Ocular Diagnostic Agents: Overview - Scene Setters
- Aid in comprehensive eye examination and accurate diagnosis.
- Used to:
- Visualize ocular structures.
- Measure Intraocular Pressure (IOP).
- Assess tear film integrity.
- Identify corneal abrasions or lesions.
- Administration routes: Topical (most common), oral, intravenous.
- Crucial for procedures: tonometry, angiography, pupillary dilation.
⭐ Most ocular diagnostic agents are administered topically for localized effect and rapid onset.
Mydriatics & Cycloplegics - Pupil Expanders
-
Parasympatholytics (Anticholinergics e.g., Atropine): Block muscarinic receptors in iris sphincter & ciliary muscle → mydriasis (pupil dilation) & cycloplegia (ciliary muscle paralysis).
-
Sympathomimetics (α1-agonists e.g., Phenylephrine): Stimulate α1 receptors in iris dilator muscle → mydriasis (no cycloplegia).
-
Comparison of Common Agents:
Drug Onset (min) Duration Mydriasis Cycloplegia Clinical Use Atropine 1% 30-40 7-10 days +++ +++ Uveitis, cycloplegic refraction in children <5 yrs Homatropine 2% 30-90 1-3 days ++ ++ Uveitis (milder alternative to atropine) Cyclopentolate 0.5-1% 30-60 1 day +++ ++ Routine cycloplegic refraction in children >5 yrs & adults Tropicamide 0.5-1% 15-30 4-6 hrs +++ + Routine fundoscopy, pre/post-op mydriasis Phenylephrine 2.5%, 10% 15-30 2-3 hrs +++ Nil Mydriasis without cycloplegia, pre-op, breaking posterior synechiae -
📌 Mnemonic: "ATropine = ATtenDS longest duration; Tropicamide = Tropical climate (short stay/acting for routine exam)"
-
⚠️ Caution: Risk of precipitating acute angle-closure glaucoma. Systemic side effects (dry mouth, tachycardia, CNS toxicity) esp. with atropine in children. Phenylephrine 10% contraindicated in infants, elderly, and patients with hypertension/cardiac disease.
⭐ Tropicamide provides rapid mydriasis with minimal cycloplegia, making it ideal for routine fundoscopy due to its short duration of action and quick recovery time for the patient. Phenylephrine is often combined with tropicamide for maximal pupil dilation without significant cycloplegia for diagnostic purposes or pre-operative preparation.
Topical Anesthetics - Surface Smoothers
- Block nerve conduction (Na+ channels) → temporary anesthesia.
- Common agents: Proparacaine, Tetracaine, Lidocaine.
- Proparacaine: Onset 15-30 sec, duration 10-20 min. 📌 Proparacaine - P for Painless Procedures.
- Tetracaine: Longer duration, more stinging.
- Lidocaine: Available as gel for prolonged contact.
- Uses: Tonometry, suture removal, foreign body removal, gonioscopy.
- Facilitate corneal/conjunctival examination by reducing discomfort.
⭐ Repeated use of topical anesthetics can lead to severe corneal toxicity (ring infiltrates) and retard healing (corneal melt).
Diagnostic Dyes - Staining Secrets
| Dye | Stains | Key Uses | Color (Filter) |
|---|---|---|---|
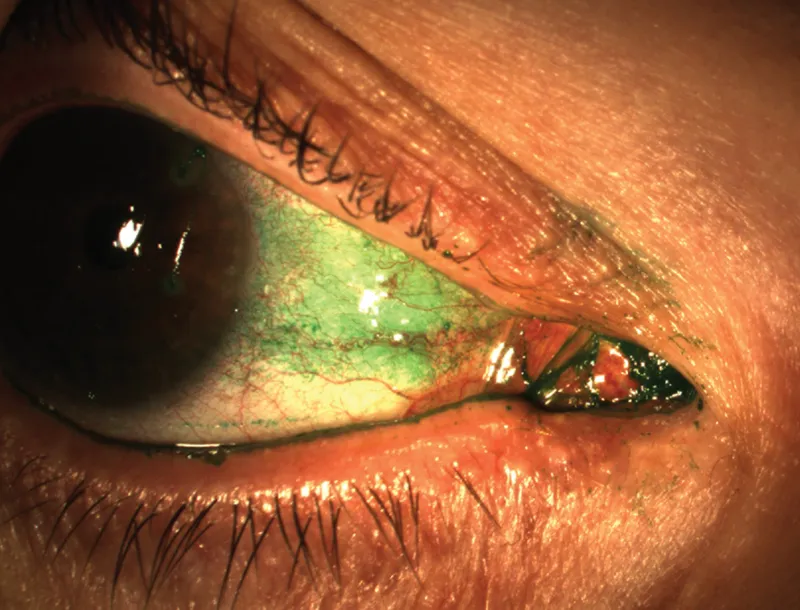
| Fluorescein Na | Epithelial defects, intercellular space | Abrasions, ulcers, Seidel's, FFA, tonometry, NLD patency | Green (Cobalt Blue) |
| Rose Bengal | Dead/devitalized cells, mucus | Dry eye (KCS), Herpetic keratitis (dendrites) | Red (White) |
| Lissamine Green | Dead/devitalized cells, mucus (gentle) | Dry eye (KCS), similar to Rose Bengal | Green (White) |
| ICG | Choroidal vessels (plasma bound) | ICGA (CNVM, PCV, tumors) | Green (Infrared) |
⭐ Fluorescein angiography (FFA) is crucial for visualizing retinal and choroidal vascular pathology.
Miotics in Diagnosis - Constriction Clues
- Pilocarpine (cholinergic agonist) tests pupillary sphincter function & denervation supersensitivity in dilated or poorly reactive pupils.
- Key Diagnostic Tests:
- Adie's Tonic Pupil: Constricts with dilute pilocarpine (0.1%-0.125%).
⭐ Dilute pilocarpine (0.1% or 0.125%) causes constriction in Adie's tonic pupil due to denervation supersensitivity.
- 1% Pilocarpine: Differentiates CN III palsy (pupil constricts if sphincter intact) from pharmacologic blockade (no constriction).
- Adie's Tonic Pupil: Constricts with dilute pilocarpine (0.1%-0.125%).
High‑Yield Points - ⚡ Biggest Takeaways
- Fluorescein sodium: Stains corneal epithelial defects, vital for Seidel's test, tonometry, FFA. Excitation 490nm, emission 530nm.
- Rose bengal & Lissamine green: Stain devitalized cells/mucus in dry eye; Lissamine is less irritating.
- Indocyanine green (ICG): For choroidal angiography (CNV); infrared fluorescence, protein-bound.
- Topical anesthetics (e.g., Proparacaine): Rapid, short-acting anesthesia for procedures; risk of corneal toxicity.
- Mydriatics: Tropicamide (cycloplegic) and Phenylephrine (non-cycloplegic) for pupil dilation during fundoscopy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

