Refractive Errors & Candidacy - Setting the Stage
- Refractive Errors:
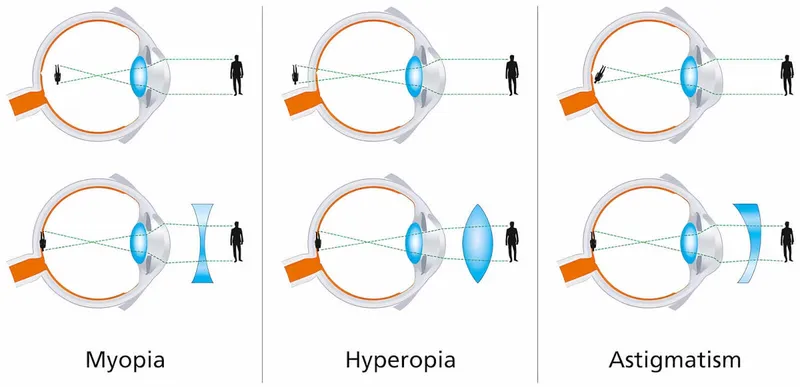
- Myopia: Focus before retina; concave (-) lens.
- Hyperopia: Focus behind retina; convex (+) lens.
- Astigmatism: Multiple foci; cylindrical lens.
- Presbyopia: Age-related ↓ accommodation.
- Candidacy Essentials: (📌 S.A.F.E.R.)
- Stable Refraction: <0.5D change/ ≥1 yr.
- Age: ≥18 yrs (ideally >21).
- Favourable Corneal Thickness (CT): Adequate (LASIK: pre-op ~500µm, RSB ≥250-300µm).
- Expectations: Realistic.
- Robust Health: No active ocular/uncontrolled systemic disease.
- (Not pregnant/lactating).
⭐ Absolute Contraindications: Keratoconus, active autoimmune disease, unrealistic expectations, severe dry eye.
Laser Vision Correction - Zapping to Clarity
Laser vision correction reshapes the cornea. Common types: LASIK, PRK, SMILE.
- Mechanism: Excimer laser (LASIK, PRK) ablates cornea; Femtosecond laser creates SMILE lenticule.
- Munnerlyn Formula: $t = S^2 \times D / 3$ ($t$=ablation depth, $S$=optical zone, $D$=diopters).
- Key Thresholds: Residual Stromal Bed (RSB) > 250-300 µm. LASIK flap: 100-120 µm.
| Feature | LASIK (Laser-Assisted In Situ Keratomileusis) | PRK (Photorefractive Keratectomy) | SMILE (Small Incision Lenticule Extraction) |
|---|---|---|---|
| Flap | Yes (Femto/Microkeratome, 100-120 µm) | No | No (Cap, not a full flap) |
| Epithelium | Preserved under flap | Removed (Alcohol/Mechanical) | Minimally disturbed |
| Pain | Minimal, 1-2 days | Moderate, 3-5 days | Minimal, 1 day |
| Visual Recovery | Rapid (1 day) | Slower (1-2 weeks) | Rapid (1-3 days) |
| Dry Eyes | Common, often transient | Less common than LASIK | Potentially least |
| Haze Risk | Low | Higher (esp. high myopia), Mitomycin C used | Very Low |
| Corneal Biomechanics | Reduced due to flap | Better preserved | Best preserved |
| Suited For | Wide range | Thin corneas, contact sports | Myopia, astigmatism, contact sports |
⭐ Exam Favourite: Most common LASIK complication: dry eye syndrome.
Lens-Based & Incisional Options - Alternative Routes
-
Phakic IOLs (PIOLs): Implanted lenses, natural lens retained.
- Indications: High myopia/hyperopia, astigmatism; laser unsuitable.
- Key Req: Anterior Chamber Depth (ACD) >2.8 mm (posterior), >3.0-3.2 mm (anterior); adequate Endothelial Cell Count (ECC).
- Types:
Type Location Fixation Examples Anterior Ant. Chamber Angle/Iris-claw Cachet, Artisan Posterior Post. Chamber Sulcus ICL (Visian/EVO) - Complications: Endothelial loss, cataract, glaucoma, pigment dispersion.
