Ophthalmic Pharmacology

On this page
🔬 Ophthalmic Drug Arsenal: Your Precision Medicine Command Center
Mastering ophthalmic pharmacology means commanding an arsenal that spans pressure reduction in glaucoma, infection eradication, inflammation control, and diagnostic precision-all delivered through a unique anatomical barrier that demands specialized formulations. You'll learn how drugs target aqueous humor dynamics, when to deploy combinations for synergistic effect, and how sustained-release innovations are transforming patient adherence. This lesson builds your clinical decision-making from mechanism to application, equipping you to select the right agent for the right eye condition with confidence and precision.
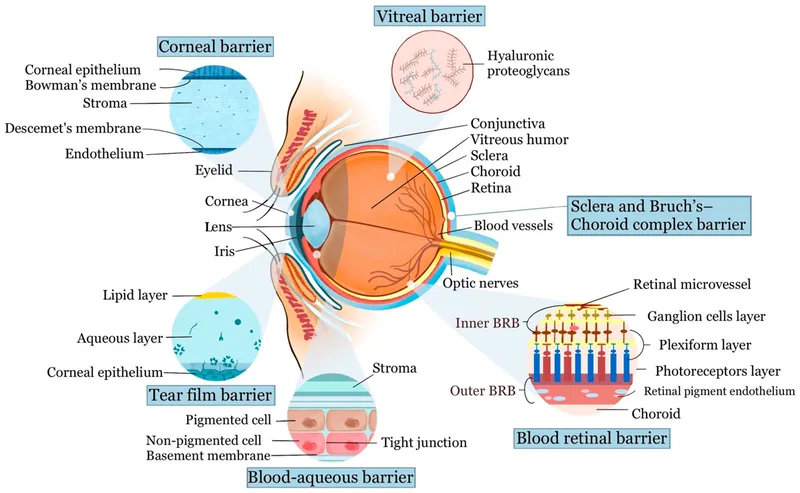
The eye's unique pharmacokinetic environment demands specialized knowledge. Unlike systemic circulation where drugs distribute freely, ocular tissues create distinct compartments with selective permeability. The blood-retinal barrier restricts systemic drug access by 95%, while topical drops achieve only 1-5% bioavailability in posterior segments. Understanding these limitations transforms your approach from hoping drugs reach their targets to engineering precise delivery strategies.
📌 Remember: TEARS - Topical absorption limited, Elimination rapid, Anatomical barriers multiple, Routes specialized, Systemic effects possible. Topical drops remain in contact for only 15-30 seconds before tear turnover eliminates 80% of applied medication.
Ocular Pharmacokinetic Foundations
-
Anterior Segment Delivery
- Corneal penetration: 1-5% of topical dose
- Conjunctival absorption: 10-20% systemic circulation
- Hydrophilic drugs: limited corneal penetration
- Lipophilic drugs: enhanced corneal uptake
- Contact time: 15-30 seconds before washout
- Tear turnover: 16% per minute baseline rate
-
Posterior Segment Challenges
- Vitreous half-life: 2-4 hours for small molecules
- Retinal penetration: <1% from topical application
- Intravitreal injection: 100% bioavailability
- Systemic route: <5% retinal penetration
- Blood-retinal barrier: 95% exclusion rate
- Choroidal clearance: 20-30 mL/min elimination
| Route | Bioavailability | Peak Time | Duration | Systemic Absorption | Clinical Use |
|---|---|---|---|---|---|
| Topical | 1-5% | 30-60 min | 4-8 hours | 10-20% | Anterior segment |
| Subconjunctival | 20-40% | 1-2 hours | 12-24 hours | 30-50% | Intermediate |
| Intravitreal | 90-100% | 2-6 hours | 30-180 days | <5% | Posterior segment |
| Systemic | <5% retinal | 2-4 hours | 6-12 hours | 100% | Limited utility |
| Sustained release | 60-80% | 24-72 hours | 30-365 days | <10% | Chronic conditions |
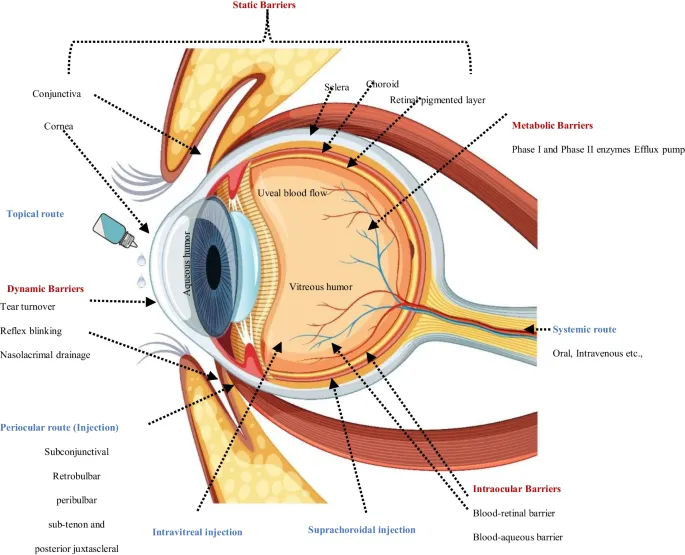
💡 Master This: The pH 7.4 tear film neutralizes most topical medications within 60 seconds. Buffered formulations maintain therapeutic pH for 2-3 minutes, increasing corneal penetration by 200-300% compared to unbuffered solutions.
