Optics and Refraction

On this page
🔬 The Light-Bending Mastery: Optical Foundations
Light bends at every interface in the eye, and mastering these refractions unlocks your ability to diagnose and correct vision with precision. You'll learn how optical principles govern image formation, why specific refractive errors produce characteristic symptoms, and how to select evidence-based treatments that restore clarity. By integrating foundational physics with pattern recognition and clinical algorithms, you'll build the systematic expertise needed to evaluate any refractive complaint confidently and prescribe the right correction every time.
📌 Remember: CORNEA - Contributes Over Roughly Nearly Eighty percent of All refractive power (43D out of 60D total)
The fundamental principle governing all optical phenomena is Snell's Law: n₁ sin θ₁ = n₂ sin θ₂, where refractive indices determine how dramatically light bends at interfaces. The cornea-air interface (n = 1.376 to n = 1.000) creates the most significant refractive change in the visual system.
- Critical Refractive Indices
- Air: 1.000 (reference standard)
- Cornea: 1.376 (primary refracting surface)
- Tear film: 1.336 (smooths optical surface)
- Corneal stroma: 1.380 (structural component)
- Aqueous humor: 1.336 (minimal refractive change)
- Crystalline lens: 1.406 (variable with accommodation)
- Vitreous: 1.336 (maintains eye shape)
⭐ Clinical Pearl: The cornea-air interface accounts for 65-75% of the eye's total refractive power, explaining why corneal irregularities cause disproportionate visual disturbances
| Optical Component | Refractive Power | Interface Change | Clinical Significance | Measurement Method | Normal Range |
|---|---|---|---|---|---|
| Cornea | +43.00D | +43.00D | Primary refractor | Keratometry | 41.00-46.00D |
| Crystalline Lens | +17.00D | +4.00D | Accommodation | A-scan biometry | 19.00-22.00D |
| Aqueous-Lens | +6.00D | +6.00D | Focusing fine-tune | Scheimpflug imaging | ±1.00D variation |
| Lens-Vitreous | -6.00D | -6.00D | Posterior surface | OCT measurement | ±0.50D variation |
| Total System | +60.00D | +60.00D | Overall convergence | Autorefraction | ±0.25D accuracy |
The concept of vergence describes light ray behavior as V = n/f, where vergence equals refractive index divided by focal length. Parallel light rays from infinity have zero vergence, while diverging rays from near objects carry negative vergence requiring additional positive vergence for retinal focus.
📌 Remember: VERGENCE - Very Essential Ray Grouping Equation: Needs Calculation Everywhere (V = n/f)
Understanding these optical principles transforms complex refractive calculations into predictable patterns, setting the foundation for mastering clinical refraction techniques and surgical planning.
🔬 The Light-Bending Mastery: Optical Foundations
⚡ The Refraction Revolution: Light's Journey Through Matter
The power of a lens in diopters equals P = (n₂ - n₁)/R, where the refractive index difference and radius of curvature determine focusing strength. For the cornea's anterior surface: P = (1.376 - 1.000)/0.0078m = +48.2D, though the effective power reduces to +43D due to corneal thickness effects.
- Refractive Power Calculations
- Anterior corneal surface: +48.20D (theoretical)
- Posterior corneal surface: -5.20D (diverging)
- Net corneal power: +43.00D (clinical measurement)
- Corneal thickness effect: -0.50D (reduces anterior power)
- Crystalline lens surfaces: +17.00D (combined)
- Anterior lens surface: +10.00D (steeper curvature)
- Posterior lens surface: +7.00D (flatter curvature)
⭐ Clinical Pearl: The posterior corneal surface contributes -5.20D of negative power, explaining why posterior corneal irregularities in conditions like Fuchs' dystrophy cause significant visual disturbance despite affecting only 12% of total corneal power

| Optical Interface | Power Contribution | Radius of Curvature | Refractive Index Change | Clinical Measurement | Pathological Range |
|---|---|---|---|---|---|
| Anterior Cornea | +48.20D | 7.8mm | +0.376 | Keratometry | >52D (steep) |
| Posterior Cornea | -5.20D | 6.2mm | -0.040 | Scheimpflug | <-6D (irregular) |
| Anterior Lens | +10.00D | 12.0mm | +0.070 | A-scan | Variable |
| Posterior Lens | +7.00D | -8.0mm | -0.070 | OCT | Age-dependent |
| Total System | +60.00D | Variable | Combined | Autorefraction | ±6.00D range |
💡 Master This: Accommodation amplitude = 15 - (age/4) provides a quick clinical estimate, explaining why presbyopia symptoms begin around age 40-45 when accommodation drops below 3.00D
📌 Remember: ACCOMMODATION - Age Causes Ciliary Optical Muscle Movement Of Diopters Always To Increase Optical Near focusing
Chromatic aberration occurs because different wavelengths refract differently, with blue light (480nm) focusing 1.50D stronger than red light (650nm). This longitudinal chromatic aberration spans approximately 2.50D across the visible spectrum, requiring careful consideration in multifocal IOL design.
