Ocular Tox Basics - Toxic Trouble Types
- Scope: Ocular toxicology investigates adverse effects of drugs, chemicals, and physical agents on eye structures and visual function.
- Routes of Exposure:
- Systemic: Ingestion, inhalation, injection (IV/IM).
- Topical: Eye drops, ointments, contact lenses.
- Direct: Chemical burns, foreign bodies, trauma.
- Intraocular: Surgical, injections.
- Mechanisms of Damage:
- Direct cytotoxicity.
- Inflammation & immune reactions.
- Vascular endothelial damage.
- Neurotoxicity (e.g., optic nerve).
- Phototoxicity.
⭐ Chloroquine/Hydroxychloroquine can cause "bull's eye" maculopathy, a classic example of drug-induced retinal toxicity.
Systemic Drugs & Eye - Eye Alarms
Many systemic drugs cause ocular toxicity. Early recognition prevents irreversible damage.
| Drug | Key Ocular Alarm | Notes (Critical Info/Dose) |
|---|---|---|
| Ethambutol | Optic neuritis (↓R-G, ↓VA) | Dose >15 mg/kg/day; Reversible if early |
| Chloroquine/HCQ | Bull's eye maculopathy, Vortex keratopathy | HCQ ≤5 mg/kg/day; Irreversible maculopathy |
| Amiodarone | Vortex keratopathy (common), Optic neuropathy (rare) | Whorl-like deposits; Monitor vision |
| Corticosteroids | Posterior Subcapsular Cataract (PSC), ↑IOP (Glaucoma) | Any route, long-term use |
| Tamoxifen | Crystalline retinopathy, Macular edema | Dose & duration dependent |
| Digoxin | Xanthopsia (yellow vision), Photopsia | Sign of toxicity |
| Sildenafil | Cyanopsia (blue vision), NAION risk | PDE5 inhibitors |
| Topiramate | Acute angle closure glaucoma, Myopic shift | Idiosyncratic, bilateral |
| Vigabatrin | Bilateral concentric visual field loss | Irreversible; Regular perimetry essential |
Topical Agents & Tox - Drop Dangers
- Benzalkonium Chloride (BAK): Most common preservative.
- Detergent; disrupts cell membranes.
- Toxicity: Corneal epithelial damage, ↓ tear film stability, conjunctival inflammation. Dose & duration-dependent.
- 📌 BAK: Bothers And Kills cornea.
- Key Agent Toxicities:
- Topical Anesthetics (e.g., Proparacaine): Abuse → ring keratitis, persistent epithelial defects.
- Miotics (e.g., Pilocarpine): Brow ache, induced myopia. Chronic use → iris cysts, anterior subcapsular cataracts.
- Mydriatics (e.g., Phenylephrine): 10% solution ↑ systemic risk (hypertension, arrhythmias) vs 2.5%. ⚠️ Caution: infants, elderly.
- Thimerosal: Mercury-based; hypersensitivity.
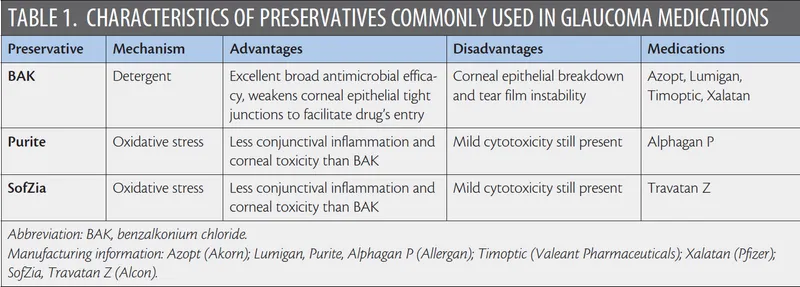
⭐ BAK-induced ocular surface disease significantly impacts long-term glaucoma management and patient adherence.
Chemicals & Plants - Eye Assaults
-
Chemical Burns:
- Acids: Coagulative necrosis (barrier). E.g., $H_2SO_4$. Less severe.
- Alkalis: Liquefactive necrosis (saponification). Deeper penetration. More severe. E.g., $NaOH$, $Ca(OH)_2$ (cement), $NH_3$.
⭐ Alkali burns are more severe than acid burns due to deeper tissue penetration.
- Management:
- Immediate copious irrigation (water/saline) for 15-30 mins.
- Check pH (target 7.0-7.4). Morgan lens.
- 📌 Mnemonic: "ALKALI = ALL KILLS EYE".
-
Plant Toxins:
- Calotropis (Madar): Milky latex → kerato-uveitis, corneal edema.
- Ricinus communis (Castor): Ricin → conjunctivitis, keratitis.
- Datura: Atropine → mydriasis, cycloplegia.
- Parthenium: Allergic conjunctivitis.
Ocular Tox Management - Eye Emergency Rx
- Priority: Rapid, thorough decontamination.
- Key Actions:
- Ensure ABCs; remove from source; remove contact lenses.
- Irrigate: Copious sterile saline/Ringer's lactate/tap water for 15-30 min. Morgan lens aids continuous flow.
- pH Testing: Check conjunctival fornix pH (normal 7.0-7.4). Continue irrigation until neutralized.
- Identify toxin.
- Medications: Topical anaesthetic, cycloplegic, antibiotic.
- Urgent ophthalmology referral.
⭐ For chemical eye burns, immediate and copious irrigation (minimum 1-2L or for 15-30 minutes) is paramount, even before full assessment.
High‑Yield Points - ⚡ Biggest Takeaways
- Chloroquine/Hydroxychloroquine: Bull's eye maculopathy; regular screening vital.
- Ethambutol: Optic neuritis (retrobulbar, dose-dependent); monitor red-green color vision.
- Corticosteroids: Posterior subcapsular cataract and steroid-induced glaucoma.
- Amiodarone: Vortex keratopathy (corneal verticillata) and optic neuropathy.
- Digitalis: Xanthopsia (yellow vision) and blurred vision.
- Tamoxifen: Crystalline retinopathy and macular edema.
- Methanol poisoning: Severe optic atrophy, "snowstorm" vision, and potential blindness.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

