pulse
- Spot separation: 2-8 μm between pulses
- Scanning speed: 25 kHz pulse frequency
- Flap creation time: 15-25 seconds total
- Flap Characteristics
- Thickness uniformity: ±5 μm across 9.0 mm diameter
- Side cut angle: 70-130 degrees programmable
- Hinge position: Superior or nasal placement
- Hinge width: 3.0-4.0 mm for stability
| Flap Parameter | Microkeratome | Femtosecond Laser | Clinical Impact | Complication Rate |
|---|---|---|---|---|
| Thickness variation | ±30 μm | ±5 μm | Predictable ablation | 2% vs 0.1% |
| Incomplete flaps | 0.3% | 0.01% | Surgical conversion | Rare with femto |
| Buttonhole | 0.2% | 0% | Surgery termination | Eliminated |
| Free cap | 0.1% | 0% | Flap loss | Prevented |
⭐ Clinical Pearl: Opaque bubble layer (OBL) occurs in 10-15% of femtosecond cases, requiring 2-4 hour delay before excimer ablation to allow bubble absorption.
- Advanced Femtosecond Applications
- SMILE lenticule creation: 120-140 μm cap thickness
- Corneal transplant: Mushroom and zigzag cuts
- Intrastromal ring channels: 70% corneal depth
- Cataract surgery: Capsulotomy and lens fragmentation
💡 Master This: Femtosecond photodisruption threshold requires 10¹³ W/cm² power density, achieved through ultrashort pulse duration creating multiphoton ionization without thermal damage.
The biomechanical advantages of femtosecond flaps include stronger adhesion (requiring 3x force to lift after 24 hours) and reduced inflammatory response compared to mechanical keratomes. These precision improvements through patient selection algorithms determine optimal surgical candidacy.
🔬 Femtosecond Technology: The Flap Creation Revolution
🎯 Patient Selection: The Candidacy Algorithm
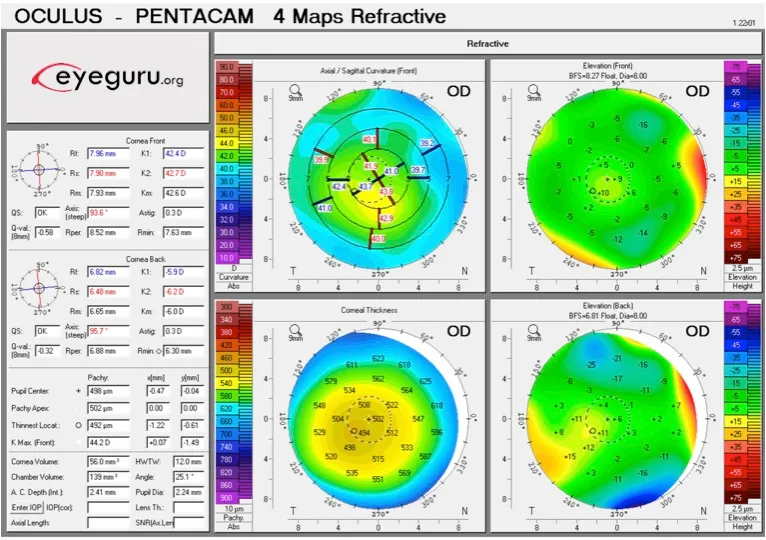
Patient selection represents the most critical determinant of surgical outcomes, with proper screening reducing complications by 90% and enhancing satisfaction rates to >95%. Systematic evaluation protocols identify absolute and relative contraindications with evidence-based thresholds.
📌 Remember: SCREEN - Stable refraction Corneal thickness Realistic expectations Ectasia risk Eye health No contraindications. Each parameter requires quantitative assessment with specific cutoff values.
