Mydriasis & Cycloplegia - Pupil Power Play
- Mydriasis: Dilation of the pupil, increasing light entry.
- Cycloplegia: Paralysis of the ciliary muscle, resulting in loss of accommodation (near vision focus).
Autonomic Control of Pupil & Accommodation:
- Iris Muscles:
- Sphincter Pupillae: Contracts pupil (miosis). Innervated by Parasympathetic (M3 receptors).
- Dilator Pupillae: Dilates pupil (mydriasis). Innervated by Sympathetic (α1 receptors).
- Ciliary Muscle: Controls accommodation (near vision). Innervated by Parasympathetic (M3 receptors).
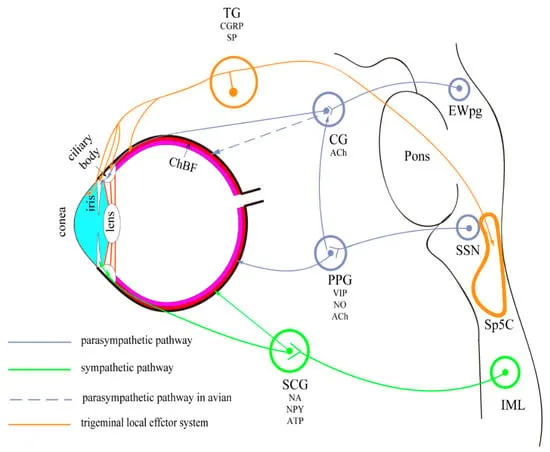
Simplified Mechanism:
⭐ Ciliary muscle contraction (leading to miosis and accommodation) is primarily mediated by parasympathetic stimulation of M3 receptors; blockade of these receptors causes cycloplegia.
📌 Mnemonic: Sympathetic = See far (mydriasis); Parasympathetic = Prepare for near (miosis, accommodation).
Anticholinergic Agents - Blurry Vision Crew
Muscarinic receptor antagonists. Block acetylcholine at muscarinic receptors in ciliary body (cycloplegia) & iris sphincter (mydriasis).
| Drug | Onset | Myd. Duration | Cyc. Duration | Potency (Myd:Cyc) | Key Uses | Cautions/Notes |
|---|---|---|---|---|---|---|
| Atropine | 30-40m/1-3h | Up to 10 d | 7-12 d | Strongest | Refraction (<7y), severe uveitis, penalization | Systemic risk; narrow angle glaucoma. |
| Homatropine | 30-90m | 1-3 d | 1-2 d | Moderate | Mild uveitis, refraction (older) | Less potent/toxic vs Atropine. |
| Cyclopentolate | 20-45m | ~24 h | 6-24 h | Strong | Routine refraction, uveitis | CNS effects (kids); rapid. |
| Tropicamide | 15-30m | 4-6 h | 4-6 h | Myd > Cyc | Fundoscopy, short cycloplegia | Shortest; stings. Least cycloplegic. |
⭐ Atropine is the most potent cycloplegic and mydriatic agent, with the longest duration of action, making it suitable for cycloplegic refraction in young children and treatment of severe uveitis.
Sympathomimetic Agents - Wide-Eyed Wonders
Mechanism: α1-agonists on iris dilator.
-
Phenylephrine
- Mechanism: Potent α1-agonist.
- Onset: ~30 min. Duration: 3-5 hrs.
- Uses: Mydriasis without cycloplegia. 2.5% (routine); 10% (caution: infants/elderly, systemic CV risks).
- Side Effects: Hypertension, tachycardia.
⭐ Phenylephrine: Mydriasis without cycloplegia; good for fundus exam if accommodation preserved or cycloplegia unwanted.
-
Hydroxyamphetamine
- Mechanism: Indirect; releases norepinephrine.
- Onset: ~45 min. Duration: ~6 hrs.
- Uses: Differentiates Horner's (pre- vs. post-ganglionic). Mydriasis if post-ganglionic neuron intact.
-
Cocaine
- Mechanism: Blocks norepinephrine reuptake.
- Onset: ~20 min. Duration: ~2 hrs.
- Uses: Horner's diagnosis (no mydriasis in affected eye).
- Note: Corneal toxicity. 📌 Cocaine: No dilation in Horner's.
Clinical Uses & Risks - Eye Spy Applications
- Therapeutic Uses
- Uveitis: Prevents synechiae, relieves ciliary spasm.
- Cycloplegic refraction: Essential in children.
- Amblyopia: Penalization of the sound eye.
- Pre/post-operative: E.g., cataract surgery for pupil dilation.
- Diagnostic Uses
- Fundoscopy: Dilated pupil for comprehensive retinal view.
- Horner's syndrome: Cocaine (confirmatory), Hydroxyamphetamine (localization).
- Ocular Adverse Effects
- Stinging, transient blurred vision, photophobia.
- ↑ IOP; risk of acute angle-closure glaucoma.
- Systemic Adverse Effects (esp. anticholinergics)
- Dry mouth, tachycardia, flushing, CNS effects (esp. in children).
- Contraindications
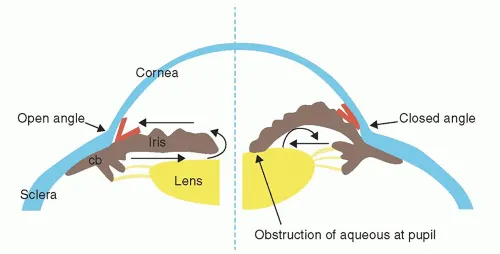
- Known narrow anterior chamber angle.
- History of angle-closure glaucoma.
⭐ A crucial contraindication for most mydriatics (especially anticholinergics) is a narrow anterior chamber angle or a history of angle-closure glaucoma, as pupillary dilation can precipitate an acute attack.
High‑Yield Points - ⚡ Biggest Takeaways
- Mydriatics (e.g., Phenylephrine) primarily dilate pupils; Cycloplegics (e.g., Atropine) also paralyze ciliary muscle & accommodation.
- Phenylephrine: Pure α1-agonist mydriatic with no cycloplegia; used for fundoscopy without affecting accommodation.
- Tropicamide: Shortest-acting anticholinergic mydriatic & cycloplegic; preferred for routine OPD examinations.
- Cyclopentolate: Stronger and longer-acting than tropicamide; standard for pediatric refraction.
- Atropine: Most potent and longest-acting anticholinergic; used for uveitis, refraction in young children, and amblyopia therapy.
- Key anticholinergic side effects: Risk of acute angle-closure glaucoma, blurred vision, photophobia, and systemic effects like dry mouth.
- Homatropine: Less potent than atropine, used for mild uveitis and has a shorter duration of action than atropine but longer than cyclopentolate and tropicamide.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

