Indications & Pre-op Eval - Setting the Stage
- Indications:
- Retinal Detachment (RD): Rhegmatogenous, Tractional
- Vitreous Hemorrhage (non-clearing)
- Macular Hole, Epiretinal Membrane (ERM)
- Proliferative Diabetic Retinopathy (PDR) complications (TRD, VH)
- Endophthalmitis, Intraocular Foreign Body (IOFB)
- Pre-op Evaluation:
- History (systemic/ocular), Visual Acuity (VA), IOP
- Slit-lamp & dilated fundus exam (indirect ophthalmoscopy)
- Key Investigations:
- B-scan: Essential for opaque media (VH, cataract)
- OCT: Macular details (MH, ERM)
- Systemic fitness, consent (risks/benefits)
⭐ B-scan ultrasonography is indispensable for diagnosing RD and planning surgery when media opacity obscures the fundus view.

Core Surgical Steps - Eye's Inner Workings
- Setup: Anesthesia (Peribulbar/GA). Conjunctival peritomy.
- Ports (Sclerotomies): 3 ports via pars plana.
- Sizes: 23G, 25G, 27G.
- Placement: Infusion (maintains IOP), Light pipe (illumination), Vitrector (cuts/aspirates vitreous).
- Distance: 3.5-4 mm (phakic/pseudophakic), 3-3.5 mm (aphakic) from limbus.
- Vitrectomy: Core (central) & Peripheral (base, often with scleral depression).
- Pathology Management: Membrane peeling, endolaser photocoagulation.
- Tamponade: Fluid-Air Exchange (FAX) → Gas ($SF_6$, $C_3F_8$) / Silicone Oil.
- Closure: Sutureless (small gauge) or sutured ports.

⭐ Silicone oil provides longer tamponade than gas; preferred for inferior breaks or Proliferative Vitreoretinopathy (PVR).
Intraocular Tamponades - Space Fillers Supreme
- Function: Internal retinal support, appose retina to RPE.
- Types:
- Gases: Absorb spontaneously.
- Air (shortest acting, ~3 days).
- Expansile: SF6 (~2 wks), C2F6 (~4 wks), C3F8 (~8 wks).
- 📌 Mnemonic (Expansion/Duration↑): Some Fine Carbon lasts Long (SF6 < C2F6 < C3F8 < Silicone Oil).
- Non-expansile conc: SF6 20%, C3F8 14%.
- Caution: No air travel/N2O with expansile gas.

- Silicone Oil: Long-term; optically clear.
- Viscosities: 1000, 5000 cS.
- Needs removal. Complications: Emulsification, keratopathy, ↑IOP.
- Gases: Absorb spontaneously.
⭐ Gases cause initial myopic shift (bubble acts as minus lens); Silicone oil causes hyperopic shift (acts as plus lens).
Post-op & Complications - Aftercare & Alerts
- Immediate Aftercare
- Strict head positioning (e.g., face-down with gas).
- Meds: Topical steroids, antibiotics, cycloplegics, analgesics.
- Monitor IOP (target <21 mmHg); report significant ↑.
- Activity: Avoid strenuous tasks, head jerks, rubbing.
- Critical Alerts (Seek Urgent Review)
- Sudden, severe, or increasing pain.
- Marked ↓vision, new floaters/flashes, field defects (curtain).
- Signs of infection: ↑Redness, discharge, lid swelling.
- Key Complications
- Early: ↑IOP, corneal edema, uveitis, vitreous hemorrhage.
- Late: Endophthalmitis (⚠️ emergency!), recurrent RD, PVR, CME, ERM, cataract.

⭐ Staphylococcus epidermidis is the most frequent cause of post-vitrectomy endophthalmitis.
Specific VR Surgeries - Spotlight Procedures
- Pars Plana Vitrectomy (PPV):
- Uses: RD, VH, ERM, MH, Endophthalmitis.
- Core: Vitreous removal, address pathology, tamponade (gas/oil).
- Scleral Buckling (SB):
- For RRD: esp. phakic, young, inferior breaks. Supports break.
- Pneumatic Retinopexy (PR):
- Select RRDs: Superior breaks (e.g., 10-2 o'clock), clear media. Gas + laser/cryo.
- Macular Hole Surgery:
- PPV + ILM peel + gas. High success.
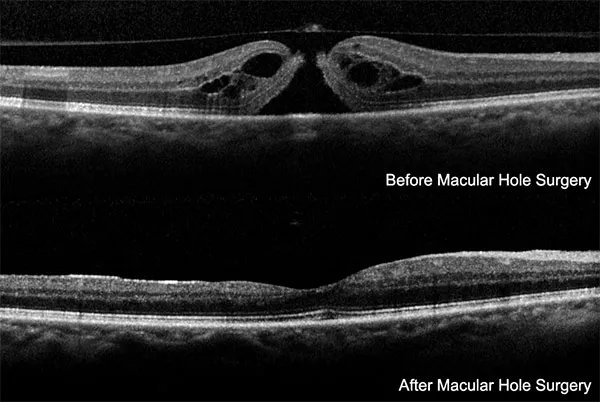
- ERM Peeling: PPV to remove macular scar tissue.
⭐ ILM peeling in macular hole surgery boosts anatomical closure (>90%) & vision.
High‑Yield Points - ⚡ Biggest Takeaways
- Pars Plana Vitrectomy (PPV): Mainstay for posterior segment issues like RD, vitreous hemorrhage.
- PPV also treats macular holes, epiretinal membranes, and removes intraocular foreign bodies (IOFBs).
- Tamponade: Silicone oil or gases (SF6, C3F8); specific post-op positioning is critical with gas.
- Endolaser photocoagulation seals retinal breaks and is used for panretinal photocoagulation (PRP).
- Scleral buckling: External procedure, often for phakic RDs with peripheral breaks.
- Commonest PPV complication: iatrogenic cataract; others: raised IOP, endophthalmitis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