Understanding these refractive principles enables precise prediction of optical outcomes, forming the foundation for advanced diagnostic techniques and surgical interventions.
⚡ The Refraction Revolution: Light's Journey Through Matter
🎯 The Pattern Recognition Arsenal: Clinical Refraction Mastery

- Systematic Refraction Protocol
- Step 1: Maximum plus to best visual acuity (20/20 target)
- Start with +1.00D above autorefraction
- Reduce plus in 0.25D steps until acuity drops
- Final sphere: most positive giving 20/20 vision
- Step 2: Cylinder axis determination (±5° accuracy)
- Use Jackson cross-cylinder technique
- Bracket axis in 15° then 5° increments
- Confirm with clock dial or fan chart
- Step 3: Cylinder power refinement (±0.25D precision)
- Apply ±0.25D cross-cylinder flips
- Patient preference determines final cylinder power
- Verify with duochrome test (red-green balance)
- Step 1: Maximum plus to best visual acuity (20/20 target)
📌 Remember: SPHERE FIRST - Start Positive, Halt Early, Refine Exactly - Follow In Repeated Small Tests
The duochrome test exploits chromatic aberration to fine-tune spherical power. Red light (650nm) focuses 0.75D behind green light (530nm), so patients preferring red letters need more plus power, while those preferring green letters are over-plussed.
⭐ Clinical Pearl: Over-minusing by just 0.50D can reduce contrast sensitivity by 15-20% and cause asthenopic symptoms in 85% of patients under age 35
| Refractive Error | Visual Symptoms | Objective Signs | Correction Strategy | Success Rate | Follow-up Timing |
|---|---|---|---|---|---|
| Myopia | Distance blur | Minus acceptance | Most negative sphere | >95% | 2-4 weeks |
| Hyperopia | Near fatigue | Plus improvement | Most positive sphere | >90% | 1-2 weeks |
| Astigmatism | Distorted vision | Cylinder clarity | Precise axis/power | >92% | 3-4 weeks |
| Presbyopia | Near difficulty | Add requirement | Progressive/bifocal | >88% | 4-6 weeks |
| Anisometropia | Eyestrain | Unequal refraction | Contact lenses | >85% | 2-3 weeks |
- Cross-Cylinder Methodology
- Axis refinement: Cross-cylinder axis 45° to trial cylinder
- Patient chooses clearer image between two positions
- Move trial cylinder axis toward cross-cylinder minus axis
- Repeat until no preference achieved
- Power refinement: Cross-cylinder axis aligned with trial cylinder
- "More" position adds +0.25D cylinder power
- "Less" position reduces -0.25D cylinder power
- Stop when patient reports equal clarity
- Axis refinement: Cross-cylinder axis 45° to trial cylinder
💡 Master This: The "FORS" rule - Flip Opposite, Rotate Same - when patient prefers the flip, move axis opposite to cross-cylinder minus; when patient prefers rotation position, move axis same direction as cross-cylinder minus
📌 Remember: CROSS-CYLINDER - Choose Rotation Or Sphere Selection - Cylinder Yields Less If Not Done Exactly Right
Binocular balancing ensures equal accommodative demand between eyes, preventing fixation preference and suppression. The prism dissociation method using 3Δ base-down before the right eye allows simultaneous comparison of both eyes' visual acuity.

These systematic approaches transform subjective refraction from guesswork into precise, reproducible measurements that optimize visual performance and patient satisfaction.
🎯 The Pattern Recognition Arsenal: Clinical Refraction Mastery
🔍 The Diagnostic Discrimination Matrix: Refractive Error Analysis
Spherical equivalent calculations provide the foundation for refractive error classification: SE = Sphere + (Cylinder/2). This formula reduces complex astigmatic prescriptions to single values enabling systematic comparison and progression tracking.