Understanding drug elimination mechanisms reveals why sustained delivery systems revolutionize treatment outcomes. Conventional drops require 4-6 daily applications to maintain therapeutic levels, while sustained-release implants provide 6-12 months of consistent drug delivery. This knowledge transforms patient compliance from 30-40% with frequent dosing to >90% with long-acting systems.
Connect these pharmacokinetic principles through specialized drug classes to understand how different therapeutic targets require distinct delivery strategies.
🔬 Ophthalmic Drug Arsenal: Your Precision Medicine Command Center
⚡ Antiglaucoma Mastery: The Pressure Control Command Center
📌 Remember: GLAUCOMA - Goal pressure individualized, Lifelong treatment required, Adherence critical, Unique mechanisms combined, Compliance monitoring essential, Ocular surface considered, Monitoring systematic, Adjustments frequent. Most patients require 2-3 medications for adequate pressure control.
Prostaglandin Analog Powerhouse
-
Mechanism Mastery
- F-prostanoid receptor activation increases uveoscleral outflow by 40-60%
- Peak effect: 8-12 hours post-application
- Latanoprost: 25-30% IOP reduction
- Bimatoprost: 28-33% IOP reduction
- Travoprost: 25-28% IOP reduction
- Duration: 24+ hours with once-daily dosing
- Baseline IOP independence: effective at all pressure levels
-
Clinical Optimization Strategies
- Evening application: 15% greater efficacy than morning
- Eyelash growth: 25% length increase, 106% thickness increase
- Onset: 4-6 weeks for cosmetic changes
- Reversal: 2-3 months after discontinuation
- Iris pigmentation: 5-15% develop permanent darkening
- Periorbital fat atrophy: 2-5% incidence with chronic use
| Agent | IOP Reduction | Onset | Peak | Unique Features | Side Effects |
|---|---|---|---|---|---|
| Latanoprost | 25-30% | 3-4 hours | 8-12 hours | First-line standard | Iris pigmentation 5% |
| Bimatoprost | 28-33% | 4 hours | 8-12 hours | Highest efficacy | Eyelash growth >90% |
| Travoprost | 25-28% | 2 hours | 12 hours | BAK-free available | Hyperemia 15-20% |
| Tafluprost | 22-27% | 2-4 hours | 12 hours | Preservative-free | Least side effects |
| Latanoprostene | 28-32% | 2 hours | 8-12 hours | Nitric oxide release | Enhanced tolerability |
⭐ Clinical Pearl: Patients switching from twice-daily beta-blockers to once-daily prostaglandin analogs show 65% improvement in adherence and 20% better long-term IOP control. The "weekend effect" shows 3-5 mmHg pressure spikes when patients miss Friday evening doses.
