VEGF & Its Blockers - The Growth Stoppers
- VEGF (Vascular Endothelial Growth Factor): Key protein promoting angiogenesis (new vessel growth) & ↑ vascular permeability.
- VEGF-A: Primary isoform in ocular neovascular diseases.
- Receptors: VEGFR-1, VEGFR-2 (main signaling for angiogenesis).
- Pathological Role: Hypoxia (e.g., diabetic retinopathy, CRVO) ↑VEGF → neovascularization (CNV, NVD, NVE) & macular edema.
- Anti-VEGF Agents: Monoclonal antibodies or fragments that bind VEGF, preventing its action, thus "stopping growth."
⭐ Upregulation of VEGF is a critical factor in the switch from dry to wet Age-related Macular Degeneration (AMD).
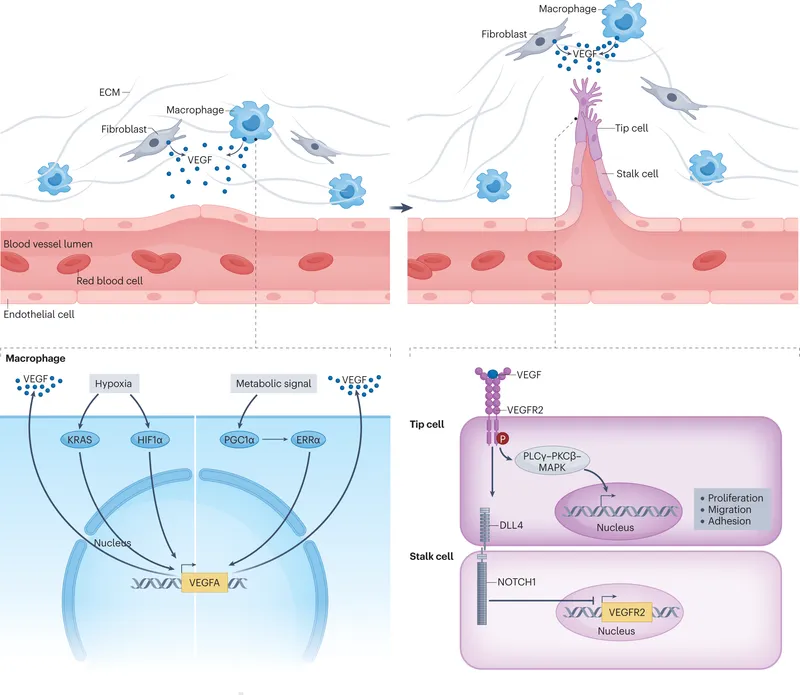
The Anti-VEGF Crew - Meet the Agents
- Ranibizumab (Lucentis): Fab fragment; Targets VEGF-A; Dose: 0.5 mg.
- Bevacizumab (Avastin): Full mAb; Targets VEGF-A; Dose: 1.25 mg (off-label); Cost-effective.
- Aflibercept (Eylea): Fusion protein (VEGF Trap); Targets VEGF-A, VEGF-B, PlGF; Dose: 2 mg.
- Brolucizumab (Pagenax/Beovu): scFv; Targets VEGF-A; Dose: 6 mg; Smallest, ⚠️ IO inflammation risk.
- Faricimab (Vabysmo): Bispecific Ab; Targets VEGF-A & Ang-2; Dose: 6 mg; Dual action.
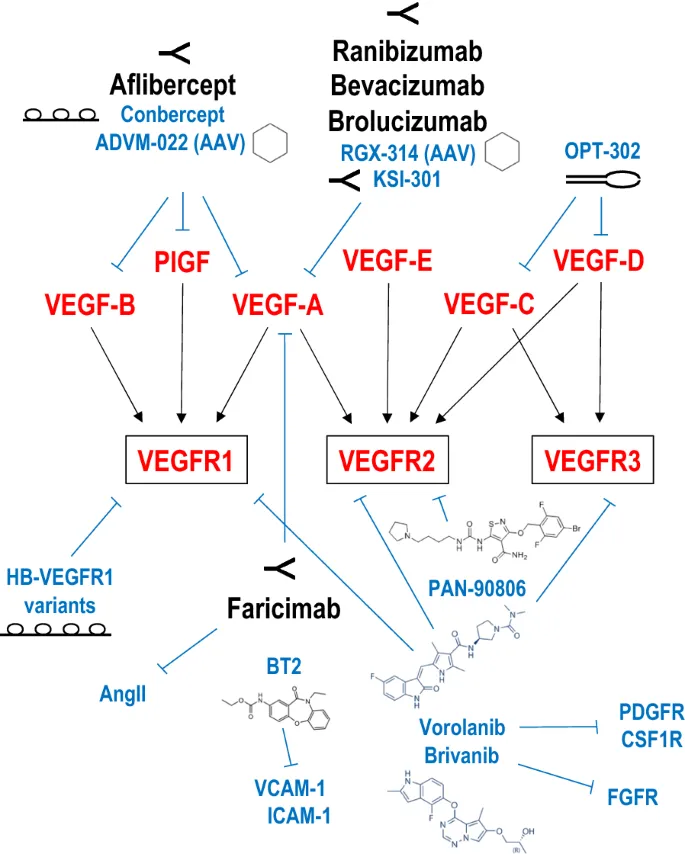
⭐ Aflibercept, a "VEGF trap," binds VEGF-A, VEGF-B, and PlGF, offering broader blockade than other early generation agents like ranibizumab or bevacizumab.
