Anterior Segment Anatomy - Eye's Front Door
- Eyelid (Layers A→P): Skin → Subcutaneous → Orbicularis oculi → Tarsal plate/Orbital septum → Palpebral conjunctiva.
- Cornea (Layers A→P): 📌 "ABCDE"
- Anterior Epithelium
- Bowman's Layer
- Corneal Stroma (~90% thickness)
- Descemet's Membrane
- Endothelium (maintains corneal clarity via deturgescence)
⭐ Corneal endothelium: ~3000 cells/mm² at birth, non-regenerative; critical for transparency.
- AC Angle (Structures P→A): 📌 "I Can See The Line" (Iris root, Ciliary body, Scleral spur, Trabecular meshwork, Schwalbe's Line)
- Trabecular Meshwork: Main aqueous outflow pathway.
- Schwalbe's Line: Peripheral termination of Descemet's membrane.
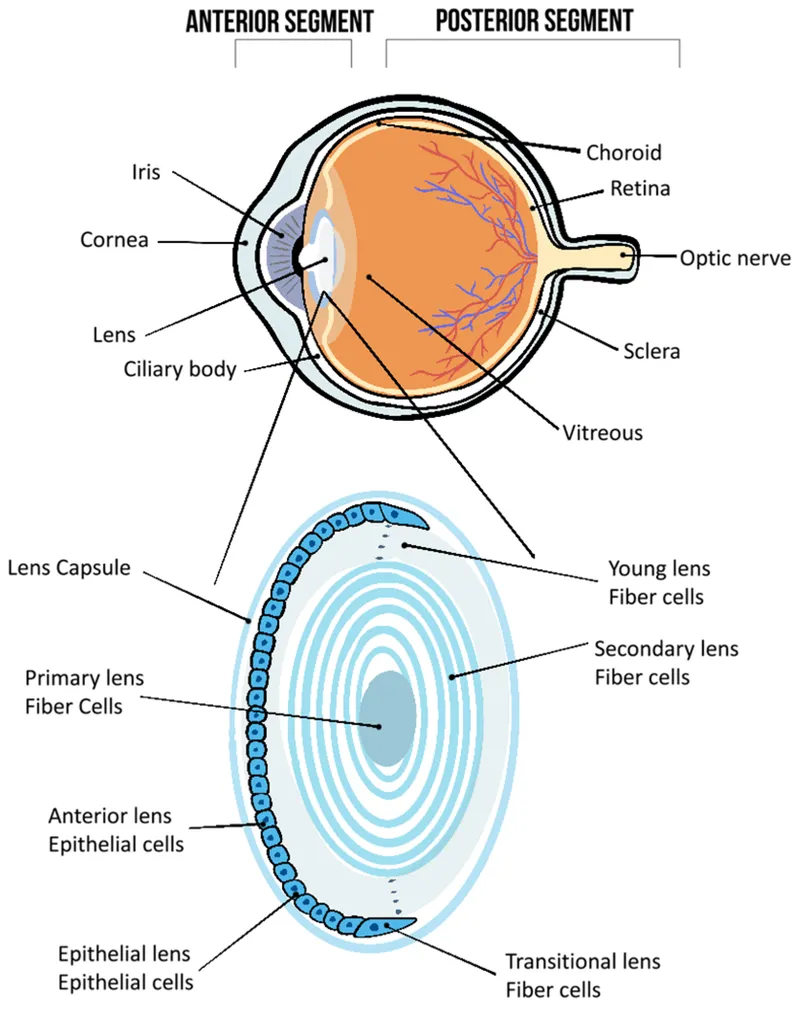
- Lens: Avascular, biconvex structure.
- Capsule (important for IOL fixation), Cortex, Nucleus (undergoes sclerosis with age). Zonules provide suspensory support.
 oka
oka
- Capsule (important for IOL fixation), Cortex, Nucleus (undergoes sclerosis with age). Zonules provide suspensory support.
Posterior Segment Anatomy - Backstage Wonders
- Vitreous Humor (80% eye volume)
- Gel: 99% water, Type II collagen, hyaluronic acid.
- Attachments (strongest first): Vitreous base (ora serrata), posterior lens capsule, optic disc margin, macula, retinal vessels. 📌 Mnemonic: "Very Strong Love Makes People Romantic".
- Retina (Neurosensory layer)
- 10 Layers (outer to inner): RPE, Photoreceptors (rods/cones), ELM, ONL, OPL, INL, IPL, GCL, NFL, ILM.
- Ora Serrata: Scalloped anterior retinal termination.
- Macula Lutea (~5.5 mm): Central, high-acuity vision.
- Fovea Centralis (~1.5 mm): Avascular; peak cone density.
- Foveola (~0.35 mm): Pure cones; sharpest vision.
- Optic Disc (Blind Spot; ~1.5 mm diameter)
- Features: Optic cup, neuroretinal rim (ISNT rule: Inf > Sup > Nasal > Temp).
- Lamina cribrosa: Scleral sieve for optic nerve axons.