- Refractive Error Classification Thresholds
- Emmetropia: ±0.50D spherical equivalent
- Low physiological variation: ±0.25D (normal)
- Borderline significance: ±0.50D (monitor)
- Clinical threshold: >±0.75D (correct)
- Myopia severity grading: Based on spherical equivalent
- Low myopia: -0.50D to -3.00D (common)
- Moderate myopia: -3.25D to -6.00D (progressive risk)
- High myopia: >-6.00D (pathological complications)
- Hyperopia management levels: Age-dependent correction
- Infants: Correct >+3.00D (amblyopia risk)
- Children: Correct >+2.00D (accommodative strain)
- Adults: Correct >+1.00D (symptomatic relief)
- Emmetropia: ±0.50D spherical equivalent
⭐ Clinical Pearl: Anisometropia exceeding 1.50D spherical equivalent difference causes amblyopia in 65% of children under 8 years, requiring immediate correction to prevent permanent visual loss
| Refractive Parameter | Normal Range | Mild Abnormality | Moderate Abnormality | Severe Abnormality | Intervention Threshold |
|---|---|---|---|---|---|
| Spherical Equivalent | ±0.50D | ±0.75-2.00D | ±2.25-6.00D | >±6.00D | >±0.75D |
| Astigmatism | <0.75D | 0.75-1.50D | 1.75-3.00D | >3.00D | >1.00D |
| Anisometropia | <1.00D | 1.00-1.50D | 1.75-3.00D | >3.00D | >1.50D |
| Accommodation | Age-dependent | 2D below norm | 4D below norm | >6D below norm | Symptomatic |
| Pupil Size | 3-5mm | 2-3mm or 5-6mm | <2mm or >6mm | Fixed size | Functional impact |
📌 Remember: ASTIGMATISM AXES - With-the-rule Is Tall (90°), Against-the-rule Goes Across (180°), Oblique Occurs Otherwise
Irregular astigmatism patterns indicate corneal pathology requiring specialized management. Keratoconus creates inferior steepening with asymmetric bow-tie patterns on topography, while pellucid marginal degeneration shows inferior thinning with crab-claw patterns.
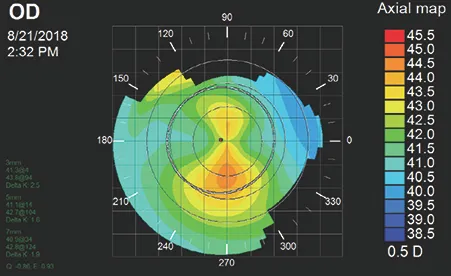
- Irregular Astigmatism Differential Diagnosis
- Keratoconus indicators: >1.50D inferior-superior asymmetry
- Topographic signs: Asymmetric bow-tie, >47D central K
- Clinical signs: Munson's sign, Fleischer ring, Vogt striae
- Progression markers: >1.00D annual steepening
- Pellucid marginal degeneration: 4-8mm inferior thinning
- Topographic pattern: Crab-claw configuration
- Clinical appearance: Clear cornea with inferior ectasia
- Against-the-rule shift: >2.00D cylinder change
- Post-surgical irregularity: Radial keratotomy complications
- Diurnal fluctuation: >1.00D variation
- Starbursts/halos: Night vision symptoms
- Progressive hyperopia: +0.25D annual shift
- Keratoconus indicators: >1.50D inferior-superior asymmetry
💡 Master This: Corneal irregularity exceeding 1.50D between superior and inferior hemispheres suggests ectatic disease, requiring rigid contact lens fitting or corneal cross-linking evaluation
Presbyopia progression follows predictable patterns: accommodation amplitude decreases from 15.00D at age 10 to 1.00D at age 60, requiring reading additions starting around age 42-45 in emmetropic patients.

These discriminatory frameworks enable precise diagnosis and appropriate management selection, transforming complex refractive presentations into systematic treatment pathways.
🔍 The Diagnostic Discrimination Matrix: Refractive Error Analysis
⚖️ The Treatment Algorithm Engine: Evidence-Based Refractive Management
Spectacle correction remains first-line treatment for 85% of refractive errors, offering safety, reversibility, and cost-effectiveness. Modern lens designs incorporate aspheric surfaces reducing spherical aberration by 40-60% and anti-reflective coatings improving light transmission to 99.5%.
