Exotropia Essentials - Outward Eye Turn
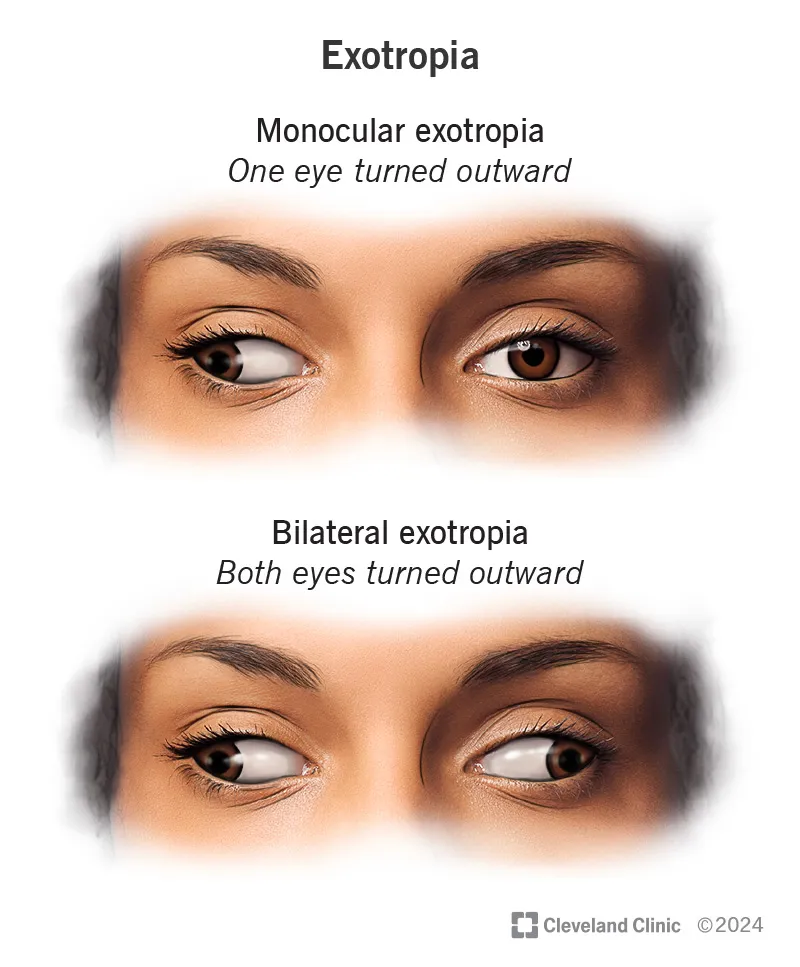
- Definition: Outward deviation (divergence) of one or both eyes.
- Types & Features:
- Intermittent Exotropia (IXT): Most common type. Eye turn occurs sometimes, especially when tired, ill, or viewing distant objects. Good fusional control initially.
- Often closes one eye in bright sunlight (photo-occlusion).
- Diplopia rare, suppression common.
- Constant Exotropia: Eye turn present at all times. May be congenital or develop from IXT.
- Sensory Exotropia: Due to poor vision in one eye (e.g., cataract, optic atrophy). Eye with poor vision deviates outwards.
- Consecutive Exotropia: Develops after surgical overcorrection of esotropia.
- Intermittent Exotropia (IXT): Most common type. Eye turn occurs sometimes, especially when tired, ill, or viewing distant objects. Good fusional control initially.
- Basic Mechanisms: Imbalance between fusional convergence and divergence mechanisms. Innervational factors (e.g., high AC/A ratio in divergence excess) or anatomical factors.
⭐ Intermittent exotropia is the most common type of childhood exotropia, often manifesting between 1-4 years of age. Control is typically worse for distance fixation than near initially in many cases (Divergence Excess type).
Exotropia Evaluation - Spotting the Drift
- History: Onset, duration, frequency (constant/intermittent), triggers (distance, fatigue, inattention), family Hx.
- Visual Acuity (VA): Best corrected; rule out/quantify amblyopia.
- Cover Tests: Key for detection.
- Cover-Uncover Test: Detects manifest XT (eye drifts OUT, refixates IN on uncover).
- Alternate Cover Test (ACT): Dissociates; reveals total deviation (phoria/intermittent tropia).
- Prism ACT (PACT): Measures deviation in PD (distance & near).
- Ocular Motility: Ductions, versions; check A/V patterns, oblique dysfunction.
- Near Point of Convergence (NPC): Receded (>10-15 cm) suggests Convergence Insufficiency.
- Cycloplegic Refraction: Essential for accurate refraction.
- Sensory Evaluation:
- Worth 4 Dot: Fusion, suppression, diplopia.
- Stereoacuity: (e.g., Titmus, TNO) quantifies depth perception.

⭐ Control of intermittent exotropia is often assessed using the Newcastle Control Score (NCS), grading home and clinic control.
Intermittent Exotropia - The On-Off Squint
- Most common exotropia; intermittent outward eye turn, often with fatigue, illness, or distance viewing.
- Clinical Features:
- Onset: Typically 1-4 years.
- Symptoms: Asthenopia, photophobia; children rarely report diplopia.
- Signs: Intermittent deviation, initially good fusional control.
⭐ Closing one eye in bright sunlight is a characteristic sign.
- Types:
- Basic: Distance deviation ≈ Near deviation.
- Convergence Insufficiency Type: Near deviation > Distance deviation.
- Divergence Excess Type: Distance deviation > Near deviation.
- Management:
- Goal: Improve control, alignment, and binocular vision.
- Options:
- Observation: Small, well-controlled deviations.
- Non-surgical: Minus lenses (if high AC/A), occlusion, orthoptic exercises (convergence).
- Surgical: For poor control, ↑ deviation, or significant symptoms (e.g., bilateral lateral rectus recession).
Exotropia Treatment - Aligning the Gaze
-
Goal: Ocular alignment, binocular vision (stereopsis), symptom relief.
-
Non-Surgical:
- Observation: Small, well-controlled intermittent XT.
- Optical Correction: Full cycloplegic refraction for significant errors.
- Occlusion Therapy: Part-time, for amblyopia or to improve XT control.
- Orthoptic Exercises: (📌 Pencil Push-ups) For convergence insufficiency (CI) type or small intermittent XT.
-
Surgical:
- Indications: Constant XT, large angle (>20 PD), poor control, progression, asthenopia.
- Timing: Usually 4-7 years; earlier for constant XT.
- Procedures: Based on XT type & angle. Bilateral Lateral Rectus (BLR) recession (common); Unilateral Recess-Resect (R&R).

⭐ Surgical success for intermittent exotropia is often defined as alignment within 10 PD of orthophoria and improved fusional control.
High‑Yield Points - ⚡ Biggest Takeaways
- Intermittent exotropia is the most common type, often presenting between 6 months and 4 years.
- Deviation worsens with fatigue, illness, or inattention; improves with visual focus.
- Monocular eye closure in bright sunlight is a characteristic sign.
- Amblyopia is less common than in esotropia but requires monitoring.
- Management includes observation, glasses (e.g., minus lenses for high AC/A), patching, orthoptics, and surgery.
- Surgical aim is often a slight initial overcorrection for better long-term alignment.
- Sensory exotropia results from poor vision in one eye.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