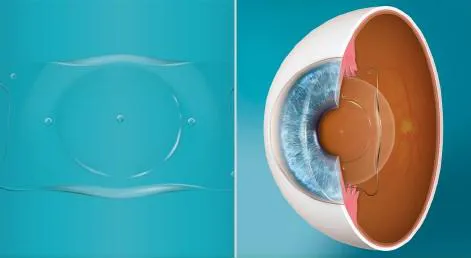
⭐ Phakic IOLs preserve accommodation & are reversible; key for high myopia, avoiding excessive corneal ablation.
-
Refractive Lens Exchange (RLE/CLE): Clear lens replaced with IOL.
- Indications: High errors, presbyopia, early cataract.
- Pros: Definitive, premium IOLs. Cons: Loses accommodation (monofocal), surgical risks.
-
Incisional Keratotomy (AK/LRIs): Corneal incisions for astigmatism.
- Uses: Native or post-op astigmatism.
- Note: Less predictable than laser methods.
Post-Op & Complications - The Aftermath
- Post-Op Regimen:
- Topical steroids (e.g., Prednisolone) & antibiotics (e.g., Moxifloxacin) tapered.
- Frequent preservative-free artificial tears.
- Protective eyewear.
- Complications:
- Early: Dry eye, flap striae, Diffuse Lamellar Keratitis (DLK), infection.
- Late: Regression, haze (PRK > LASIK), corneal ectasia, epithelial ingrowth.

| Complication | Management Highlights |
|---|---|
| Dry Eye | Lubricants, Punctal Plugs |
| Flap Striae | Observe or Flap lift & reposition/stretch |
| DLK | ↑Steroids; Flap lift & irrigation (severe) |
| Epithelial Ingrowth | Observe or Debridement ± MMC |
| %%{init: {'flowchart': {'htmlLabels': true}}}%% | |
| flowchart TD |
Start["👁️ Flap Striae
• Post-LASIK finding• Corneal wrinkles"]
Decision["📋 Assessment
• Visual impact?• Check symptoms"]
Monitor["👁️ Monitoring
• Observe progress• Routine follow-up"]
Treatment["💊 Flap Repair
• Lift and reposition• Stretch the flap"]
Outcome["✅ Assess Result
• Check VA levels• Resolution status"]
Start --> Decision Decision -->|No| Monitor Decision -->|Yes| Treatment Treatment --> Outcome
style Start fill:#F7F5FD, stroke:#F0EDFA, stroke-width:1.5px, rx:12, ry:12, color:#6B21A8 style Decision fill:#FEF8EC, stroke:#FBECCA, stroke-width:1.5px, rx:12, ry:12, color:#854D0E style Monitor fill:#EEFAFF, stroke:#DAF3FF, stroke-width:1.5px, rx:12, ry:12, color:#0369A1 style Treatment fill:#F1FCF5, stroke:#BEF4D8, stroke-width:1.5px, rx:12, ry:12, color:#166534 style Outcome fill:#F6F5F5, stroke:#E7E6E6, stroke-width:1.5px, rx:12, ry:12, color:#525252
> ⭐ Corneal ectasia: most feared long-term complication. Risk factors: thin residual stromal bed (<**300**µm), high myopia, abnormal pre-op topography.
## High‑Yield Points - ⚡ Biggest Takeaways
> * **LASIK**: **Corneal flap** for excimer ablation. **PRK**: **Epithelium removed**, then **stromal surface ablation**.
> * **SMILE**: **Flapless**; femtosecond laser creates intrastromal **lenticule**, then extracted.
> * **Wavefront/Topography-guided** ablations reduce **higher-order aberrations** (HOAs) for better vision quality.
> * Commonest side effect: **Dry eye**. Most serious risk: **Corneal ectasia** (maintain **Residual Stromal Bed**).
> * Ideal candidates: Age >**18 years**, **stable refraction** (≥1 year), adequate **corneal thickness** & topography.
> * Contraindications: **Keratoconus**, **thin corneas**, **unstable refraction**, active ocular/systemic inflammation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