Candidacy Assessment Matrix
| Parameter | LASIK Requirements | PRK Requirements | SMILE Requirements | Disqualifying Values |
|---|---|---|---|---|
| Age | 18-65 years | 18-70 years | 18-45 years | <18 or >70 years |
| Refractive stability | <0.5 D change/year | <0.5 D change/year | <0.5 D change/year | >0.5 D change |
| Corneal thickness | >500 μm | >450 μm | >480 μm | <400 μm |
| Pupil size | <7.0 mm scotopic | <8.0 mm scotopic | <7.5 mm scotopic | >8.0 mm |
| Dry eye severity | Mild acceptable | Moderate acceptable | Mild acceptable | Severe dry eye |
- Central corneal thickness: >500 μm for LASIK
- Posterior elevation: <20 μm above BFS
- Corneal hysteresis: >9.0 mmHg (normal biomechanics)
- Resistance factor: >7.5 mmHg (ectasia screening)
- Refractive Error Limits
- Myopia: -0.5 to -12.0 D (LASIK), -0.5 to -8.0 D (PRK)
- Hyperopia: +0.5 to +6.0 D (all procedures)
- Astigmatism: ≤6.0 D cylinder correction
- Anisometropia: ≤3.0 D difference between eyes
⭐ Clinical Pearl: Forme fruste keratoconus affects 12% of keratoconus family members, requiring Pentacam screening with BAD-D >1.6 indicating ectasia risk.
- Absolute Contraindications
- Progressive keratoconus or pellucid marginal degeneration
- Autoimmune diseases: Sjögren's, rheumatoid arthritis
- Pregnancy and nursing (hormonal instability)
- Uncontrolled diabetes (HbA1c >8.0%)
- Relative Contraindications
- Dry eye disease (OSDI score >22)
- Large pupils (>7.0 mm scotopic)
- Thin corneas (450-500 μm range)
- High myopia (>-8.0 D) with thin corneas
💡 Master This: Ectasia risk calculation uses ERSS score: Age, CCT, topography, RSB thickness. Score >3 indicates high risk requiring enhanced screening or procedure modification.
The psychological assessment identifies unrealistic expectations in 15% of consultations, with detailed counseling improving satisfaction rates from 85% to >95%. These candidacy principles through surgical technique selection optimize individual patient outcomes.
🎯 Patient Selection: The Candidacy Algorithm
⚖️ Surgical Technique Selection: The Precision Decision Matrix
Surgical technique selection integrates corneal biomechanics, refractive error magnitude, lifestyle factors, and healing characteristics to optimize visual outcomes. Evidence-based algorithms match patient profiles to procedure advantages with quantified success metrics.
📌 Remember: MATCH - Myopia magnitude Age considerations Tissue thickness Corneal shape Healing factors. Each technique offers specific advantages for defined patient populations.
Technique Selection Algorithm
- LASIK Optimization
- Ideal candidates: -1.0 to -8.0 D myopia, CCT >500 μm
- Advantages: Rapid recovery (24-48 hours), minimal pain
- Success rate: >98% within ±0.5 D target
- Enhancement rate: <5% at 12 months
- PRK Advantages
- Thin corneas: 450-500 μm thickness range
- Contact sports: No flap complications possible
- Irregular astigmatism: Better surface regularization
- Epithelial basement membrane dystrophy: Therapeutic benefit
| Technique | Recovery Time | Pain Level | Flap Risk | Max Correction | Biomechanical Impact |
|---|---|---|---|---|---|
| LASIK | 24-48 hours | Minimal | Present | -12.0 D | Moderate |
| PRK | 3-5 days | Moderate | None | -8.0 D | Minimal |
| SMILE | 24-72 hours | Mild | Minimal | -10.0 D | Least |
| Phakic IOL | Immediate | Minimal | None | -20.0 D | None |
⭐ Clinical Pearl: SMILE preserves 65% more anterior stromal fibers than LASIK, maintaining corneal biomechanical strength with 40% less reduction in corneal hysteresis.
- SMILE Specific Advantages
- Biomechanical preservation: Minimal anterior fiber disruption
- Dry eye reduction: 70% less severe dry eye vs LASIK
- No flap complications: Eliminates displacement, striae, epithelial ingrowth
- Learning curve: 100+ cases for optimal outcomes
- Phakic IOL Indications
- High myopia: >-8.0 D with thin corneas
- Hyperopia: >+4.0 D (limited corneal options)
- Reversibility: Lens removal restores original cornea
- Presbyopia: Multifocal phakic IOLs available
💡 Master This: Biomechanical impact hierarchy: PRK (minimal) < SMILE (mild) < LASIK (moderate). Anterior stromal preservation correlates with long-term stability and ectasia resistance.
The enhancement rate varies by technique: LASIK 3-5%, PRK 5-8%, SMILE 2-4%, with timing protocols requiring 3-month stability before retreatment. These outcome patterns through complication management strategies ensure optimal long-term results.