- Contact Lens Selection Algorithm
- Spherical errors: Soft daily disposables preferred
- Low to moderate myopia: -1.00D to -6.00D range
- Success rate: >92% first-time wearers
- Replacement schedule: Daily (lowest infection risk)
- Astigmatism correction: Toric lens designs required
- Cylinder range: -0.75D to -2.25D available
- Axis availability: 10° increments standard
- Stability requirement: <15° rotation acceptable
- High ametropia: Rigid gas permeable lenses optimal
- Myopia >-8.00D: Reduces minification effects
- Hyperopia >+4.00D: Improves field of view
- Irregular astigmatism: Masks corneal irregularities
- Spherical errors: Soft daily disposables preferred
⭐ Clinical Pearl: Contact lens-induced corneal warpage occurs in 15-20% of long-term PMMA wearers, requiring 6-8 weeks of discontinuation before accurate refraction or refractive surgery evaluation
| Treatment Option | Success Rate | Adaptation Time | Cost Factor | Maintenance | Complication Risk |
|---|---|---|---|---|---|
| Spectacles | >95% | Immediate | Low | Minimal | <1% |
| Soft Contact Lens | >90% | 1-2 weeks | Moderate | Daily care | 5-8% |
| RGP Contact Lens | >85% | 4-6 weeks | Moderate | Daily care | 3-5% |
| LASIK Surgery | >95% | 1-3 months | High | None | 2-3% |
| PRK Surgery | >92% | 3-6 months | High | None | 1-2% |
- Progressive Lens Design Parameters
- Corridor length: 14-22mm (longer = smoother transition)
- Short corridor: 14-16mm (compact frames)
- Standard corridor: 18-20mm (optimal comfort)
- Long corridor: 20-22mm (minimal distortion)
- Addition power progression: Age-related requirements
- Age 42-45: +1.00D to +1.50D addition
- Age 46-50: +1.75D to +2.25D addition
- Age 51-60: +2.50D to +3.00D addition
- Age >60: +3.00D to +3.50D maximum
- Corridor length: 14-22mm (longer = smoother transition)
📌 Remember: PROGRESSIVE LENSES - Patient Requires Optimal Gradual Reading Enhancement Smoothly Starting In Vision Early
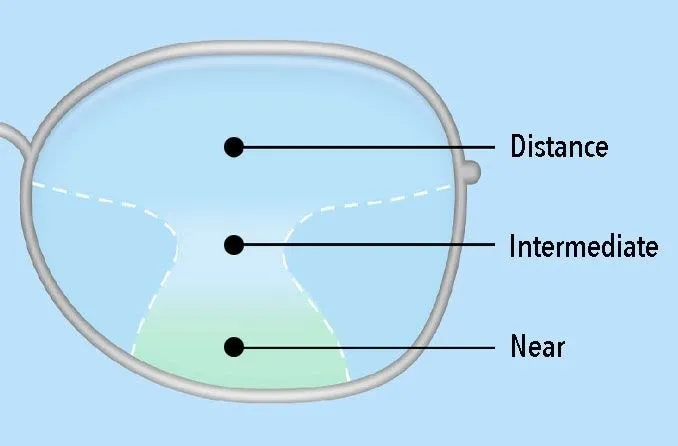
Refractive surgery candidacy requires comprehensive evaluation including corneal thickness (>500μm post-ablation), pupil size (<6mm photopic), and refractive stability (<0.50D change annually for 2 years).
💡 Master This: LASIK flap thickness (100-160μm) plus ablation depth (12-15μm per diopter) must leave >250μm residual stromal bed to prevent post-operative ectasia
Multifocal contact lens designs utilize simultaneous vision principles, where distance and near zones create overlapping images on the retina. Neuroadaptation occurs over 6-12 weeks, with success rates of 75-85% in motivated patients.
These evidence-based algorithms ensure optimal treatment selection, maximizing visual outcomes while minimizing complications and patient dissatisfaction.
⚖️ The Treatment Algorithm Engine: Evidence-Based Refractive Management
🔗 The Integration Nexus: Multi-System Optical Convergence
Accommodative-convergence coupling links focusing and eye alignment through shared neural pathways. The AC/A ratio (accommodative convergence per diopter of accommodation) averages 4Δ/D, meaning every 1.00D of accommodation triggers 4 prism diopters of convergence movement.