Eye Spy a Problem? - Indications Unveiled
Anti-VEGF agents target pathological angiogenesis and vascular leakage. Key indications:
- Wet AMD (nAMD): Primary therapy for choroidal neovascularization.
- Diabetic Macular Edema (DME): First-line for center-involving DME.
- Retinal Vein Occlusion (RVO): Reduces macular edema in CRVO & BRVO.
- Myopic Choroidal Neovascularization (mCNV): Effective for subfoveal/juxtafoveal lesions.
- Neovascular Glaucoma (NVG): Adjunctive to regress iris/angle neovessels pre-PRP.
- Proliferative Diabetic Retinopathy (PDR): Adjunct to PRP, or with vitreous hemorrhage.
- Retinopathy of Prematurity (ROP): For aggressive posterior ROP (Zone I, posterior Zone II).
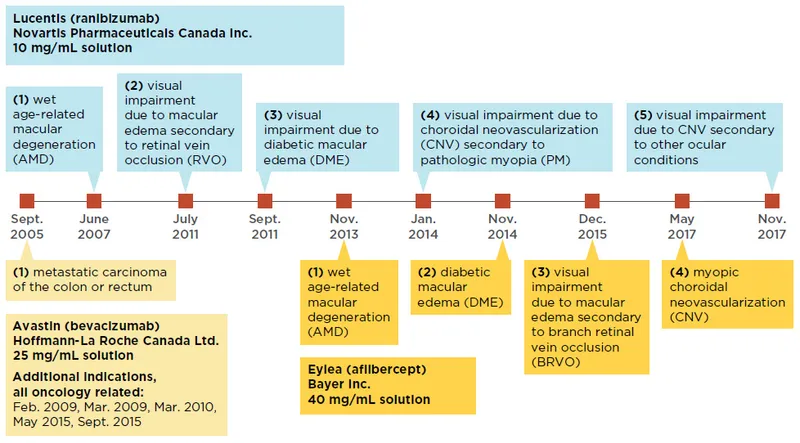
⭐ For Wet AMD, early and consistent anti-VEGF treatment is crucial for preserving vision.
The Jab & The Plan - Dosing & Delivery
-
Route: Intravitreal injection (IVT) - "The Jab".
-
Technique: Strict asepsis, topical anesthesia, povidone-iodine. Post-injection IOP check, patient education on warning signs.
-
Common Doses:
- Ranibizumab: 0.5 mg
- Bevacizumab (off-label): 1.25 mg
- Aflibercept: 2 mg
- Brolucizumab: 6 mg ⚠️ (risk of IOI/vasculitis)
- Faricimab: 6 mg
-
Dosing Strategies ("The Plan"): Goal: Maximize vision, minimize injections.
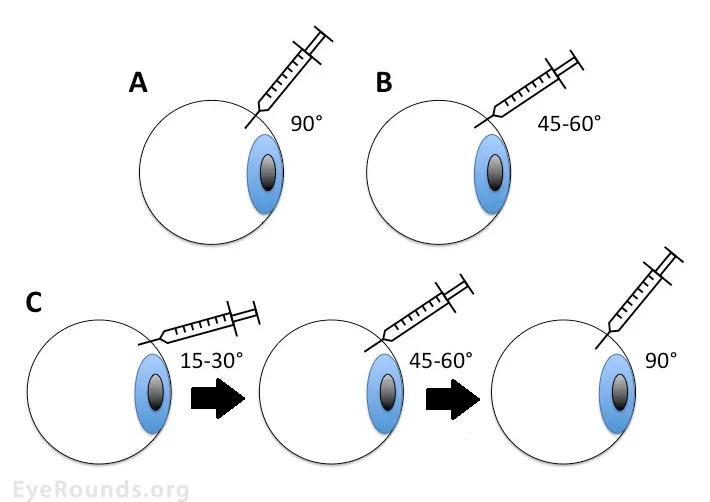
⭐ The "Treat-and-Extend" (T&E) regimen aims to reduce treatment burden while maintaining efficacy.
Uh Oh! Side Effects - Risks & Red Flags
- Ocular (Local):
- Endophthalmitis (⚠️ vision-threatening infection!)
- Intraocular inflammation (uveitis)
- ↑IOP (transient or sustained)
- Retinal detachment, vitreous/conjunctival hemorrhage
- Cataract (progression/new)
- Systemic (Rare but Serious):
- Arterial Thromboembolic Events (ATE): Stroke, MI
- Hypertension, proteinuria
- Impaired wound healing
- Contraindications/Cautions:
- Active ocular/periocular infection
- Pregnancy (teratogenic)
- Recent CVA/MI (high risk)
⭐ Risk of endophthalmitis post-injection is approximately 0.05% per injection; strict aseptic technique is crucial.
High‑Yield Points - ⚡ Biggest Takeaways
- Anti-VEGF agents (Ranibizumab, Bevacizumab, Aflibercept) inhibit angiogenesis by binding VEGF-A.
- Key indications: wet AMD, Diabetic Macular Edema (DME), Retinal Vein Occlusion (RVO).
- Administered via intravitreal injection; Bevacizumab is a common off-label choice.
- Aflibercept also binds PlGF and VEGF-B, acting as a trap receptor.
- Ranibizumab is a monoclonal antibody fragment (Fab) with shorter systemic half-life.
- Major risks: endophthalmitis, sterile inflammation/uveitis, ↑IOP, rare thromboembolic events.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