Beta-Blocker Precision Control
-
Aqueous Production Suppression
- Ciliary body beta-2 receptor blockade reduces aqueous production by 20-25%
- Peak effect: 2 hours post-application
- Timolol: 20-25% IOP reduction
- Betaxolol: 18-23% IOP reduction (cardioselective)
- Levobunolol: 25-28% IOP reduction
- Tachyphylaxis: 10-15% efficacy loss over 6-12 months
- Systemic absorption: 80% via nasolacrimal drainage
-
Cardiovascular Considerations
- Heart rate reduction: 15-20% with non-selective agents
- Contraindications: COPD, asthma, heart block >1st degree
- Betaxolol: 50% less respiratory effects (beta-1 selective)
- Nasal punctal occlusion: 65% reduction in systemic absorption
- Drug interactions: additive effects with systemic beta-blockers
- Masking hypoglycemia: critical consideration in diabetics
💡 Master This: Twice-daily beta-blocker dosing provides 30% better 24-hour IOP control than once-daily dosing, despite manufacturers' claims. The circadian aqueous production peak at 6-8 AM requires morning coverage for optimal pressure control.
Connect these first-line agents through combination strategies to understand how multiple mechanisms achieve superior pressure control with enhanced patient compliance.
⚡ Antiglaucoma Mastery: The Pressure Control Command Center
🎯 Combination Therapy Architecture: The Synergistic Strategy Matrix
📌 Remember: COMBINE - Complementary mechanisms, Once-daily preferred, Minimal preservatives, Better adherence, IOP targets achieved, No antagonistic effects, Enhanced efficacy. Fixed combinations reduce daily drop instillations from 6-8 to 2-3 applications.
Alpha-Agonist Integration Strategies
-
Brimonidine Mechanism Mastery
- Alpha-2 receptor activation: dual mechanism action
- Aqueous production ↓ 20-25% (ciliary body)
- Uveoscleral outflow ↑ 15-20% (secondary effect)
- Peak effect: 2 hours, duration 8-12 hours
- IOP reduction: 18-25% as monotherapy
- Neuroprotective effects: independent of IOP reduction
- Alpha-2 receptor activation: dual mechanism action
-
Combination Optimization
- With prostaglandins: additive 40-50% total reduction
- With beta-blockers: synergistic aqueous suppression
- Morning brimonidine + evening prostaglandin
- Addresses circadian IOP fluctuation patterns
- Allergic reactions: 15-20% incidence (highest among glaucoma drugs)
- CNS effects: fatigue 25%, dry mouth 35% in elderly
| Combination | Total IOP Reduction | Dosing | Adherence Benefit | Key Advantages | Monitoring Points |
|---|---|---|---|---|---|
| PGA + Beta-blocker | 40-50% | BID | +60% | Complementary mechanisms | Systemic beta effects |
| PGA + Brimonidine | 35-45% | BID | +40% | Neuroprotection added | Allergic reactions |
| Beta + CAI | 35-40% | BID-TID | +30% | Aqueous suppression | Sulfa allergies |
| Triple therapy | 45-55% | BID-TID | Variable | Maximum medical therapy | Side effect burden |
| PGA + Netarsudil | 40-48% | QD | +70% | Novel ROCK inhibition | Conjunctival hyperemia |
-
Aqueous Production Blockade
- Ciliary body carbonic anhydrase II inhibition
- Aqueous production ↓ 40-60% (most potent suppressors)
- Dorzolamide: 15-20% IOP reduction
- Brinzolamide: 17-21% IOP reduction
- Acetazolamide: 25-40% reduction (systemic)
- pH effects: corneal edema risk with topical agents
- Systemic CAIs: reserved for acute situations
-
Clinical Application Mastery
- Combination with prostaglandins: most effective pairing
- Sulfa allergy: absolute contraindication (10% cross-reactivity)
- Kidney stones: 2-4% incidence with chronic systemic use
- Increased fluid intake: >2L daily prevention
- Potassium supplementation: prevents hypokalemia
- Taste alterations: 25-30% with topical agents
⭐ Clinical Pearl: Fixed-dose combinations show 85% better adherence at 12 months compared to separate bottles. The Cosopt (timolol + dorzolamide) combination provides 38-42% IOP reduction with twice-daily dosing, matching three separate medications.
💡 Master This: Preservative-free combinations reduce ocular surface disease by 60% compared to multiple preserved drops. Patients using ≥3 preserved medications develop moderate-severe dry eye in 70% of cases within 2 years.
Connect these combination strategies through novel delivery mechanisms to understand how sustained-release systems eliminate compliance issues while providing superior pressure control.