- Binocular Vision Integration Mechanisms
- Accommodative system: Parasympathetic control via Edinger-Westphal nucleus
- Accommodation lag: 0.50-0.75D behind stimulus
- Response time: 300-400 milliseconds for 2.00D change
- Depth of focus: ±0.50D before blur detection
- Convergence system: Medial rectus coordination
- Fusional convergence: 25-40Δ reserve capacity
- Proximal convergence: Distance-independent component
- Tonic convergence: Baseline resting position
- Pupillary system: Light and near response integration
- Pupil constriction: 1-2mm diameter reduction
- Depth of field: Increases 2-3x with miosis
- Aberration reduction: Improved optical quality
- Accommodative system: Parasympathetic control via Edinger-Westphal nucleus
⭐ Clinical Pearl: Accommodative insufficiency affects 15-20% of computer users, causing asthenopic symptoms despite perfect refractive correction, requiring plus lenses for near work
Contrast sensitivity function reveals spatial frequency processing capabilities beyond standard visual acuity. Peak sensitivity occurs at 3-5 cycles per degree, with significant reduction at high frequencies (>20 cpd) indicating optical aberrations or neural processing deficits.
| Spatial Frequency | Normal Threshold | Mild Reduction | Moderate Loss | Severe Impairment | Clinical Significance |
|---|---|---|---|---|---|
| 1.5 cpd | >100 | 50-100 | 20-50 | <20 | Mobility function |
| 3.0 cpd | >200 | 100-200 | 50-100 | <50 | Face recognition |
| 6.0 cpd | >150 | 75-150 | 30-75 | <30 | Reading ability |
| 12.0 cpd | >50 | 25-50 | 10-25 | <10 | Detail discrimination |
| 18.0 cpd | >20 | 10-20 | 5-10 | <5 | Fine visual tasks |
Wavefront aberrometry quantifies higher-order aberrations using Zernike polynomials, revealing optical imperfections beyond sphere and cylinder. Root mean square (RMS) values above 0.30μm for higher-order aberrations significantly impact visual quality.
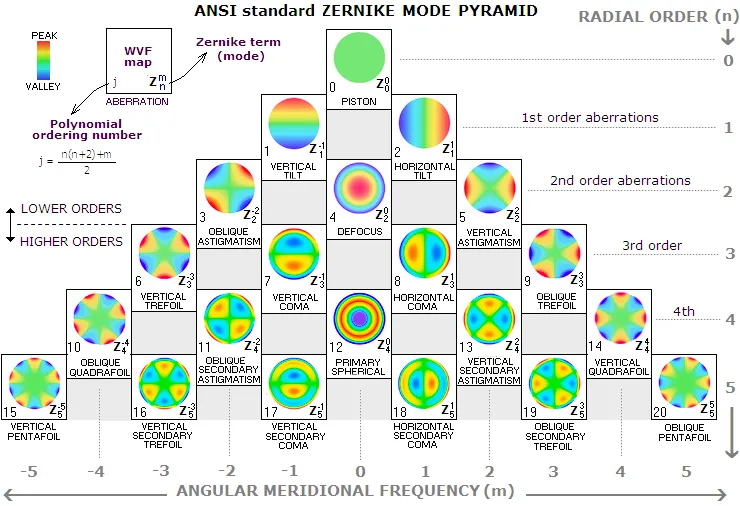
- Higher-Order Aberration Clinical Impact
- Spherical aberration (Z₄⁰): Pupil size dependent
- Positive SA: +0.10-0.30μm (normal aging)
- Night vision impact: Halos and starbursts
- IOL selection: Aspheric designs reduce SA
- Coma aberration (Z₃¹, Z₃⁻¹): Asymmetric blur
- Decentered optics: Contact lens or IOL displacement
- Corneal irregularity: Post-surgical complications
- Threshold: >0.20μm causes noticeable symptoms
- Trefoil aberration (Z₃³, Z₃⁻³): Three-fold symmetry
- Corneal warpage: Contact lens induced changes
- Surgical complications: Irregular healing patterns
- Correction difficulty: Requires specialized optics
- Spherical aberration (Z₄⁰): Pupil size dependent
💡 Master This: Pupil size changes from 2mm (bright) to 7mm (dark) increase spherical aberration by 16-fold (fourth power relationship), explaining night vision complaints in post-refractive surgery patients
Neuroplasticity enables visual system adaptation to optical changes over weeks to months. Multifocal IOL patients develop neural suppression of out-of-focus images, achieving functional vision despite simultaneous retinal images.
