Ocular Steroids - Powerhouse Potions
- Potent anti-inflammatory & immunosuppressive agents, crucial in ophthalmology.
- Mechanism:
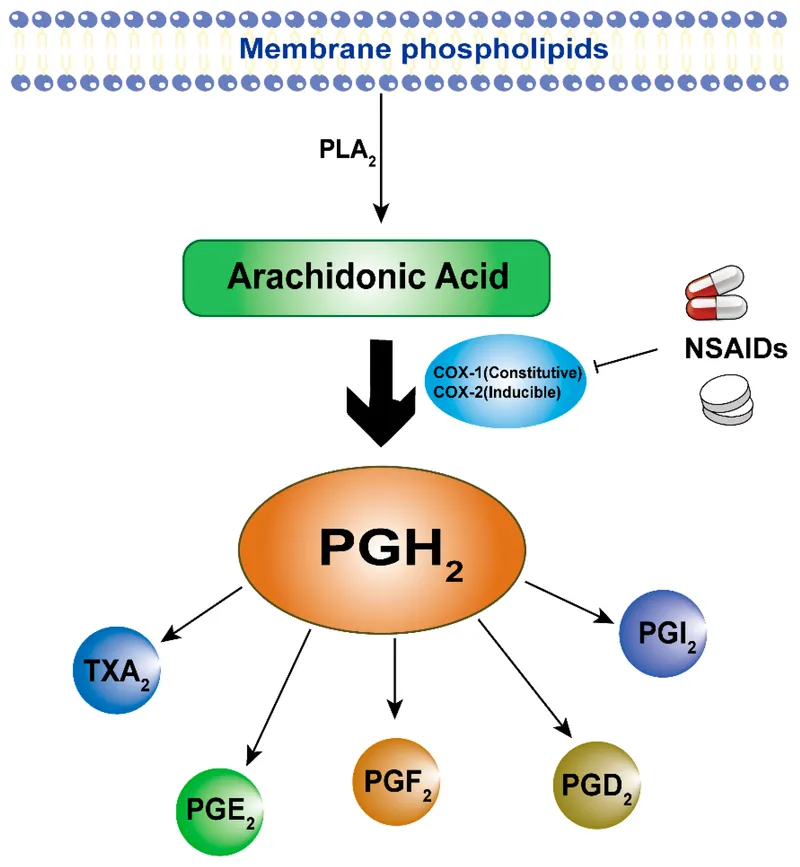
- Inhibit phospholipase A2 (PLA2) via lipocortin → ↓ arachidonic acid synthesis → ↓ prostaglandins & leukotrienes.
- Stabilize mast cells, reduce capillary permeability & cellular exudation.
- Types (Potency & Penetration):
- Strong (High Potency): Prednisolone acetate (1% susp.), Dexamethasone (0.1%), Difluprednate (0.05% emulsion - very potent).
- Excellent penetration: Prednisolone acetate, Difluprednate.
- Moderate Potency: Fluorometholone (FML) (0.1%), Loteprednol etabonate (0.2%, 0.5%).
- 📌 "Soft steroids" (Loteprednol, FML): Ester-based, rapidly metabolized locally; lower risk of ↑ IOP.
- Weak Potency: Medrysone, Hydrocortisone (rarely used topically for significant inflammation).
- Strong (High Potency): Prednisolone acetate (1% susp.), Dexamethasone (0.1%), Difluprednate (0.05% emulsion - very potent).
- Key Indications: Uveitis (all forms), severe allergic conjunctivitis/keratoconjunctivitis, post-operative inflammation, non-necrotizing scleritis, interstitial keratitis (non-infectious).
- Major Side Effects:
- ↑ Intraocular Pressure (IOP) → Steroid-induced glaucoma (monitor closely!).
- ⭐ > Most common type of cataract induced by steroids is Posterior Subcapsular Cataract (PSC).
- Delayed corneal epithelial wound healing.
- ↑ Susceptibility to secondary infections (e.g., fungal keratitis, HSV reactivation).
- Corneal thinning/perforation (prolonged use).
- ⚠️ Cautions: Active infections (esp. dendritic HSV keratitis, fungal). Always taper dose gradually to prevent rebound inflammation.

Ocular NSAIDs - Soothing Cyclo-Stoppers
- Mechanism: Inhibit cyclooxygenase (COX-1 & COX-2) enzymes $ ightarrow$ ↓ prostaglandin synthesis.
- Key Drugs & Properties:
- Ketorolac 0.4% / 0.5%: Potent analgesic; widely used post-op.
- Diclofenac 0.1%: Good anti-inflammatory; stings on instillation.
- Flurbiprofen 0.03%: Intraoperative miosis inhibition.
- Nepafenac 0.1% / 0.3%: Prodrug, better penetration; used for CME prevention post-cataract surgery.
- Bromfenac 0.09%: Long half-life, once/twice daily dosing.
- Primary Uses:
- Post-operative inflammation & pain (cataract, refractive surgery).
- Cystoid Macular Edema (CME) prophylaxis & treatment.
- Allergic conjunctivitis (mild cases).
- Episcleritis/Scleritis (adjunct or alternative to steroids).
- Corneal abrasion pain relief.
- Side Effects:
- Stinging/burning on instillation (common).
- Delayed corneal epithelial healing.
- Rare: Corneal thinning/melt (especially with prolonged use or in compromised corneas).
⭐ Topical NSAIDs, especially ketorolac and diclofenac, can be associated with corneal melt in predisposed eyes (e.g., dry eye, rheumatoid arthritis).
- Advantages over Steroids:
- No risk of ↑ Intraocular Pressure (IOP).
- No risk of cataract formation.
- Less immunosuppression. 📌 No Sight-threatening Adverse Incidents Daily (usually safe, but watch cornea!)
Other Immunomodulators - Specialized Shields
- For chronic/severe immune ocular conditions; steroid-sparing.
- Cyclosporine A (CsA): Calcineurin inhibitor; ↓ T-cell activation.
- Topical (0.05%, 0.09%): ↑ tear production in KCS; VKC, AKC.
⭐ Topical Cyclosporine A (e.g., 0.05%) works by inhibiting T-cell activation and cytokine production, approved for increasing tear production in keratoconjunctivitis sicca (KCS).
- Systemic: Severe uveitis (e.g., Behçet's). Key SE: Nephrotoxicity.
- Tacrolimus (FK506): Calcineurin inhibitor (potent).
- Topical (0.03%): VKC, AKC.
- Systemic: Severe uveitis.
- Sirolimus (Rapamycin): mTOR inhibitor. Uveitis.
- Other Systemic Agents: For refractory uveitis.
- Antimetabolites: Methotrexate, Azathioprine, Mycophenolate Mofetil (MMF).
- Biologics: TNF-α inhibitors (e.g., Adalimumab for JIA-uveitis).
High‑Yield Points - ⚡ Biggest Takeaways
Error: Failed to generate content for this concept group.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