🎯 Combination Therapy Architecture: The Synergistic Strategy Matrix
🚀 Novel Delivery Revolution: The Sustained-Release Breakthrough Matrix
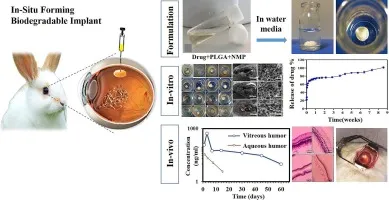
📌 Remember: SUSTAINED - Single administration, Uniform drug levels, Superior compliance, Targeted delivery, Adverse effects minimized, Implantation required, No daily dosing, Extended duration, Drug reservoir controlled. Implants eliminate >95% of compliance-related treatment failures.
Biodegradable Implant Mastery
-
Bimatoprost Sustained-Release (Durysta)
- 10 mcg biodegradable implant: 6-month duration
- IOP reduction: 30-35% sustained throughout treatment period
- Month 1: 32% reduction from baseline
- Month 6: 28% reduction maintained
- No tachyphylaxis: consistent efficacy over time
- Intracameral injection: office-based procedure
- Biodegradation: complete absorption by 18 months
-
Clinical Implementation Strategy
- Patient selection: poor compliance or multiple medications
- Contraindications: corneal endothelial compromise, active inflammation
- Endothelial cell count: >1500 cells/mm² required
- Anterior chamber depth: >2.5 mm minimum
- Monitoring: monthly IOP checks first 3 months
- Repeat implantation: safe and effective after biodegradation
| System | Duration | Drug | IOP Reduction | Procedure | Key Benefits |
|---|---|---|---|---|---|
| Durysta | 6 months | Bimatoprost | 30-35% | Intracameral injection | FDA-approved, biodegradable |
| iDose TR | 6-9 months | Travoprost | 25-30% | Intracameral implant | Refillable system |
| Punctal plugs | 30-90 days | Various | 20-25% | Office insertion | Reversible, non-invasive |
| Contact lenses | 24 hours | Timolol | 15-20% | Patient-applied | Daily wear system |
| Hydrogel inserts | 7 days | Brimonidine | 18-22% | Weekly replacement | Extended wear |
-
Supraciliary Space Delivery
- CLS-TA (triamcinolone): supraciliary injection
- Duration: 6-9 months anti-inflammatory effect
- Uveitis treatment: single injection replaces daily steroids
- Macular edema: superior efficacy to topical therapy
- Minimally invasive: 30-gauge needle, office procedure
- Systemic exposure: <5% compared to oral administration
-
Transscleral Drug Delivery
- Posterior segment targeting: bypasses systemic circulation
- Drug depot formation: sustained release over 3-6 months
- Anti-VEGF agents: quarterly injections vs monthly
- Steroids: 6-month duration vs daily drops
- Scleral permeability: enhanced by molecular size <40 kDa
- Choroidal clearance: minimized by depot formation
⭐ Clinical Pearl: Sustained-release systems reduce healthcare costs by 40-60% through decreased office visits, reduced medication waste, and improved outcomes. Durysta patients show 90% treatment satisfaction compared to 45% with multiple daily drops.
💡 Master This: Combination sustained-release systems delivering multiple drug classes simultaneously represent the future of glaucoma therapy. Dual-drug implants providing prostaglandin + beta-blocker effects for 12 months are entering clinical trials with 50-60% IOP reductions.
Connect these delivery innovations through anti-inflammatory precision to understand how targeted steroid and immunomodulator therapy manages ocular surface disease and posterior segment inflammation.
🚀 Novel Delivery Revolution: The Sustained-Release Breakthrough Matrix
🛡️ Anti-Inflammatory Precision: The Immune Control Command Center

📌 Remember: STEROID - Start high, taper slow, Timing critical, Eyes monitored closely, Risks vs benefits, Ocular pressure watched, Infection ruled out, Duration minimized. Prednisolone acetate 1% every 1-2 hours initially, then taper over 6-8 weeks based on response.