⚖️ Surgical Technique Selection: The Precision Decision Matrix
🔗 Advanced Integration: The Multi-Modal Precision Platform
📌 Remember: INTEGRATE - Imaging Navigation Topography Eye tracking Guidance Real-time Adjustment Treatment Enhancement. Modern systems process 1000+ data points for personalized treatment.
Multi-Modal Integration Matrix
- Wavefront-Guided Treatments
- Higher-order aberration reduction: 40-60% improvement
- Contrast sensitivity: 25% enhancement in mesopic conditions
- Pupil-optimized zones: 6.0-6.5 mm based on scotopic measurements
- Asphericity control: Q-value optimization reduces spherical aberration
- Corneal Biomechanical Integration
- Corneal hysteresis: >10.0 mmHg indicates strong biomechanics
- Corneal resistance factor: >8.0 mmHg reduces ectasia risk
- Stress-strain index: <1.0 normal, >1.25 high risk
- Integrated radius: Combines topography with biomechanics
| Integration Level | Diagnostic Components | Treatment Precision | Outcome Improvement | Complication Reduction |
|---|---|---|---|---|
| Basic | Topography + Pachymetry | ±0.25 D | 90% satisfaction | Standard rates |
| Advanced | + Wavefront + Biomechanics | ±0.12 D | 95% satisfaction | 50% reduction |
| AI-Enhanced | + Machine Learning + Prediction | ±0.06 D | 98% satisfaction | 75% reduction |
⭐ Clinical Pearl: Corneal biomechanical factor (CBiF) combines multiple parameters into single metric, with values <0.5 indicating excellent surgical candidates and >1.0 requiring enhanced screening.
- Artificial Intelligence Integration
- Machine learning algorithms analyze >100,000 cases
- Predictive modeling: 85% accuracy for visual outcomes
- Risk stratification: Automated red flags for ectasia
- Treatment optimization: Personalized ablation patterns
- Real-Time Surgical Feedback
- Eye tracking: 1050 Hz frequency with <1.0 mm accuracy
- Iris registration: Cyclotorsion compensation ±15 degrees
- Pachymetry monitoring: Real-time thickness measurement
- Ablation depth control: Automatic safety stops
💡 Master This: Integrated platforms reduce surgeon decision fatigue by 60% while improving outcome predictability through standardized protocols and automated safety checks.
The future integration includes genetic markers for healing prediction, tear film analysis for dry eye risk, and lifestyle algorithms for procedure selection. These comprehensive approaches through outcome optimization strategies maximize patient satisfaction and safety.
🔗 Advanced Integration: The Multi-Modal Precision Platform
🎯 Mastery Framework: The Refractive Surgery Command Center
📌 Remember: MASTER - Multi-modal assessment Algorithmic decisions Systematic protocols Technique optimization Evidence-based Results. Expert practice requires >500 cases experience with continuous outcome analysis.
Essential Clinical Arsenal
| Critical Threshold | Value | Clinical Significance | Action Required |
|---|---|---|---|
| Residual stromal bed | <250 μm | Ectasia risk | Modify technique |
| Corneal hysteresis | <9.0 mmHg | Weak biomechanics | Enhanced screening |
| Pupil size scotopic | >7.0 mm | Night vision risk | Larger optical zone |
| Dry eye OSDI | >22 points | Severe symptoms | Pretreat before surgery |
| Age factor | >45 years | Presbyopia onset | Discuss monovision |
- STOP criteria: Stable refraction, Thickness adequate, Ocular health, Patient expectations
- GO criteria: Good candidate, Optimal technique selected
- Decision time: <5 minutes for experienced surgeons
- Documentation: 15+ parameters recorded systematically
⭐ Clinical Pearl: The 3-2-1 Rule: 3 months refractive stability, 2 comprehensive exams, 1 clear technique choice before proceeding with surgery.
💡 Master This: Expert surgeons achieve <1% enhancement rate through meticulous patient selection, optimal technique matching, and precise surgical execution with systematic protocols.
Outcome Optimization Checklist:
- Preoperative: 15-point comprehensive assessment
- Intraoperative: Real-time monitoring with safety protocols
- Postoperative: Structured follow-up at 1 day, 1 week, 1 month, 3 months
The mastery pathway requires continuous learning, outcome analysis, and technique refinement to maintain >98% patient satisfaction with <0.1% serious complications through evidence-based practice excellence.
🎯 Mastery Framework: The Refractive Surgery Command Center
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app