Tear film dynamics create the eye's first optical surface, with lipid layer thickness of 50-100nm preventing evaporation and mucin layer ensuring uniform spreading. Tear breakup time below 10 seconds causes optical fluctuations affecting visual quality.
These integrated systems demonstrate how optimal vision requires coordination between optical, neural, and physiological components, explaining why successful refractive outcomes depend on comprehensive evaluation beyond simple refraction.
🔗 The Integration Nexus: Multi-System Optical Convergence
🎯 The Clinical Mastery Toolkit: Rapid-Fire Refractive Expertise
Essential Refractive Thresholds form the foundation of clinical decision-making, providing instant reference points for treatment planning and outcome prediction.
- Critical Clinical Numbers Arsenal
- Corneal power: 43.00D (41-46D normal range)
- Total eye power: 60.00D (±3.00D variation)
- Accommodation amplitude: 15 - (age/4) formula
- Anisometropia threshold: 1.50D (amblyopia risk)
- Astigmatism significance: >0.75D (correction needed)
- AC/A ratio: 4Δ/D (normal convergence)
- Pupil size range: 2-7mm (light-dependent)
- Tear breakup time: >10 seconds (stable optics)
📌 Remember: RAPID REFRACTION - Recall All Power Important Diopter - Ranges Essential For Reliable Accurate Clinical Treatment In Ophthalmology Now
| Clinical Scenario | Immediate Action | Key Threshold | Success Predictor | Follow-up Timing | Red Flag Warning |
|---|---|---|---|---|---|
| New Myopia | Cycloplegic refraction | >-0.50D | Stable measurement | 6 months | >1.00D/year |
| Presbyopia Onset | Near addition | +1.00D start | Gradual increase | Annual | Sudden change |
| Astigmatism | Axis verification | >0.75D | Stable axis | 2 years | Irregular pattern |
| Anisometropia | Amblyopia screen | >1.50D | Equal acuity | 3 months | Suppression |
| Contact lens | Fit assessment | Movement <1mm | Comfort >8hrs | 1 week | Red eye |
⭐ Clinical Pearl: "20/20 but can't see" complaints suggest contrast sensitivity loss, higher-order aberrations, or binocular dysfunction requiring specialized testing beyond routine refraction
Advanced Integration Protocols synthesize multiple data sources for comprehensive management decisions.
- Systematic Integration Framework
- Objective measurements: Autorefraction + Keratometry + Biometry
- Correlation check: ±0.50D agreement expected
- Reliability indicators: Standard deviation <0.25D
- Repeatability: 3 measurements within ±0.25D
- Subjective refinement: Patient preferences + Lifestyle demands
- Visual priorities: Distance vs near emphasis
- Occupational needs: Computer work vs driving
- Recreational activities: Sports vs reading
- Binocular assessment: Fusion + Accommodation + Convergence
- Phoria measurements: Distance and near positions
- Fusional reserves: Convergence and divergence amplitudes
- Accommodation facility: ±2.00D flippers >8 cpm
- Objective measurements: Autorefraction + Keratometry + Biometry
💡 Master This: Successful refractive outcomes require matching correction to visual demands - computer users need slight under-correction (-0.25D) while drivers require full distance correction
Emergency Recognition Patterns identify urgent referral situations requiring immediate attention.
📌 Remember: URGENT REFERRAL - Unusual Rapid Growing Eye Needs Thorough - Retinal Examination Fundus Evaluation Right Right Away Lest Loss
- Red Flag Indicators
- Sudden refractive change: >1.00D in <6 months
- Unilateral myopia: New onset in adult
- Irregular astigmatism: Asymmetric topography pattern
- Reduced best-corrected acuity: Unexplained vision loss
- Fluctuating vision: Diabetes or medication related
These rapid-access tools and systematic protocols transform complex refractive cases into manageable clinical decisions, ensuring optimal outcomes through evidence-based practice and pattern recognition mastery.
🎯 The Clinical Mastery Toolkit: Rapid-Fire Refractive Expertise
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