Corticosteroid Mastery Matrix
-
Potency and Penetration Hierarchy
- Prednisolone acetate: gold standard for anterior inflammation
- Corneal penetration: superior to other preparations
- Anti-inflammatory potency: 4x hydrocortisone equivalent
- Dosing: every 1-2 hours acute phase, taper gradually
- Dexamethasone: highest potency, posterior penetration
- 7x hydrocortisone equivalent potency
- Intravitreal implant: Ozurdex provides 3-6 months effect
- Fluorometholone: lower potency, reduced IOP risk
- 10x less IOP elevation than prednisolone
- Chronic use: preferred for maintenance therapy
- Prednisolone acetate: gold standard for anterior inflammation
-
Strategic Application Protocols
- Acute anterior uveitis: prednisolone acetate 1% every 1-2 hours
- Chronic inflammation: fluorometholone 0.1% twice daily
- Steroid-sparing approach: minimize long-term complications
- Pulse therapy: high-dose short courses for flares
- Posterior uveitis: intravitreal dexamethasone or systemic therapy
- Allergic conjunctivitis: mild steroids or antihistamines
| Steroid | Potency | IOP Risk | Penetration | Primary Use | Monitoring |
|---|---|---|---|---|---|
| Prednisolone acetate | High | 25-30% | Excellent anterior | Acute uveitis | Weekly IOP |
| Dexamethasone | Highest | 30-35% | Good posterior | Severe inflammation | Bi-weekly IOP |
| Fluorometholone | Low-moderate | 5-10% | Moderate | Chronic maintenance | Monthly IOP |
| Loteprednol | Moderate | <5% | Good anterior | Allergic conditions | As needed |
| Rimexolone | Low | <10% | Limited | Mild inflammation | Monthly |
-
Calcineurin Inhibitor Precision
- Cyclosporine 0.05%: dry eye and chronic inflammation
- Mechanism: T-cell activation blockade
- Onset: 6-12 weeks for full effect
- Tear production ↑ 15-20% in responders
- Tacrolimus 0.1%: severe atopic keratoconjunctivitis
- 100x more potent than cyclosporine
- Systemic absorption: minimal with topical use
- Steroid-sparing effect: reduces steroid requirements by 70-80%
- Cyclosporine 0.05%: dry eye and chronic inflammation
-
Novel Anti-Inflammatory Agents
- Lifitegrast: lymphocyte function-associated antigen-1 (LFA-1) antagonist
- Dry eye disease: twice-daily application
- Symptom improvement: 40-50% at 12 weeks
- Steroid-free option for chronic management
- Anakinra: interleukin-1 receptor antagonist
- Refractory uveitis: off-label topical use
- Systemic alternatives: adalimumab, infliximab for severe cases
- Lifitegrast: lymphocyte function-associated antigen-1 (LFA-1) antagonist
⭐ Clinical Pearl: Steroid-induced IOP elevation occurs in 25-30% of patients within 2-6 weeks. Genetic predisposition (TIGR/MYOC mutations) increases risk to >90%. Weekly IOP monitoring during first month prevents steroid-induced glaucoma.
💡 Master This: Combination therapy with steroid + antibiotic (e.g., TobraDex) provides dual coverage for infectious-inflammatory conditions. However, steroids mask infection signs, requiring confirmed bacterial etiology before initiation.
Connect these anti-inflammatory strategies through anti-infective precision to understand how antimicrobial therapy targets specific pathogens while preventing resistance development.
🛡️ Anti-Inflammatory Precision: The Immune Control Command Center
🦠 Anti-Infective Arsenal: The Pathogen Elimination Command Center
📌 Remember: INFECTION - Immediate treatment, Narrow spectrum when possible, Frequent dosing initially, Empirical then targeted, Cultures before treatment, Toxicity monitoring, Improvement expected 48-72h, Ocular penetration critical, No delays permitted. Fortified antibiotics provide 10-50x higher concentrations than commercial preparations.
