Overview & Classification - Flow & Folly
Orbital vascular lesions: congenital/acquired vessel anomalies. Understanding flow is key to diagnosis, management, avoiding pitfalls ("folly").
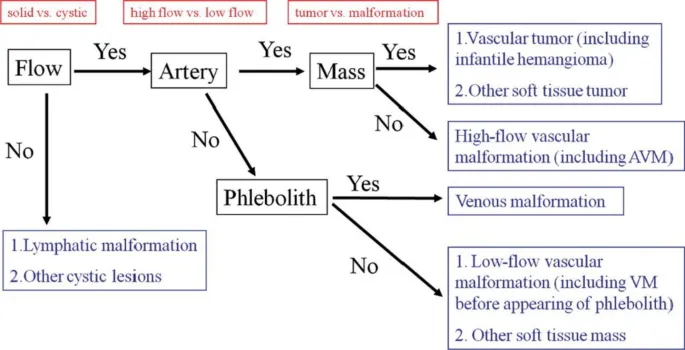
- Classification by Hemodynamics:
- Low-Flow (Venous/Capillary/Lymphatic):
- More common; gradual, non-pulsatile proptosis.
- Often compressible; may ↑ with Valsalva (e.g., varices).
- Types: Capillary Hemangioma, Cavernous Hemangioma, Lymphangioma, Orbital Varix.
- High-Flow (Arterial):
- Less common; acute/subacute onset.
- Pulsatile proptosis, audible bruit, chemosis, arterialized conjunctival veins.
- Types: Carotid-Cavernous Fistula (CCF), Arteriovenous Malformation (AVM).
- Low-Flow (Venous/Capillary/Lymphatic):
⭐ Proptosis is the most common presenting sign of orbital vascular lesions.
Common Hemangiomas - Benign Blobs
Capillary (infantile) vs. Cavernous (adult).
| Feature | Capillary Hemangioma (Infantile) | Cavernous Hemangioma (Adult) |
|---|---|---|
| Age | Infancy (birth-months) | Adults (30-50 yrs) |
| Presentation | "Strawberry nevus" (superficial), bluish (deep); Rapid growth, then involution. Risk: ptosis, amblyopia. | Gradual, painless, axial proptosis; diplopia; optic neuropathy. |
| Histology | Plump endothelial cells, small lumina. | Large, dilated vascular channels; fibrous capsule. |
| Key Imaging | MRI: T1 hypo, T2 hyper, flow voids, strong enhancement. | MRI: Well-defined, intraconal; T1 iso/hypo, T2 markedly hyper; progressive enhancement. |
| Management | Observation. Vision-threat: Propranolol (0.5-3 mg/kg/day), steroids. | Surgical excision if symptomatic. |
⭐ Cavernous hemangioma is the most common benign orbital tumor in adults.
Varices & Lymphangiomas - Drainage Dramas
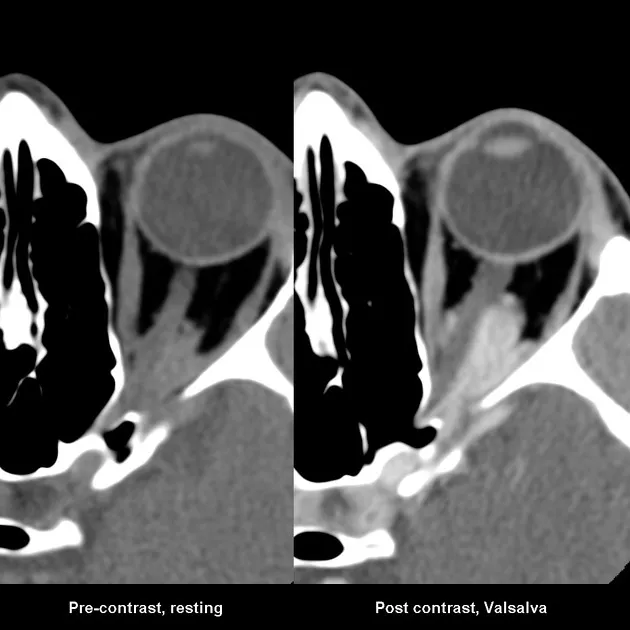
Orbital Varix (Venous Malformation)
- Low-flow venous channels; dilate with Valsalva or dependent head position.