⭐ The foveola (~0.35 mm) contains only cones, their nuclei (part of ONL), Henle's fiber layer (OPL), and ILM; offering maximal visual acuity.
Extraocular Muscles & Orbit - Eye's Support Crew
- Extraocular Muscles (EOMs): 4 Recti, 2 Obliques.
- 📌 Innervation: LR6SO4R3 (LR: CN VI, SO: CN IV, Rest: CN III).
| Muscle | Primary Action(s) | Innervation |
|---|---|---|
| Lateral Rectus | Abduction | CN VI |
| Medial Rectus | Adduction | CN III |
| Superior Rectus | Elevation, Adduction, Intorsion | CN III |
| Inferior Rectus | Depression, Adduction, Extorsion | CN III |
| Superior Oblique | Intorsion, Depression, Abduction | CN IV |
| Inferior Oblique | Extorsion, Elevation, Abduction | CN III |
- Roof: Frontal, Sphenoid (Lesser wing).
- Floor: Maxilla, Zygomatic, Palatine. (Blowout # site)
- Medial: Ethmoid (Lamina papyracea), Lacrimal, Maxilla, Sphenoid.
- Lateral: Zygomatic, Sphenoid (Greater wing).
- Key Openings & Contents:
- Optic Canal: CN II, Ophthalmic Artery.
- Superior Orbital Fissure (SOF): CN III, IV, V1, VI; Sup. Ophthalmic Vein.
- Inferior Orbital Fissure (IOF): CN V2, Infraorbital vessels; Inf. Ophthalmic Vein.
⭐ The orbital floor (maxillary bone) is the most common site for "blowout" fractures.
ContentView
Ocular Neurovascular Supply - Eye's Lifelines
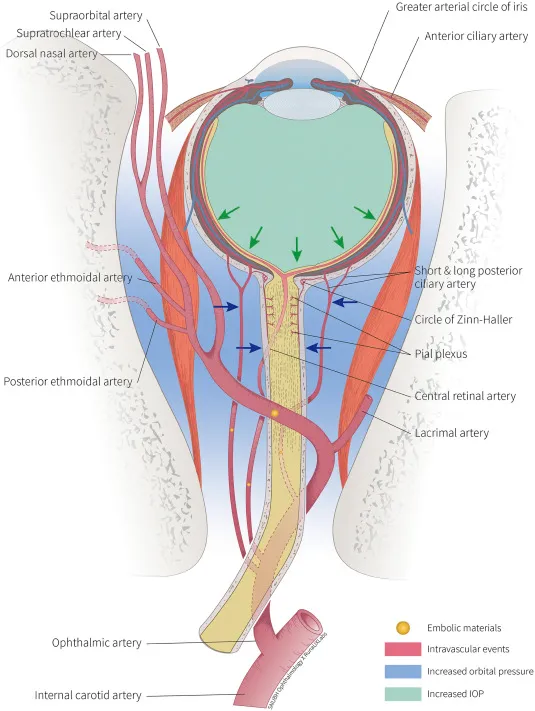
- Arterial Supply: Ophthalmic Artery (branch of Internal Carotid Artery) is key.
- Central Retinal Artery (CRA): Inner retina; end-artery.
- Short Posterior Ciliary Arteries (SPCAs): Choroid, optic disc (Circle of Zinn-Haller).
- Long Posterior Ciliary Arteries (LPCAs): Ciliary body, iris, major arterial circle.
- Anterior Ciliary Arteries (ACAs): From muscular arteries; supply anterior segment.
- Venous Drainage: Vortex veins (choroid), CRV (retina), ACVs → Superior & Inferior Ophthalmic Veins → Cavernous Sinus.
- Innervation:
- Sensory: CN V1 (Nasociliary → cornea/iris; Frontal; Lacrimal).
- Motor: CN III (most EOMs, LPS), CN IV (SO), CN VI (LR).
- Autonomic:
- Parasympathetic (CN III via ciliary ganglion): Sphincter pupillae, ciliary muscle.
- Sympathetic (Carotid plexus): Dilator pupillae, Müller's muscle.
⭐ Central Retinal Artery is an end-artery; its occlusion leads to sudden, painless vision loss.
High‑Yield Points - ⚡ Biggest Takeaways
- Cornea: 5 layers; Descemet's membrane and Endothelium are vital for transparency and function.
- Anterior Chamber Angle: Structures like Trabecular Meshwork and Schlemm's Canal are crucial for aqueous outflow and glaucoma surgery.
- Ora Serrata: Marks the anterior termination of the retina; a key landmark for pars plana vitrectomy.
- Extraocular Muscle Insertions (Spiral of Tillaux): Distances from limbus are MR 5.5mm, IR 6.5mm, LR 6.9mm, SR 7.7mm.
- Sclera: Thinnest (~0.3mm) just posterior to the rectus muscle insertions.
- Vortex Veins: Typically 4-7 in number, drain the choroid, and exit sclera posterior to the equator; critical to identify and preserve during retinal surgery.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