Bacterial Warfare Mastery
-
Fluoroquinolone Precision Targeting
- Fourth-generation agents: moxifloxacin, gatifloxacin
- Gram-positive coverage: excellent including MRSA
- Gram-negative coverage: broad spectrum including Pseudomonas
- Corneal penetration: therapeutic levels achieved topically
- Resistance rates: <5% for most common pathogens
- Dosing strategy: every 15-30 minutes first 6 hours, then hourly
- Monotherapy efficacy: >90% for bacterial keratitis
- Fourth-generation agents: moxifloxacin, gatifloxacin
-
Fortified Antibiotic Protocols
- Vancomycin 25-50 mg/mL: Gram-positive including MRSA
- Endophthalmitis: intravitreal 1-2.25 mg injection
- Severe keratitis: topical every 30-60 minutes
- Ceftazidime 50 mg/mL: Gram-negative including Pseudomonas
- Synergistic combination with aminoglycosides
- Intravitreal dose: 2-2.25 mg for endophthalmitis
- Tobramycin 15 mg/mL: aminoglycoside for severe infections
- Concentration-dependent killing: peak levels critical
- Ototoxicity risk: minimal with topical use
- Vancomycin 25-50 mg/mL: Gram-positive including MRSA
| Pathogen | First-Line Agent | Concentration | Dosing | Resistance Rate | Special Considerations |
|---|---|---|---|---|---|
| S. aureus (MSSA) | Moxifloxacin | 0.5% | Q1-2h | <5% | Excellent penetration |
| S. aureus (MRSA) | Vancomycin | 25-50 mg/mL | Q30-60min | <2% | Fortified preparation |
| Pseudomonas | Ceftazidime | 50 mg/mL | Q30-60min | <10% | Combination therapy |
| Streptococcus | Moxifloxacin | 0.5% | Q1-2h | <3% | Rapid bactericidal |
| Enterococcus | Vancomycin | 25-50 mg/mL | Q30-60min | <5% | VRE considerations |
-
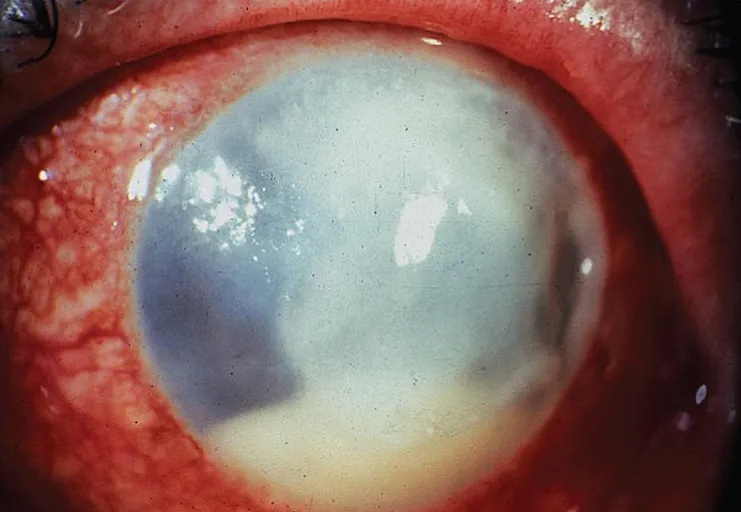
Herpes Simplex Virus Management
- Ganciclovir 0.15%: first-line topical therapy
- Superior efficacy: >90% epithelial healing at 2 weeks
- Lower toxicity: minimal corneal toxicity vs older agents
- Dosing: 5 times daily until healing, then 3 times daily
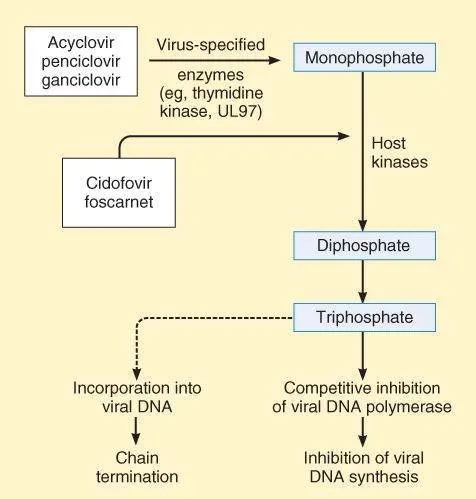
- Oral acyclovir: systemic coverage for severe cases
- 800 mg 5 times daily for 7-10 days
- Stromal keratitis: combination topical + oral therapy
- Prophylaxis: 400 mg twice daily for recurrent disease
- Ganciclovir 0.15%: first-line topical therapy
-
Cytomegalovirus Retinitis Protocols
- Intravitreal ganciclovir: 2 mg injection every 1-2 weeks
- Ganciclovir implant: 6-month sustained release
- Vitrasert: 1 mcg/hour release rate
- Local therapy: avoids systemic toxicity
- Oral valganciclovir: 900 mg twice daily induction
- Maintenance: 900 mg daily long-term
- Bioavailability: 60% vs 5% with ganciclovir
⭐ Clinical Pearl: Culture-negative infections occur in 30-40% of cases due to prior antibiotic use or fastidious organisms. PCR testing identifies pathogens in 80-90% of culture-negative cases, enabling targeted therapy.