- Key: Intermittent, non-pulsatile proptosis.
- Gaze-evoked proptosis is a classic sign.
- Imaging (CT/MRI): Shows distensible vascular channels, phleboliths may be present.
- Management: Observation for asymptomatic cases; surgical excision or sclerotherapy if symptomatic or compressive optic neuropathy.
Lymphangioma (Lymphatic Malformation)
- Developmental vascular anomaly; typically presents in 1st decade.
- Infiltrative growth pattern, lacks a true capsule, making complete excision difficult.
- Prone to spontaneous intralesional hemorrhage → sudden painful proptosis.
- Characteristic "chocolate cysts" (blood-filled lymphatic spaces).
- Management: Challenging due to infiltrative nature. Options: observation, sclerotherapy (e.g., OK-432, bleomycin), debulking surgery, CO2 laser. High recurrence rate.
⭐ Lymphangiomas are notorious for sudden hemorrhage leading to 'chocolate cysts' and acute proptosis.
High-Flow Lesions & Diagnostics - Arterial Alerts
High-flow: Arteriovenous Malformations (AVMs) & Carotid-Cavernous Fistulas (CCFs).
- AVMs/CCFs - Key Signs:
- Pulsatile proptosis
- Orbital bruit (auscultation)
- Chemosis, dilated "corkscrew" episcleral vessels
- Ophthalmoplegia, ↑IOP, vision loss risk
⭐ Direct Carotid-Cavernous Fistulas (CCFs) often present with the classic triad of pulsatile proptosis, chemosis, and an orbital bruit.
CCFs: Barrow's Classification (Simplified):
- Type A: Direct (ICA to Cavernous Sinus) - High flow.
- Type B: Indirect Dural (ICA meningeal branches to CS) - Low flow.
- Type C: Indirect Dural (ECA meningeal branches to CS) - Low flow.
- Type D: Indirect Dural (ICA & ECA meningeal branches to CS) - Low flow. 📌 Mnemonic for CCF Types (flow): Always High (Type A is High flow), B, C, D are Low.
Diagnostics: Imaging is vital. DSA is gold standard for CCF/AVM.
| Lesion | Doppler USG | CTA | MRA | DSA (Gold Standard) |
|---|---|---|---|---|
| CCF (Direct) | ↑ flow, arterialized SOV | Dilated SOV, proptosis | Dilated SOV, flow voids | Shows fistula, feeders |
| CCF (Indirect) | Variable SOV flow | Subtle SOV changes | Dural enhancement | Identifies feeders |
| Orbital AVM | High-flow, low resistance | Tangled vessels, early venous fill | Flow voids, nidus | Maps angioarchitecture |
High‑Yield Points - ⚡ Biggest Takeaways
- Capillary Hemangioma: Most common orbital tumor in childhood; spontaneous regression frequent. Propranolol is first-line medical therapy.
- Cavernous Hemangioma: Most common benign orbital tumor in adults; encapsulated, causing slow, progressive, painless proptosis.
- Lymphangioma: Non-encapsulated, infiltrative lesion; presents with sudden proptosis due to intralesional hemorrhage ("chocolate cysts").
- Orbital Varix: Characterized by intermittent proptosis that ↑ with Valsalva maneuver or dependent head position; phleboliths may be present.
- Carotid-Cavernous Fistula (Direct): Classic triad: pulsatile exophthalmos, orbital bruit, and marked chemosis with arterialized conjunctival veins.
- Sturge-Weber Syndrome: Associated with ipsilateral facial port-wine stain, choroidal hemangioma, and glaucoma (often congenital).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

