Orbital Imaging Intro & X-ray - Pixel Peepshow Kickoff
- Orbital imaging: Vital for diagnosis, pre-operative planning, and post-operative evaluation.
- X-ray (Plain Radiography):
- Initial, accessible, low-cost modality.
- Primarily for bony orbit trauma (fractures), radio-opaque foreign bodies.
- Limited soft tissue detail.
- Standard Views:
- Waters (Occipito-mental): Orbital floor.
- Caldwell (Occipito-frontal): Superior/lateral orbital rims.
- Lateral view.
- Look for: "Teardrop sign" (herniated orbital contents).
⭐ Waters view (occipito-mental) is best for orbital floor blowout fractures.
Ocular/Orbital Ultrasound - Echoes in the Orbit
- Non-ionizing, dynamic imaging using sound waves. High-frequency probes (10-20 MHz for globe) offer detailed views.
- A-scan (Amplitude):
- 1D display.
- Measures axial length (IOL power).
- Differentiates tissue (e.g., tumor spikes).
- B-scan (Brightness):
- 2D cross-sectional image.
- Assesses posterior segment, orbit.
- Key for opaque media.
- Detects retinal detachment, tumors, vitreous hemorrhage.
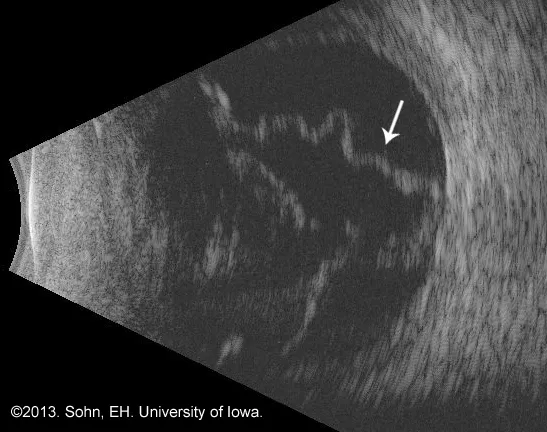
⭐ B-scan ultrasound is invaluable for evaluating intraocular structures when the media is opaque (e.g., dense cataract, vitreous hemorrhage).
Orbital CT Scan - CT's Bony Bonanza
- Primary Use: Evaluating orbital bones, fractures, and calcifications.
- Technique: Uses X-rays for cross-sectional imaging.
- Strengths:
- 🦴 Superior bony detail (gold standard for fractures).
- ⏱️ Rapid scans (ideal for trauma).
- Detects calcification & metallic foreign bodies.
- Good for acute hemorrhage.
- Limitations:
- Radiation exposure (⚠️ caution in children).
- Poorer soft tissue contrast than MRI.
- Key Indications:
- Orbital trauma (e.g., blowout fractures).
- Orbital cellulitis/abscess (bony involvement).
- Suspected calcified tumors.
⭐ CT scan is the gold standard for evaluating orbital trauma, especially fractures, and for identifying calcifications within orbital lesions.
Orbital MRI - MRI's Magnetic Magic
- Excels for soft tissue, optic nerve, intracranial views.
- No radiation. Gadolinium: caution in pregnancy.
- Key Sequences:
- T1W: Anatomy. Fat bright.
- +Gadolinium (T1W FS): Enhances lesions.
- T2W: Water bright (edema, cysts). Fat bright.
- Fat Suppression (STIR, T1FS): Vital for lesion conspicuity.
⭐ Fat suppression sequences (e.g., STIR, T1FS) on MRI are crucial for delineating inflammatory lesions or tumors within orbital fat, enhancing their conspicuity.
- DWI: Ischemia, abscess.
- T1W: Anatomy. Fat bright.
- Indications: Optic neuritis, tumors, inflammation (TED), vascular lesions.
- Avoid: Metal implants, pacemakers. 📌 MRI: No Metal Inside!
Imaging Modality Face-Off - Modality Match-Up Mania
Selecting the right orbital imaging is key. Match modality to suspected pathology:
⭐ For suspected optic nerve lesions or demyelinating disease affecting the orbit, MRI with gadolinium contrast and fat suppression is the investigation of choice.
High‑Yield Points - ⚡ Biggest Takeaways
- CT scan is the modality of choice for bony orbital trauma and calcifications.
- MRI excels for soft tissue differentiation, optic nerve, and orbital apex lesions.
- T1-weighted MRI highlights anatomy and fat; T2-weighted shows water, edema, or inflammation.
- Gadolinium contrast on MRI enhances vascular lesions, inflammation, and tumors.
- Ultrasound B-scan is valuable for anterior segment, globe lesions, and optic nerve drusen.
- Dacryocystography (DCG) is specific for evaluating the lacrimal drainage system.
- Plain X-rays have a limited role, mainly for metallic foreign bodies and gross fractures if CT is unavailable.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more