💡 Master This: Combination antifungal therapy with topical + systemic agents improves outcomes in severe fungal keratitis by 40-50%. Natamycin 5% remains first-line for filamentous fungi, while amphotericin B 0.15% targets yeasts effectively.
Connect these anti-infective strategies through diagnostic precision to understand how specialized diagnostic agents enable accurate assessment and monitoring of ocular conditions.
🦠 Anti-Infective Arsenal: The Pathogen Elimination Command Center
🔍 Diagnostic Precision Arsenal: The Clinical Assessment Command Center
📌 Remember: DIAGNOSE - Dye selection critical, Injection technique proper, Allergic reactions possible, Good visualization essential, Normal vs abnormal patterns, Optimal timing crucial, Safety protocols followed, Emergency management ready. Fluorescein shows <1% serious adverse reactions, while ICG has <0.1% severe complications.
Fluorescein Mastery Matrix
-
Topical Fluorescein Applications
- Epithelial defect detection: 2% sodium fluorescein strips
- Corneal abrasions: bright green staining under cobalt blue light
- Dry eye assessment: tear break-up time measurement
- Contact lens fitting: fluorescein pattern analysis
- Applanation tonometry: essential for accurate IOP measurement
- Goldmann standard: fluorescein semicircles for pressure assessment
- Optimal pattern: inner edges just touching
- Seidel test: aqueous leak detection post-trauma/surgery
- Positive test: streaming fluorescein indicates full-thickness defect
- Epithelial defect detection: 2% sodium fluorescein strips
-
Intravenous Fluorescein Angiography
- Dosing protocol: 5-10 mL of 10% sodium fluorescein
- Circulation timing: arm-to-retina in 10-15 seconds
- Choroidal phase: 10-15 seconds post-injection
- Arterial phase: 15-20 seconds filling
- Venous phase: 20-30 seconds complete filling
- Late phase: 5-10 minutes for leakage assessment
- Pathology detection: microaneurysms, neovascularization, leakage
| Application | Concentration | Method | Timing | Key Findings | Clinical Significance |
|---|---|---|---|---|---|
| Epithelial defects | 2% strips | Topical | Immediate | Green staining | Trauma, infection, dry eye |
| Tear film assessment | 2% strips | Topical | <10 seconds | Break-up patterns | Dry eye severity |
| Angiography | 10% solution | IV | 10-15 seconds | Vascular filling | Retinal pathology |
| Leak detection | 2% strips | Topical | Immediate | Streaming dye | Surgical complications |
| Tonometry | 2% strips | Topical | Immediate | Semicircle pattern | IOP measurement |
-
Indocyanine Green Precision
- Choroidal circulation mapping: superior to fluorescein
- Near-infrared imaging: 805nm excitation, 835nm emission
- Protein binding: 98% allows choroidal vessel visualization
- Dosing: 25 mg in 5 mL sterile water
- Clinical applications: choroidal neovascularization, polypoidal choroidal vasculopathy
- PCV detection: >90% sensitivity vs <50% with fluorescein
- Treatment guidance: photodynamic therapy targeting
- Safety profile: <0.1% severe reactions, contraindicated in iodine allergy
- Choroidal circulation mapping: superior to fluorescein
-
Optical Coherence Tomography Contrast
- Fluorescein-guided OCT: real-time perfusion assessment
- Enhanced depth imaging: choroidal thickness measurement
- Normal thickness: 200-400 microns depending on age/location
- Pathological changes: <150 microns or >500 microns
- Quantitative analysis: objective measurements replace subjective interpretation
⭐ Clinical Pearl: Combination fluorescein + ICG angiography provides complementary information in 80% of complex retinal cases. Sequential imaging within same session reduces patient burden while maximizing diagnostic yield.
💡 Master This: Fundus autofluorescence using lipofuscin as endogenous fluorophore detects RPE pathology without exogenous dyes. Increased autofluorescence indicates RPE dysfunction, while decreased signal suggests RPE atrophy or blocking lesions.
These diagnostic precision tools complete the comprehensive ophthalmic pharmacology arsenal, enabling clinicians to detect pathology early, monitor treatment response accurately, and guide therapeutic interventions with scientific precision rather than clinical guesswork.
🔍 Diagnostic Precision Arsenal: The Clinical Assessment Command Center
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app






















